Timeline: How long until the COVID-19 vaccine gets to the general public?
- Share via
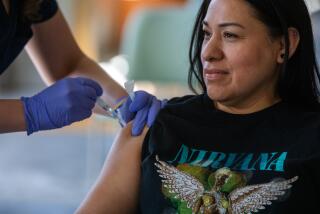
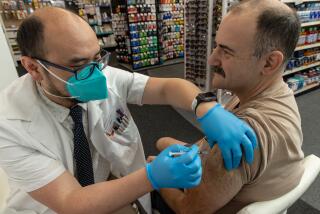
Now that the federal government has given emergency authorization for the first COVID-19 vaccine, how long will it take to get it to the general public?
Many details are still being worked out, and how the vaccine will be distributed across California will depend on state and federal guidance.
But experts say it will probably be spring, and possibly summer or even fall, before the vaccine is available to healthy people who are not essential workers or in other high-risk groups. The first batch of doses will go to front-line healthcare workers with direct exposure to the virus and residents of long-term care facilities, followed by other specific at-risk groups.
Here is what we know about the California timeline.
First round, in the coming days
The first doses are expected to be given to healthcare workers who are at direct risk of exposure to the coronavirus. Residents and staff at skilled nursing facilities and other long-term care settings will also be at the front of the line.
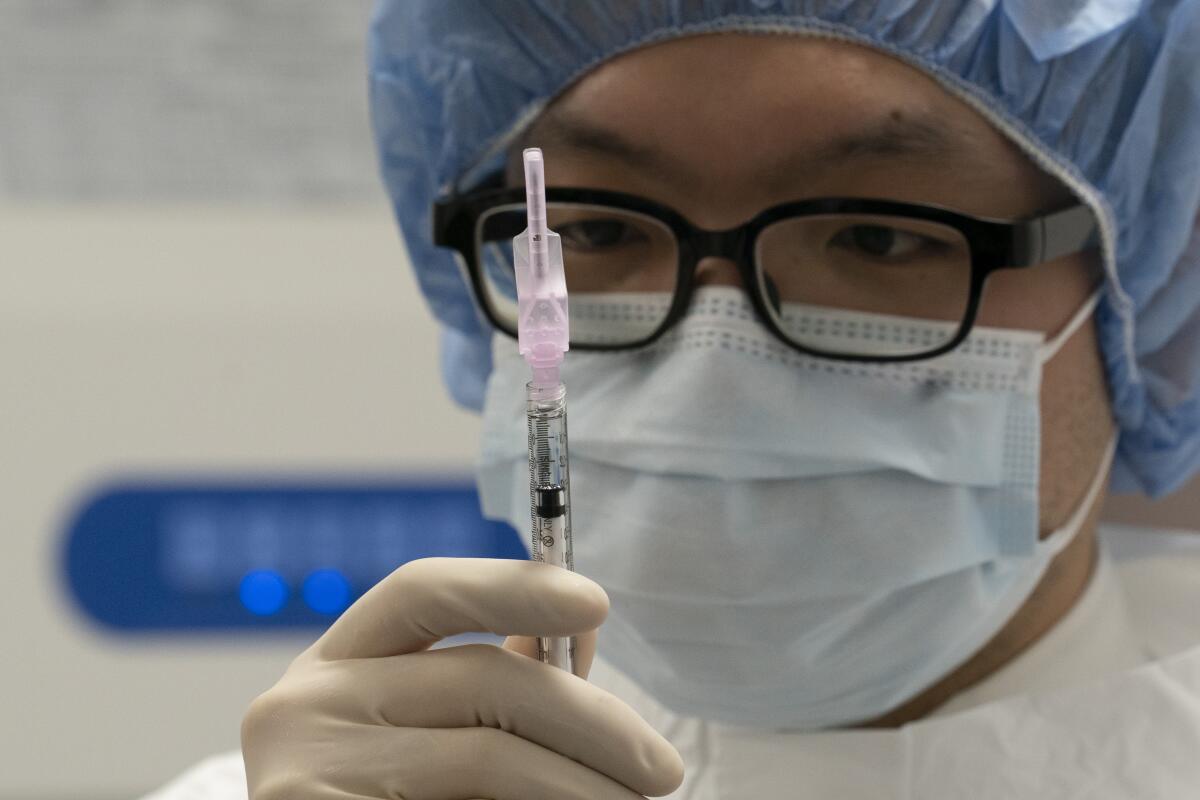
California has an estimated 2.4 million healthcare workers. The state’s first shipment of vaccine from Pfizer will contain about 327,000 doses.
U.S. officials say the nation’s first COVID-19 vaccine will begin arriving in states Monday morning, three days after FDA emergency approval.
“You can do the math and see we won’t get beyond that high-risk group even with the initial allotments we are supposed to receive,” said UCLA epidemiologist Dr. Timothy Brewer.
