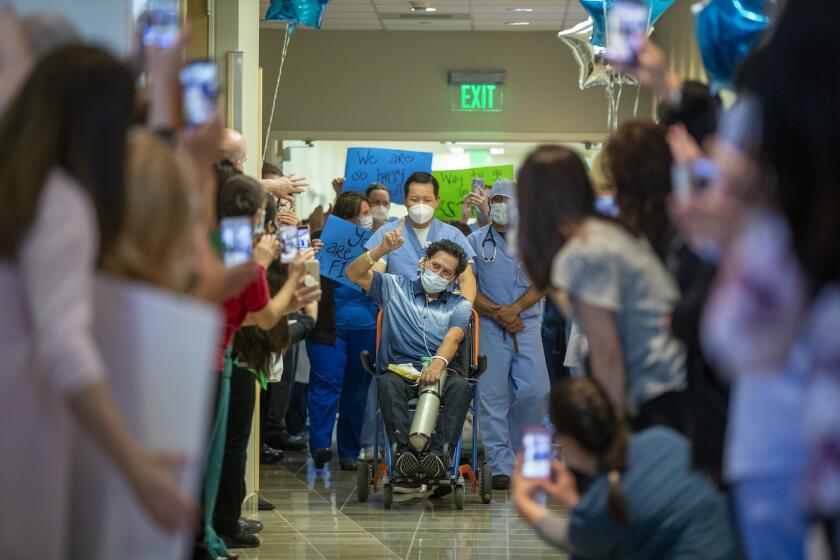
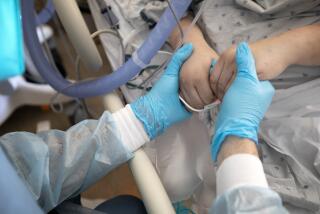
The silent, deadly spread of coronavirus in California began far earlier than first reported

- Share via
New information emerging in the last week in California paints a very different picture of the spread of the novel coronavirus than the one suggested by the first, official version.
Postmortem testing indicates that two Santa Clara County residents who died in their homes in early to mid-February were infected with the novel coronavirus that now has killed more than 1,400 Californians, the county medical examiner announced Tuesday. The new information, combined with antibody testing results, suggests that the coronavirus was circulating in California for at least a month before it first came to light — the earliest cluster of infection so far reported in the United States.
The new testing results mean that a 57-year-old San Jose woman who died Feb. 6 was the first person in the United States known to die of COVID-19, the disease caused by the coronavirus. The second would have been a 69-year-old man who died Feb. 17, according to the new information from the medical examiner.
Those cases push the date of COVID-19 community spread in the United States backward three weeks from the first announced death, that of a man in his 50s in Kirkland, Wash., who died Feb. 28. It was later reported that two residents of a Kirkland nursing home had died two days earlier.
The medical examiner’s office also confirmed a Los Angeles Times report on signs of early spread of the virus that included a third early death, a man who died at his San Jose home March 6. In addition, The Times found data that showed a Santa Clara County resident of an assisted living facility who tested positive for COVID-19 had fallen ill in mid-February.
“They’re really like iceberg tips” representing a larger body of undetected cases, said Santa Clara County Health Director Dr. Sara Cody. “There must have been somewhat a significant degree of community transmission.”
The pandemic’s toll: Lives lost in California
Hundreds of people have died in California due to the COVID-19 pandemic. These are some of their stories.
Cody said she now believes the novel coronavirus was circulating in the San Francisco Bay Area as early as January.
The new information from the coroner holds important keys to understanding the first cases of COVID-19, which spread silently within communities at a time when health officials still focused entirely on infections from travelers entering the United States from abroad, or off cruise ships.
Researchers at Stanford University and USC are seeking just such historical glimpses of novel coronavirus activity to understand how fast it spreads and how lethal it is. That information helps build better computer models that public officials such as California Gov. Gavin Newsom rely on to decide when to ratchet down stay-at-home orders and when it might be safe to allow people to resume a more normal life or go back to work.
Those same models will also factor heavily in decision-making if there is a second wave of virus outbreaks once restrictions are lifted.
Initial reports from the federal Centers for Disease Control and Prevention said COVID-19 cases in the United States were confined to 11 travelers from Wuhan, China, and members of their households, six of them in California. The earliest of those California cases was not diagnosed until Jan. 27.
Researchers and health officials now believe that by that time the virus was already circulating through the Bay Area, especially Silicon Valley, and probably had been introduced weeks before.
These are some of the unusual new scenes across the Southland during the coronavirus outbreak.
With influenza hitting hard at the same time in the Bay Area, Cody said, it would have been difficult to pick out which of those illnesses were cases of COVID-19.
Newsom said Wednesday that he had “directed” coroners “beyond Santa Clara” to screen for COVID-19 cases as early as December. The Times could not verify such a request. The California Department of Public Health did not respond to questions. Nine coroners’ offices, including the one in Los Angeles, said they did not know of the governor’s directive.
Newsom did not directly answer a question about what decisions he would have made differently had the state known a month earlier that COVID-19 was spreading unheeded. However, he said, “When this occurred is important forensic information, profoundly significant in terms of understanding of the epidemiology of this disease.”
Cody said that had she known that the virus was spreading through Santa Clara County and that people were dying, the county would have issued public health orders much earlier. As it was, Santa Clara was the among half a dozen Bay Area counties that were the first in the state to announce shelter-in-place orders as the region became one of the nation’s first virus hot spots.
