Too many ‘shiny objects’: Why it’s risky to promise a coronavirus vaccine and cure

- Share via
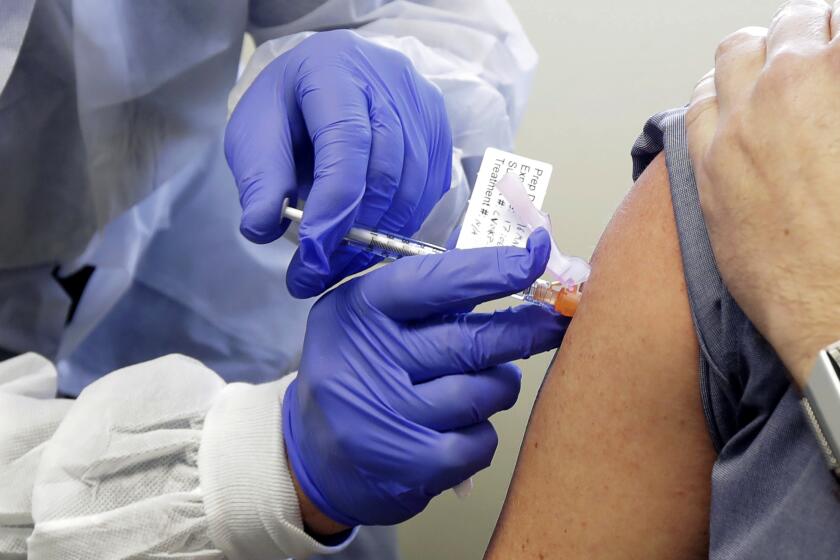
A surge of optimism has followed each recent announcement about possible cures and vaccines for COVID-19, including this week’s disclosure of a treatment that was first developed for the Ebola virus.
But there is a price to pay for promising too much as the economy reels and the world anxiously awaits even a marginally effective therapeutic. Some promising announcements have been followed by reality checks, further muddling the picture about which ones will come to the rescue.
For the record:
6:13 p.m. Oct. 16, 2020A previous version of this story incorrectly stated that the novel coronavirus has DNA; the virus’s genetic information is encoded in RNA.
The latest came this week after Dr. Anthony Fauci, the chief of the federal government’s top institute for infectious diseases, indicated that an anti-viral drug developed by Bay Area biotech giant Gilead Sciences sped up by several days the recovery of about half the people with COVID-19.
That same day, however, the celebration was tempered by news that China had tested the same drug, used effectively against Ebola, and had found no benefit against the disease. In addition, both tests apparently showed little or no improvement in the fatality rates of those infected.
Research chiefs and health experts around the world said in interviews that they are confident drugs to help treat the sick will be available within this year, with an effective vaccine coming by next year. But the research is still far too early to decide which set of drugs will work.
“We can’t move day to day and press conference to press conference to the next shiny object,” said Peter Pitts, a University of Paris visiting professor and former FDA associate commissioner. Gilead’s drug, known as remdesivir, “is not a game-changing proposition for any person or any nation, but it could help seriously ill people and lord knows some good news is appreciated these days.”
Ultimately, a successful drug to treat infected people would have to result in significantly fewer deaths, said Wayne Chanon, chairman of United Kingdom-based Stabilitech Biopharma Ltd., which is developing its own novel treatment.
With more than 100 organizations working on vaccines and drugs to prevent or cure the disease, there are bound to be a large set of failures and a number of possible winners. Scientists say it is vital to have more than one drug type to fight the disease.
“What we want is not to put all our eggs in one basket,” said Kate Broderick, research director at the San Diego lab of Inovio Pharmaceuticals, the second drug company to begin human testing of a drug. “We need to try many different options, because we need a solution as soon as possible.”
The virus, formally known as SARS-CoV-2, is both lethal and highly infectious, a combination unlike any respiratory disease in the last 100 years.
When a healthy person walks into a mucous cloud left by an infected individual, hundreds or thousands of individual viruses are inhaled into the respiratory system.
