Downey congresswoman backs Antonio Villaraigosa for governor
California farmworkers will have to undergo sexual assault prevention training

Gov. Jerry Brown on Monday signed legislation to ensure farm labor contractors train employees on how to prevent and report sexual assault, a response to a 2013 PBS Frontline investigation that found sexual violence against women was a pervasive problem in California fields.
Senate Bill 295 by Sen. Bill Monning (D-Carmel) makes sexual harassment training mandatory at all businesses that supervise farm employees or provide them with lodging, transportation or other services.
The training has to be conducted or interpreted in a language that employees can understand, the law stipulates, and farm labor contractors will have to provide proof of all of their materials and resources to the Farm Labor Commission as part of the license renewal process.
Under the new law, the state labor commission also will be able to charge a $100 civil fine for any violation of the new requirements.
The PBS Frontline investigative documenatory, “Rape in the Fields, The Hidden Story of Rape on the Job in America” found more than half a million women work in U.S. fields. Most do not have legal residency in the country, and sexual harassment and violence often go unreported. A 2012 Human Rights Watch survey found 80% of 150 women in California’s Central Valley had experienced some form of the abuse.
Los Angeles voters can cast ballots in Assembly race on Tuesday

The political dominoes from U.S. Sen. Barbara Boxer’s retirement are almost done falling.
Her decision two years ago to forgo reelection led to a reshuffling that eventually left vacant a state Assembly seat in Los Angeles.
There are 13 candidates running in the special election, and the primary is Tuesday.
California Politics Podcast: Lawmakers say their focus on housing has just begun
For months, lawmakers in Sacramento said that their effort to pass a package of bills aimed at California’s housing woes was only the beginning.
They repeated that pledge on Friday, even after acknowledging the heavy political lift it took just to pass the simple steps signed into law by Gov. Jerry Brown.
On this week’s podcast episode, we discuss the political and practical impact of the new housing laws, as well as what might be in store for 2018.
We also discuss Brown’s decision to move California’s presidential primary from June to March, and whether it has any hope of making the state relevant in the race for the White House.
Other topics on this week’s podcast include a push for a property tax proposal on next year’s statewide ballot, and a new poll showing a number of likely voters think Sen. Dianne Feinstein should step down when her current term ends.
I’m joined by Times staff writer Liam Dillon and Marisa Lagos of KQED.
Gov. Brown signs major housing legislation
At a signing ceremony in San Francisco on Friday morning, Gov. Jerry Brown signed 15 bills aimed at addressing the state’s mounting housing problems.
“It is a big challenge,” Brown said. “We have risen to it this year.”
The bills could add nearly $1 billion in new funding for low-income housing developments in the near term as well as lessen regulations that slow growth.
Watch live: Gov. Jerry Brown signs bills to tackle California’s housing crisis
Gov. Jerry Brown and state lawmakers are gathered in San Francisco for the signing into law of a package of proposals designed to tackle some of the most pressing parts of California’s housing crisis.
Businesses in California will be required to tell customers exactly how much their automatic renewal will cost
California will require online businesses that offer free trials to tell customers exactly how much an automatic renewal will cost under a law signed by Gov. Jerry Brown on Thursday.
The law’s author, Sen. Bob Hertzberg (D-Van Nuys), thinks the bill, known as SB 313, will make it easier for customers to cancel service.
“Consumers need to know what they are signing up for and that they can just as easily cancel any service or subscription online as when they started it online,” Hertzberg said in a statement.
Streaming services like Hulu and Spotify and the file-sharing site Dropbox have elicited lawsuits and consumer complaints about their automatic service renewals, according to Hertzberg’s statement.
The law goes into effect in July.
Antonio Villaraigosa wants to bring back an urban renewal program to fund low-income housing

California candidate for governor Antonio Villaraigosa wants the state to bring back an urban renewal program to fund low-income housing.
“Solving our state’s growing housing crisis will take a sustained commitment and creative thinking,” Villaraigosa wrote in an op-ed in the San Francisco Chronicle. “But when it comes to giving local governments the tools they need, we don’t need to reinvent the wheel.”
Gov. Jerry Brown and lawmakers eliminated a state redevelopment program in 2011 as a cost-cutting move aimed at saving nearly $2 billion during the state’s budget crisis. The program allowed cities to target run-down neighborhoods for investment and use a share of property tax dollars generated by development to fund improvements, including financing low-income housing. But doing so required the state to spend more to support public schools, and Brown derided the agencies as being rife with abuses of taxpayer dollars.
Villaraigosa, a former mayor of Los Angeles, said a revived program would allow for greater state assistance to address housing problems.
Lawmakers passed a large package of housing legislation earlier this month, including a new real estate transaction fee and a bond measure for the November 2018 ballot. But even with that new spending, state subsidies will remain billions of dollars’ short of what’s needed to finance housing for its neediest residents, according to state and third-party estimates.
Will California Republicans in the House support a tax proposal that would hit their districts hard?

One-third of Californian taxpayers could be forced to pay thousands more in federal taxes from the repeal of one deduction under a GOP proposal released Wednesday, setting up another political dilemma for California Republicans facing tough reelection battles next year as Democrats work to win back the House of Representatives.
The potential repeal of the state and local tax (SALT) deduction, which allows taxpayers to write off those taxes on their federal returns, would hit especially hard in wealthier areas, some of which are on the exact turf Democrats are trying to win over in Southern California.
Details of the overall tax reform plan have yet to be worked out, but so far, vulnerable California Republicans are not joining GOP colleagues in other states who have said they won’t accept the repeal of the deduction, and some of them seem willing to negotiate.
Here’s why California’s early primary in 2020 is destined to pick the next president. (Nah, not really)

Today we answer questions.
Woo-hoo! Now that Gov. Jerry Brown has signed the bill, it looks like California is moving up its 2020 presidential primary. Finally!
Uh.
No more watching from the sidelines as small-fry states like Iowa and New Hampshire throw their weight around.
Um.
I’m already fluffing pillows and prepping the guestroom for all the 2020 hopefuls who’ll be camped out.
Er.
What? You don’t seem too excited.
Look, it would be great if California voted in a truly meaningful presidential primary. It’s been about 50 years since that happened. But it’s about as likely in 2020 as President Trump dumping Vice President Pence and running for reelection on a unity ticket with Hillary Clinton.
How can that be?
Lots of reasons, both political and practical.
Do tell.
Poll: Californians like Obamacare more than ever but are divided on single-payer healthcare

As the latest attempt to repeal the Affordable Care Act fizzles, the law has reached its highest popularity in California in four years, according to a new poll released Wednesday by the Public Policy Institute of California.
Nearly 60% of the Californians hold a generally favorable view of the healthcare law, and just over a third of Californians see it unfavorably — the highest approval rating since PPIC began tracking the law’s popularity in 2013.
But while Democrats and independents back the law, known as Obamacare, with strong majorities, three-quarters of Republicans have negative views of it.
Only 18% of Californians believe congressional Republicans should try again to repeal and replace the Affordable Care Act, and 58% of adults want to see bipartisan efforts to improve the law.
Underscoring the GOP’s challenge in dramatically reducing government’s role in healthcare, two-thirds of the state’s adults believe it is the federal government’s responsibility to ensure that all Americans have health coverage.
But Californians are divided on whether to substantially increase government involvement through a single-payer system, such as the “Medicare for All” proposal recently introduced by Sen. Bernie Sanders (I-Vermont).
A national single-payer insurance program such as “Medicare for All” gets support from 35% of Californians, according to the poll. Support is higher among Democrats — 44% — and independents — 34% — than among Republicans. Only 6% of Republicans back such a system.
But the current system, a patchwork of government and private insurance options, isn’t particularly adored by Californians.
Just under 30% of adults support continuing with a mix of private and public insurance options, while 36% of Democrats, 21% of Republicans and 31% of independents see that mixed system as the best way to provide health coverage.
Half of California’s likely voters think Sen. Dianne Feinstein should retire, poll finds

