Coming back from COVID-19: ‘Your mind is active, but you cannot talk, you cannot write, you’re stuck inside’
- Share via
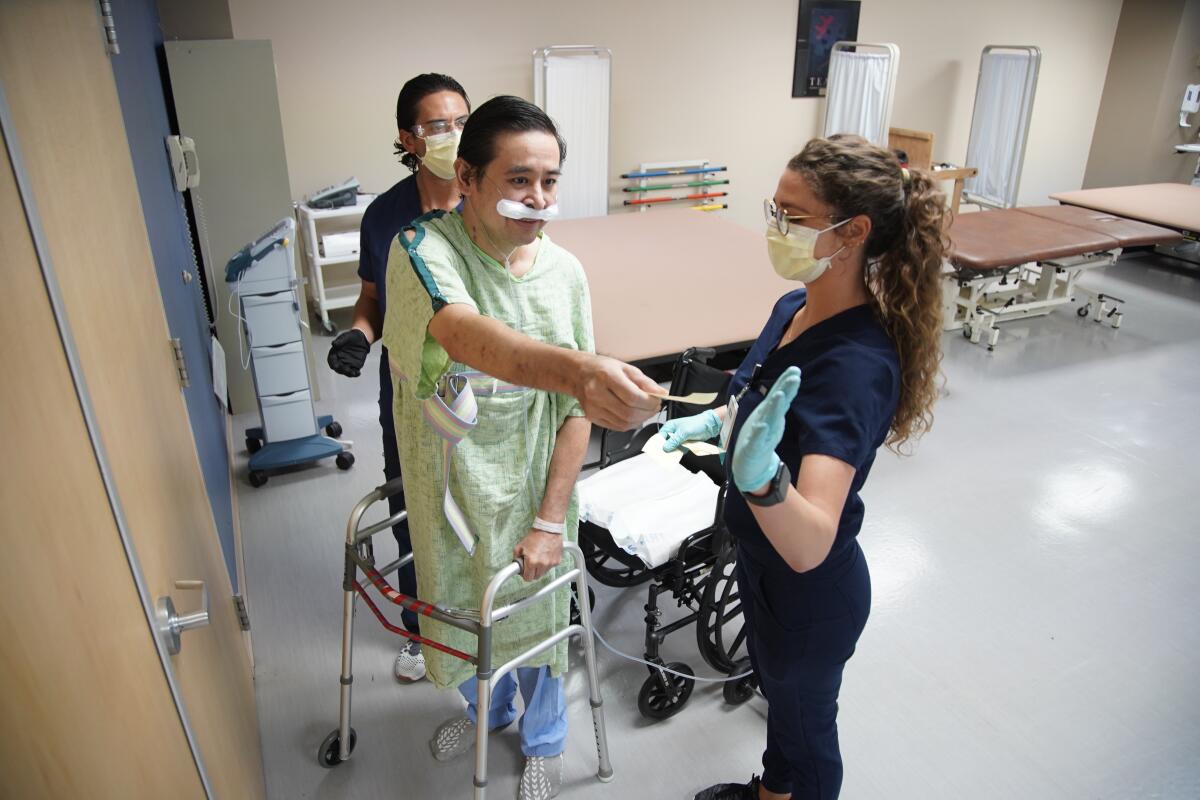
Dr. Jay Buenaflor slowly wound his way through a spacious rehabilitation room on a recent afternoon, reaching high and low to pick numbered yellow Post-It notes from walls, doors and equipment.
He got them in order, and he got them without stumbling, a victory that would have seemed improbable on June 12 when the pediatrician from Brawley, Calif., was admitted to a local hospital after spotting telltale patchy spots on his own chest X-ray. To this day, though he and his family members report taking all possible precautions, it is not clear how he became infected.
What followed was a bare-knuckled brawl with COVID-19. Neither donated blood plasma nor antiviral drugs provided the edge needed to overcome his illness, forcing transport by air ambulance to UCSD Jacobs Medical Center in La Jolla. There, the husband and father of three school-aged children required the help of a special machine to add oxygen and remove carbon dioxide from his blood because his lungs were too inflamed to do the job on their own.
He spent a total of 52 days with his entire blood supply circulating outside his body. It is not an ideal situation for anyone, and especially a man with Type 2 diabetes.
Months of lying in a hospital bed while on a breathing machine stripped away more than 50 pounds, much of it muscle mass. When he awoke on June 30, still in a heavily-medicated fog, he found that just sitting up was an exhausting struggle.
