Omicron deaths and cases hit Southern California harder than rest of state
- Share via
The winter Omicron surge hit Southern California harder than any other part of the state, a Times data analysis found, again underscoring the region’s vulnerability.
The data — from Dec. 1, when the state’s first Omicron case was confirmed, through Monday — help paint a more complete picture of Omicron’s rampage throughout California and demonstrate how the pandemic’s pain continues to be unequal.
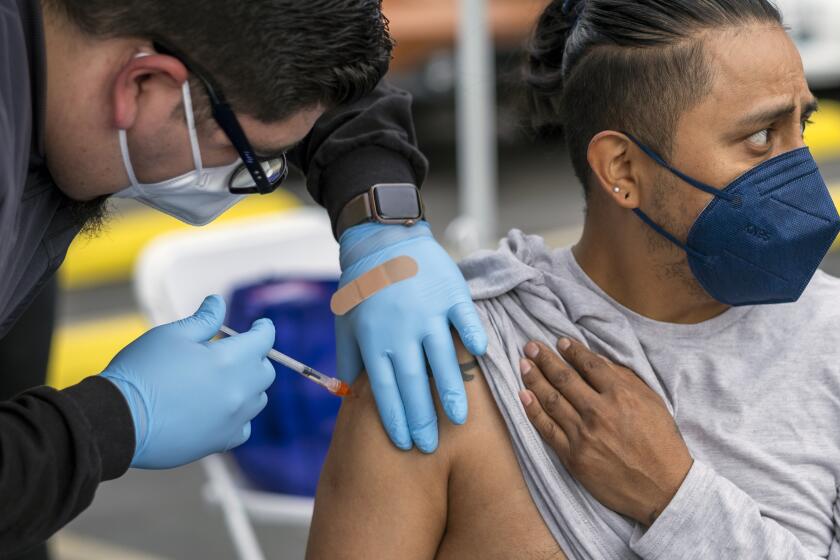
But the figures also lend further credence to what health officials have long maintained: that the surest way to stave off the worst ravages of the coronavirus is through robust vaccination.
The widely vaccinated and boosted San Francisco Bay Area, for instance, noted the lowest hospitalization and death rates in the state during the recent surge by the coronavirus variant, despite having the second-highest case rates.
Conversely, rural Northern California’s death rate was roughly the same as Southern California’s, even though the latter’s case rate was more than twice as high.
Throughout the pandemic, the U.S. has followed Europe by several weeks in waves of cases, and that may happen again, health experts warn.
Boosting vaccination rates, health officials and experts say, is all the more pressing given the widespread relaxation of other measures — namely mask mandates — that had been imposed to help stymie the virus’ spread.
Getting more people to roll up their sleeves is also important given that another wave is already emerging in other parts of the globe.
“None of us want to go back to masking everywhere, restricting travel, restricting workplaces. I think everybody agrees on that goal,” Dr. Robert Wachter, chair of UC San Francisco’s Department of Medicine, said Wednesday during a roundtable hosted by the U.S. House Select Subcommittee on the Coronavirus Crisis.
“The question,” he continued, “is what can we do that allows people to live a life as normal as possible, with as few restrictions and allows our economy to be as open as possible? Clearly, to do that we need to encourage more vaccination, more boosting, potentially another booster may be in our future. We need to allow for more testing and we need to have treatments out there.”
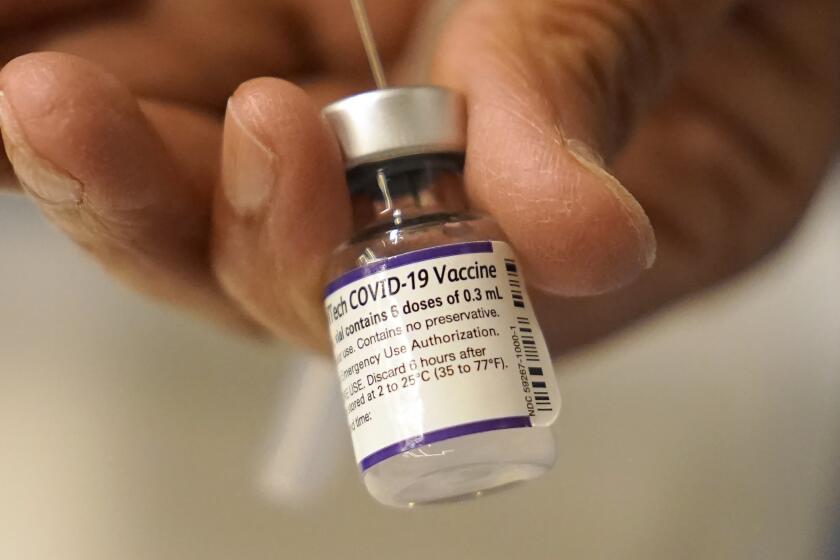
Health officials battle myths and disinformation in convincing people to get their COVID-19 booster shots.
Since Dec. 1, Southern California has recorded 10,103 coronavirus cases per 100,000 people — the highest of the state’s five regions, according to a Times analysis of data from the California Department of Public Health.
