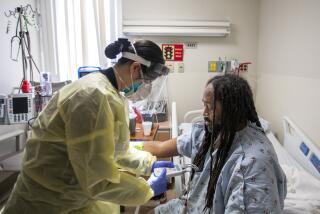
There isn’t just a shortage of ventilators, but of the medical workers who operate them

- Share via
A nationwide shortage of ventilators to treat COVID-19 patients has prompted governors to plead for more machines from the federal government as factories race to start building them.
But ventilators alone aren’t much use to patients without respiratory therapists — the medical workers trained to operate them. And the rapidly growing demand, combined with the limited number of licensed therapists, could impede efforts to treat COVID-19 patients as they begin to overwhelm hospitals and the pandemic worsens, experts say.
Each patient on a ventilator, which pushes air in and out of the lungs, needs care from a doctor, a nurse and a respiratory therapist.
“A ventilator without that stuff is a kinda cool paperweight,” said Dr. Lewis Rubinson, a New Jersey critical care doctor who has been treating COVID-19 patients in the intensive care unit.
It’s difficult to estimate the exact number of ventilators and health workers needed to respond to COVID-19 since it depends on how many people ultimately catch the coronavirus and over what period of time, both of which are affected by the recently implemented social distancing measures.
But even if hospitals can get all the ventilators they need, they may not have the staffing.
A 2015 study found that a limited number of respiratory therapists would likely constrain how many patients on ventilators a hospital could treat during a pandemic.
“I have nurses reaching out to me — ‘Can you give me the crash course on the ventilator? Can you help me?’” said Andrea Tuma, a respiratory therapist who works at a hospital in Redding. “This isn’t something I can teach how to do in a 30-minute crash course.”
The coronavirus attacks the lungs, and the lungs are the respiratory therapists’ domain. The roughly 110,000 working in hospitals nationwide train for two years to learn how to care for patients on ventilators, but also to help people with asthma, emphysema and other conditions that cause breathing problems.
The pandemic is shining a light on a profession that typically goes unmentioned, with patients often mistaking respiratory therapists for doctors and nurses.
“I’ve never heard them use the word ventilator in the news as much as I’ve heard it in the last week or so, and talking about respiratory therapists in the news was relatively nonexistent,” said Jeffrey Davis, director of respiratory care services at Ronald Reagan UCLA Medical Center. “Now we’re in the news like crazy.”
Respiratory therapists in hospitals respond to “code blue” calls, an emergency alert that a patient isn’t breathing. They might do chest compressions or provide a breathing treatment to a child having an asthma attack. They closely watch patients on life support, adjusting the settings on their ventilators, monitoring their oxygen and blood pressure.
“I like to say anywhere where somebody needs to breathe in the hospital, a respiratory therapist may have to work that day,” Davis said.
The profession was established in 1947, but didn’t begin to grow until the 1970s, when schools offering formalized respiratory therapy training began popping up, said Tim Myers, chief business officer for the American Assn. for Respiratory Care. The median annual salary for respiratory therapists, who are licensed by each state, is about $60,000 nationwide and $80,000 in California, according to the Bureau of Labor Statistics.
Even before COVID-19, there was a shortage looming in the field. The Bureau of Labor Statistics has said there will be a 20% increase in available jobs over the next decade, but large numbers are reaching retirement age.
And in the coming months, respiratory therapists in the United States could be stretched thin by the sheer number of patients who need ventilators.
Who lives and who dies? It’s an inevitable choice doctors face if coronavirus cases keep surging.
Critical care doctors can be supplemented by physicians from other, related specialties, such as emergency medicine, but it’s not as easy to boost the supply of respiratory therapists because of their specialized training.
In the 2015 study, published in the journal Disaster Medicine and Public Health Preparedness, researchers modeled different scenarios for how hospitals could staff up if they needed to care for more patients on ventilators during a public health crisis.
In the most extreme scenario, available beds nationwide increased tenfold and nurses were assigned six patients at a time instead of one to handle the workload. Respiratory therapists were assigned 12 patients at once, instead of a typical four, but that wasn’t enough to ease the shortfall.
“At the crisis capacity level, the number of available respiratory therapists was the key constraining component,” the authors wrote. “Even if bed capacity and some staff capacity could be expanded by including general ward beds and employing the services of noncritical care physicians and nurses, U.S. ventilation capacity would still be limited by the number of trained respiratory therapists.”
In California, nurses and other hospital staff beginning to see COVID-19 patients trickle in say they are terrified that a surge may mean they have to care for patients on ventilators without the guidance of a respiratory therapist. The AARC is promoting videos online showing people how to run the three types of ventilators that are stored in the Strategic National Stockpile and are being distributed to states.
“I could not even tell you what a respiratory therapist does, exactly. But I can tell you that we’d all be toast without one on hand, especially with COVID patients,” said a California Pacific Medical Center nurse, who was not authorized by her institution to speak to the media.
Last week, Gov. Gavin Newsom asked health workers who are recently retired and in training to volunteer to help on the frontlines of the COVID-19 fight. High on the list are respiratory therapists.
Already, respiratory therapists are feeling the effects of the pandemic on their hospitals. The nature of respiratory therapists jobs’ — bedside contact with very sick patients — puts them at high risk for exposure to the virus.
Cynthia Fayne, a respiratory therapist at Lakewood Medical Center, was paged on March 11 to do a breathing treatment for a patient gasping for air. The man had been admitted to the hospital with a fever, sore throat and shortness of breath.
Four days later, Fayne’s boss called to tell her the patient had tested positive for COVID-19. She hadn’t been wearing a mask while treating him , and she had to remove his own mask to do the breathing treatment.
“If you’re standing there with the patient, you’re of course going to inhale what he’s exhaling,” said Fayne, 52. “I had to quarantine my whole household.”
Her husband, brother and mother also had to stay home from work for two weeks due to their contact with Fayne. None of them developed any symptoms, and Fayne returned to work this week, she said.
“Of course I’m kind of worried, but I’m ready to get back to work,” she said.
Rich Kallet, who recently retired after decades as a respiratory therapist at UC San Francisco, said the COVID-19 epidemic will likely be the defining moment of many respiratory therapists’ careers.
For him, it was the AIDS crisis. When he started at the hospital in 1981, the ICU was filled with patients on ventilators who were struggling to breathe, he recalled.
“All we did was just run from room to room to room to just try to keep these poor guys comfortable and adjust their breathing machines,” he said. “That was a terrifying time and I think this is even more terrifying than that.”
Though still difficult to watch people suffer, it quickly became clear to medical staff treating AIDS patients that they could not get sick from the people they were caring for. The coronavirus, however, can be spread through saliva and mucus, putting health workers themselves at risk.
Ten years ago, during the H1N1 flu epidemic, Kallet was adjusting the circuits on a patient’s ventilator when it split open and sprayed him in the face with mucus.
The fear he felt then is likely what younger respiratory therapists are experiencing now when caring for COVID-19 patients: “This could be me — one mistake, this could be me in a couple of weeks.”
Those fears have been exacerbated by a potential shortage of protective gear, concerns that have put even respiratory therapists with decades of experience on edge, said Tuma, in Redding.
“They’re saying for the first time in their career they’re afraid — they’re afraid because there’s a shortage of what we need to do our job,” she said.
Times staff writers Emily Baumgaertner and Harriet Ryan contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.