One L.A. County hospital ICU is operating at triple its capacity amid COVID-19 surge

- Share via
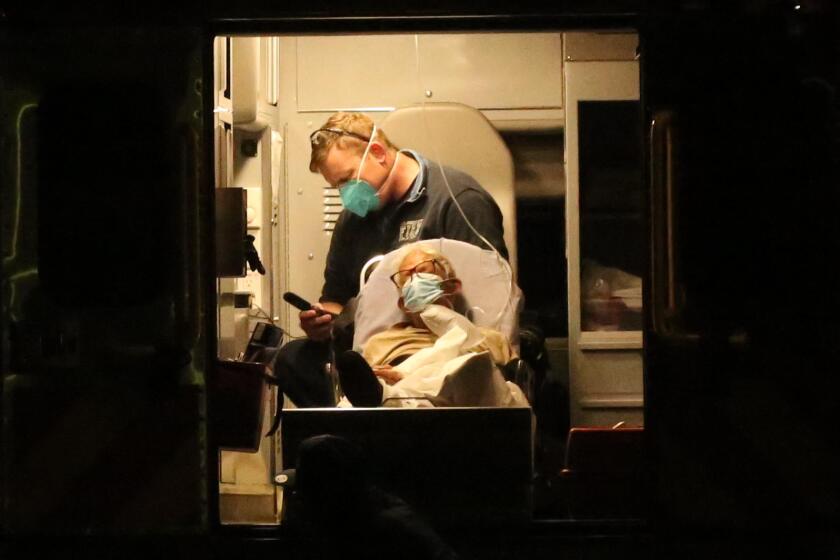
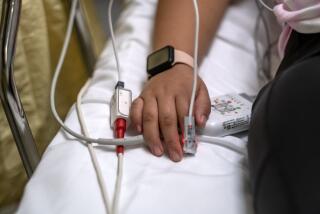
While new COVID-19 hospitalizations have leveled off recently in Los Angeles County, many medical facilities remain overwhelmed. The intensive care unit at one hospital in the South Bay, Memorial Hospital of Gardena, is at 320% occupancy, officials said Wednesday.
The 172-bed medical center has been in various levels of “internal disaster status” since March, and the latest coronavirus surge is manifesting in alarming but increasingly familiar ways — including shortages of home oxygen supplies that are delaying the discharge of many COVID-19 patients and keeping beds occupied.
Demand for oxygen within the hospital has skyrocketed as well, according to hospital spokeswoman Amie Boersma.
“Bulk oxygen delivery has gone from one time per month to every three days and narrowing,” Boersma said in an email. “We must monitor every single day.”
But it is staffing shortages that are presenting the greatest challenge. In a region besieged by COVID-19, “it remains very difficult to find enough ICU nurses,” Boersma said, adding that the hospital is seeking traveling nurses from around the country and has also requested nursing resources from the National Guard.
The state has seen morgues filled, hospitals overwhelmed and oxygen in short supply. That is beginning to change, but it’s far from clear whether California is fully rebounding.
While the hospital awaits extra assistance, it has implemented a team structure that enables staff from closed departments, such as same-day outpatient surgery, to help ease workloads and allow ICU nurses to focus on the most critical tasks.
The hospital is also using advanced registered nurse practitioners and physician assistants to supplement the 10-bed ICU and emergency departments and provide “another set of hands and eyes,” Boersma said, along with hiring final-year nursing students to serve as nursing assistants.
Nearly two dozen patients requiring intensive care are also being treated on the telemetry floor and in recovery rooms, she said.
And although ambulances with critical advanced life support patients are being diverted because most would require ICU admissions, Boersma said the request for diversion can only do so much.
“When the majority of hospitals are on ALS diversion, nobody is on diversion,” she said.
L.A. County hospitals have reported an average of 750 to 800 new COVID-19 hospitalizations a day — an astonishing number that has largely remained steady since Christmas Eve. The count has led ICUs to be effectively over capacity, and hospital morgues are so full that the National Guard has been called to help move bodies to the county coroner’s office until funeral homes and mortuaries can work through the backlog.
