Staffing shortages feared at some California hospitals as COVID-19 fills up beds
- Share via
As California hospitals rapidly approach capacity because of the unprecedented spike in coronavirus cases, there are growing concerns about shortages of workers as the healthcare system strains to handle the growing demand.
Officials have contingency plans of opening up additional facilities if hospitals become overwhelmed, something developed by the first COVID-19 surge this past spring. But conditions have changed in significant ways since then that could make staffing an issue.
For one thing, the spring surge was more limited in scope, with some parts of California — and the nation — being hit harder than others. That allowed more room for shifting resources and bringing in medical professionals from areas that could spare them. The current surge is not only larger than the spring one but also much more widespread, leaving fewer areas with nurses and doctors to spare.
Moreover, some patients avoided emergency rooms and optional medical appointments in the spring, fearful of being infected. Fewer people are staying away now, and that is taxing hospitals as they see an influx of COVID-19 patients.
“Please know that those resources are not unlimited,” said Dr. Christina Ghaly, who directs the county agency that operates four acute care public hospitals and several clinics, at a Wednesday news conference. “Staffing is tight, and it’s tighter than it normally would be in a hospital.”
Hospitals are filling up fast, but so far they have been able to handle the surge. County health officials anticipate that, in one week, L.A. County could see between 275 and 500 new COVID-19 admissions each day. Based on current modeling, if the rate of new cases continues to climb, L.A. County will have a shortage of ICU beds over the next four weeks, according to county officials.
Coronavirus cases and hospitalizations have hit unprecedented levels in California, and officials expect conditions to deteriorate rapidly in the coming weeks.
There are options when conditions worsen.
Hospitals can limit nonessential outpatient care, cancel nonessential surgeries and more quickly discharge patients who could be cared for in rehabilitation hospitals and care facilities. Hospitals can also, and often do, open overflow patient areas.
To increase staffing in critical areas during the pandemic, hospitals have asked outpatient staff with emergency and intensive care backgrounds to work in ERs and COVID units. Facilities have also contracted with traveling nurses to beef up staffing numbers.
Some hospitals are also seeking waivers from the state that would allow nurses to care for more patients than otherwise allowed under state law.\
Gov. Gavin Newsom has announced a stay-at-home order affecting most of California.
Anxiety inside medical facilities is growing as cases surge and workers feel they are entering uncharted territory during this pandemic.
Unlike in the spring, emergency rooms across L.A. County, both at public and private hospitals, are busy.
“The number of COVID-19 cases and hospitalizations has been steadily increasing in the recent weeks,” Darlene Scafiddi, vice president of nursing at Pomona Valley Hospital Medical Center, said at a recent Board of Supervisors meeting. “Our numbers at the hospital have doubled in the last three weeks. As the only trauma center in the east San Gabriel Valley, and a comprehensive stroke center, right now all of our ICU beds are full, and we are in surge.”
A leader at Greater El Monte Community Hospital echoed a similar sentiment, noting that the facility was seeing a “substantial surge.”
Coronavirus hospitalizations in California are at an all-time high. Doctors and nurses at some hospitals say their long-feared nightmare has arrived.
In the spring, during the first wave of the COVID-19 pandemic, people were avoiding the hospital out of fear of contracting the virus, and the emergency room saw a decrease in its volume of patients because of the public’s fear to seek care, said Claude Stang, emergency department executive director at Cedars-Sinai Medical Center.
“That’s changed. In this third wave, patients are coming to the hospital for various conditions, and they don’t seem as fearful about coming to the hospital,” Stang said.
That isn’t a bad thing, as people need care and shouldn’t delay it, he said.
During the first wave, Cedars-Sinai, like most others, postponed elective surgeries and had an average daily census of only about 600 patients. In this third wave, Cedars-Sinai is one of many hospitals continuing to operate and has a census of about 900 patients.
Stang fears what will happen to his staff as cases continue to surge. He said he worries about healthcare workers getting sick as more virus spreads in the community.
Since early November, cases among healthcare workers have increased 71%, according to data presented by L.A. County officials on Wednesday.
As more people fall sick, it becomes easier for others to contract the virus as the percentage of people infected in the community grows. These patterns have caused surging numbers of cases recently among not just healthcare workers, but also at skilled nursing facilities, schools and other workplaces.
A nurse at a Kaiser hospital in L.A. County said he feels fatigued by the constant looming threat of COVID-19. When he comes into work, he never knows if he’ll be assigned a patient infected with the virus.
“It feels bad because you want to help the patients, but at the same time I’m just so burned out,” said the nurse, who asked not to be named because his hospital bars medical staff from talking to the media. “I just feel like the stress of working right now, it’s just too much. I’m just over it — I’ve never hated my job more.”
He said sometimes they find out after treating a patient that they actually had COVID-19. Their minds race trying to determine how long and how closely they interacted with them.
“Everyone goes into a panic,” he said.
Unlike earlier in the year, his hospital isn’t short on PPE. Now, it seems, the limiting factor is beds, and projections show the hospital could run out soon.
“We’re hitting a peak we never hit the first round,” he said.
He said the hospital has begun moving nurses around and bringing in temporary staff to prepare for a greater surge. Elective surgeries are being canceled as of this week, he said. “Just a lot of changes happening now,” he said.
