First, we stop the dying
- Share via
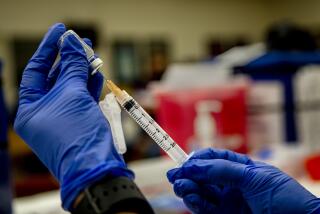
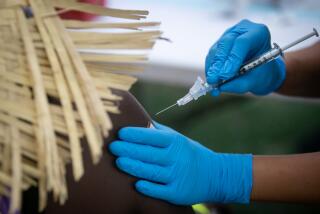
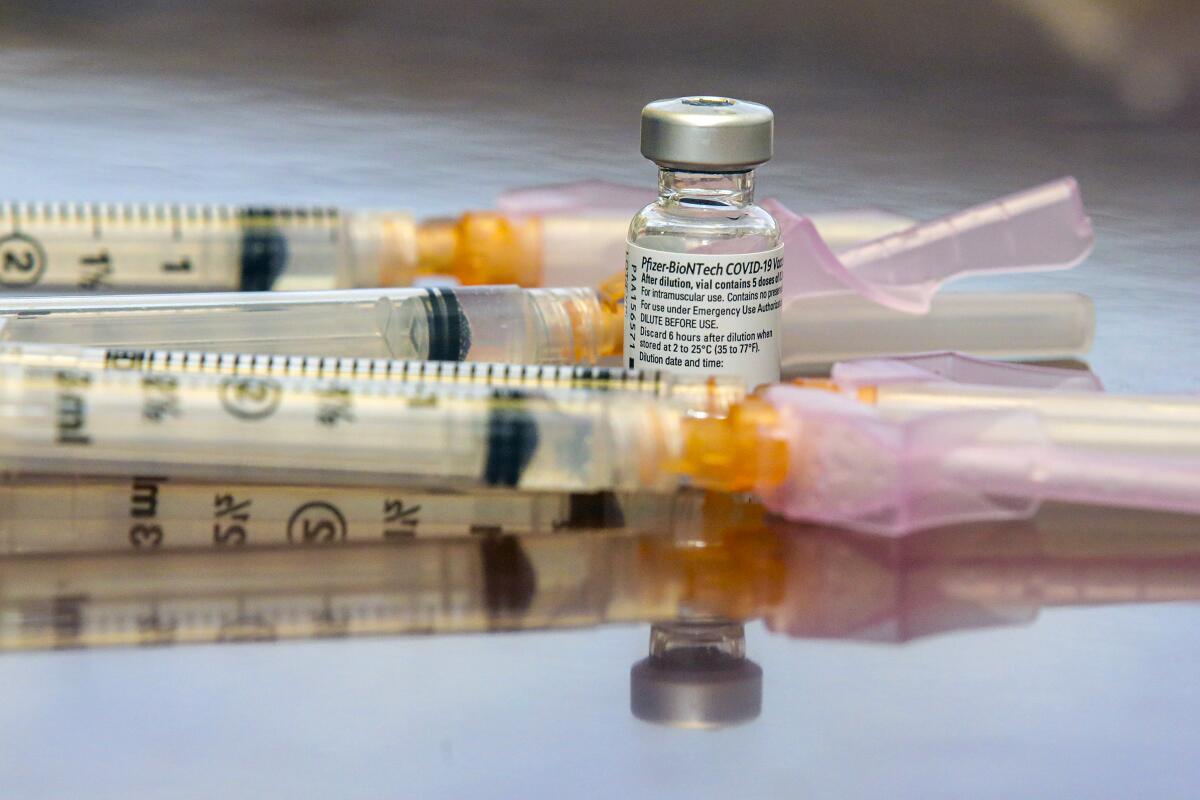
The first batches of COVID-19 vaccine, which arrived last week to much fanfare, have been appropriately reserved for front-line healthcare workers and nursing home staff and residents.
That was an easy call. Healthy nurses, doctors and other healthcare workers are crucially important to keeping hospitals functioning amid the surge of seriously sick COVID-19 patients. Residents of nursing homes are in acute danger, accounting for 40% of the more than the 312,000 COVID-19 deaths in the U.S.
But who’s next? It will be weeks, even months, until there are enough doses of COVID-19 vaccine available to inoculate those in the first phase, accounting for about 2.5 million people in California alone. Nevertheless, the public focus is shifting to who should be next in line.
Everyone seems to have an opinion. Anyone over 65? All essential workers? Uber thinks its drivers should have a place near the front of the line because they provide transportation to healthcare workers. Airline unions argue that aviation workers are essential to the nation and should have the highest priority. Teachers and farmworkers and dentists and meat processors are lobbying for special consideration. And on and on.
We have an opinion, too: Stop the dying first.
Everybody can’t go next. Even if there were enough supplies for the 87 million Americans, and 12 million Californians, working in industries designated as essential, it would require weeks if not longer to reach them all. Meanwhile, people will continue to get sick and die, and COVID-overloaded hospitals will struggle to meet the needs of patients with other life-threatening illnesses and injuries.
Until there are many millions more doses available, the focus should be on reducing death — not reopening businesses or placating influential interests. That means giving priority to those with the greatest risk of dying from COVID and who, because of their living or working situation, are less able to avoid infection.
“This is where we check our biases over who we find more important,” said Nancy Berlinger, a research scholar at the Hastings Center who spearheaded a COVID-19 ethical guide for the healthcare sector. Why? Because so many of those who are dying work and live on the bottom rungs of society.
That includes low-wage “essential” workers in jobs where exposure is highest and people with preexisting conditions that could exacerbate a COVID-19 infection; both groups are largely Black and Latino. Communities of color have been clobbered by outbreaks, as have those living in crowded apartments, group homes, homeless shelters, prisons and jails.
Yet much of the discussion is focusing solely on which broad group of essential workers should go next.
On Sunday, the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices is expected to vote on recommendations that designate certain categories of essential workers for the next phase of priority. Later this week, California is expected to finalize its own proposal to prioritize workers in emergency service, education and child care, and food and agriculture, broad categories that include about 5.9 million people.
Part of the effort to give essential workers priority is to ensure equitable treatment of historically underserved communities, and we appreciate that. These workers too often get short shrift. But not all essential jobs are equally high-risk or have the same level of potential exposure, and not all at-risk people work in essential jobs — and that should be made clear in the guidelines. Protecting the most vulnerable individuals from death, regardless of their perceived value to society or the job they hold, should be a clear and unambiguous priority.
Ultimately, how the scarce COVID-19 vaccine is doled out will be largely in the hands of the clinics and workplaces authorized to distribute them. While these distributors in California will be obligated to follow the state’s guidelines, there’s a risk that the high-priority groups will be defined broadly enough to leave loopholes to be exploited by those with means and connections, who are already jockeying to skip the line.
This is infuriating. We saw how unequal access played out in the chaotic early days of the pandemic, when diagnostic tests were in similarly short supply. It can’t be allowed to occur again. The state needs to set not just the right priorities for vaccination, but the right criteria for deciding who belongs in each group. This is one of the rare cases in which each needle stick is literally a matter of life and death.
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.