As Democratic Sen. Dianne Feinstein contemplates a 2018 bid for reelection, a new poll has found that 50% of California’s likely voters think she shouldn’t run again.
Just 43% of likely voters support Feinstein running for a sixth term, according to a Public Policy Institute of California poll released Wednesday. The results are similar among all California adults, not just likely voters, with 46% saying she should not run for another term and 41% saying she should run.
Feinstein, 84, has come under increased pressure from members of California’s left, many of whom were infuriated when earlier this month she called for “patience” with President Trump and refused to back demands for his impeachment.
Still, the poll found that Feinstein remains popular. More than half of likely voters — 54% — approve of the job she’s doing, compared with 38% who disapprove.
That’s on par with Gov. Jerry Brown’s approval rating, and it bests the marks for California’s other Democratic senator, Kamala Harris. When likely voters were asked about Harris, the former state attorney general elected to the Senate in November, 47% approved of the job she was doing in Washington and 30% disapproved. Almost a quarter of voters didn’t offer an opinion about Harris.
The contrasting results on Feinstein are difficult to decipher but at the very least indicate voters remain restless.
“Partly, this is a holdover from last year’s election in which you saw many Democrats wanting a more liberal alternative at the presidential level and you saw many independents wanting an outsider,” said Mark Baldassare, president of Public Policy Institute of California. “As people are looking to next year, there’s a desire for something new.”
Speculation continues that Feinstein may face a Democratic challenger. Among those who have been mentioned is state Senate leader Kevin de León (D-Los Angeles), who is weighing his next political move after he terms out of office in 2018. De León lashed out at Feinstein after her comments about Trump in early September.
In her last election, Feinstein trounced her Republican opponent, Elizabeth Emken, by a 25-percentage-point margin in 2012. She won by almost an identical margin in 2006 when challenged by former Republican state Sen. Richard Mountjoy.
However, California has since switched to a top-two primary system. The two candidates who receive the most voters in the June primary election will advance to the 2018 general election, regardless of their party.
Two Democrats faced off in the finale of California’s 2016 U.S. Senate election, with Harris besting then-Rep. Loretta Sanchez.
Want to see ‘Hamilton’ in L.A.? Rep. Cardenas is raffling tickets as a fundraiser
Rep. Tony Cardenas (D-Los Angeles) is raffling off a set of tickets to “Hamilton” in Los Angeles as a campaign fundraiser.
According to the small print in an email the campaign sent to supporters, one winner will be randomly selected among donors by 11:59 p.m. PST on Oct. 3. The tickets are for the Oct. 19 showing of the hit musical and have an approximate retail value of $824. Entries for the raffle can also be made without donating to the campaign.
Cardenas is friends with the father of Lin-Manuel Miranda, the Tony- and Pulitzer-winning creator of “Hamilton.” When the show opened in Los Angeles in mid-August, Miranda spoke to nearly 1,000 students in Cardenas’ largely Latino San Fernando Valley district.
The congressman isn’t the only one with the idea. Gubernatorial candidate John Chiang is raffling tickets to the Nov. 1 show to those who follow him on Instagram — if they fill out a form on his campaign website.
Barbara Boxer says if Sen. Dianne Feinstein runs for another term, she should expect a tough race

It’s one of the hottest political parlor games in California right now: Will she run again?
Everyone is waiting for Sen. Dianne Feinstein to announce if she’ll seek a sixth term.
And even though they served as colleagues in Washington for more than two decades, former Sen. Barbara Boxer said she has no inside intel on what Feinstein will do in 2018.
“I believe she is running until I see any other indication,” Boxer said Wednesday at a Sacramento Press Club lunch. “Every single race is hard.... Anyone who runs against her will give her a tough race.”
Feinstein, 84, has made clear she is taking her time, even as ambitious politicians eye the seat she has held since 1992. One long-shot Democrat already is raising money for the race, and Feinstein recently drew criticism from California Senate President Pro Tem Kevin de León, who has not ruled out a primary challenge against her.
Boxer said Wednesday her own priority for next year’s midterm election is flipping several Republican-held House seats in Southern California.
“There’s no such thing as an off election year,” she said. “It’s an on year.”
Much of this work will be done through the political action committee Boxer founded, PAC for a Change. The organization also supports electing more Democrats to the Senate and standing up to President Trump’s policies, she said.
Since leaving the Senate in January, Boxer has also given speeches and promoted her book, “The Art of Tough.” She doesn’t like to consider herself a retiree.
Boxer also skirted a question about her pick for governor in a race that already is crowded with several Democrats. All of the candidates, she joked, are “like my sons and daughters.”
California’s top elections officer now says his agency’s website wasn’t the one ‘scanned’ by Russian hackers

Five days after saying he had been told Russian hackers scanned the state’s main elections website for weaknesses in 2016, California Secretary of State Alex Padilla said Wednesday that it turns out it didn’t actually happen that way.
Padilla said that his office was given incorrect information by the U.S. Department of Homeland Security and that the Russian operation was instead focused on “scanning” the network of the state Department of Technology.
“Our notification from DHS last Friday was not only a year late, it also turned out to be bad information,” Padilla said in a statement.
Bryce Brown, a spokesman for the state’s information technology agency, said officials had long known about “suspect activity that occurred on our network last summer” but didn’t know anything else until the notification from federal officials.
“Although we did not have knowledge of the source until now, we have confirmed our security systems worked as planned and the activity was blocked as it happened in 2016,” he said.
The Department of Homeland Security did not respond to a request for comment.
On Tuesday, the Associated Press reported that federal officials also reversed course in a notification they had made to Wisconsin elections officials about Russian activity. In June, federal officials told Congress that 21 states’ elections systems were targeted by Russian activity.
Padilla insisted last week that the “scanning” incident found no vulnerabilities or access to any California voter information, and he criticized DHS officials for the delay in sharing information about 2016 activities. On Wednesday, he said hopes that federal officials will continue to work with the states in preventing cyberattacks.
“I remain committed to a partnership with DHS and other intelligence agencies; however, elections officials and the American public expect and deserve timely and accurate information,” Padilla said.
California moves its presidential primary to March in push for electoral relevance
Backing an effort for California to claim a bigger share of the attention from presidential candidates, Gov. Jerry Brown has signed a bill moving the state’s primary elections to early March.
Brown’s decision, announced without fanfare on Wednesday, means the state will hold its presidential primary on March 3, 2020. It’s a reversal from a decision he made in 2011 to push the state’s primary elections back until June, after years of trying — and failing — to entice major candidates to bring their campaigns to California instead of smaller, more rural states.
Democrats who embraced the push for an early primary said they were motivated in part by the election of President Trump, whose successful bid for the Republican Party nomination was well on its way to reality by the time California voters cast ballots on June 7, 2016.
“We have a greater responsibility and a greater role to promote a different sort of agenda at the national level,” said state Sen. Ricardo Lara (D-Bell Gardens), the author of the bill. “We need to have a greater influence at the national level.”
The new law also moves California’s congressional and legislative primaries to March, a change which some have suggested could make it difficult for challengers to raise money and quickly put together a credible campaign for challenging established incumbents.
Under current projections, California’s primary would come fifth in the presidential nominating process in 2020 — following caucuses in Iowa and Nevada and primaries in New Hampshire and South Carolina. Lara said he realizes that the Democratic National Committee may not like the state moving its election up to the early slot, but that he hopes party officials will work with California officials over the next few years to accommodate the change.
“California’s role has clearly changed,” he said.
California first tried the March primary in 1996. But by election day, 27 states had already held their own presidential primary or caucus, passing over California – one of the most expensive places to buy political advertising time in the nation.
The state’s most successful early presidential primary was in February 2008, when 57.7% of registered voters turned out in a race won by Democrat Hillary Clinton and Republican John McCain. That was the highest voter turnout for a California presidential primary since 1980. But even then, enough states had already voted that the relative impact of the early election was small.
Last year, 47.7% of registered voters cast ballots in the state’s June presidential primary.
Several Democratic lawmakers praised Brown’s decision to allow another try at the early primary.
“Candidates will not be able to ignore the largest, most diverse state in the nation as they seek our country’s highest office,” said Secretary of State Alex Padilla.
The bill does not change the scheduled 2018 statewide primary, which will be held in June.
Brown has one other closely watched bill on his desk with the potential for national political impact: A proposal to deny access to the California ballot for any presidential candidate who won’t release personal tax returns to the public – a not-so-subtle jab at Trump’s refusal to do so in 2016. The governor has until Oct. 15 to act on that, and other, bills passed by the Legislature before it adjourned earlier this month.
UPDATES:
2:54 p.m.: This article was updated with additional information on California’s past attempts to move up its primary, as well as details about the 2016 campaign and comment from Secretary Padilla.
This article was originally published at 1:48 p.m.
ALSO:
California’s Democratic leaders have a plan for thwarting Trump in 2020
Skelton: Brown should junk the presidential election bills on his desk
Hollywood tour buses could get more rules slapped on them under the law Gov. Jerry Brown just signed

