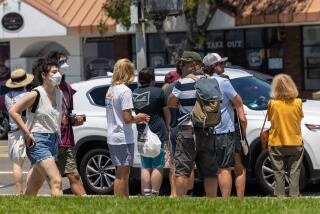How Florida fell so far behind California in battling the coronavirus
- Share via
Since the beginning of the COVID-19 pandemic, California and Florida have stood as polar opposites in how government has responded to the coronavirus.
Gov. Gavin Newsom last year backed sweeping stay-at-home orders in California, and this summer supported targeted vaccination requirements and indoor mask rules. In Florida, Gov. Ron DeSantis led efforts to quash health rules: He issued an order prohibiting mask requirements and signed a law banning vaccine passports — mandates by businesses or government agencies to show proof of vaccination to gain services.
The divergent approaches have been the subject of endless partisan debate.
But with the Delta variant raging this summer, data show Florida has fallen significantly behind California in many key metrics. It marks a reversal for the Sunshine State, which last winter was hailed by some conservatives for keeping COVID-19 deaths and coronavirus cases relatively modest without major restrictions.
A Los Angeles Times analysis found that of the nation’s 50 states, Florida had the worst COVID-19 death and coronavirus case rate for the summer.
California’s summer death rate was about one-sixth of Florida’s, and its coronavirus case rate was about two-thirds lower.
Florida recorded 14,334 COVID-19 deaths in the summer, or 70 fatalities per every 100,000 residents — the worst tally of any state. California saw 4,874 deaths during the same period, according to Johns Hopkins University, equaling 12 per every 100,000 residents.
California and Florida have followed differing paths during this 19-month pandemic: Through the fall of 2020, Florida’s death rate was much worse than California’s — at one point 84% worse. Californians credited early implementation of stay-at-home orders as critical to keeping death rates low in the first two waves of the pandemic, while Florida reopened fairly quickly.
But California’s devastating fall and winter surge led to a dramatic worsening of its death rate, and by the start of spring, Florida’s death rate was just 7% worse than California’s. Some critics of health orders wondered whether lockdown measures were worth the trouble.
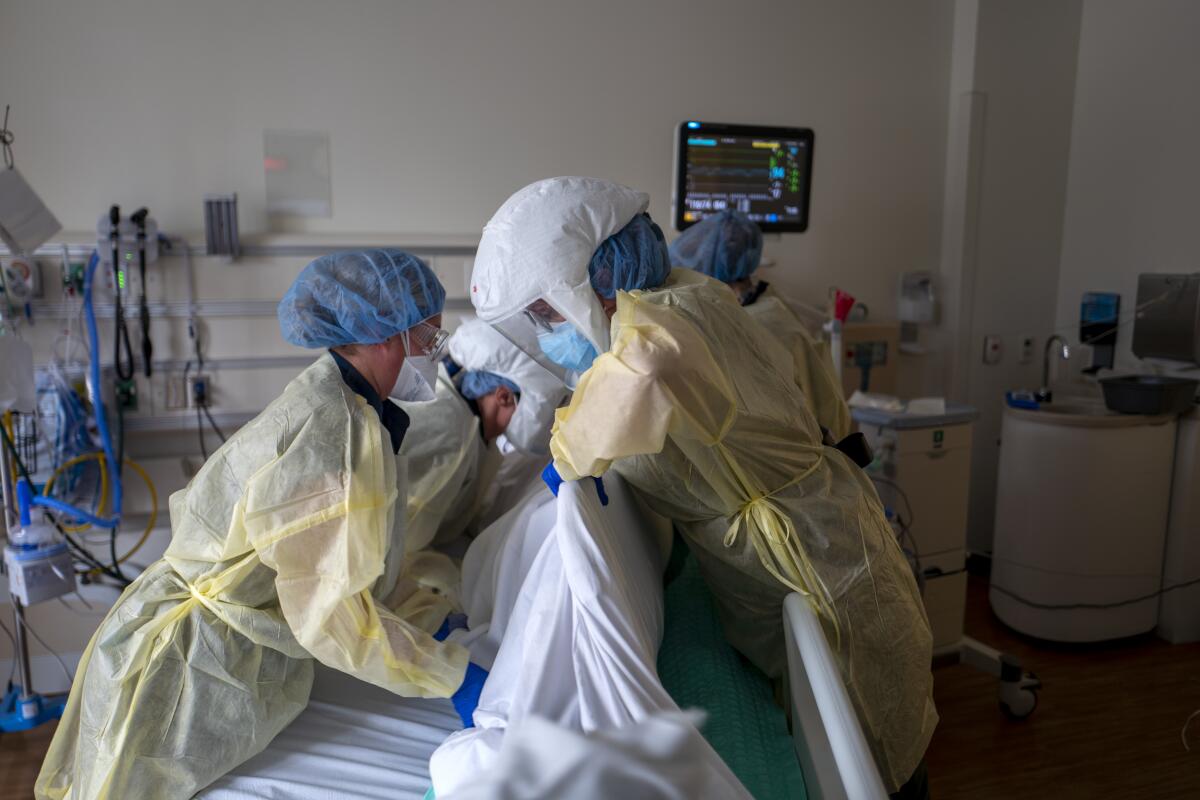
Then the Delta surge hit this summer. Hemmed in by relatively low vaccination rates among younger adults and bans on mask mandates, Florida’s hospitals became overwhelmed. Now the state’s cumulative COVID-19 death rate is 49% worse than California’s.
