California needs nurses. So why is the state about to give up 10,000 prospects?

- Share via
SACRAMENTO — Amid a frantic scramble to open hospitals and increase the number of healthcare workers, California nursing schools are warning state officials that an estimated 10,000 nursing students are in jeopardy of not graduating, meaning they will be unable help evaluate and treat patients amid the coronavirus pandemic.
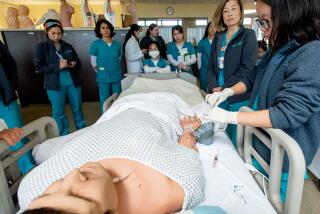
Under state rules, nursing students must spend a substantial part of their clinical education in hospitals, but they are barred from doing so now because of hospital lockdown orders. Unless the state loosens its rules, students set to graduate in coming months will find it impossible to become a licensed nurse.
As a result, public and private nursing schools are pleading with Gov. Gavin Newsom and the state’s Board of Registered Nursing to allow greater flexibility in how students meet their clinical education requirement after many hospitals discontinued training placements because of safety concerns and to focus on the tidal wave of COVID-19 patients.
“I went through 19 months of training and the end is near and everything is coming to a screeching halt,” said Ryane Panasewicz, 27, who attends nursing school at West Coast University’s campus in Anaheim. “Keeping graduating nursing students out of the healthcare system at this time will make problems worse.”

California has been bracing for an onslaught of COVID-19 patients, with Newsom saying this week that the state will need 50,000 additional beds and many additional healthcare workers. With the number of confirmed COVID-19 cases rising daily, nursing schools say the backdrop of their urgent request is clear.
On Wednesday, a Kaiser executive vice president and infectious disease expert said about half of Kaiser Permanente’s San Jose hospital has been filled with patients confirmed or suspected to have the new coronavirus, prompting a need to boost staffing. Meanwhile, California has begun leasing medical facilities, with one in Daly City beginning to accept up to 220 COVID-19 patients this week, which will also require more healthcare workers.
On Monday, Newsom said the state is exploring ways to get nursing students licensed earlier, but no additional details were provided by his administration Wednesday.
From March 1 to March 25, 139 companies in California reported laying off 18,998 employees. That’s just a fraction of the real total.
The Board of Registered Nursing, an appointed body that enforces laws on nursing education and licensure, has not indicated publicly what changes, if any, it is seeking. Michael Deangelo Jackson, president of the board, and Loretta Melby, the board’s acting executive officer, referred questions to a spokeswoman, who declined to comment, saying she expected “more up-to-date information in the coming days.”
“We could use these 10,000 nurses right now,” said Joanne Spetz, an associate director of research at Healthforce Center at UC San Francisco, which produces supply and demand forecasts on registered nurses in the state. “Getting them out the door and practicing is incredibly important.”
The Idaho Board of Nursing last week announced an apprentice program to move nursing students into hospitals and a temporary emergency license for students who are nearing graduation. This month, in response to the pandemic, the Texas Board of Nursing relaxed its rules on how many hours nursing students must work in hospital training rotations.
Critics say California’s slow response is rooted in a lack of urgency on behalf of the state’s nursing board.

“So far, our governor and the California Board of Registered Nursing hasn’t taken any action and we just aren’t getting anywhere,” said Scott Casanover, senior vice president of governmental affairs for West Coast University and American Career College, which operate nursing schools in Anaheim, Los Angeles and Ontario.
“We started appealing to the board three weeks ago saying this will be a huge problem if we can’t graduate nurses,” Casanover said. “There are no more nurses going into the pipeline until we solve this.”
The University of California, California State University and California Community Colleges, which each operate nursing programs on various campuses, sent letters urging the governor and state nursing board to increase temporarily the number of clinical hours nursing students may complete through simulations.
Currently, the state requires 75% of a nursing student’s clinical education to be in a hospital, with the remaining 25% allowed to be simulation. Students must also pass board exams after graduating.
Nursing schools are asking the state to reduce the required amount of in-hospital hours to 50% of a student’s clinical education, thus allowing the schools to do more computer simulation with coursework that has already been moved online because of campus closures from the coronavirus outbreak.
Alison Wrynn, associate vice chancellor for academic programs, innovations and faculty development at California State University, said the vast majority of students expected to graduate this spring have had their clinical placement sites closed, largely because of the lack of available personal protective equipment.
The California State University system, one of the largest issuers of nursing degrees in the state, graduates about 4,000 nursing students every year.
Wrynn said allowing for more simulation education is a necessity, with only a small number of Cal State nursing students continuing with clinical placements in hospitals.
“Other states have initiated a 50% simulation and their graduates are successful,” Wrynn said. “We have high-quality simulation software from respected vendors. Our faculty monitor these experiences and evaluate the students. We’ve been doing this and we’ve been doing it well.… This is not going to impact the quality of our nursing education.”
Fresno City College President Carole Goldsmith said the state nursing board would be “incredibly shortsighted” if it did not ease the graduation requirements. Fresno City College produces about 200 nursing graduates each year and it’s unclear, Goldsmith said, how many students could still graduate in May without the change.
Goldsmith closed the school’s campus, but in-person elements for programs that train workers in essential services, like police work, firefighting and nursing, are continuing, per guidance from the state chancellor’s office and requests from local public health and safety officials.
The latest maps and charts on the spread of COVID-19 in California.
Goldsmith said her college works with close to a dozen local sites to offer clinical placements for nursing students; only one of those, St. Agnes Medical Center, is still taking students.
“Our capacity … has been greatly diminished,” Goldsmith said.
With a limited number of healthcare workers, and many of those in a high-risk group for COVID-19, “there are so many things our students could be doing,” Goldsmith said, such as initial screenings, vitals and triage.
She said temporarily relaxing the state’s rules on how much time a nurse must spend in a hospital rotation to graduate will not come at a cost to patients. She pointed to a comprehensive 2014 study by the National Council of State Boards of Nursing that showed there was no significant difference in learning or clinical performance between students who did 25% of their clinical education in simulations and those who did 50%.
“And that was in 2014,” Goldsmith said. “Technology has improved in that time.”
For now, nursing student Brea Ortiz of Whittier said, it’s a waiting game. She’s watching every news conference given by Newsom in hopes of hearing there will be some changes so she can graduate.
“There is a need for us and we can be helpful,” said Ortiz, 24, who is supposed to start a hospital rotation April 10 or her August graduation will be pushed back. The hospital rotation in a critical care unit is currently suspended.
“All these new beds are going to need staffing,” Ortiz said. “Those on the front lines are going to experience burnout or exposure and the need for us is there. We just need help so we can get in there.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.