A single virus can initiate the disease, but thousands of them will hamper the body’s immune system to mount a speedy attack on the virus. It is one metric that determines how sick a person will get.
Within hours, the virus begins to replicate itself and release copies to infect other nearby lung cells. Quickly, possibly within a day, a single infected cell can release potentially millions of copies of the virus to begin assaulting the respiratory system.
When sick people go to the hospital, little can be done for them beyond making sure they are hydrated and provided oxygen. Some experts say the rush to build respirators was probably not a great investment, because death rates of patients on those machines are so high.
Despite all that is known about the virus, great mysteries remain, even exactly how it causes death. In some cases, the infection travels from the sinus and bronchial tubes into deep lung tissue, triggering severe pneumonia that drowns the victim. But in other cases, the virus triggers an immune overreaction known as a cytokine storm that begins to attack healthy tissue and can lead to organ failure throughout the body.
Scientists see a wide range of options in combating COVID-19.
Research teams are attempting to help individual cells use their innate self-defense capabilities to fight the initial entry of the virus. Others teams are trying to give coded information to the body’s immune system to understand how to produce antibodies that can fight the disease. And others still are trying to find molecules that can be put into the human body that will bond to the virus and disable it.
The researchers are attacking the problem with myriad cutting-edge techniques, genetic sequencing, sophisticated mathematical models and the fastest super-computers in the world.
As researchers race to develop a vaccine for COVID-19, the potential for the coronavirus to perpetually rebound has ramped up the urgency in finding a worldwide cure.
Jacob Glanville, chief executive of Bay Area-based Distributed Bio and a scientific adviser to Stanford University and UC San Francisco, is pursuing both a vaccine and an antibody drug. The latter could be ready by August, he said.
The company took five known antibodies that were effective against severe acute respiratory syndrome, the SARS epidemic of 2002-03, and ran computations of billions of mutations to find a structure that could attack the new coronavirus, he said. The potent molecules were recently sent for animal tests in labs around the world.
“Our feeling is that the crisis is sufficiently resolved when you have an antibody treatment,” Glanville said.
Inovio is taking a different approach, creating segments of genetic code from the coronavirus. The code would tell the human immune system how to create antibodies that would fight the virus when it appears, said Broderick, the research chief. The entire package was synthesized within a day after the research team had examined the genetic code of the virus, she said, and was the second treatment in the U.S. to enter human trials.
“I like to think of our DNA medicine like an FBI wanted poster,” she said. “If you see this bad guy, attack it.”
Meanwhile, Oxford University, Johnson & Johnson and several Energy Department laboratories that conduct bioterrorism research are looking at other approaches. Thousand Oaks-based Amgen is working on an antibody therapy as well.
Another team of academic experts is looking at how individual cells defend themselves against a virus, before the human immune system can mobilize.
Research by Charles Brenner of the University of Iowa, Anthony Fehr of the University of Kansas and Michael Cohen of Oregon Health & Science University are examining the role of a substance central to cell metabolism, known as nicotinamide adenine dinucleotide, or NAD.
When a cell is attacked by a coronavirus, the NAD is used up in the fight, weakening the cell. The team is trying to assess whether a dietary supplement known as niagen can boost NAD and help fight the virus. Niagen is produced by Los Angeles-based ChromaDex.
“The type of immunity we are investigating is innate to the cell, not depending on antibodies,” Brenner said. “The cell has an immune defense system that gets turned on that uses up the NAD.”
In the United Kingdom, Stabilitech Biopharma Ltd. Is investigating a treatment that targets the body’s mucous membranes, the first line of defense against infections, said company chairman Wayne Channon.
The company has taken a harmless virus common in the human body and modified its genetic structure to include two genes that are responsible for the now famous spikes in the coronavirus. It is formulated into a pill that, when digested, would prompt the immune system to produce antibodies to attack the coronavirus spikes.
The approach requires small amounts of the drug, meaning it would be easier to manufacture for universal consumption.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.