The discovery of early Santa Clara County cases is in line with testing that found COVID-19 antibodies among some 3,300 county residents this month, suggesting an infection rate 50 to 85 times greater than the number of confirmed cases at the time.
“When you start seeing the first death, actually, the number of cases in the population is probably pretty high already. It’s been in the community for a long time,” said Neeraj Sood, a professor at USC’s Price School of Public Policy, coauthor of the Santa Clara County study and lead investigator in a similar COVID-19 serology study in Los Angeles County. “And you have to believe that it is contagious, that it’s doubling” every three to four days.
In its calculations of the disease spread rates, Sood said, the study used Jan. 31 as the date when the virus appeared in the Bay Area. He called that date “conservative.” Sood said he believes the virus was circulating weeks before the newfound death.
“I would take three weeks before that [death] as the potential first seed,” Sood said.
The Times confirmed independently that Santa Clara County’s Feb. 6 COVID-19 death was that of Patricia Dowd, 57, a senior quality manager for a global semiconductor company headquartered in Fremont.
Family members said Dowd became unusually sick with flu-like symptoms in late January and was forced to cancel plans to go to a weekend funeral. But her death was unexpected. She had improved and was working from home, corresponding with a colleague about 8 a.m. the day of her death. About two hours later, her daughter found her lifeless body. At first, family members suspected a heart attack, but as news of other COVID-19 deaths spread and knowledge about the symptoms deepened, their suspicions grew.
Family members said Dowd had not gone abroad recently but had a history of foreign travel, as did her co-workers at Lam Research. Her brother-in-law, Jeff Macias, said Dowd traveled “multiple times a year to different global locations.”
“Where did this come from if it wasn’t her traveling?” Macias said. “We don’t know if Patricia was the first. But this opens up the door to find out.”
Her husband, Dean, works for the Santa Clara County Sheriff’s Office. Past records show he was assigned to the jail staff. The Sheriff’s Office said COVID-19 cases began showing up among jail staff March 22.
Patricia Dowd’s sister is a pharmacist at a San Jose hospital. Macias, who also works at Lam Research, said he did not believe any family members had been offered COVID-19 testing.
A public relations firm hired by Lam Research returned calls seeking comment but offered no statement.
The Santa Clara County medical examiner’s office said it could not yet verify that Dowd’s death is its Feb. 6 case.
Other county coroners also are testing using nasal swabs and lung scans to screen some deceased for COVID-19 infection, but the policies are widely divergent and so are the outcomes.
Alameda County, north of Santa Clara, is testing those who died with flu-like symptoms and randomly taking swabs of others whose bodies come to the morgue. None of the tests have come back positive.
To the west, San Mateo County’s coroner for several weeks has tested every case it handles for COVID-19 and found no more than six that had the virus. Coroner Robert Foucrault said his office is still discussing whether it is possible to test those who died as early as February.
The Santa Clara County medical examiner’s office said it currently tests only those who were known to have had flu-like symptoms before their deaths. Dr. Michelle Jordan, the county medical examiner, said the office sent autopsy tissue from two February deaths to the CDC for confirmation in mid-March.
The CDC lab results were returned to Santa Clara County’s health lab Friday but not forwarded to the medical examiner until Tuesday. Jordan said she had “high suspicion” that these cases could have been COVID-19 and therefore preserved the samples for testing. No other such tissue samples have been sent for testing, she said.
However, Jordan said, her office now has a standing protocol to screen those known to have experienced fever, coughing or other flu-like symptoms before death. Such was the case of an elderly San Jose resident who died at home March 6.
Los Angeles County began screening coroner cases for infection on March 11 by testing those who showed any signs of a flu-like illness. By swabbing nasal cavities and scanning lungs, the agency identified at least three COVID-19 cases among some 70 people who were tested, said Medical Examiner Dr. Jonathan Lucas.
Health officials offered slightly rosier projections about the trajectory of the virus in L.A. County but cautioned that the improved outlook was contingent on residents continuing to practice physical distancing.
Each of those three people died at home. The oldest was 93, the youngest, 55. The capability of extending that testing raises questions Lucas said he cannot yet answer, such as how much time the coroner’s office has to seek a virus sample before the test would fail on even positive cases.
Los Angeles County has not seen an increase in home deaths, said coroner’s office spokeswoman Sarah Ardalani. But out of caution, the agency has acquired large refrigerator trucks and portable buildings to triple its storage capacity to 1,500 bodies should the pandemic begin to swamp funeral homes and mortuaries.
“We didn’t know what was happening for us” when planning began in early March, Lucas said. “We didn’t know what we were going to see.”
In Orange County, postmortem testing for COVID-19 is largely limited to cases that fit the profile of the disease, such as signs of compromised lungs. Sometimes there is no clue. The coroner found COVID-19 in five cases, including a 45-year-old woman found dead March 29 inside her car at a church parking lot.
Fresno County, by contrast, has swabbed a single body for COVID-19. Coroner Kelly Matlock said the test came back negative. The agrarian Central Valley county to date has reported only seven COVID-19 deaths.
San Joaquin County has been testing all apparent natural-cause deaths for COVID-19 since March 11. But medical examiners in Sacramento, Tulare, Contra Costa and Stanislaus counties said they had done limited COVID-19 testing. None said they planned to look at older cases.
Annette Choi, a graduate student at the UC Berkeley Graduate School of Journalism, contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.