Dr. Robert Schechter, a California Department of Public Health medical officer, told a vaccine advisory panel Wednesday that the initial 327,000 doses are “likely to end up largely in hospital settings.” If the FDA provides emergency authorization for Moderna’s vaccine soon, California could receive 2 million or more doses of the two vaccines “by the end of the month, and then followed by more,” Schechter said.
Los Angeles County expects to receive about 84,000 vaccine doses early next week, said Dr. Paul Simon, chief science officer for the county Department of Public Health. The doses will be shipped from Pfizer to nine medical facilities with ultra-cold freezers that can keep the Pfizer doses at the required temperature of minus-70 degrees Celsius.
From there, the doses will be distributed to 83 acute-care hospitals, Simon said. Not all employees at those hospitals will receive immunizations in the first shipment, L.A. County Public Health Director Barbara Ferrer told county officials earlier this week.
“The supply of vaccine is expected to be limited, while the need will be high,” she said.
More doses in the next few weeks
If emergency-use authorization for the Moderna vaccine comes this month, L.A. County will receive about 240,000 to 250,000 doses of it and the Pfizer vaccine — the week of Dec. 21. An additional 150,000 doses will arrive by the end of the month, Simon said.
Those doses will be used to immunize more acute-care hospital workers, as well as some staff and residents at skilled nursing facilities, Ferrer said.
L.A. County has an estimated 240,000 workers at acute-care hospitals, as well as 30,000 emergency medical workers, 70,000 long-term care healthcare workers and staff, 34,000 residents at nursing homes and 64,000 residents at other long-term care facilities, according to the county Department of Public Health.
That’s a total of about 438,000 people who would each need two shots — or about 876,000 doses.
The Pfizer vaccine doses need to be administered at least three weeks apart; the Moderna doses, four weeks apart. Someone who receives a first dose of the Moderna vaccine cannot complete the course of immunizations with a second shot provided by Pfizer, or vice versa.
The doses that arrive in December will all be first doses, Simon said. He said the county has been told by federal officials that enough vaccine will arrive in January to fulfill the second-dose requirements.
As more doses arrive, the county will continue to widen the scope of immunizations to include healthcare settings such as psychiatric hospitals, community health clinics and dialysis clinics, as well as health workers who face a higher risk of COVID-19, including emergency medical technicians and community health workers.
Immunizations for residents and staff at long-term care facilities will be delivered through a federal partnership with CVS and Walgreens, Simon said. If that partnership is not finalized in time, the county will use “strike teams” that will begin the immunization process, Ferrer said.
Future rounds in early 2021
Once medical professionals get the vaccine, officials must determine which essential workers will get the vaccine next.
California officials have not determined the order of vaccinations for other essential industries. Trade groups and labor unions are actively lobbying for earlier slots for their members working in law enforcement, agriculture, meatpacking, dentistry, child care, schooling and many other sectors.
“There’s a lot of haziness about how you would define an essential worker,” Simon said. “That’s a very broad group.”
There has also been a push to get the vaccine to people with health conditions that make them especially vulnerable.
Some county leaders have advocated for prioritizing people in jail, where the virus can spread quickly in crowded conditions. They also expressed concerns about ensuring that communities of color have equitable access to the vaccine. Early in the pandemic, when the county first set up its COVID-19 testing sites, those communities did not have adequate access to testing — in some cases none — even as their residents were being hardest hit by the virus.
County Supervisor Hilda Solis has suggested the county use libraries, clinics and other community sites for vaccinations. Supervisor Janice Hahn asked the county to explore schools as vaccination sites, which L.A. schools Supt. Austin Beutner supports.
Ferrer said in a recent report that, at least at first, using schools as vaccination sites might not be doable.
General public in spring, summer or fall
Brewer, the UCLA epidemiologist, said that the FDA giving emergency authorization to a COVID-19 vaccine would be an “important step forward,” but he cautioned against regarding it as a sign that normal life is just around the corner.
It’s unlikely the general public would get access to the vaccine until spring or summer, he said. Even with the vaccine, people will probably still have to practice physical distancing and wear masks.
The San Francisco Department of Health said Wednesday that the general population will not have access to the shots “until the vaccine supply is no longer limited,” which is likely to occur in the summer or fall.
“If I were planning a wedding for next summer, I would plan it in a way so that everything is cancelable,” Brewer said.
It may be best for activities like nonessential travel, including vacations abroad, to wait until after the summer — or be planned with fully refundable tickets — depending on the information to come out of ongoing studies of the virus and vaccines.
International trips could still pose risks, Brewer noted, since other countries will need time to build up their own vaccination programs, supply chains and infrastructure, particularly cold storage. He said, though, that the U.S. could reach herd immunity with around 60% to 70% of the population vaccinated by mid- to late 2021.
“I’m optimistic we will have a better Thanksgiving and Christmas next year than we did this year.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.