Infection rates were 7,714 per 100,000 people in the Bay Area, 7,341 in the San Joaquin Valley, 6,459 in Greater Sacramento and 4,892 in Northern California, data showed.
The state defines Southern California as Imperial, Inyo, Los Angeles, Mono, Orange, Riverside, San Bernardino, San Diego, San Luis Obispo, Santa Barbara and Ventura counties.
While it’s not surprising this region — home to more than half of all Californians — had high raw numbers of cases, the analysis revealed that many counties in the area ranked among the hardest hit in infections, even when counting for population.
Of California’s 58 counties, L.A. had the highest overall case rate during the Omicron surge. San Diego was third; Imperial, fourth; San Bernardino, eighth; Riverside, ninth; Santa Barbara, 10th; and Ventura, 11th.
These high case rates reflect a staggering number of infections. Combined, the seven Southern California counties tallied 2.1 million new coronavirus cases in the last three and a half months — including 1.2 million in L.A. County alone.
When asked about The Times’ analysis Thursday, L.A. County Public Health Director Barbara Ferrer said the findings don’t come as a surprise.
“I don’t think at the beginning of the Omicron surge we appreciated how very contagious this new variant was,” she said. “And I think, in fact, in a community our size, with as much industry as we have, we really do take a very hard hit.”
The case count is larger than the combined population of San Diego, Orange and Riverside counties, and equivalent to nearly 25% of Californians testing positive at some point in the past two-plus years.
The massive caseload was fueled by Southern California’s testing — the most per capita of any region, The Times’ analysis showed. But experts have long noted that official infection counts are likely to be incomplete, as some people may never get screened or have their results disclosed to public health agencies. Exacerbating that issue is the availability of at-home tests, which were widely used during the Omicron surge but are not reliably reported.
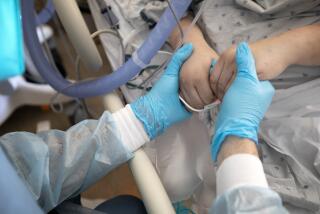
Regardless of the actual count, the sheer enormity of cases had devastating effects throughout the region. More than 7,500 Southern Californians died from COVID-19 — a rate of 32.2 per 100,000 people from Dec. 1 through March 14.
While still the worst in the state, the gap in death rates between Southern California and the four other state regions is not as wide as case rates. Both the San Joaquin Valley (just under 32.2 per 100,000 people) and Northern California (31.7 per 100,000) had only fractionally different death rates. That’s despite their surge case rates being lower (27% and 52%, respectively) than Southern California’s.
Those regions have routinely been the least-vaccinated in the state. Nearly 53% of Northern California residents and 55% of those in the San Joaquin Valley are fully vaccinated, compared with about 64% in Greater Sacramento, 69% in Southern California and 80% in the Bay Area.
Under new guidance, businesses can choose to keep their mask requirement for both customers and employees.
Booster uptake has also been far slower in those regions. The proportion of boosted residents is 22% in the San Joaquin Valley, 26% in Northern California, 33% in Southern California, 34% in Greater Sacramento and almost 50% in the Bay Area.
The Bay Area was the most insulated against severe health outcomes during the Omicron surge. Its death and hospitalization rates were the lowest of any region.
Despite being home to almost twice as many people, the Bay Area reported fewer COVID-19 deaths than the San Joaquin Valley during the analysis period: 1,218 compared with 1,470.
“We know that due to our very high vaccine coverage rates, our relatively high booster rates, combined with the fact that Omicron was not as biologically virulent as some of our prior variants, our deaths were not nearly as proportional to case rates as they were in January of 2021. Thankfully, that is the case,” San Francisco Health Director Dr. Grant Colfax told city health commissioners this week.
Yet low vaccination rates are only one factor in coronavirus spread. Health experts have regularly said socioeconomic elements — such as the proportion of residents who live in crowded housing or need to physically leave home to work in a frontline job — can heighten the risk of transmission.
Residents in unhealthier areas, such as those near freeways with dirtier air, also may suffer from higher rates of respiratory disease, putting them at greater risk. More rural or impoverished areas lack the same healthcare resources as wealthier communities, making it more difficult to manage chronic conditions or treat new illnesses.
In L.A. County, all of those societal ills have played a role during the pandemic, Ferrer said.
“We have some of the densest neighborhoods in the entire country,” she said. “We have also many people, an extraordinarily large number of people, who live in communities that are both under-resourced and they themselves are living at or below the poverty level — making it, again, super hard for folks to have the resources that they might need to protect themselves. We’re also an industrial county. We have a lot of heavy industry. We have a lot of manufacturing industry. We have ports.”
That adds up to many residents who had to keep working on site, even during the surge.
“Throughout most of the Omicron period nothing closed here,” Ferrer said. “That had its advantages, kept us on a recovery journey, but also created a lot of exposures for people who work in all of these essential services that were open during the entire pandemic.”