Gov. Jerry Brown on Wednesday signed legislation aimed at reining in the proliferation of tour buses offering to take fans to the homes and gathering spots of celebrities in Hollywood and other trendy neighborhoods.
The measure allows cities and counties to adopt rules that restrict the routes or streets used by the tour buses, and prohibit the use of loudspeakers on open-topped buses and vans.
Assemblyman Adrin Nazarian (D-Sherman Oaks) introduced the proposal in response to a report by NBC Los Angeles that found some tour buses were operating unsafely without proper permits. He also cited complaints about topless buses on narrow streets of the Hollywood Hills, Malibu and Bel-Air.
Latino state lawmakers back Antonio Villaraigosa for California governor

The Legislature’s California Latino Caucus on Wednesday endorsed former Los Angeles Mayor Antonio Villaraigosa for governor.
While expected, the nod from the politically influential caucus is a boon for Villaraigosa, a former Democratic Assembly speaker and the only major Latino candidate running for governor. Villaraigosa has lagged behind Lt. Gov. Gavin Newson in early polls and fundraising.
“As Assembly speaker and Los Angeles mayor, Antonio Villaraigosa worked to strengthen our economy, expand our healthcare, improve our schools and invest in strategic infrastructure projects that create middle-class jobs,” Sen. Ben Hueso (D-San Diego), chair of the caucus, said in a statement Wednesday morning.
An intriguing aspect of the endorsement is that one of the most prominent members of the California Latino Caucus is Senate leader Kevin de León (D-Los Angeles). In Sacramento, speculation abounds over whether De León may run for governor, and the Villaraigosa endorsement could indicate De León has other plans for his political future.
Villaraigosa joins a slate of other Latino statewide candidates endorsed by the caucus: Sen. Ed Hernandez (D-Azusa) for lieutenant governor; current appointee Xavier Becerra for attorney general; incumbent Alex Padilla for secretary of state; Sen. Ricardo Lara (D-Bell Gardens) for insurance commissioner; and Assemblyman Tony Thurmond (D-Richmond) for superintendent of public instruction.
California is trying to educate people about marijuana before recreational sales start
Months before California allows the sale of marijuana for recreational use, the state has launched an education campaign about the drug, including highlighting the potential harms of cannabis for minors and pregnant women.
The state is scheduled to issue licenses starting Jan. 2 for growing and selling marijuana for recreational use, expanding a program that currently allows cannabis use for medical purposes.
In response, the California Department of Public Health has created a website to educate Californians about the drug and its impacts, including how to purchase and safely store cannabis.
“We are committed to providing Californians with science-based information to ensure safe and informed choices,” said State Public Health Officer Dr. Karen Smith.
The website, “Let’s Talk Cannabis,” notes it is illegal for people under 21 to buy marijuana for non-medical use and warns that “using cannabis regularly in your teens and early 20s may lead to physical changes in your brain.”
The site also warns that marijuana edibles may have higher concentrations of tetrahydrocannabinol, or THC. “If you eat too much, too fast you are at higher risk for poisoning,” the website warns.
The state urges parents and guardians to talk to their teenagers about legal and health issues surrounding marijuana use.
The state officials also say consuming cannabis is not recommended for women who are pregnant or breastfeeding, or who plan to become pregnant soon, noting that it “can affect the health of your baby.”
The website got good marks from legalization activist Ellen Komp, deputy director of California’s chapter of National Organization for the Reform of Marijuana Laws.
The website is “fairly accurate,” she said, but added, “The risks with pregnancy are somewhat overstated, telling women they should not use cannabis for nausea or even if they are thinking of getting pregnant.”
Some 43% of Californians have used marijuana for recreational purposes and 54% said they have not, according to a USC Dornsife/Los Angeles Times poll last November.
Among those who have not used it, just 2% said they are much more likely to use it if Proposition 64 passed, which it did, while 5% said they are somewhat more likely to use it, and 89% said they are no more likely to smoke pot if it was legalized.
Other advice from the state’s site: driving under the influence of cannabis is illegal and increases the chance of a car accident, and cannabis should be stored in a locked area to avoid poisoning children and pets.
Updated at 11:30 am to include data from poll on marijuana use.
Combustion engines could go the way of the horse and buggy in California, top air regulator says

Imagine a future where only zero-emission vehicles could be registered in California or driven on the state’s freeways.
Those are two tactics that could be used to help the world’s sixth largest economy phase out combustion engines, suggested California Air Resources Board Chair Mary Nichols in a recent interview with Bloomberg.
The state already has far-reaching policies for fighting climate change, but Nichols said Gov. Jerry Brown wants to make sure California is keeping pace with goals set by other countries.
Britain and France plan to ban vehicles powered by gasoline or diesel fuel by 2040, and China recently announced it would set its own deadline.
“I’ve gotten messages from the governor asking, ‘Why haven’t we done something already?’” Nichols said in the Bloomberg interview. “The governor has certainly indicated an interest in why China can do this and not California.”
The discussion is not a new one for California leaders. Brown signed legislation last year requiring the state to reduce greenhouse gas emissions to 40% below 1990 levels by 2030, but an even more ambitious target was included in a 2005 executive order from Gov. Arnold Schwarzenegger.
To hit the goal of slashing emissions to 80% below 1990 levels by 2050, California would need nearly every new vehicle sold between 2040 and 2050 to produce zero emissions, according to an analysis from the Air Resources Board.
So far, California has struggled to meet more modest goals of getting more electric cars on the road, and emissions from transportation have recently increased.
“Given the existential challenge we face, the administration is looking at many, many possible measures – including additional action on electric vehicles – to help rapidly decarbonize the economy and protect the health of our citizens,” Dave Clegern, a spokesman for the Air Resources Board, said in a statement.
Police body camera footage depicting rape victims won’t be released in California under new law

Gov. Jerry Brown signed a measure Tuesday that would prohibit the public release of police body camera footage or other videos that depict victims of rape, incest, sexual assault, domestic violence or child abuse.
The new law will not change existing policy. Generally, police departments across California don’t release body camera footage outside of a courtroom. This measure, Assembly Bill 459 from Assemblyman Ed Chau (D-Arcadia) enshrines extra protection for such footage into state law.
Lawmakers have struggled to pass more wide-ranging police body camera policies. A bill that would have allowed much more footage to be released did not advance this year.
After meeting with Trump, California Democrats say they want a seat at the tax reform table
Ahead of Republicans’ plans to unveil a more detailed overview of their tax reform plan Wednesday, President Trump sat down with a bipartisan group of members that included California Democratic Reps. Linda Sanchez and Mike Thompson.
Sanchez, of Whittier, who serves on the House committee that has authority over tax legislation, said members didn’t learn much about the details of the plan Tuesday.
“There were kind of generalities but no specificity, which is why we’re interested to see what they put out tomorrow, because clearly it’s not something that’s had Democratic input,” Sanchez said.
According to a White House transcript of part of the meeting, Trump said the plan is focused on making the tax code “simple and fair,” increasing the deduction most families can take, lowering the business tax rate and bringing wealth stored overseas back to the United States.
Thompson, of St. Helena, said the president listened to what Democrats had to say, but he didn’t get the impression that the policy plan would change before it becomes public Wednesday.
“I don’t think it was that kind of meeting. We all agreed we wanted a fair, easy-to-work-with tax code that generates more jobs,” said Thompson, who is also on the committee. “He said repeatedly he wants to be successful.”
Republicans are set to unveil a “consensus document” Wednesday they say will be a much more detailed overview than previous tax policy papers they’ve released. But it is not expected to be an actual plan or bill.
Republicans will huddle with Vice President Mike Pence for half of Wednesday to discuss tax reform. Democrats are holding their own tax reform forum too.
It’s been 30 years since Congress has passed a major tax overhaul, and Republican leaders have set an ambitious timeline for passing a tax-reform measure, indicating they want to get it to Trump’s desk by the end of the year.
Sanchez said she tried to stress in the meeting that Democrats should play a role in writing the final bill. There wasn’t discussion about the group sitting down with Trump again, she said.
“The president was very pleased that it was a bipartisan effort, which sort of confused me because that was the first meeting where there were members of the Democratic side of the Ways and Means Committee there,” Sanchez said. “I don’t know if they’ve been telling him that the process is bipartisan or if he knew it wasn’t bipartisan but didn’t care, but I thought that was kind of odd.”
Tom Steyer won’t rule out challenging Sen. Dianne Feinstein, but warns against reading too much into that

