Nearly 250,000 new coronavirus cases in 8 days: Where is L.A. County Omicron surge heading?

- Share via
Over the last eight days, there have been nearly 250,000 positive cases of coronavirus reported in Los Angeles County, a record-breaking number that shows how fast the Omicron variant is spreading.
Moreover, with an average of nearly 115,000 people being tested each day over the last seven days, more than 20% of people are testing positive for the virus.
This spike is breathtaking but also expected, given the way Omicron earlier marched through South Africa, Europe and American cities such as New York. But there are some bright spots, including far fewer critically ill patients than during last winter’s surge. Those who are vaccinated and boosted generally are avoiding major illness.
So where is Omicron going and how much worse will it get? Officials expect infection tallies to keep going up. Here’s where we stand now:
L.A. County sees a record 44,000 new coronavirus cases as staff shortages strain hospitals
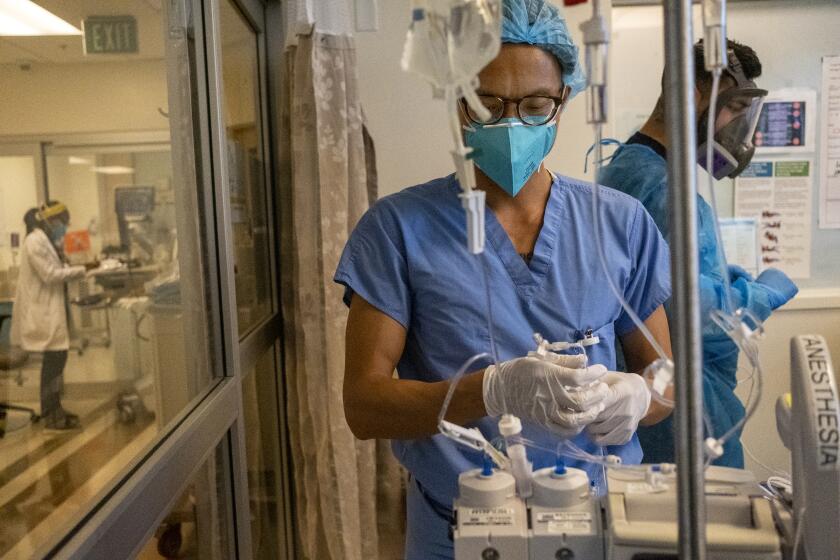
Hospitals
Hospitalizations in Los Angeles County nearly doubled over the last week, to 3,472 patients as of Sunday. The rapid COVID-19 spread has left medical facilities with lower staffing and raised fears about care.
Yet fewer people are becoming severely ill from the Omicron variant. Even the hospitalization numbers don’t tell the whole story, as some counties are seeing a growing percentage of patients entering hospitals with a coronavirus infection but being treated for something other than COVID-19.
“This is very different than what we were experiencing a year ago,” Dr. Brad Spellberg, chief medical officer at Los Angeles County-USC Medical Center, said Friday. “Clearly, the number of positive tests is actually higher than it was a year ago — and I understand why that’s very scary, in terms of these numbers going up — but the average sickness level is substantially lower.”
During the last winter surge, about 80% of coronavirus-positive patients in the flagship public hospital’s emergency department were being admitted to the hospital, and nearly half of those went to the intensive care unit, Spellberg said. Now, only about a third of coronavirus-positive patients are admitted and about 20% to 25% of those are going to the ICU.
“That gives you a sense of the difference in magnitude,” he said. “This is why last year was much more stressful in many ways. We did come within a hair’s breadth of triaging patients last year.”
Ambulances are waiting longer to offload patients in Orange County, echoing a similar problem in L.A. County as coronavirus infections increase.
In Orange County, about five of its 25 hospitals are asking for more staffing from the state “because they are experiencing extreme staffing shortages,” and more requests are expected, Dr. Regina Chinsio-Kwong, a deputy county health officer, said Friday.
Emergency rooms have a limited number of beds and staffers to work with. Chinsio-Kwong said that she has heard anywhere from 10% to 20% of workers are unavailable because of coronavirus-related reasons, calling it a “dire situation.”
Ambulances are waiting as long as 52 minutes at hospitals to drop off patients, well above the 30-minute goal, Chinsio-Kwong said. In addition, most hospitals have set up surge tents to increase capacity, and Orange County has stopped accepting hospital patients diverted from neighboring counties. So far, however, hospitals are not seeing a critical shortage of ICU beds.
The state Department of Public Health issued new guidance that permits hospitals and skilled nursing facilities to direct healthcare workers who have been exposed to or tested positive for the coronavirus, and are asymptomatic, to return to work immediately, without isolation or additional testing.
The workers must wear N95 respirators and should ideally interact only with coronavirus-positive patients. However, the state acknowledged that this might not be possible in the event of extreme staffing shortages or in settings such as emergency departments, where it’s not always immediately clear which patients are infected.
The facilities that adopt the relaxed rules must first consider modifications to nonessential procedures and make every attempt to bring in additional contract or registry staff, the state said in the guidance, which took effect Saturday and will stay in place through Feb. 1.
Health officials halted L.A. County’s home COVID testing program this week because of a “backlog in the logistics” of processing test kits, which had been limited to 4,000 a day.
Testing
Getting coronavirus tests can be a frustrating experience, with long lines and a lack of at-home tests.
The increased demand for testing prompted L.A. County health officials to pause a home testing program as they deal with a “backlog in the logistics of processing these kits.”
Some at-home antigen tests are reselling for triple the retail price. To help curb price gougers, Gov. Gavin Newsom signed an executive order Saturday to protect buyers.
Under the order, sellers cannot increase prices on at-home coronavirus test kits by more than 10% of the highest price initially charged by the seller on Dec. 1. The order also prohibits sellers who haven’t previously sold at-home test kits to set a price greater than 50% of what they paid for the test kit.
It also provides additional tools for agencies such as the California Department of Justice and local law enforcement to take action against price gougers. A violation can result in a fine of up to $1,000, imprisonment for up to six months, or both. The violation also could trigger an infringement of the Unfair Competition Law, which could lead to more penalties.
California Atty. Gen. Rob Bonta announced those who have been a victim of price gouging should file a complaint to his office at oag.ca.gov/report or contact their local law enforcement agency.
Newsom also announced Friday that National Guard troops would be deployed throughout the state to help with testing.
“The National Guard plan will deploy over 200 Cal Guard members across 50 Optum Serve sites around the state, providing interim clinical staff while permanent staff are hired, adding capacity for walk-ins, assisting with crowd control and back-filling for staff absences — all in an effort to conduct more tests for more Californians. Additional members of the Guard will be deployed next week in similar capacities,” the governor’s office said in a statement.
California would spend $2.7 billion on new efforts to respond to COVID-19 cases under a budget proposal Gov. Gavin Newsom will send to lawmakers next week.
Funding
California would spend $2.7 billion on new efforts to respond to the surge in coronavirus cases, including additional testing capacity and assistance to hospitals, under a budget proposal Newsom will send to state lawmakers next week.
The governor also will ask legislators to help craft new COVID sick pay rules for Californians, modeled after the policy that expired last fall, requiring businesses with 26 or more workers to offer up to two weeks of supplemental paid sick leave for employees to care for themselves or a family member.
Advisors to Newsom said Saturday the governor will ask the Legislature to take quick action on authorizing the first $1.4 billion of the new pandemic response package when he sends his annual state spending plan to the Legislature on Monday. Most of the early funding would go to expand testing programs, with the remaining portion spent on virus response efforts inside California prisons.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.