There are still fears that new hospitalizations could rise yet again, a result of transmission over the winter holidays. Should that happen, hospitals across L.A. County may need to ration care, activating teams of triage officials who will have to decide which patients get critical care nurses, respiratory therapists and access to ventilators, and which patients are given palliative care as they die.
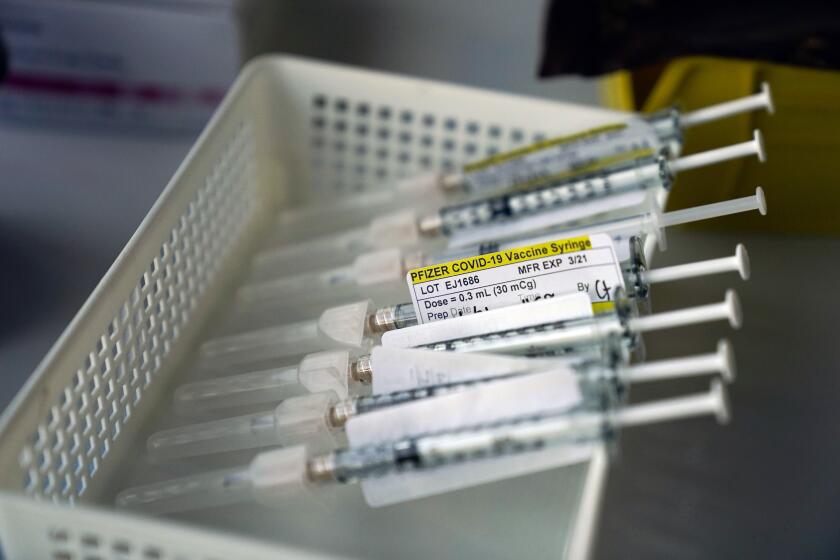
Wait times for vaccines still could last weeks as counties struggle to keep up with demand.
Dr. Christina Ghaly, the L.A. County director of health services, said that hospitalization numbers have leveled off somewhat in recent days — at just below 8,000.
While not increasing at the rapid rate seen earlier in the surge, “they have leveled at a rate that is really not sustainable,” she said during a briefing Wednesday. “This high plateau does not leave enough open beds to care for patients.”
That’s especially the case, Ghaly said, because the county has yet to determine the full ramifications of potential post-holiday exposures. Any increases in transmission, she warned, “would be absolutely devastating to our hospitals.”
“For there to be any meaningful relief for healthcare providers, we need a swift and significant decline in hospitalizations for a period of one to two months at a minimum,” she said.
The county is still reporting an extremely high number of new infections — more than 15,000 a day, on average — and officials say a portion of those testing positive will, invariably, require hospital care two to three weeks later.
As of Tuesday, the most recent day for which complete data from the state are available, there were 7,906 coronavirus-positive patients hospitalized in L.A. County, with 1,699 in intensive care.
Though both those figures have remained relatively level, or even decreased slightly, Ghaly emphasized they remain “unprecedented in the course of this pandemic in L.A. County, and everyone should continue to be concerned about what could happen” if they keep going up.
Any optimism also needs to be couched by the reality that post-holiday transmission remains unclear, she added.
“If our case numbers continue to be this high, and even go up some, that bodes very poorly for the hospitals,” said Barbara Ferrer, L.A. County’s public health director.
Unless conditions improve, Ferrer said it’s possible the county will pursue further restrictions — particularly given the looming threat posed by the new variant of the coronavirus that was first detected in the United Kingdom and is considered to be even more contagious.
“We are considering all options at this point,” she said. “We are very, very worried about the continued high number of cases and feel like there really is not a huge window here to try and get the surge under control.”
The stakes, she said, are literally life and death for many — and all Angelenos must redouble their efforts to protect themselves.
“Do it as if your life or the life of a loved one depends on it,” she said. “Because it just may.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.