Billionaire environmentalist Tom Steyer did a little political two-step Tuesday when a reporter pressed him on whether he might challenge Democratic Sen. Dianne Feinstein if she runs for reelection.
Capital Public Radio’s Ben Adler tweeted that he asked Steyer if he would rule out running against Feinstein, and that Steyer would not nix the idea. Steyer was visiting a Sacramento high school to encourage students to register to vote.
Steyer quickly added that he hates answering speculative questions such as the one posed to him because there’s always a chance it might “bite you in the rear end.”
“I’d rather come out with what I do want to do as opposed to eliminating all the things I don’t want to do,” he told Adler.
Steyer, a Democrat who has openly contemplated a run for governor, said he is still weighing his political prospects and has not decided if he will run for office in 2018.
Feinstein has been facing increased pressure from progressive activists who believe she’s out of touch with her constituents. That intensified earlier this month when Feinstein refused to back the impeachment of President Trump, instead calling for “patience” during his presidency, which prompted a rebuke from state Senate leader Kevin De León.
Feinstein has been coy so far about whether she’ll retire or run again in 2018, but she does have a hefty $3.5 million in campaign funds socked away.
Judge rewrites summary of proposed gas tax repeal initiative, saying it was ‘fundamentally flawed’

A judge on Monday rewrote the title and summary for a proposed initiative that would repeal recent gas tax increases in California. He rejected a title and summary written by the state attorney general’s office as “fundamentally flawed.”
Sacramento Superior Court Judge Timothy M. Frawley criticized the attorney general’s office for not mentioning in the title that the ballot measure would repeal newly approved taxes or fees.
“This is not a situation where reasonable minds may differ,” Frawley wrote in his ruling. “The Attorney General’s title and summary ... must be changed to avoid misleading the voters and creating prejudice against the measure.”
The initiative proposed by Assemblyman Travis Allen (R-Huntington Beach) would repeal a bill approved in April by the Legislature and governor that would raise the gas tax by 12 cents per gallon and increase vehicle fees in order to generate $5.2 billion for road repairs and to improve mass transit.
The title and summary will be placed on petitions to be circulated by those trying to qualify the measure for the November 2018 ballot. The title and summary are also placed on the ballot if enough signatures are collected.
The original title written by Atty. Gen. Xavier Becerra’s office was: “Eliminates recently enacted road repair and transportation funding by repealing revenues dedicated for those purposes.”
Allen’s attorneys argued the voter could read that to mean that the Legislature identified existing funds for transportation and the initiative would take those funds away.
The judge’s title says: “Repeals recently enacted gas and diesel taxes and vehicle registration fees. Eliminates road repair and transportation programs funded by these taxes and fees.”
The judge also made it clear in the summary that an Independent Office of Audits and Investigations that would be eliminated by the initiative is “newly established.”
Representatives of the attorney general’s office were not immediately available to comment on whether the ruling would be appealed.
Democrats to try to force vote on Dream Act with rarely successful procedural move
House Democrats are trying to force a vote on Rep. Lucille Roybal-Allard’s version of the Dream Act, they announced in a news conference Monday.
The House and Senate have less than six months to address the legal status of people brought into the country illegally as children before the program protecting them from deportation ends in March.
In the weeks since President Trump announced he was ending the Deferred Action for Childhood Arrivals program, Democrats have pushed for a quick vote on Roybal-Allard’s bill, which is backed by every House Democrat and four Republicans. There are also a handful of other Republican-sponsored bills that could be considered.
To force a vote, Democrats would need a majority of the House — 218 members — to sign what’s called a discharge petition to pull the bill from the House Judiciary Committee and bring it to the House floor.
Roybal-Allard, a Democrat from Downey, said she believes there is enough support to pass the bill if Democrats can get it to the House floor. Democratic leaders said they expect all House Democrats will sign the petition.
“The American people overwhelmingly oppose deporting our ‘Dreamers,’” Roybal-Allard said. “But the Republican leadership is ignoring the wishes of a majority of the American people.”
Democrats hold only 194 seats, and would have to convince 24 Republicans to buck their party leaders and sign the petition.
House leaders control which bills come to the floor for a vote and when. Although discharge petitions have been used in the past to shame congressional leadership into letting a bill move forward, the procedural move is rarely successful.
This month, Republican Rep. Mike Coffman of Colorado filed a discharge petition for the Bridge Act, a Republican- sponsored bill to address the legal status of people brought to the country illegally as children. Five members of Congress had signed on as of Monday.
FOR THE RECORD
Sept 26, 12:38 p.m.: An earlier version of this post identified the member of Congress who filed a discharge petition for the Bridge Act as Rep. Mike Thompson. It was Rep. Mike Coffman.
California lawmakers grant some megaprojects relief from environmental law, but not others

When professional sports team owners, Facebook and big developers have asked California lawmakers for some relief from the state’s main environmental law over growth, the answer usually has been yes.
The law, the California Environmental Quality Act, requires developers to disclose and reduce a project’s effects on the environment — a process that often can get tied up in lengthy litigation.
This year, legislators passed a measure aiming to shorten any potential environmental lawsuit against Facebook’s expansion of its headquarters, two skyscrapers planned in Hollywood and other megaprojects to less than nine months. Doing so has led many to question why only big projects get such relief.
The fate of California’s biggest campaign donor disclosure bill may hinge on some small details

You wouldn’t expect to see the leader of California’s campaign watchdog agency rooting for Gov. Jerry Brown to veto sweeping new disclosure rules for political donors. And yet, that’s where things stand in a seven-year debate over helping voters follow the money.
“I think we can do better than this bill,” said Jodi Remke, chair of the California Fair Political Practices Commission.
Remke and her staff have raised a red flag about the fine print tucked inside Assembly Bill 249, the “California Disclose Act,” that rewrites rules for campaign contributions that are “earmarked.”
Bay Area Rep. Eric Swalwell backs Gavin Newsom for governor
Oceanside lifeguard receives California’s highest public safety honor

An Oceanside Fire Department officer who risked his life to save a boater received the state’s highest award for public safety officers on Monday.
Gov. Jerry Brown and Atty. Gen. Xavier Becerra presented David Wilson with the Public Safety Medal of Valor at a ceremony at the state Capitol.
In July 2016, Wilson rescued a man whose boat crashed into a jetty in Oceanside Harbor. The victim was barely conscious and jammed between two rocks. With only a short window between each set of waves, Wilson dove underneath the water and swam into the boulders to free the victim’s legs.
“You earned it,” Brown said at the ceremony. “You were assaulted by the waves and the rocks, and you went ahead anyways. That’s why you are the only one getting a medal of honor.”
A review board made up of law enforcement officers reviewed 21 nominations for the Medal of Valor.
The award is given out once a year. There can be more than one recipient, but this year Brown chose one.
California joins 11 states to oppose one of the ways Ohio cancels a voter’s registration

California’s attorney general joined a group of other states on Monday to ask the Supreme Court to abolish a controversial policy in Ohio that cancels a voter’s registration for not frequently casting a ballot.
A federal appeals court earlier this year found the Ohio practice to be illegal. Though California doesn’t use a similar process, state Atty. Gen. Xavier Becerra signed on to a court filing with 11 other states and the District of Columbia to urge the justices to uphold the lower court’s ruling.
“Removing eligible voters from registration lists serves to silence and suppress citizens,” Becerra said in a written statement. “All too often, state policies like the one we’re opposing in Ohio make it harder for our most vulnerable citizens to vote.”
The case centers on Ohio’s practice of sending a registration notice to those who don’t cast any ballot in a two-year period. If a voter doesn’t respond or vote over the following four years, his or her registration is canceled.
In California, elections officials generally remove voters from their lists only if there’s proof the person has died or if it’s clear through other research methods that he or she has moved. Otherwise, those who don’t cast ballots over a period of time are moved to an “inactive list” of voters.
“Aggressive purging of voter rolls jeopardizes the fundamental rights of American citizens,” California Secretary of State Alex Padilla said in a written statement. “States should not have free rein to kick voters off the rolls merely because they sit out elections.”
Ohio elections officials maintain that the system has been in use for a number of years, and that it’s been used to keep the lists of voters accurate. Critics who filed the original lawsuit argued that the purging of names has been used selectively in a way that penalizes only certain voters for not casting a ballot.
Put Californians before Republicans on healthcare vote, Dianne Feinstein tells GOP House members

