The mental health effects of living with long COVID
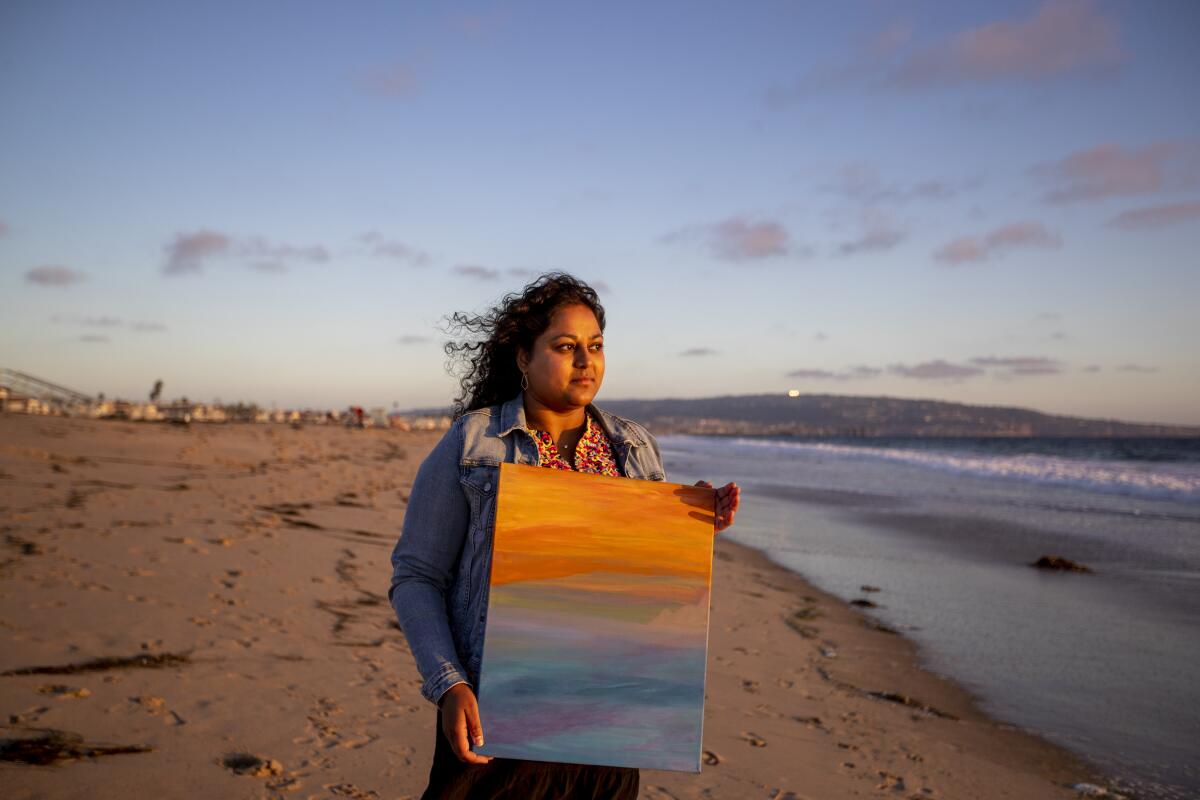
- Share via
I go to the Strand at Hermosa Beach each week and take in the fresh air. Most weeks, I get there and the sun is setting, the sky is an orangish-purple-pink Creamsicle color and the clouds are fluffy. The predictability of this place calms me: the salty air, the sounds of rushing waves, the pitter-patter of the runners, seagulls chirping and the wind dancing on the sand. My visits allow me to have a clear slate for the week and reflect on the progress I’ve made mentally and physically.
About 2½ years ago, I started showing symptoms of COVID-19. But unlike my friends and family members who bounced back from the infection, some of my symptoms continued. It would take dozens of doctor’s and medical appointments to confirm that I had long COVID.
I am a data journalist at the Los Angeles Times and have a deep appreciation for spreadsheets, so my inclination was to track my symptoms.
