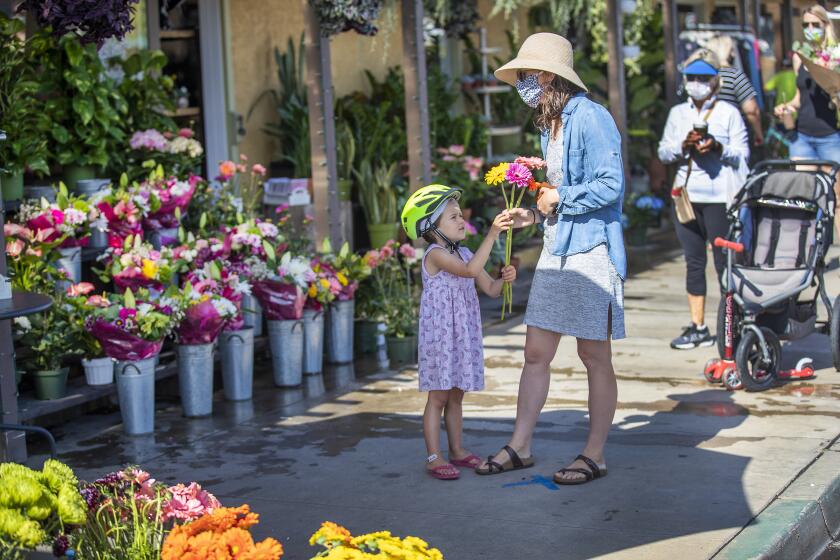L.A. County coronavirus cases top 30,000 as some businesses reopen

- Share via
As the number of new coronavirus-related deaths in Los Angeles County plateaued, officials Friday were easing into an economic recovery plan.
The county reported 883 additional cases of the coronavirus and 51 related deaths, bringing the county’s total to more than 30,200 cases and 1,468 COVID-19 fatalities.
With hospital bed availability and testing capacity reaching recommended levels, some retailers were being allowed to reopen for curbside pickup Friday. Recreational venues such as golf courses and some trails will reopen Saturday.
“We are not moving beyond COVID-19. We are just learning to live with it,” Los Angeles Mayor Eric Garcetti said Friday evening.
Garcetti said the city has launched a series of “working groups” comprised of leaders in industries such as manufacturing, retail, film and television, and higher education to assist in creating guidelines and advising business owners in operating safely during this transition phase.
Additional staff will monitor hiking trails and other recreational areas, but Garcetti noted that maintaining physical distancing will depend on individuals.
In the following weeks, officials will continue to monitor key criteria to determine whether Los Angeles can keep moving forward, including the availability of hospital beds, personal protective equipment for healthcare workers and businesses, and contact tracing.
But the positive steps taken this week don’t mean people won’t get sick, Garcetti said.
“We know people will get sick, we just don’t want them to unnecessarily die as a result,” he said.
Public health officials are urging caution, saying the healthcare system could be overwhelmed by a surge of new cases if people resume their daily activities without taking the proper precautions.
“As these places reopen, we do need to remember the new normal,” Barbara Ferrer, the county’s public health director, said Friday. “When we’re out and about more, we have to behave as if anyone could be infected with COVID-19, and that we also could be infected.”
Parts of California, including Los Angeles County, are allowing some businesses to offer curbside service Friday.
The day before, she pointed to a recent study as an example. The data found that more than 4% of L.A. County adults have antibodies to the virus in their blood, an indication of past exposure.
If 1 million of the county’s 10 million residents stop staying home and 5% of them are infected, that would amount to about 50,000 people infected with the coronavirus who are circulating in the community, Ferrer said. And if even 5% of those 50,000 people become seriously ill and need hospitalization, that would result in 2,500 patients.
“Since on any given day, there’s an average of only 2,000 available beds in hospitals across L.A. County, it could be pretty quick that 2,500 new cases that need hospitalization may overwhelm or start overwhelming our healthcare system,” Ferrer said Thursday.
“These numbers demonstrate that there is a lot at stake as we relax Safer at Home [orders] and that reopening our county, even slowly, only works if we are all really committed to being careful.”
Reopening California begins -- but very slowly, cautiously and under the shadow of a second wave.
