Hospitals prepare for wave of mental health disorders among their workers
- Share via
WASHINGTON — Nurse Camille Davis has watched more than 30 patients die of coronavirus infection, and has sobbed while holding her phone close to them so loved ones could say their goodbyes. Her long drives home are filled with worry about transmitting the disease to her 8-year-old son.
“I had a colleague who wanted to quit, it was too much for her, and I told her, ‘We can’t quit. We have to keep working until we get sick,’” said Davis, a nurse at Mt. Sinai Hospital in Manhattan. “That is how we are getting through this. But I wonder what we will be left to deal with when it’s all over. I’m worried I will develop PTSD.”
Hospital administrators say Davis’ experiences are hardly unique, and that is why they expect to confront a surge of mental health disorders affecting physicians and nurses who have battled COVID-19. As many as 20% to 25% of healthcare workers in hard-hit areas, experts say, are likely to develop disorders such as anxiety, depression or post-traumatic stress — a rate similar to what is reported in soldiers returning from combat.
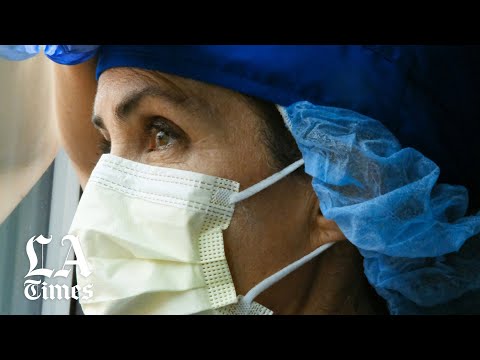
“The degree of stress that front-line healthcare workers are experiencing is extraordinary,” said Dr. Dennis Charney, the dean of the Icahn School of Medicine at Mt. Sinai and an authority on post-traumatic stress disorder. “There is a massive amount of stress that is comparable to a war.”
In their own words, doctors and nurses in New York, the epicenter of the COVID-19 crisis in the U.S., chronicle their experiences.
Mental health practitioners pointed to the suicide late last month of Dr. Lorna Breen as a warning flare. Colleagues said the 49-year-old Breen, an emergency room physician at NewYork-Presbyterian Allen Hospital in Manhattan, took her life after becoming overwhelmed by the volume of coronavirus patients who died on her watch.
“People at these elite medical institutions are talented, disciplined, strong and resilient,” said Dr. Jeffrey Lieberman, the chair of psychiatry at Columbia University Medical Center, where Breen was an assistant professor of emergency medicine. “But everyone has a breaking point. Tragically, in her case, her dedication pushed her past the breaking point.”
Healthcare professionals said the potential for trouble is particularly acute in New York, which has emerged as ground zero in the U.S. for COVID-19, the disease caused by the coronavirus.
Its hospitals have been crushed by an onslaught of severely ill patients. With no proven treatments or cures, physicians and nurses say they have often felt powerless to prevent the sickest from dying. Nearly 14,000 people have perished from the disease in the city, health officials say. During the height of the outbreak a month ago, doctors at Mt. Sinai Hospital were reporting at least 20 deaths a day. Typically, the hospital has one or two.
“The mortality that even veteran clinicians are witnessing has been massive and devastating to healthcare workers,” Lieberman said.
With families barred from hospitals, providers have struggled to maintain emotional distance from their patients. Doctors have been forced to relay final messages from loved ones. Nurses have become comforters — holding their patients’ hands, brushing their hair before FaceTime calls with relatives. Such intimate interactions, psychiatrists said, exacerbate the stress of a patient succumbing to the virus.
Then there is the fear of catching the disease and bringing it home to their families.
“This is very hard on them,” said Dr. Marra Ackerman, a clinical assistant professor of psychiatry at the NYU Grossman School of Medicine. “This pushes against what they would normally do: go into a room, bring a patient a cup of tea, check on a bandage. Instead, they have to limit their time in there to protect themselves, to limit their exposure. They worry about giving this to their families.”
Psychiatrists said doctors and nurses will grapple with such stress for months and years, well after the last coronavirus patients leave their hospitals.
“So a lot of the times in the heat of the battle, that is all you are focused on, your own survival, and the adrenaline is very high and you seem fine,” said Charney of Mt. Sinai. “When it’s over, that’s when the memories start coming back, and PTSD emerges. That is what you worry about, and you have to provide support well after the actual trauma.”
The long-term costs to the healthcare system will be staggering in personal and financial terms, mental health professionals say. Performance will suffer. Doctors and nurses will leave their jobs just when they are needed most. Some will become estranged from spouses and families, or even take their own lives. The healthcare system doesn’t have much slack — it was already shuddering under high rates of stress, depression and burnout.
The frenzy for equipment to fight the coronavirus has led to a chaotic marketplace where states, cities and hospitals have had to rely on middlemen.
Hospital administrators said they are racing to establish initiatives to reduce the severity of such disorders and to identify those who need help. Mt. Sinai Health System is setting up a program to train doctors and nurses to be more resilient, identify those in danger of becoming overwhelmed and provide counseling to those who need it. Other major hospitals in New York City, including those affiliated with New York and Columbia universities, have launched similar efforts.
More than 1.2 million people have become infected with COVID-19 in the U.S., and more than 70,000 have died of the disease.
Doctors and nurses across the country will confront the same kinds of stress when treating patients and providing emotional support even if they don’t endure New York-sized caseloads. The economic toll from lockdowns associated with the pandemic is also fraught with stress. Hospitals, facing a massive drop-off in lucrative elective surgical procedures, have laid off and furloughed staff. Spouses in other fields have lost jobs.
“This is going to cause different stressors at different times,” said Dr. Jessica Gold, a psychiatrist at Washington University School of Medicine in St. Louis who treats healthcare workers. “It’s a whole big package of things that cause stress, and you can’t just pinpoint on a map mortality rates and say, ‘That is where we are going to see the worst PTSD.’”
More to Read
Get the L.A. Times Politics newsletter
Deeply reported insights into legislation, politics and policy from Sacramento, Washington and beyond. In your inbox twice per week.
You may occasionally receive promotional content from the Los Angeles Times.