The Golden State has benefited from its willingness to adopt new policies throughout the pandemic, including COVID-19 vaccine mandates and, in many counties, indoor mask requirements, UC San Francisco epidemiologist Dr. Kirsten Bibbins-Domingo said.
States like Florida have shown “a real desire not to adopt any of these other strategies, and in fact, highly politicizing these other strategies,” Bibbins-Domingo said.
Trying out new control strategies as the Delta variant hit was essential, she said.
“The Delta variant threw [California] a big curveball, and all of a sudden, it meant that the margins for error — the margins that were — we didn’t have them anymore,” Bibbins-Domingo said. “And so even though we had high vaccination rates, they were not going to be high enough. And we were going to have to do something else in order to keep the rates low.”
Higher vaccination rates and mask use indoors “have helped to blunt this fourth surge in California as compared to Florida,” said Dr. Robert Kim-Farley, medical epidemiologist and infectious diseases expert at the UCLA Fielding School of Public Health. “We are seeing better application of public health measures in California compared to Florida.”
Of the nation’s 10 most populous states, Florida now has the second worst cumulative COVID-19 death rate since the pandemic began, with 262 deaths for every 100,000 residents. Only New York has a higher death rate — 281. California’s rate is 176.
Florida’s position deteriorated dramatically from the last day of winter, when it had the eighth worst death rate among the 10 most populated states. By contrast, California has remained in ninth place among those 10 states.
In other words, if California had Florida’s cumulative COVID-19 death rate, an additional 34,000 residents would have died. And if Florida had California’s death rate, 18,000 fewer would have died there.
One likely reason for varying pandemic outcomes is the dramatically different vaccination rates among young people.
At first glance, California and Florida don’t have vastly different rates of vaccination: among everyone age 12 and older, 83.8% in California have received at least one dose, as have 76.7% in Florida.
But while Florida’s seniors have been vaccinated at even greater rates than in California, Florida’s younger people are vaccinated at significantly lower rates.
In California, 76% of adults age 18 to 49 are at least partially vaccinated, but in Florida, only 61% of adults age 20 to 49 have received at least one dose.
That’s a big difference, said Dr. Monica Gandhi, a UC San Francisco infectious diseases expert.
Rates of new daily COVID-19 hospitalizations in Florida were four times worse than in California for every adult age group during the height of the summer Delta surge — except for those age 70 and up, which was three times as bad as California’s. During the states’ respective peaks of the surge, for every 100,000 residents in their 30s, about 2 Californians were being newly hospitalized daily for COVID-19, as were 8 Floridians, according to CDC data.
Subscribers get early access to this story
We’re offering L.A. Times subscribers first access to our best journalism. Thank you for your support.
A high number of coronavirus cases among younger adults — who are more likely than seniors to go out to work and socialize — will increase coronavirus transmission to such an extent that the virus will be more likely to find people who are older or have underlying health conditions, and are more likely to die if they are infected, especially if they are unvaccinated.
Elevated levels of coronavirus transmission also increase the odds of a breakthrough infection among vaccinated people. And elderly people are more likely to suffer from severe complications of COVID-19, Gandhi said.
In contrast to Florida, where vaccine mandates are banned, elected leaders in many parts of California have embraced targeted requirements, such as for healthcare workers and college students; in some cities, inoculations are needed to enter restaurants and gyms.
In mid-July, the University of California system ordered vaccinations for all students and faculty. Around the same time, some bars in Los Angeles and San Francisco began implementing their own requirements for customers to show proof of vaccination to enter, acting weeks before local officials in both regions imposed a similar requirement through health orders.
By mid-summer, California was issuing orders for healthcare workers to be vaccinated and for school employees to be vaccinated or test weekly. Los Angeles city and county officials, as well as the city of San Diego, ordered their own government employees to get fully vaccinated unless granted an exemption for medical or religious purposes.
Those requirements are likely nudging more people to get vaccinated.
L.A. City Council considers a stricter COVID-19 order requiring visitors to restaurants, gyms, malls, salons and elsewhere to be fully vaccinated.
“We were the first to put in vaccine mandates in the entire country,” Gandhi, who sees vaccine requirements as essential to ending the pandemic, said of California. “A public health crisis demands that we all get vaccinated for each other,” Gandhi said. “That’s what happened with the smallpox pandemic in 1905,” when too many people weren’t getting vaccinated.