She said that it’s crucial for people to do everything they can to practice physical distancing, wear face coverings in public and wash or sanitize their hands frequently. People older than 65 or with underlying medical conditions should continue to stay home unless it’s absolutely necessary, she said.
Garcetti encouraged those who don’t live with their mothers to celebrate this Mother’s Day with a phone call instead, and visit hiking trails and outdoor areas on days that are likely to be less crowded.
“If you’re golfing or hiking...bring your own clubs,” he said. “Pre-pay, if you can. Check trails in advance and bring a backpack to pack up any of your trash.”
Under the California’s reopening plan, counties can apply for a variance to reopen more quickly than the statewide standard, but Ferrer said she does not expect L.A. County to qualify for an exception anytime soon.
“This may apply much more easily for the very small counties that already have seen a significant decrease or may have had no deaths at all to date, but for the larger counties, we will only be able to apply for a variance under these conditions when the pandemic is over,” she said.
As of Friday, more than 214,000 people in L.A. County had been tested and received their results, with about 12% testing positive.
So far this week, L.A. County has reported 4,755 new cases of the coronavirus and 243 people have died. Long Beach reported 23 additional cases and two deaths Friday, bringing the county’s total to 30,319 cases and 1,470 deaths.
The county now accounts for nearly half of all coronavirus cases in California and more than half of all of the state’s deaths.
“This pandemic has not gone away,” Gov. Gavin Newsom said Friday. “We may be exhausted by it, we may be chomping at the bit to get back to some semblance of normalcy, but we had 1,898 new positive cases yesterday... We had 81 individuals and families that were torn apart because of the loss of a loved one.”
Statewide, California has reported more than 62,500 cases of the coronavirus and more than 2,500 related deaths.
The state continues to see a decline in both COVID-19 hospitalizations and intensive care patients, Newsom said Friday.
“We’ve extended for many, many, many weeks a trendline that’s increasingly becoming a headline of stability with modest reductions,” he said, though he noted that some parts of the state have been harder-hit by the virus than others.
As of Friday, there were 1,790 COVID-19 patients in L.A. County hospitals, with 29% in intensive care and 16% on ventilators. The hospitalization rate has remained relatively stable for the past week and a half, Ferrer said.
Officials remained concerned about outbreaks in institutional settings. Public health officials were investigating 356 congregate settings, including skilled nursing homes, correctional facilities, shelters, workplaces and retailers, with at least one confirmed or suspected case. There was a total of 7,373 coronavirus cases in such settings — up 325 from the day before — including 4,633 residents and 2,740 staff members.
The number of institutional residents who died stood at 713 and now represent 49% of all COVID-19 deaths in L.A. County, officials said Friday. The vast majority of them were residents in skilled nursing facilities.
Ferrer said that mitigating the spread of the virus in such settings “is one of our biggest priorities at the moment.”
As of Friday morning, 95 of the county’s skilled nursing facilities had been able to test all residents and staff, and the Department of Public Health was working with the remaining facilities to complete testing, she said. But the effort has faced some barriers, including staffing shortages that make it hard to prioritize both testing and medical care and delays in both receiving test kits and receiving test results, she said.
She said that officials are continuing to conduct routine inspections of skilled nursing facilities and take regular surveys to assess bed capacity, staffing and the availability of personal protective equipment.
The virus’ death toll continued to shine a light on racial and economic disparities, with a rate of 89 deaths per 100,000 people among native Hawaiian and Pacific Islanders and of 18 per 100,000 people among black people, compared with 15.5 for Latinos, 12 for Asians and 9 for white people, Ferrer said.
“These rates are significantly higher than the mortality rate for other races and ethnicities, and although some of the numbers are small, they are still very concerning,” Ferrer said.
People who live in areas with high poverty rates have four times the rate of death from COVID-19 — 29 deaths per 100,000 people, compared with eight per 100,000 people in communities with low poverty rates, she said.
She said that public health officials have been working to address the disparities by opening more testing sites in hard-hit communities, participating in virtual town halls, releasing public service announcements, and ensuring that more racial and ethnic minorities are sampled in a new round of serology testing research.
“Systematic injustices including discriminatory policies and institutional racism have led to the unequal distribution of wealth, resources and opportunities, and this is in fact contributing to the staggering disproportionality we see in the outcomes around COVID-19,” Ferrer said. “Only through a collaborative approach will we see improvements for our tremendously impacted communities.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.