California orders skilled nursing facilities to accept coronavirus patients

- Share via
As fears escalate about the toll the coronavirus will take on the sick and elderly in nursing homes — who are among the most vulnerable to the deadly virus — California regulators have told skilled nursing facility operators that they must accept patients even if they have the disease.
The order comes amid a fierce debate between healthcare providers. Hospitals are desperate to clear space for an expected wave of COVID-19 patients, so they are discharging as many patients as possible, including nursing home residents.
Many nursing home administrators are equally desperate to keep those residents out until they are proven virus-free, fearing a catastrophic result if the deadly pathogen gains a foothold in their institutions.
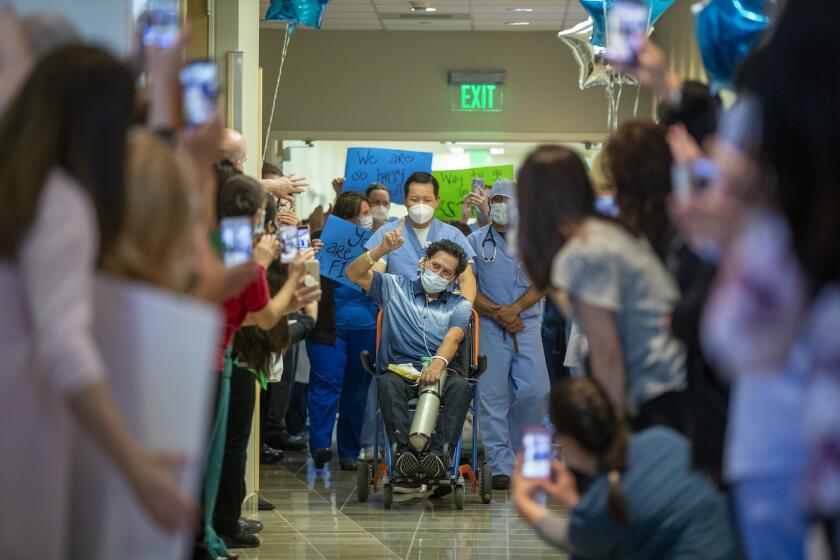
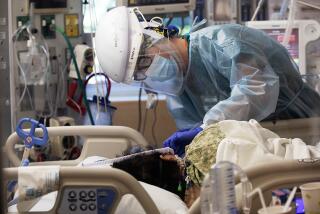
These are some of the unusual new scenes across the Southland during the coronavirus outbreak.
The directive, in a letter to facilities on Monday from California Department of Public Health Deputy Director Heidi Steinecker, appears to side squarely with the hospitals. It says skilled nursing facilities “shall not refuse to admit or readmit a resident based on their status as a suspected or confirmed COVID-19 case.”
California nursing home administrators and advocates for the elderly view the order as an alarming move by Gov. Gavin Newsom’s administration.
“Sacrificing the lives of beloved nursing home residents is beyond unconscionable,” said Patricia McGinnis, executive director of California Advocates for Nursing Home Reform.
“California’s directive is nothing less than a death sentence for countless residents. The state should instead look to alternative locations such as hotels and conference centers as much safer places to send COVID-19 patients for care,” McGinnis said.
Reached by phone by a Times reporter on Wednesday afternoon, Steinecker, who signed the letter, said “more nuanced” guidance would be sent to home operators “today.” She declined to say what the guidance would be.
The order applies to the more than 1,000 skilled nursing facilities licensed by the California Department of Public Health. Assisted living and other long-term elder care homes, which do not provide the same level of medical care, are regulated by the state’s Department of Social Services and are not subject to Steinecker’s directive.
Dr. Michael Wasserman, a geriatrician for more than 30 years and president of the California Assn. of Long Term Care Medicine, has been lobbying California regulators not to force homes to take in people unless they are proven virus-free. Doing otherwise, he said, is “akin to premeditated murder.”
So when he and his colleagues first saw the new order Monday night, they were “inconsolable,” he said.
“I didn’t sleep, I was in tears.... the problem is our government isn’t listening to the experts.”
The toll coronavirus can take on a confined, sick and elderly population became starkly clear at the Life Care Center nursing home in Kirkland, Wash., one of the first hot spots in the U.S. Two-thirds of the residents and 47 workers fell ill, and 37 people died.
Since then, outbreaks have been occurring in nursing homes across the country at terrifying speed — forcing operators to ban visitors, confine patients to their rooms and scramble to create sterile wings to treat residents who come down with the disease.
Hundreds of long-term care facilities in the U.S. now have residents who are infected with the virus. On Tuesday, health officials in Washington state reported 108 outbreaks at long-term care facilities. And at a single nursing home in Tennessee, more than 100 residents have tested positive.
In Connecticut, state officials are reopening previously closed facilities to create separate nursing homes only for residents who are positive for COVID-19 — like modern-day leper colonies. The “extreme precaution” is warranted, according to Connecticut officials, because the results can be catastrophic when the virus gets loose among such a vulnerable population.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.