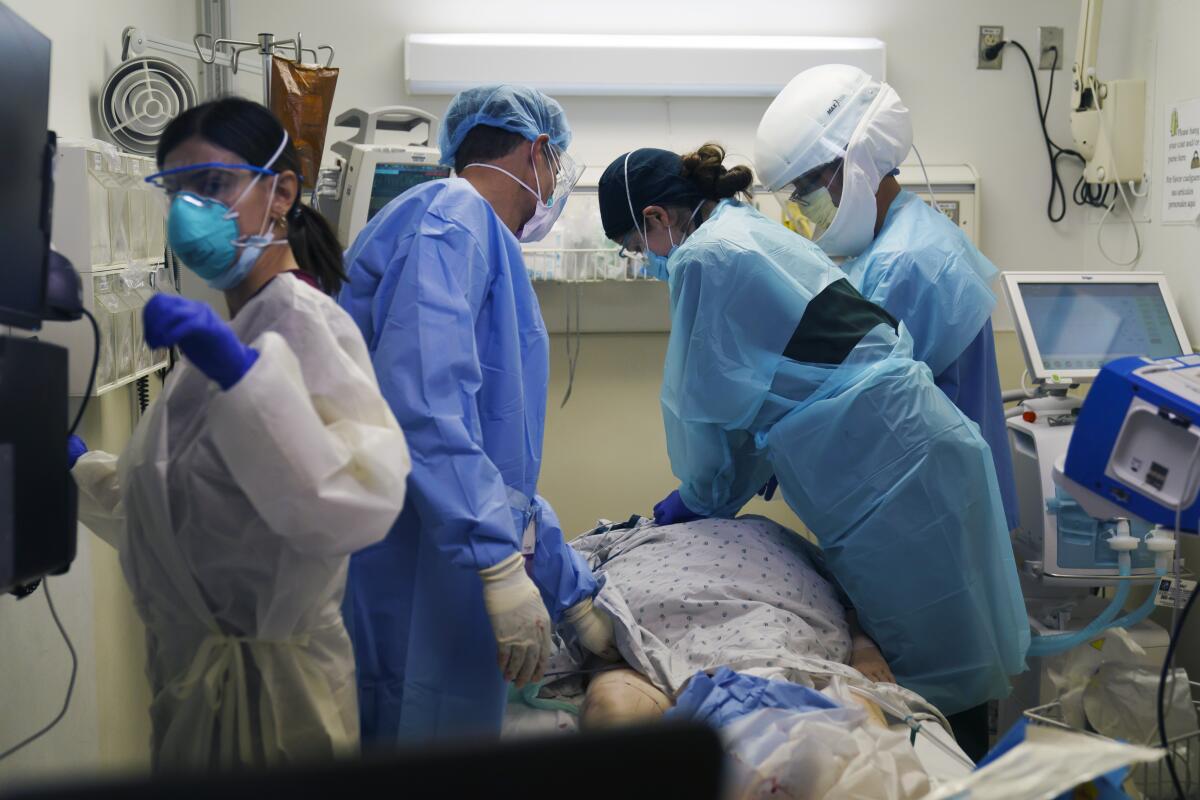
A new surge of COVID-19 is battering Southern California, bearing down on exhausted healthcare workers, raising anxiety levels on hospital wards and stoking fears that there might not be enough staff and supplies for the difficult weeks ahead.
One proposed remedy to lighten the load of hospitals has proved controversial.
Early in the pandemic, concerns over hospital staffing led Gov. Gavin Newsom and the California Department of Public Health to start allowing hospitals to apply for waivers, only when they’re seeing a COVID-19 surge or staffing shortages because of the pandemic, that allow them to exceed mandated nurse-to-patient ratios. (California is the only state in the country with mandated nurse-to-patient ratios at acute care hospitals.)
About 115 hospitals in California have been approved for waivers since the start of the pandemic — some multiple times, as the waivers last 90 days — including about 31 facilities in L.A. County, according to an analysis of California Department of Public Health data. Most recently, Antelope Valley Hospital in Lancaster received approval shortly after Thanksgiving.
Antelope Valley Hospital, which a hospital spokeswoman said has the second-busiest emergency room in the state, has been inundated in recent weeks with not only COVID-19 patients but also trauma patients.
The hospital received a waiver to temporarily change its staffing ratio on its telemetry floor, the unit for patients who require a heart monitor. Instead of 1 nurse to every 4 patients, the staffing ratio is 1 to 5.
“It’s a temporary measure until we can recover from the patient surge and staffing shortage,” hospital spokeswoman Cynthia Frausto said, adding that several nurses are sick with COVID-19 and other ailments.
Earlier this week, registered nurses held a news conference to protest the staffing change, which they say stretches their exhausted staff too thin.
Maria Altamirano, a registered nurse who has worked at the hospital for 13 years, said nurses do more than regularly turn patients, manage their medications, help them to the restroom and provide overall healthcare. Because family members cannot visit loved ones with COVID-19, she said, nurses must also help patients with video calls.
Meanwhile, they’re also wearing a substantial amount of protective gear, and they do not generally have time for a break. Sometimes Altamirano has had to wait eight hours to use the restroom. Sometimes she’s gone an entire shift without a break. Two weeks ago, she was so tired that when she got home, she could not feel her feet. She woke up on her couch in her bathrobe, the chamomile tea and dinner her husband made her still waiting in the kitchen.
On a recent shift, she started at 7 a.m. and didn’t eat or drink anything until 11:30 a.m., when she gulped down some tea and a doughnut and went back to work. The nurses no longer hug or talk or have time to offer support to one another, despite the tremendous mental toll the pandemic has taken on them, she said.
“You worry constantly [while on break] about ‘Who’s looking after my patient? No one?’ So we all do as much as we can to help each other out,” she said. “We haven’t had a break since March.”
On Thanksgiving night, the hospital saw a “tremendous surge” of COVID-19 and trauma patients, she said.
“Our ICU is now bombarded as well with COVID patients, and we have to still keep beds open for our trauma patients and major surgeries, and what’s going to happen when those beds are taken up by COVID patients?” Altamirano said. “We’re not going to be able to take care [of them].… There will be no beds.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.