My planner became a living document in which I detail the good days and the bad using color-coded dots to denote how I am feeling. I used to take an even more comprehensive approach, tracking in a spreadsheet every time I had shortness of breath, my blood pressure dropped or I lost my voice. The reality is, although the note-taking was helpful for taking to doctor’s appointments, the daily data collection for a year wore on me.
How To Save A Life
Pandemic stress, traumatic events and economic uncertainty have upended our world. This series aims to make the cascade of threats to your mental health a little easier to manage.
I wanted to believe that my meticulous data keeping would result in answers from my doctors, a precious “aha” moment that every person with a rare disorder longs for. But by the late summer of 2021, I felt completely overwhelmed with test results, research I came across in my long COVID support group and the reality that no one doctor has a perfect solution for dealing with my symptoms.
The Times is publishing a series of personal essays by people who have all taken different approaches to mental health challenges.
There were days when I had to make calls to get the earliest available appointments, do interviews, go to one or two doctor’s appointments and analyze data, as well as manage my day-to-day life. The doctors kept saying, “We just don’t know anything yet” and “Let’s try this new medicine, but we’ll have to monitor you for two to three months.” That, on top of the news I was covering every day, made me feel as though I was wading deeper and deeper into the dark ocean.
My doctors told me if I didn’t schedule a break, my body would take one for me. So I took a step back from work and said “yes” to taking care of myself. I am very fortunate to have a supportive employer and family and friends and the financial means to go on leave. Rest is crucial after COVID, but unfortunately the systems in this country don’t support mental health well or the physical health needs of folks who need it the most. My leave allowed me to focus on my health and only my health, instead of trying to juggle five things at once.
I realized that, as much as I enjoy data collection, it was time to ditch the spreadsheet of my personal symptoms and shift my focus and energy and just be kinder to myself.
Column One: Being a COVID long hauler has taught me to be fearless, push back and take lots of notes
More than one year after Sandhya Kambhampati was diagnosed with COVID-19, she shares her story as she continues to recover.
I swapped my spreadsheet for an Apple Watch and spent more time outside, focusing on the gains I could make during walks — each day a little bit longer and more challenging. It freed up my brain space to think about what I really enjoy doing. I started to paint during my leave to still use my creative side, especially since I was not writing much. At first, it offered an escape on my worst days, but over the last few months, it has developed into much more.
Painting allows me to express myself in a way that reporting, writing and data analysis doesn’t. It is the one space in my life where I don’t have a deadline, a color palette I must abide by, or a set routine I need to follow. Often my paintings are of the cotton candy clouds I see at the beach at 7 p.m. In a space of uncertainty, painting sunsets allows me to have a feeling of normality and calmness. These moments let me leave my body just for a minute and focus on the wet paint, bright pink hues and take me back to sitting in the sand, watching the horizon and ocean melt into one another.
If you have long-term symptoms of COVID-19 or any other condition, navigating the healthcare system can be rough. Tips for getting the care you need.
Painting also allows me to find balance and the resilience to keep helping others. Along with shifting my personal data tracking, I’ve also shifted from tracking daily coronavirus cases to doing longer interviews with other long COVID patients. I’m able to empathize with a whole pool of younger people, like myself, who are faced with learning to live with a chronic illness much earlier than they imagined. Although I enjoy doing the interviews, some of them remind me of my early days of trying to get the care I needed and leave me wanting to do something more to help these people. On these days, painting gives me a place to release the medical trauma that people share with me and keep going.
And though my symptoms are tapering off, I’m still pacing myself and allowing time to paint, even if I’m not at my worst. There’s nothing quite like peeling the plastic off a new canvas, squirting a little glob of acrylic paint onto my palette and letting the brush glide across, capturing another sunset.
The L.A. Times wants to hear from long haul COVID-19 patients in California and their caregivers about how they’re navigating the challenges of their illness.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.