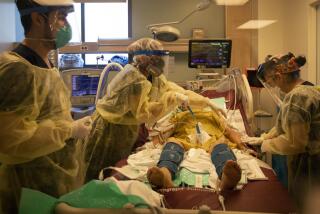
Reopening a city that still throbs with loss
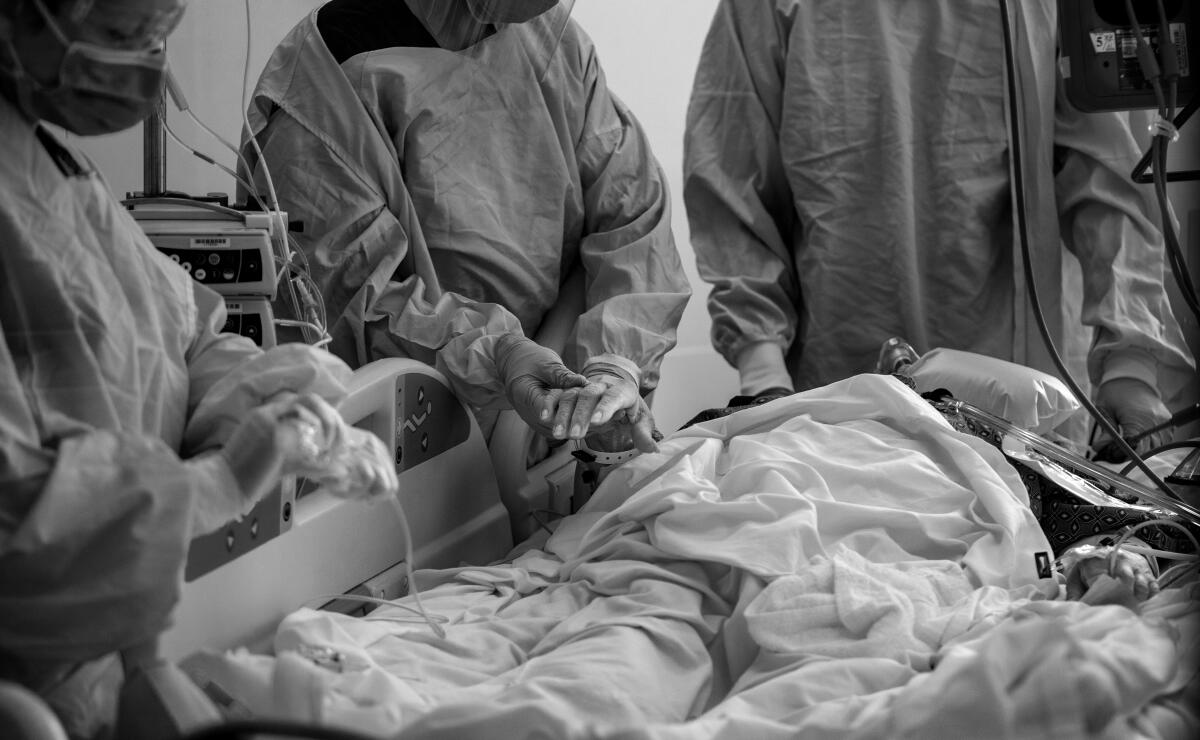
- Share via
In this last stretch of spring in Los Angeles, the world around me is changing. I can stroll into Trader Joe’s without braving a serpentine line to buy produce and peanut butter. Maskless young couples kiss at crosswalks on Sunset Boulevard.
I am fully vaccinated; I can take off my mask in the office I share with vaccinated colleagues. But doing so feels transgressive, a violation of something I can’t name.
“June 15! Almost back to normal!” a friend texted, though the idea of normalcy feels more slippery and shapeless than ever before.
On Tuesday, California will fully reopen. Vaccinated people can forgo masks in places such as gyms, bars and stores. Unvaccinated people must stay masked in these same places, though the process of verifying one’s vaccination status remains opaque.