Sen. Dianne Feinstein made a direct appeal to her 14 California congressional Republican colleagues on Monday, asking them to stop the latest GOP healthcare bill if it gets to the House.
The Senate hasn’t scheduled a vote on the plan, and it’s not clear it would pass if a vote was held. But if it did, California House members could determine whether it goes to President Trump’s desk or not.
If it gets through Congress, the Senate bill is expected to have an outsized effect on California, slashing more than $100 billion in federal funding for the state over the next decade and tens of billions more in the years that follow.
“If this bill makes it to the House, you have an opportunity to stop it. I implore you to do so. This is about putting people over politics, Californians ahead of party,” Feinstein wrote in a letter to House Majority Leader Kevin McCarthy of Bakersfield.
Senate leaders want to take up the bill this week because a Senate rule that allows Republicans to pass the bill with a simple majority expires Sept. 30. Democratic senators, including Feinstein and Kamala Harris, oppose the bill.
“While I will do all I can to defeat this bill, I ask that if it passes you put politics aside and vote in the best interest of those you represent and help defeat this dangerous bill,” Feinstein said in her letter. “It is no secret that the bill was drafted to take federal funds from California and other states that expanded Medicaid (in order to cover low-income working adults) and give it to states that put politics ahead of their people and failed to expand Medicaid.”
Many of the state’s conservative-leaning districts benefited the most from Obamacare’s expansion of Medi-Cal to include more low-income adults, a group of people that would likely lose coverage if the bill passes and the federal government no longer contributes as much to pay for their healthcare.
California’s House Republicans all voted in favor of a GOP plan to repeal the Affordable Care Act in May. Several politically vulnerable Republicans said they did so because they believed the Senate would return a bill to the House that would address their concerns with the House bill.
Seven California Republicans face particularly tough reelection campaigns in 2018, in part because their districts backed Hillary Clinton for president in 2018, and many of their opponents have already started using the May vote against them.
7.5 million Californians could lose coverage under latest Obamacare repeal effort, state health insurance exchange says

Californians who get their health coverage on the individual market could face dire consequences under the current Republican effort to dismantle the Affordable Care Act, warned a new analysis released Monday by Covered California, the state’s health insurance exchange.
Under the latest plan, which is being led by Sens. Lindsey Graham (R-S.C.) and Bill Cassidy (R-La.), 7.5 million Californians could lose their health insurance by 2027, the analysis said. It also said the repeal could trigger a collapse of the state’s individual insurance market.
“The Graham-Cassidy plan takes resources away from California and from the majority of states, which means that far fewer Americans would have insurance or the existing protections from insurers,” said Peter V. Lee, executive director of Covered California, in a statement.
“The effect on California would be devastating, and lead not only to there being more uninsured people than there were before the Affordable Care Act, but would also cause huge negative impacts on the health care delivery system, the economy and on those with employer-based coverage,” Lee said.
The report comes on the heels of another grim analysis by Gov. Jerry Brown’s administration, which estimated that the Senate proposal would strip California of nearly $139 billion in federal funds from 2020 to 2027.
The Covered California report looked at two different scenarios for how state officials could respond to such a slash in federal dollars. If the state chose to prioritize protecting Medi-Cal, which provides coverage for low-income Californians, the analysis projects the collapse of the individual insurance market by 2021.
If officials chose to direct attention to the individual market by stepping in to cover subsidies now paid for by the federal government, that could lead to large reductions in the Medi-Cal program.
In both scenarios, the result would be up to 7.5 million fewer Californians with health insurance, according to the report.
“Proponents claim Graham-Cassidy gives states flexibility and choice, but in reality it puts states into a lose-lose situation,” Lee said. “Under this plan, California and states across the nation would be forced to either turn their backs on their most needy residents, or let the individual market be destroyed. Either way, millions lose coverage.”
Keep an eye out for these 10 California bills that could become law
In a flurry of floor debates, committee meetings and deal-making to wrap up the first year of the Legislature’s session, lawmakers sent hundreds of bills to the governor’s desk.
While high-profile legislation to make California a “sanctuary state” and address the state’s housing crisis may have stood out, other bills that can have an effect on daily life could also become law.
Here are 10 bills awaiting Gov. Jerry Brown’s signature:
- Landlords won’t be able to threaten to deport immigrant tenants
- Students could attend their first year at community college for free
- Knowingly exposing a sexual partner to HIV would no longer be considered a felony
- People who smoke pot while driving or riding in a car could be punished by fine
- Parks and beaches would be tobacco- and marijuana-free
- Taxpayers could pay $270 million if the Los Angeles 2028 Olympic bid goes over budget
- There may be a gender-neutral option for state driver’s licenses
- New parents at small businesses could get 12 weeks of leave to care for a new child
- California teachers could get paid pregnancy leave
- Public schools with low-income students might provide free menstrual products
Democrats make it clear the Golden State Warriors are welcome in the state Capitol
The Golden State Warriors may not be swinging by the White House to mark their 2017 NBA championship, but they’ll still be feted in the state Capitol.
Democratic legislators took to Twitter over the weekend to make clear the Warriors would be welcomed in Sacramento, after President Trump tweeted on Saturday that a White House invitation was “withdrawn” due to star point guard Stephen Curry’s disinclination to visit the president.
State Sen. Nancy Skinner (D-Berkeley), whose district includes Oakland, the team’s hometown, said the Warriors were invited to the state Capitol well before the Twitter fracas, as is customary whenever California teams win a national championship.
But she said it was important to reiterate that invitation in light of Trump’s comment.
“Look at the amount of tweets that guy sends out. No way do we respond to every tweet,” Skinner said. “But when it’s to disinvite the three-time NBA champions, that deserves a response.”
No date for a Warriors visit has been set as of yet.
Skinner lauded the team’s handling of Trump’s tweet, pointing to a statement in which the Warriors said they’d find ways to “celebrate equality, diversity and inclusion” on their trip to Washington.
“While of course as Californians, we’re incredibly proud that it’s a California team that won the NBA championship, there’s
even that much more pride that it’s a team that lives and expresses those values that we try to put into practice every day,” she said.
Senate President Pro Tem Kevin de León (D-Los Angeles) also chimed in with an invitation.
Attorney running against Sen. Dianne Feinstein is hosting Hollywood fundraiser
Pat Harris may be a long-shot candidate for U.S. Senate, but he’s not fundraising like one.
On Monday Harris, a Democrat challenging Sen. Dianne Feinstein, is set to tread territory familiar to many prominent statewide candidates looking for cash: the Hollywood fundraiser.
The event is to be held at the Catalina Jazz Club on Sunset Boulevard and is being billed as a CD release party for Carol Welman, a jazz musician and Harris’ wife. Tickets range from $150 for a single ticket to $2,700 for a VIP dinner for two. (An email to Welman’s subscriber list earlier this week advertised tickets for as little as $30).
Harris announced that he was running last month on a platform that includes support for single-payer healthcare and a pledge that he will only take campaign donations from individuals.
Facing pressure from progressive activists, Feinstein has been coy so far about whether she’ll retire or run again in 2018. Either way, she’s stockpiled $3.5 million in her campaign war chest. As of June 30, Harris had raised no money except for $104,685 he loaned his own campaign.
Three other candidates have also filed to run against Feinstein: Democrats Steve Stokes and David Hildebrand, and independent Jerry Carroll.
Rep. Keith Ellison headlines dinner for Orange County Democrats, who declare ‘orange is the new blue’
The focus was on 2018 as Orange County Democrats gathered Saturday night in Costa Mesa to bask in their high hopes here.
Headliner and deputy chairman of the Democratic National Committee, Rep. Keith Ellison of Minnesota, urged unity as dozens of Democrats navigate crowded primaries throughout the state.
The theme of the annual awards dinner was “Orange is the New Blue,” a twist on the title of a popular Netflix show and the latest indication of Democrats’ rosy outlook as they try to flip the county’s four GOP-held House seats next year.
Ellison told the crowd it was “not the proper role” of the DNC to choose among the many primary contenders. “But you will sort it out running spirited campaigns, you will sort it out over ideas, and when it is over we need you to hold hands and support the Democrat.”
Ellison pushed for a return to grass-roots organizing and outreach to voters of all stripes — and not just during election years.
“We cannot come a month before the election, tell them ... ‘Come vote for us,’” Ellison said. “We’ve got to be in their lives in a physical, palpable way. Then we do have to have the right words, we do have to stand up for them.”
In an interview, Ellison also stressed the need to pass legislation for young people brought to the country illegally who were allowed to stay and work under the Obama Administration’s Deferred Action for Childhood Arrivals program.
Ellison said Democrats are open to negotiating certain immigration enforcement provisions in order pass a replacement for DACA, which President Trump announced he will end in March. But he said Democrats won’t acquiesce to Trump’s demand for a border wall or allow additional capacity for immigration detentions.
“There are certain things that are simply not on the table — the wall or more detention beds, we’re just not doing that,” he said.
California Politics Podcast: Here’s the impact from the state lawsuit against Trump’s border wall plans
Last week’s California lawsuit against the proposed new border wall with Mexico was a dramatic challenge to President Trump. But politically it was very much in line with the narrative that’s been crafted all year long.
On this week’s episode of the California Politics Podcast, we take a closer look at how the new lawsuit may be the biggest moment so far for state Atty. Gen. Xavier Becerra.
We then turn to two other items in the news in which significant challenges have appeared: a rebuke of Gov. Jerry Brown’s controversial plan to build a pair of Northern California water tunnels, and some closely watched bills that quietly fizzled in the final hours of the California Legislature’s 2017 session.
I’m joined by Times staff writer Melanie Mason and Marisa Lagos of KQED News.
California Republican won’t say if he supports Graham-Cassidy healthcare bill
Orange County Rep. Ed Royce was noncommittal about his stance on the controversial Graham-Cassidy healthcare bill designed to roll back provisions of the Affordable Care Act.
“I have not looked at the details in it,” Royce said as he arrived at an event at his Yorba Linda campaign office. “We’ll see if something passes out of the Senate.”
California’s congressional Republicans have stayed mum on the bill so far. An expected vote on the measure in the Senate next week could be stymied by Sen. John McCain’s announcement Friday that he would not support the bill.
Asked about President Trump’s announcement that he was ending the Deferred Action for Childhood Arrivals program, which allowed young people who came to the country illegally as children to stay and work, Royce said he would try to “work out a solution in tandem with border security.”
Royce addressed several dozen volunteers at his campaign headquarters Saturday afternoon.
About 40 volunteers showed up to knock on doors and make phone calls for his reelection campaign. He already has drawn more than half a dozen challengers as Democrats attempt to reclaim the House. The Royce campaign office has been up and running for a couple of months.
It’s rare for a congressional incumbent to begin campaigning so early in an off-year, but Royce is one of nine California Republicans deemed potentially vulnerable in 2018.
Earlier in the day, several dozen protesters showed up to picket outside and protest Royce’s vote to repeal Obamacare earlier this year.
One of the protesters returned hours later, when Royce showed up at the office. She also asked about his position on the Graham-Cassidy bill.
“We’re going to see what legislation comes out,” Royce told her.
Russians tried to find weaknesses in California’s election website last year, say state officials