For months now, severe COVID-19 cases like Buenaflor’s tested the outer limits of critical care and rehabilitation, requiring both patients and caregivers to find inner cores of perseverance and creativity in the work of recovering from an illness that sometimes leaves the body depleted of its reserves.
Buenaflor, 48, has been at it for more than two months now.
A senior World Health Organization official says its ‘best estimates’ indicate that roughly 1 in 10 people worldwide may have had the coronavirus.
While it might not look like much to someone who does not know his story, picking sticky notes in the rehabilitation gym at Select Specialty Hospital San Diego represents a level of mobility, of fluidity, of balance and stamina, that seemed perfectly impossible when he woke up in late June.
In fact, having suffered through terrible dreams while sedated, including one terrifying glimpse of his own funeral, Buenaflor said he considered just giving up after regaining consciousness and learning he was so weak he could barely move, let alone stand.
“There was a point where I said, ‘that’s it,’ when I was waking up,” Buenaflor said.
In that moment of defeat, and in many more that followed, memories of his children and wife, Valerie, always appeared, providing a reminder of what he would miss if he just gave up.
“There is always that spark, that ‘just give me one more, just let me see them one more time, that’s it, that’s all I’m asking,’” he said.
With his family as motivation, he began to do the grueling work of relearning how to swallow, how to speak, how to stand and to step. Only after more than a month of such fundamentals were standing and walking remotely on the agenda.
“It’s a humbling experience, but I’m lucky I’m still here,” Buenaflor said.
Just saying that sentence is a victory.
It took two weeks, said Valerie Buenaflor, for her husband to regain the ability to say “I love you” using hand gestures in video calls.
For days after waking up, what was once a sure hand used to writing prescriptions produced only scribbles, regardless of the messages his mind sent.
“Your mind is active, but you cannot talk, you cannot write, you’re stuck inside, that’s the scary thing,” Buenaflor said.
Patients do not eat or drink while sedated, and that experience, Buenaflor said, left him praying constantly for water.
Eventually, he made enough progress to start receiving ice chips. “When they started giving me applesauce, it was like the most delicious food I ever had,” Buenaflor said.
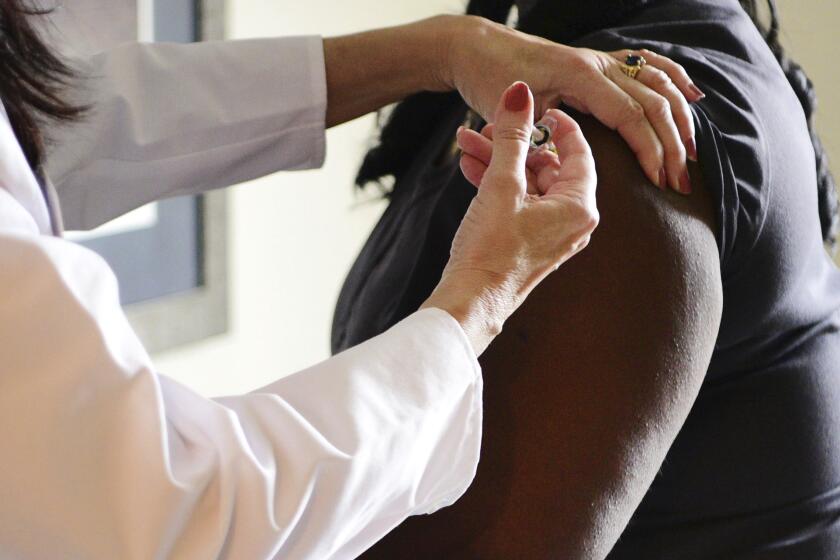
A U.S. advisory panel says decisions about who should get priority for COVID-19 vaccines should focus on disadvantaged areas to remedy racial health disparities.
A key treatment
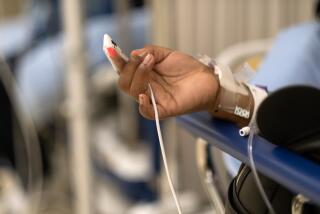
It is unlikely he would have made it to a moment so sweet if not for extracorporeal membrane oxygenation. Often called ECMO, the process requires inserting long tubes called cannulas into a patient’s major blood vessels, making it possible to continuously pump their entire blood supply through a high-tech filter capable of adding oxygen and stripping away carbon dioxide.
It is clear that COVID-19 patients are spending longer on ECMO than was previously common in the world of critical care.
