Delta variant likely to bring a fall and winter of masks, vaccine mandates, anxiety

- Share via
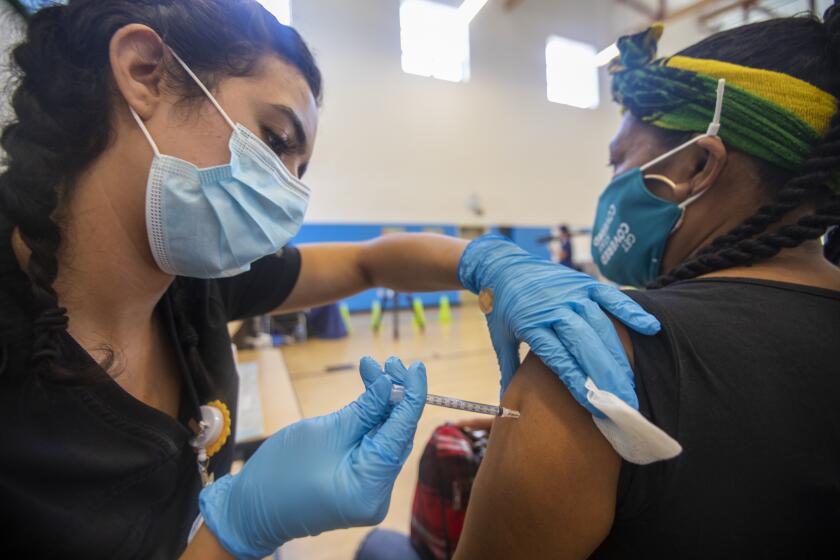
The rise of the Delta variant has upended previous optimistic projections of herd immunity and a return to normal life, with many health experts believing mask mandates and tougher vaccine requirements will be needed in the coming months to avoid more serious coronavirus surges.
While there are promising signs that California’s fourth COVID-19 surge may be starting to flatten, the fall and winter will bring new challenges as people stay indoors more often and vaccine immunity begins to wane.
The rapid spread of Delta among the unvaccinated — and the still relatively small number of “breakthrough” cases among the vaccinated — shows that significant increases in inoculations will help stop the spread. In fact, officials are now preparing to provide booster shots to those who already got their first series of vaccinations, saying the extra dose is needed to keep people protected.
Still, “the vaccines themselves are not going to likely be sufficient. And during times of increased transmission, we’ll need other tools available to protect all of us — and particularly those who, at this time, can’t be vaccinated, like our children,” said UC San Francisco epidemiologist Dr. Kirsten Bibbins-Domingo.
California is in a better position than other states because of relatively higher vaccination rates, and there is little appetite for a return to stay-at-home orders. But in settings where more people gather, strategies that can be used to keep COVID-19 controlled include ensuring people are either vaccinated, have a recent negative coronavirus test or both, Bibbins-Domingo said.
“There will be a time when we have our masks off again as transmission goes back down. But I think we’re going to have to be prepared that if we’re in an environment when there’s more virus around, that it is sensible that we have another layer of protection — and that will be masks,” Bibbins-Domingo said. “And I don’t think we’re going to be totally throwing our masks away anytime soon, frankly.”
The increase comes as a growing list of municipalities, businesses and venues are moving to require the shots for employees and, in some cases, customers.
Policies like mandatory masking and requiring vaccines or regular testing in workplaces “are going to be very important if we are ever going to get over this pandemic,” said Dr. Robert Kim-Farley, a medical epidemiologist and infectious-diseases expert at the UCLA Fielding School of Public Health.
It was once thought that as soon as 70% to 85% of a population was vaccinated, communities would reach a high enough level of herd immunity that the threat of COVID-19 would be mostly behind us. Now, “that’s out the window,” Bibbins-Domingo said, and computer models suggest the coronavirus will be with us for the foreseeable future. “Almost certainly, we’ll be dealing with it this winter.”
How long the pandemic will last depends on any new variants that emerge, the ability to adapt the vaccines to them and temporary measures that may be needed to tamp down surges, Bibbins-Domingo said.
There are several key factors that have altered what we previously understood about COVID-19 and underscore just how far off the end of the pandemic still is.
The first is the emergence of the Delta variant — at least twice as transmissible as the previous dominant variant, Alpha, and capable of producing a viral load up to 1,000 times greater in the upper throat.
“The big challenge with Delta is that it’s so much more transmissible than the original strain. ... And really, this is possibly an unprecedented change in terms of the amount of the” shift in the so-called R-naught, or the basic reproductive rate of the coronavirus, Shane Crotty, a vaccine researcher at the La Jolla Institute for Immunology, recently told a forum at UC San Francisco.
Originally, a person infected with the ancestral strain of the coronavirus spread it to 2.5 other people on average. But the Delta variant is estimated to spread to five to eight other people. That means that within 10 cycles of transmission of the virus, in a population with no immunity to the virus, instead of fewer than 10,000 people being infected, more than 60 million will be infected, Dr. Carlos del Rio, an Emory University epidemiologist and infectious-diseases expert, said at the same UC San Francisco forum.
This is why vaccine mandates will become more important, especially at places of employment, del Rio said. “I think the going phrase that we’re hearing over and over is: ‘No jab, no job.’ And I think mandates are going to make a big difference,” he said.