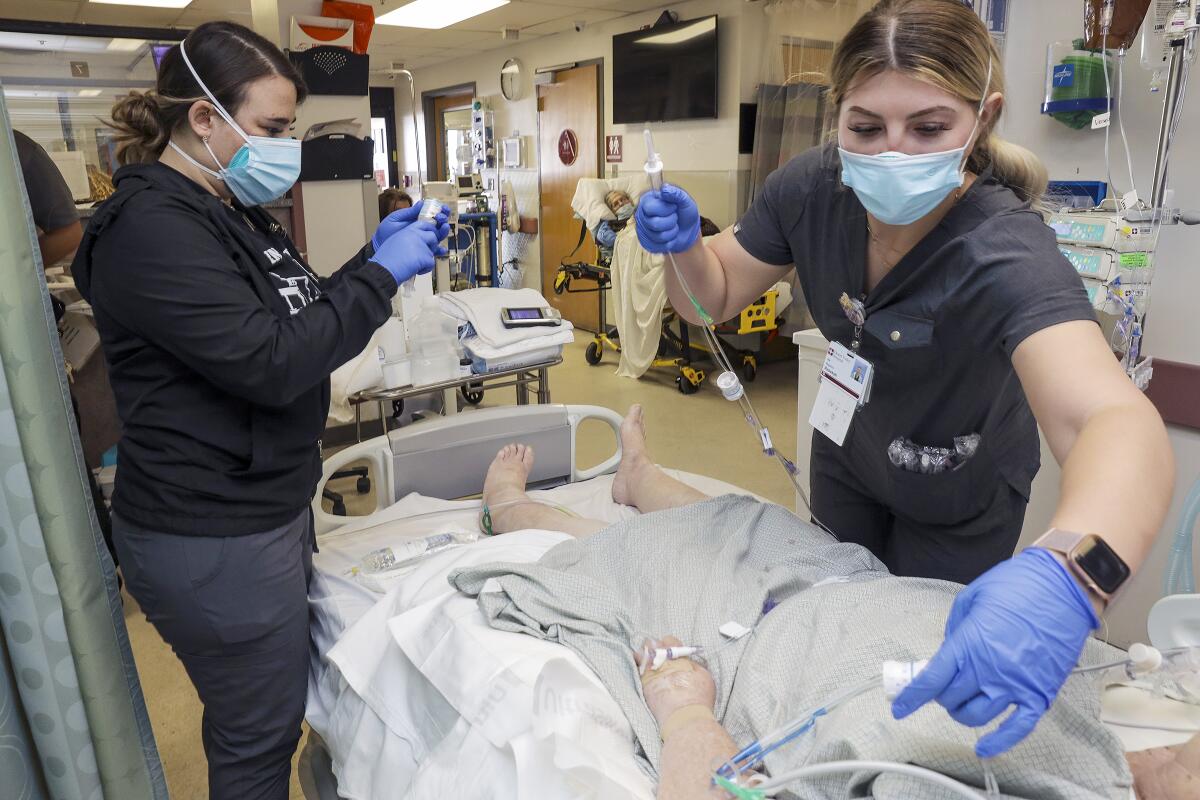
Community clinics, which provide care to poor and uninsured patients, have struggled to hire and hang onto workers as the pandemic has dragged on.
But officials also say vaccines have a clear benefit. While case, hospitalization and death rates rose for both vaccinated and unvaccinated Californians during the Omicron surge, the increases were particularly large for unvaccinated residents, and their relative risks remain higher even as the latest wave wanes, state data show.
According to the most recent available figures, unvaccinated Californians were five times more likely to get COVID-19, seven times more likely to be hospitalized and almost 15 times more likely to die from the disease than those who were fully vaccinated and boosted.
While precautions such as avoiding crowded situations or wearing masks indoors will afford additional protection, many health officials are increasingly comfortable with those who have gotten all their shots resuming pre-pandemic normalcy.
That rationale is rooted both in science and sociology. Transmission has tumbled since the height of Omicron, and though the protection afforded by vaccines diminishes over time, evidence indicates the shots remain highly protective against severe disease. There’s ample testing supply, and more treatments are available than ever — though those are a bit harder to come by.
What accounts for BA.2’s recent success? It’s not due to an ability to evade the protection of COVID-19 vaccines, a new study finds.
There’s also the simple truth that, after two years marked by at-times stringent restrictions, many residents are eager for a taste of life circa 2019.
While it’s important to keep an eye on emerging trends elsewhere, as well as do everything possible to prepare for potential new surges at home, officials say it makes sense to alter requirements and recommendations as conditions allow.
“Individuals who are vaccinated and boosted are generally very well-protected from severe illness, and now we also have treatments, we have testing, we have other tools that help us to be able to live with COVID,” Dr. Leana Wen, a professor of health policy and management at George Washington University, told the coronavirus Select Subcommittee. “And so, for the majority of Americans, it is possible to return back to pre-pandemic normal — not because the pandemic is over, but while we have this relative lull, with a reduced number of cases, I believe it’s important for us to urge people to resume their lives.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.