Will Memorial Day 2020 be remembered as the holiday when COVID-19 got the upper hand?

- Share via
We may have the reason to remember Memorial Day 2020 as the holiday when COVID-19 exploded. Looking around the country over the weekend, there was little evidence that people were making the sacrifices needed to save their own lives and those of their friends and family.
In preparation for a TV interview on Monday afternoon, I compared Sunday’s COVID case reports with those of a month ago. The numbers tell an interesting — and worrying — tale.
First the good news: On March 30, New Jersey reported 3,250 new cases of COVID-19 to New York’s 9,000. No one who lives in Manhattan, as I do, will forget that day of constant sirens. On Saturday, two months later, the number of new cases in New Jersey was 1,050, down about 60% In New York, 1,772 new cases were reported on Saturday, down about 80% from March 30.
Because of social distancing and mask wearing, which we now know work, the epidemic in both places, while far from over, is waning.
Now the bad news: On March 30, the numbers of new cases for Illinois was 460 and for Wisconsin 109. On Saturday, Illinois reported 2,508 new cases, a more than fivefold increase. Wisconsin reported 400 new cases, a nearly fourfold increase. Yet on Monday’s holiday, in the midst of a rapidly growing epidemic in the state, Wisconsin lake shores were packed with maskless celebrants.
Many Southern states are also seeing a rise in cases. Compared with March 30, COVID cases are up about threefold in Alabama, Arkansas and Texas. The epidemic has not abated in Georgia, Florida and Ohio, where the numbers of new cases is close to what it was two months ago. In California, COVID cases are still on the rise.
When holiday revelers were asked on camera why they were out and about as normal over the weekend, the usual answers were some variation of “The cure is worse than the disease” or “The infection is rarely lethal, less than 1%.”
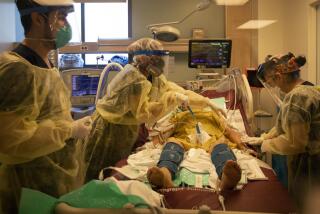
Do these people remember that so far nearly 100,000 Americans have died? And that figure doesn’t even count the seriously ill. About 20% of those who get the virus get very, very sick. When you ask those survivors to talk about what they went through, it’s an alarming picture.
They describe exquisite pain while acutely ill and long-term consequences after the virus has run its course. Some will be on kidney dialysis for the rest of their lives. Some of the young children who caught the virus will have permanently weakened hearts. And, weeks after recovering, many who had the virus are still having trouble catching their breath and recovering their energy.
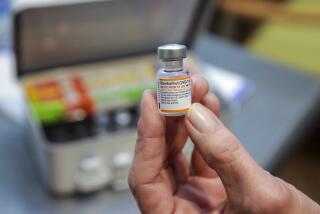
Because I am a biomedical scientist who has brought new drugs and vaccines to market, I am often asked when we will have a vaccine. By October? By the end of the year? By early next year?
My experience tells me the actual question should be not when we will have a new vaccine, but if. Success is by no means assured. Thirty-five years ago I predicted it might be decades, if ever, before we would have an effective vaccine for HIV/AIDS. We still do not have one.
I do not think making a vaccine to prevent COVID-19 will be as difficult as for AIDS, but neither is it a “slam dunk” that a vaccine will come to our rescue. Why? For one thing, the ability to respond to a new vaccine decreases sharply with age, and it is older people who are hardest hit. In other words, those who need it the most might benefit the least, even if a vaccine is developed quickly. Also, infections like COVID-19 contracted though the lining of the nose are very difficult to prevent.
If we do get a vaccine soon, it is likely to be only partially effective for the young and may not be effective at all for the old. And remember, a vaccine that is to be given to hundreds of millions, or even billions, of healthy people must be demonstrably safe before it is brought to market. That is a very tall order for any medication.
So without any certainty of a vaccine savior, what can we do? We know what works: aggressive social distancing — which means staying at home — coupled with widespread testing, contact tracing and mandatory 14-day isolation for those exposed to the virus.
To give up what we know works while hoping for a distant and highly uncertain medical miracle is folly, and we will certainly pay for it with many more lives lost and widespread economic ruin.
William Haseltine, a former Harvard Medical School professor, serves as chair and president of the global health think tank, ACCESS Health International.
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.