Patrons of indoor events of 1,000 people or more will have to verify they either have been vaccinated or tested negative for the coronavirus in the prior 72 hours.
Second, breakthrough infections — in which fully vaccinated people become infected with COVID-19 — are still uncommon but no longer rare. “I think vaccinated persons are much safer than unvaccinated persons, but they’re not completely safe. Breakthrough infections occur often enough with Delta that you will see them,” del Rio said.
While a vaccinated person with a breakthrough infection can transmit the virus to others, he or she is likely to be infectious for a significantly fewer number of days, del Rio said. “And therefore your contribution to transmission is much lower if you’re vaccinated than if you’re not.”
And that’s why wearing masks indoors remains important. Del Rio said many infectious-diseases doctors never stopped masking indoors, even after the U.S. Centers for Disease Control and Prevention said it wasn’t necessary for fully vaccinated people.
Vaccinated people with breakthrough infections have much more mild illnesses because the body is already equipped to defend itself against the virus and likely can avoid lung illnesses or hospitalization, said Dr. Regina Chinsio-Kwong, a deputy health officer for Orange County. But without prior immunity, the virus can lodge deeper into the body and cause more severe illness, eventually making it very difficult to breathe.
In Los Angeles County in April, fully vaccinated people accounted for 5% of all coronavirus cases; by July, they accounted for 30%. But fully vaccinated people, who now account for 55% of L.A. County residents of all ages, continue to be well-protected against hospitalization.
Unvaccinated older adults — age 50 and above — are 12 times more likely to be hospitalized than their vaccinated counterparts, and unvaccinated younger adults are 25 times more likely to be hospitalized than those who are fully vaccinated in that age group.
Federal officials also now say there’s evidence that the effectiveness of vaccines to protect against mild and moderate illness decreases over time. A study published by the CDC on Wednesday showed that vaccine effectiveness against infection for adults in New York in the late spring and early summer declined from 92% to 80%; effectiveness against hospitalizations, however, remained stable at between 92% and 95%.
A preliminary study from the Mayo Clinic that reviewed vaccine effectiveness against infection among 80,000 vaccinated and unvaccinated individuals found that it declined over time — from 76% to 42% for those who got the Pfizer-BioNTech vaccine, and from 86% to 76% for those who got the Moderna vaccine, according to CDC Director Dr. Rochelle Walensky.
There also are reports from Israel and elsewhere that suggest an increased risk of severe disease in people who were among the first to get vaccinated against COVID-19, Walensky said.
That’s why officials signaled a federal plan, pending a review by the Food and Drug Administration, to offer COVID-19 booster shots to fully vaccinated adults for those inoculated with the Pfizer-BioNTech or Moderna vaccines eight months after having received the second dose, beginning Sept. 20. Boosters likely will also be needed for people who received the Johnson & Johnson vaccine.
Decreasing efficacy of the vaccines could mean “we need to start shifting our thinking from eradication and disease elimination in COVID anytime soon to more disease management,” del Rio said.
Unleashing a fast-spreading coronavirus variant on a half-vaccinated population can lead to a vaccine-resistant strain.
Finally, there’s emerging evidence underscoring how relying on a past COVID-19 infection, rather than vaccination, may leave people vulnerable to reinfection.
A study conducted in Kentucky found that among those previously infected with the coronavirus in 2020, unvaccinated residents had more than twice the odds of being reinfected with the coronavirus than people who were fully vaccinated.
And the latest data continue to demonstrate that unvaccinated people are, on the whole, significantly more likely to be infected. In California, between Aug. 9 and 15, unvaccinated residents were being infected at a rate of 51 cases for every 100,000 unvaccinated people a day. That’s more than six times worse than the rate for vaccinated people, which was 7.6 cases for every 100,000 residents.
We look at the science behind the need for COVID-19 booster shots.
Unvaccinated children — some too young to be eligible — are also at greater risk of illness if their families haven’t received their shots. At Children’s Hospital of Orange County, officials have noticed a pattern in which “the children who are hospitalized for COVID are unvaccinated and their families are also unvaccinated,” Chinsio-Kwong said.
Much of the coronavirus transmission among schoolchildren “is not happening in the schools, it’s happening in the house. The biggest risk a kid has is the parents are not vaccinated,” del Rio said.
Teenagers and younger adults are among those least likely to have been vaccinated in L.A. County. While 73% of all county residents 12 and older have received at least one dose of vaccine, only 63% of the youngest adults — age 18 to 29 — are at least partially vaccinated; about 65% of 16- and 17-year-olds are, as are 56% of those 12 to 15.
This pandemic will eventually end, as all pandemics do. But controlling it will be challenging, and how it’s done will likely depend on human behavior, del Rio said.
“You’re going to see societies where the virus is well-controlled [in places like] Japan, where all the kids are going to be in school wearing masks, and they’re not going to have outbreaks. And then you’re going to have outbreaks in states like mine [Georgia], or Tennessee, where you have school districts where kids are not using masks,” del Rio said.
L.A. County Public Health Director Barbara Ferrer said she is in favor of targeted mandatory vaccination policies, particularly in settings where people are at highest risk.
“This is our best tool for not getting back into a horrible winter surge,” Ferrer said. “It’s completely possible for us to end this pandemic, but it’s going to be done because we’re going to get many more people vaccinated.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.