California’s chief elections officer said U.S. government officials believe Russian hackers tried to find weaknesses in the state’s election website during the 2016 campaign, but that there’s no evidence their effort was successful.
Secretary of State Alex Padilla said the Department of Homeland Security only told him on Friday of last year’s attempt. He described the attack as a “scanning” of the state’s website in hopes of finding weaknesses in its computer network.
“Our office actively monitors scanning activity as part of our routine cybersecurity protocols,” Padilla said in a statement. “We have no information or evidence that our systems have been breached in any way or that any voter information was compromised.”
Those involved were “Russian cyber actors” according to Padilla’s description of information he received from federal officials. In June, a top federal official told the Senate Intelligence Committee that systems in 21 states were believed to have been scoured by cyberattackers.
The election website, www.sos.ca.gov, contains public information about voting procedures as well as data on past election results and current issues. More sensitive data, including the electronic files of some 17 million registered voters, are not included on the website.
A leaked National Security Agency document earlier this year outlined a Russian effort to hack into devices made by a Florida-based voting software company. One California county, Humboldt, used the company’s software, but did not find any evidence of tampering.
Padilla, a frequent critic of President Trump’s special panel investigating the potential of voter fraud, said federal officials should have notified him much earlier of the attempted breach.
“The practice of withholding critical information from elections officials is a detriment to the security of our elections and our democracy,” he said.
Antonio Villaraigosa jabs at Gavin Newsom over his apparent embrace of single-payer healthcare bill
Supporters of a measure to establish single-payer healthcare in California were thrilled by Lt. Gov. Gavin Newsom’s embrace of their bill on Friday, but a rival gubernatorial campaign was less impressed with his position.
A spokesman for former Los Angeles Mayor Antonio Villaraigosa accused the lieutenant governor of flip-flopping because after Newsom was asked if he explicitly endorsed the legislation — Senate Bill 562 — he responded that he endorsed “getting this debate going again.”
“This is an outrageous parsing of words when millions of people are at risk of losing their healthcare,” Villaraigosa spokesman Luis Vizcaino said in a statement.
“It is a yes or no question, lieutenant governor. Are you for SB 562 or not? The nurses and California voters deserve the truth,” Vizcaino added.
The question of backing SB 562 is thorny since it was shelved earlier this year after Assembly Speaker Anthony Rendon (D-Paramount) called it “woefully incomplete.” Backers have said they’d be willing to make changes to the measure, but the contours of those proposed changes have not been made public.
Vizcaino said Villaraigosa “has always supported universal healthcare and the concept of single payer,” but agreed with Speaker Rendon that the bill couldn’t be sent to the governor without a funding plan.
Speaking to reporters, Newsom said he saw a single-payer system in which the government covers healthcare costs as the best way to achieve universal coverage and said he would be “actively engaged in designing and developing it” if SB 562 does not pass next year.
RoseAnn DeMoro, executive director of the California Nurses Assn./National Nurses United, said she saw Newsom’s remarks as a clear endorsement of their measure and a stance she said was not surprising.
“We always knew Gavin would support our bill,” DeMoro said.
She lambasted Villaraigosa — who does not support SB 562 — for criticizing Newsom, whom her group endorsed nearly two years ago.
“I want Villaraigosa to explain to the Latino community why he doesn’t think they should have ... comprehensive healthcare,” she said. “Villaraigosa’s being disingenuous. He knows better. He’s just politically posturing trying to find a wedge issue and he knows better.”
UPDATE
4:32 p.m.: This post was updated with an additional statement from Villaraigosa’s spokesperson on the former L.A. mayor’s support for universal healthcare.
In San Francisco, Bernie Sanders plays two roles: Obamacare defender and single-payer advocate
Sen. Bernie Sanders headed west to drum up support for his recently unveiled “Medicare for All” proposal Friday, but first trained his sights on the Obamacare repeal bill currently gripping Congress.
Sanders (I-Vt.), whose speech was the cornerstone of a California Nurses Assn. gathering in San Francisco, blasted the Republican plan led by Sens. Bill Cassidy of Louisiana and Lindsey Graham of South Carolina as “horrific legislation.”
“How cruel, how immoral it is, to say to those millions of Americans, we are going to take away that health insurance that keeps you alive,” Sanders said.
Sen. John McCain announced on Friday he could not support the measure, dealing the GOP plan a blow. Sanders thanked McCain for his stance, prompting the liberal crowd to cheer the Arizona Republican.
Some Democrats had worried that Sanders’ push for his single-payer plan could distract from efforts to oppose the repeal bill. But the senator was explicit in his appeal to the approximately 2,000 supporters in attendance to focus their energy on defeating the repeal measure.
“Our job is to continue to make sure the Republicans do not get the 50 votes they need ... I beg of you, please, do everything you can to stop the bill,” he said.
Still, the crux of Sanders’ speech focused on his single-payer bill, which he sold as an improvement over the status quo.
“The Affordable Care Act, as we all know, made significant improvements to our healthcare system,” Sanders said, citing the expansion of the number of Americans with health insurance and the ban on insurance companies’ ability to deny coverage to people with preexisting conditions.
“But we must be honest and acknowledge that with all the gains of the Affordable Care Act, it does not go far enough,” he added.
The bill expands the Medicare program to cover the healthcare costs of all Americans with no out-of-pocket payments for patients. The measure does not include a plan to finance such a system, but Sanders has released a report laying out various ways to cover the costs, including a progressive income tax.
During his pitch, Sanders said the implications extended beyond health policy.
“It is a struggle about what this great nation stands for,” Sanders said. “It is a struggle about whether or not every working person in this country has healthcare as a right or whether we allow insurance companies and drug companies to continue to rip us off.”
Graham-Cassidy Obamacare repeal plan ‘devastating,’ could cost California almost $139 billion, state officials warn
Healthcare advisors to Gov. Jerry Brown believe the latest effort on Capitol Hill to repeal the Affordable Care Act would blow a monstrous hole in the state budget, slashing federal health funds by $138.8-billion over a seven-year period.
The estimate, released Friday by the state Department of Healthcare Services, comes on the heels of increased focus on the Republican bill championed by Louisiana Sen. Bill Cassidy and South Carolina Sen. Lindsey Graham.
It is the third time since President Trump took office that GOP lawmakers in Washington have proposed changes to federal health subsidies that would downsize California’s share of federal funds. No firm estimates have been made of the number of state residents who might lose health coverage under the Cassidy-Graham proposal, though earlier efforts from congressional Republicans were estimated to put millions of Californians at risk.
“Simply stated, this proposal is the most devastating of the three federal health care proposals that we have evaluated this year,” wrote Jennifer Kent, director of the Department of Healthcare Services in a memo to Diana Dooley, the governor’s secretary of health and human services.
The report estimates a loss of $4.4 billion to the state budget in 2020 through reduced dollars for Medi-Cal, the state’s version of the federal Medicaid program. By 2026, state officials estimate the annual reduction in health dollars would grow to $22.5 billion.
That moment in time is key, say state officials, because the Senate GOP plan calls for no additional dollars under a new “block grant” healthcare funding plan beyond 2026.
“The Graham-Cassidy proposal represents a significant shift of costs from the federal government to states,” wrote Kent.
The expansion of Medicaid dollars under the Affordable Care Act has had a dramatic impact on reducing the number of uninsured people in the state. Estimates are that almost one of every three Californians is now enrolled in the Medi-Cal program.
With a $183.2-billion state budget, California would have no easy options for replacing even a portion of the missing dollars. The state is projected to have an $8.5-billion “rainy-day fund” by next summer, which would cover only a portion of the lost federal dollars and even then, only for a single year.
“Given our state’s significant population of low-income individuals,” Kent wrote, “this proposal abandons our traditional state/federal partnership and shifts billions in additional costs to California.”
Gas tax foes win victory as they try to get a repeal on November 2018 ballot