A recent study published in the American College of Cardiology found that the median time on ECMO devices for patients with viral pneumonia connected to influenza infection was 10 days compared with 14 days for patients with COVID-19.
But treatment for much longer than the median is increasingly common. Scripps Health in San Diego has a patient still in intensive care who has been on an ECMO machine for 60 days.
Such long run times, said Dr. Samuel Glickman, a critical-care specialist at Scripps, increase the chances of complications such as internal bleeding and stroke but can also provide enough time for damaged lungs to heal. That damage, he added, is unlike anything he has seen so far in his career.
“In these really sick COVID patients, it’s more profound than anything I’ve ever experienced,” Glickman said. “I can’t think of anyone before this time that got this sick for so long.”
Because ECMO keeps the blood in good condition, it is not technically necessary for patients to breathe. But the human instinct to draw another breath is insatiable and, while patients are sedated, pulmonologists and respiratory therapists must manage mechanical ventilator settings to provide the sensation of breathing without allowing such deep breaths that the lungs are stressed. The whole point, after all, is to give them enough of a break that they can heal.
But such long times receiving such an invasive treatment create their own rehabilitation challenges.
Critical-care teams do what they can to get their patients moving as soon as possible, starting with simple movements of hips, wrists, ankles and upper extremities while patients are still in bed. Eventually, patients will be helped to stand briefly while the ECMO cannulas are still inserted, pumping blood out of the body and returning it at a rate of 4 liters per minute.
Given that the average human contains only 5 liters of blood, this is nervous work. A dislodged cannula would quickly be fatal. At first, standing patients up on ECMO was nerve-racking, but the experience has become less so with practice and consultation with colleagues at UC San Diego.
“We’re able to kind of prove to ourselves that you can safely achieve a decent amount of movement as long as you’re taking the appropriate precautions,” Glickman said.
More than 1 million have died from COVID-19 worldwide, with the numbers continuing to climb.
On the move
Buenaflor experienced this early-up routine at UCSD Jacobs Medical Center where, surrounded by healthcare workers in protective equipment, he was able to briefly stand on July 3 with ECMO in place and running. Valerie, who nervously watched the process live over a video link, said she watched her husband, whom she had been unable to visit in person, stand and step in place while holding onto a walker for about 10 seconds.
“When he made eye contact with me, he motioned for a writing utensil, but couldn’t write,” she said. “But that day was a great day altogether, to be able to see him in motion. It was just a little bit, but it was a lot for everyone.”
Nearly two months later, on Aug. 25, Buenaflor was admitted to Specialty hospital in Hillcrest.
Over the last month, Select’s physical therapists have gradually increased his activity levels, recently moving him from high-flow to low-flow supplemental oxygen.
It is the kind of work that takes infinite patience. Setbacks are common and gains can be so small they’re almost imperceptible.
Dr. Samuel “Buddy” Hammerman, chief medical officer for Select’s long-term acute-care division, said his organization’s 98 such facilities across 28 states have collectively worked with about 3,000 COVID-19 patients recovering from long hospital stays.
Making progress when deficits are initially so great, he said, requires a “slow grind” mentality that accepts the reality that there will be setbacks.
“The slow grind is to keep working with the patient even though there will be some patterns of disease that will come and go,” Hammerman said. “Our persistence is critical.”
It is a journey that is particularly exhausting for families.
Valerie said she has been allowed to visit her husband just once since June 12, and has otherwise had to make do with video visits. None of the couple’s three school-aged children — 10-year-old twins Victoria and Jorja and 9-year-old Catherine — has been able to visit their father’s bedside because of no-visitors policies that have continued since the spring.
And the stress has not been limited to Jay Buenaflor.
A nurse practitioner who works with her husband in the family practice, Valerie recently picked up her father from the Windsor Gardens skilled nursing center where he convalesced after being admitted for COVID-19 treatment on June 25. As her husband was being flown to San Diego for advanced treatment, her father was being admitted.
The family has done what it can to be as close as possible, driving all the way from Brawley to stand on the sidewalk in front of Select hospital, texting a picture of themselves just outside with the message “that’s as close as we can get to you.”
It is not lost on the man just a few floors up. His eyes welling up, he said not being able to be in the same room with his loved ones has brought the greatest anguish of all.
Once he finally makes it home, he said, family will come first. Days of leaving for work before his daughters wake and returning after they are asleep are over.
“A lot of things we can disregard, but that’s the most important thing,” he said. “Sometimes we work too much, so we disregard the most important things.”
Sisson writes for the San Diego Union-Tribune.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.