Some epidemiologists and infectious diseases experts say Florida was hurt by leaders there making statements contradicting leading scientists and the U.S. Centers for Disease Control and Prevention, which advised by late July that masks again be worn in indoor public settings.
University of Florida epidemiologist Cindy Prins has been tracking coronavirus numbers and saw in real time how, by late June, “it was looking like we were going in the wrong direction” as the Delta variant was emerging among cases in the state. While the state had gotten down to 10,500 cases a week by June 11, Prins found that by July 2, cases were at 23,000, and then up to 45,000 a week later.
DeSantis, Florida’s governor, has made statements contradicting the CDC, stating in an executive order that “forcing students to wear masks lacks a well-grounded scientific justification.” There is plenty of evidence suggesting masks help: A study published last week by the CDC found that, in Arizona’s two most populous counties, schools without mask requirements were 3½ times more likely to have coronavirus outbreaks than those with mask rules.
Last week, DeSantis appointed a new surgeon general, Dr. Joseph Ladapo, who has opposed the kind of targeted vaccination requirements that have been supported by the CDC’s director, Dr. Rochelle Walensky, as being effective.
The coronavirus’ Delta variant has upended the calculations of economic forecasters at UCLA, who have dampened their expectations for economic growth in California and across the country.
In Florida, Prins said, she and other public health experts found their work and expertise criticized, misconstrued and politicized around the issue of masking, vaccine efficacy and the merits of social distancing.
“It just feels disheartening sometimes, because I see that when some folks don’t take advice that I feel so strongly and know ... and then they get very sick, or they die,” Prins said. “I wish that people would really listen to the science.”
The Delta variant is far more transmissible than previous strains of the coronavirus, yet Florida’s leaders “kept doing exactly what they were doing,” said Ali Mokdad, an epidemiologist at the Institute for Health Metrics and Evaluation at the University of Washington, which runs a widely cited forecast of pandemic projections. “Quite honestly, the leadership in Florida didn’t take this virus seriously and they let it spread. And that’s what has resulted: more deaths, unfortunately.”
Florida was blessed with some advantages earlier in the pandemic. California’s rate of overcrowding in homes is more than double Florida’s, a huge vulnerability during the winter surge at a time vaccines weren’t widely available. Living in dense multigenerational households made it easy for the virus to spread from workers to family members, continuing a long chain of viral transmission.
Meanwhile, many elderly people in Florida decided on their own to stay home and declined guests, keeping a very vulnerable population safe. “Because of the elderly population, nobody would come — who is going to visit their parents in winter of last year and bring COVID-19 to his family or her family?” Mokdad said.
Mokdad lamented key steps that could’ve inspired more people to get vaccinated. DeSantis, for instance, notably declined to get vaccinated in front of news cameras, and held an event criticizing government vaccination requirements, where he stood along side several workers employed by the city of Gainesville who said the government shouldn’t force them to get vaccinated, according to the Associated Press.
In California, Delta’s arrival led many local health officials to reinstate mask requirements, but in Florida, the “laissez faire attitude that worked” relatively speaking last winter evaporated, Mokdad said. When officials failed to change their strategy, “the Delta variant was able to infect the population.”
Eventually, California and Florida will achieve similar levels of immunity, Mokdad said, but California is on track to achieve it “through vaccination and less suffering and less deaths.”
Further study is needed to determine if overwhelmed hospitals contributed to Florida’s relatively high death rate, or if there are other explanations behind it. For every 1,000 recorded coronavirus cases this summer, 12 people died in Florida, whereas in California, six died.
Comparing states’ COVID-19 death rates can be problematic without more study. California and Florida each has its own vulnerabilities; Florida has an older population, who are more susceptible to severe COVID-19, while California has higher levels of poverty, density and overcrowding, which can contribute to rapid spread of the virus.
There could also be differences in whether cases or deaths are being reported withthe same degree of accuracy.
Los Angeles County Public Health Director Barbara Ferrer said recently that, for the two-week period that ended Sept. 18, L.A. County recorded 4 COVID-19 deaths for every 100,000 residents, while Florida recorded 22.
“In places where sensible steps have not been taken to reduce the spread of the virus, the Delta strain continues to ruin futures and take lives at a rapid pace,” Ferrer said. “Our pandemic history has told us that we make our best progress when we actively take steps to reduce the spread of the virus.”
Some experts hope that ever-rising immunity levels in California will help head off a severe fifth wave of COVID-19 later this fall and winter. But it will be important to decisively counteract waves of misinformation about the safety of the vaccines, which circulate despite the record of safety among the billions of doses administered worldwide.
“There is a lot of deliberate misinformation out on social media that are causing people to unnecessarily hesitate to get vaccinated,” said Dr. George Rutherford, a UC San Francisco epidemiologist. “And I would hope we could get by that.”
Times staff writer Luke Money contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.