In a rare court rebuke of the state Attorney General’s Office, a judge said Friday that the title and summary written for a proposed initiative is misleading — and that he’d do a rewrite himself to make it clear the measure would repeal recently approved increases to gas taxes and vehicle fees.
Sacramento Superior Court Judge Timothy M. Frawley said he would draft a new title and summary to be placed on petitions for the initiative after attorneys for the state and proponents of the ballot measure could not agree on compromise language.
“In this circumstance, I honestly believe that the circulated title and summary that has been prepared is misleading,” Frawley told attorneys during a court hearing Friday. He hopes to release the new title and summary by Monday.
The initiative proposed by Assemblyman Travis Allen (R-Huntington Beach) would repeal a bill approved in April by the Legislature and governor that would raise the gas tax by 12 cents per gallon and increase vehicle fees to generate $5.2 billion annually to fix the state’s roads and bridges and improve mass transit.
Allen and his attorneys said the state attorney general sought to confuse voters with a title that does not use the words “taxes” or “fees.”
The title was proposed to say: “Eliminates recently enacted road repair and transportation funding by repealing revenues dedicated for those purposes.”
Allen, who is running for governor in 2018, said the court decision showed the attorney general was trying to sway voters against the initiative.
“Justice is being served for the voters of California,” Allen said after the court hearing. “I think that he [the judge] has properly seen that the attorney general has tried to intentionally mislead the voters of California because he has tried to prejudice their vote and tried to keep increased taxes for Californians.”
A coalition of business, labor and government officials called Fix Our Roads, which supports the gas tax legislation, had representatives in the courtroom who later criticized Allen for seeking political gain at the expense of California motorists.
“This is more about Travis Allen’s gubernatorial race than anything else,” said coalition spokeswoman Kathy Fairbanks. “He’s condemning voters to driving on potholed roads and being stuck in traffic.”
Allen said the initiative and his campaign for governor are both aimed at giving voters power to fight higher taxes.
“Finally ordinary Californians are understanding that they actually can hold Sacramento accountable,” Allen said. “This is why I’m running to be the next governor of California, because for too long Sacramento has been run by out-of-touch elitists that are coming from Sacramento and the Bay Area of San Francisco.”
A second initiative to repeal the gas tax has been proposed by a different group of Republican activists.
Allen said he supports the second initiative but noted it has to collect many more signatures because it seeks to change the state constitution. “It has a long way to go,” Allen said.
If the judge issues a new title and summary Monday, Allen said the petitions will hit the streets immediately and he is confident they will get the 365,880 signatures to qualify the measure for the November 2018 ballot.
‘We will have universal healthcare in the state of California,’ Gavin Newsom promises single-payer advocates
Lt. Gov. Gavin Newsom has made his most explicit endorsement yet of a controversial single-payer healthcare proposal that has roiled Democratic politics in California.
Newsom appeared Friday before the California Nurses Assn., the most ardent backers of SB 562, a stalled bill to establish a system in which the state would cover all residents’ healthcare costs.
“There’s no reason to wait around on universal healthcare and single-payer in California,” Newsom said. “It’s time to move 562. It’s time to get it out of committee.” The line prompted cheers and a standing ovation from the audience of about 1,500 members of the nurses’ union.
He capped off his remarks with a promise: “If we can’t get it done next year, you have my firm and absolute commitment as your next governor that I will lead the effort to get it done. We will have universal healthcare in the state of California.”
Enthusiastic nurses in the room heard an unequivocal backing of their effort to push forward with the bill.
“When he says he’s going to get this done, he means, seriously, that he will pass SB 562 and make sure that there is healthcare for all Californians,” said Catherine Kennedy, a neonatal nurse from Roseville.
But speaking to reporters after his address, Newsom was less clear in embracing the specifics of the proposal.
“I 100% support moving this process along, getting this debate going again and addressing the concerns, the open-ended issues that the nurses themselves have acknowledged as it relates to the need of going through the legislative process and to fill in the blanks on the financing plan, among other issues,” he said.
President Obama appears in an Assembly race mailer in California — but read it closely
The race to replace Jimmy Gomez, who was elected to Congress earlier this year, has so far been waged by mail and door-knocking in northeast Los Angeles.
Most of the mailers feature local leaders and endorsements from groups including Planned Parenthood and the Sierra Club.
But one mailer that arrived in my mailbox Thursday has a much more familiar face — former President Barack Obama. While it might seem like one to the casual voter sorting through junk mail, this isn’t an endorsement.
“Want to know what kind of job Gabriel Sandoval will do in the Assembly? Listen to the people he’s worked with in the past,” the mailer reads, above Obama’s official White House portrait.
In small type, it notes that Sandoval “served as a Senior Civil Rights Attorney and Senior Advisor” for a White House initiative within the Department of Education.
It features a glowing quote over an image of a July 12, 2013, letter from the president to Sandoval written on White House letterhead.
Healthcare a hot issue in race for California governor

With the hyperpartisan politics surrounding healthcare stirred up by efforts to repeal Obamacare and calls for a single-payer system, both Lt. Gov. Gavin Newsom and former Los Angeles Antonio Villaraigosa are claiming the mantle of healthcare visionary.
On the campaign trail the two Democratic candidates for governor are touting their signature healthcare accomplishments from earlier in their political careers as their bona fides.
For Newsom, it’s about Healthy San Francisco, the nation’s first municipal universal healthcare program, approved while he was mayor; and for Villaraigosa, it’s Healthy Families, which provided healthcare coverage to the children of California’s working poor, legislation he authored as a California assemblyman.
But do they deserve all the credit? It sure doesn’t look that way.
Healthy San Francisco is one of the many topics Newsom is expected to highlight when he speaks to the California Nurses Assn. convention in the Bay Area on Friday morning.
On Thursday night, Newsom took a shot at the latest Republican effort in Washington to roll back the Affordable Care Act – a bill written by Sens. Lindsey Graham (R-S.C.) and Bill Cassidy (R-La.)
“The numbers on this make my skin crawl. Under Graham-Cassidy, an individual with metastatic cancer could see their premiums increase by $142,650. Diabetes? $5,600. Want to tackle the opioid crisis? Gets a lot tougher if an individual suffering from drug dependence sees their premiums go up by $20,450,” Newsom said in an email sent out by his campaign. “This is not a game. Lives are at stake.”
Rep. Duncan Hunter calls for preemptive strike against North Korea

Rep. Duncan Hunter said that the United States needs to launch a preemptive strike against North Korea in order to prevent the rogue nation from harming the U.S. first.
“You could assume, right now, that we have a nuclear missile aimed at the United States, and here in San Diego. Why would they not aim here, at Hawaii, Guam, our major naval bases?” Hunter, an Alpine Republican, said Thursday during an appearance on San Diego television station KUSI.
“The question is, do you wait for one of those? Or two? Do you preemptively strike them? And that’s what the president has to wrestle with. I would preemptively strike them. You could call it declaring war, call it whatever you want,” Hunter continued.
Hunter, a member of a House Armed Services Committee and the subcommittee with jurisdiction over the United States’ nuclear arsenal, did not say whether the military should strike North Korea with conventional or nuclear weapons.
Will Bernie Sanders’ push for ‘Medicare for All’ help or hinder the California effort for single-payer?
When Vermont Sen. Bernie Sanders visited Beverly Hills last May, he made a full-throated appeal for California to “lead the country” and pass a pending state proposal to establish single-payer healthcare.
On Friday, he’ll return to California for a San Francisco speech trumpeting his own higher-stakes plan — a bill to drastically overhaul the nation’s healthcare system by covering everyone through Medicare.
The push for single-payer, in which the government pays for residents’ medical care, has already rattled California’s political landscape. Now, the Sanders measure brings an additional jolt, elevating the issue to a national debate that has implications for the future direction of the Democratic Party and early jockeying in the 2020 presidential race.
One of Jeff Denham’s Democratic challengers drops out
Republican Rep. Jeff Denham of Turlock still has at least nine challengers..
What will Kevin de León do when his term in the California Senate expires next year?