A year ago, deep in the waters of loneliness and isolation, the possibility of a June 15 was both raft and lifejacket to me. But caring for patients and families as a palliative care doctor over the last year has left me ambivalent about what comes next.
I fear the complacency that reopening will surely breed, the false certainty that we have “beaten” the coronavirus. Only 47% of adults in Los Angeles are fully vaccinated. Dangerous variants continue to emerge; COVID-19 continues to devastate the lives of millions. I wonder how much our quest for normalcy will obscure the way the city and the world still throb with loss.
Not long ago, on the way to La Cañada, I passed a school where a beloved teacher taught for 25 years before she died of COVID in April 2020. Her family was one of the first I had to speak with over Zoom.
I told them about her damaged lungs and the limits of the ventilator, struggling to offer empathy and support through the screen, unable to offer tissues or lean forward when someone’s voice trembled.
I struggled to be her doctor when PPE shortages and ICU restrictions separated us. I watched her husband cry onscreen in his bedroom, febrile from COVID himself and isolated from his children. I was in her room only on the day she died, beneath a canopy of faux flowers the ICU nurses strung above her hospital bed. I met her husband and son in person just minutes before.
Hearing a police siren last week in Silver Lake reminded me of the cop whose father survived a risky surgery and its long aftermath, only to contract COVID shortly after returning home. On Zoom, the officer was stoic and reserved, asking unwavering questions about his father’s health on behalf of his aggrieved mother. Just before Christmas, a colleague and I called him at work to tell him that his father’s body was shutting down, one organ system after another. He was silent, until his voice shook with tears. I didn’t know how to answer him when he asked why God pulled his father through surgery, but not COVID.
A morning came when I saw the name of a dear friend’s father on the ICU list. A Pakistani immigrant, he was the proud father of his four daughters, doctors all. He refused to believe that being a woman meant chasing smaller dreams, my friend told me. How am I supposed to live without him, she asked? On the day he died, I huddled with her family outside the hospital, listening as they decided which two people should be at his side: Who needed this closure the most?
When I walk the hospital halls, I remember what happened room by room. A couple, married for decades, died down the hall from one another in the ICU. The wife, lucid and lipsticked until she was intubated, suppressed her own gasps to join Zoom calls about her husband’s condition. After her husband died, her children argued in their agony that she would be willing to go through tremendous suffering to protect her children from abandonment.
Ordinary sights knocked loose memories I didn’t realize I had. Seeing my neighbor walk his huskies brought me back to the bedside of a young man with back pain. He had been so afraid of COVID, he said, he didn’t get checked out. He hadn’t torn a muscle while walking his own husky, as he’d hoped. An aggressive cancer had instead gnawed through his spine.
In the midst of the year’s chaos, there was no way to make sense of it all. But points of transition force a reckoning. My June 15 ambivalence doesn’t stem from fear of change or survivor’s guilt. It is, in the words of poet Seamus Heaney, “the strumming, rooted, long-tailed pull of grief.”
Reopening is an economic and social necessity, but moving forward isn’t the same as moving on. We are still a city of ghosts and orphans.
Our lives continue in reconfigured places — streets with shuttered businesses, homes with empty seats at dining tables. What sort of suffering will accompany “normality”? How many more will die? How will it feel to toggle, indefinitely, between restriction and liberation, anguish and joy? What will our collective trauma come to mean?
Navigating the uncertainty that accompanies tragedy is the art of palliative care. I offer my patients far more questions than answers. Sometimes the questions themselves are the path forward.
June 15 will be another scene, not an ending, in the longer story of COVID. This moment isn’t a postscript, but rather a preamble to the next phase of the pandemic.
As we excavate and live through its varied meanings, let us not bury the dead.
Sunita Puri is the author of “That Good Night: Life and Medicine in the Eleventh Hour.” She is the director of the palliative medicine program at Keck Hospital and Norris Cancer Center of USC. @sunitapurimd
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.