As he gaveled down what may be his last full year as leader of the California Senate on Saturday, Kevin de León had still not said what he planned to do next.
Will he run for governor or U.S. Senate? Does he want to be mayor of Los Angeles some day? De León told reporters they will have to wait to find out.
His advisors, supporters and political observers have their own ideas what De León could do next.
‘Who the hell is Dana Rohrabacher?’ Seth Meyers asks on ‘Late Night’ as he slams the congressman
“Late Night” host Seth Meyers focused on Orange County Rep. Dana Rohrabacher on Wednesday in a segment looking at the Republican congressman’s relationship with Russia, titled “Who the Hell is Dana Rohrabacher?”
The seven-minute segment highlights Rohrabacher’s recent trip to meet with Wikileaks founder Julian Assange, who claims he has evidence Russia wasn’t involved in hacking Democratic emails during the election, then hits on some of Rohrabacher’s other more eccentric moments — his patriotic songwriting, medical marijuana use and musing about whether global warming was caused by dinosaur flatulence.
Rohrabacher’s friendliness toward Russia has drawn increased attention in recent months, especially as his name has popped up on the periphery of the House and Senate investigations into Russian attempts to interfere with the 2016 election.
Rohrabacher is one of nine Republicans whom Democrats have identified as vulnerable in California, and Rohrabacher’s 2018 opponents have tried to use the congressman’s relationship with Russia against him.
One of his challengers, biotech firm chief executive and Democrat Hans Keirstead, made a statement early Thursday on the segment.
“I, like many people in Orange County, wish we could laugh at some late-night TV and then turn it off and move on, but unfortunately Dana Rohrabacher is our representative in Congress,” Keirstead said. “For too long he has put his own career and ideology before the people of Southern California, and it’s time we had someone representing us whose No. 1 priority is the quality of life for the people in our community.”
Rohrabacher did not immediately respond to a request for comment.
Skelton: The presidential election bills on Gov. Brown’s desk may be satisfying politics, but they’re risky ideas
Two presidential election bills are on Gov. Jerry Brown’s desk, sent to him by the Democratic Legislature. Both should be tossed in the trash.
No doubt I’m in the minority on this. These bills do offer some fun, even if they’re flawed.
One has strong pluses that are outweighed by unacceptable minuses.
The second is a mean-spirited “gotcha” bill aimed at the Democrats’ No. 1 enemy: President Trump. It may be satisfying politics, but it sets a risky precedent.
The first bill moves up California’s presidential primary from June to March. Great idea. But it also moves up the state primary along with it. A horrible idea.
The second measure would require all presidential candidates to release their tax returns for the last five years. Anyone who refused wouldn’t be allowed on the California ballot. That’s a sharp poke at Trump, who in 2016 was the first presidential candidate in 40 years not to release his taxes.
Yes, watching Trump squirm would be entertaining. And maybe the tax information would be useful for some voters. But even if the disclosure requirement were constitutional — and there’s substantial doubt about that — it’s a crummy precedent.
This millennial is running as an independent and thinks he can unseat Orange County Rep. Dana Rohrabacher
Orange County Rep. Dana Rohrabacher officially got another challenger this week. Kevin Kensinger, 33, is an investor from Aliso Viejo and is running as an independent in the 48th Congressional District.
Kensinger, who filed papers with the Federal Election Commission this week, says he thinks using an agenda-driven campaign will appeal to members of both parties as well as the district’s growing number of voters who don’t register by party.
(Most voters who identify as independents still tend to vote for one party or another).
“We’re in a purple district that voted for Hillary [Clinton] and Dana [Rohrabacher],” Kensinger said in an interview. “I know a lot of people that could never bring themselves to pull the lever for a Democrat.”
A former Democrat himself, Kensinger says his policy proposals, which include support for single-payer healthcare and allowing states that allow legalized marijuana use to create banking structures that can accommodate the industry, will transcend the district’s 11-point voter registration advantage for Republicans.
“We’re at a crossroads where both parties seem to have lost their direction,” he said. “I believe we have the opportunity to speak to both sides of the fence in this election.”
Rohrabacher is one of nine Republicans the Democratic Congressional Campaign Committee has identified as vulnerable in California. He has faced increasing criticism for his fondness for Russia and antics such as a visit with Wikileaks founder Julian Assange and his comments on the recent violence in Charlottesville, Va.
California Republicans have been mum on Graham-Cassidy bill so far, but this GOP challenger says he supports it
California could stand to lose the most under the Graham-Cassidy healthcare bill that would roll back the Affordable Care Act, which is perhaps why GOP members of Congress have stayed mostly silent on the Republican-backed proposal.
But one congressional challenger, Republican James Veltmeyer, called it a “major step in the right direction.”
Veltmeyer, a physician from La Jolla, is running against Rep. Scott Peters (D-San Diego) in the 52nd Congressional District. “There is a lot of good stuff in this legislation,” he said in a statement Wednesday.
The measure leaves major details to be determined and the Congressional Budget Office likely won’t have time to release a full analysis of the bill’s impacts before the Senate’s scheduled vote next week.
California’s GOP members have not indicated how they might vote if the bill makes it to the House, but all 14 of them voted in favor of repealing Obamacare earlier this year.
Veltmeyer praised the proposal to use block grants to states to fund healthcare, saying it allows states “the flexibility to run their own healthcare systems” and that the repeal of Obamacare’s individual mandate would help create jobs.
Veltmeyer, who has called Obamacare a failure, recently wrote an op-ed supporting a membership-based model of healthcare. Peters is one of four Democrats the National Republican Congressional Committee is hoping to unseat in 2018. Other candidates running in the June primary include Republicans Daniel Casara and Omar Qudrat and Democrat Alexander Miller.
Ads target California’s GOP House members on new healthcare bill but it’s not clear who’s paying for them
Five of California’s House Republicans are being featured in new digital ads urging them to oppose the so-called Graham-Cassidy healthcare bill to roll back Obamacare.
But the newly formed group that’s running the ads isn’t saying where it’s getting the money for them.
The ads, which began running Thursday, highlight the bill’s provisions, saying they would would “gut Medicaid” and get rid of affordable coverage for patients with preexisting conditions.
The nonprofit behind them, SoCal Health Care Coalition, was formed over the last few weeks and is “supported by a diverse group of donors who believe healthcare is a criticial issue for Californians,” according to spokesman Yusef Robb.
Robb declined to identify the group’s major donors or who funded the ads. The group’s website was registered at the end of August, and its social media accounts became active last week.
They are aimed at five Republicans who are being targeted by Democrats in 2018: Rep. Darrell Issa (Vista); Rep. Steve Knight (Palmdale); Rep. Dana Rohrabacher (Costa Mesa); Rep. Ed Royce (Fullerton) and Rep. Mimi Walters (Irvine).
The video ads are part of a five-figure campaign that will reach “hundreds of thousands” of constituents in their districts, Robb said.
All 14 of California’s GOP House members voted for an earlier Obamacare repeal bill. None of them have released public statements about the newest effort, which would likely leave millions more Americans uninsured and hit states such as California the hardest.
Graham-Cassidy is first expected to face a vote in the Senate next week.
California Senate leader preparing for legal fight over ‘sanctuary state’ legislation

Gov. Jerry Brown hasn’t yet signed legislation making California a so-called sanctuary state, but state Senate President Pro Tem Kevin de León is preparing to defend it in court.
In between several immigration events in Washington on Wednesday, De León (D-Los Angeles) said he met with former U.S. Atty. Gen. Eric H. Holder Jr. — who has served as outside counsel to the Legislature for much of the year — “to continue to further discuss inoculating California from [U.S. Atty. Gen.] Jeff Sessions’ Department of Justice.”
Passed early Saturday by the Legislature, the sanctuary state bill would limit state and local law enforcement communication with federal immigration authorities and prevent officers from questioning and holding people on immigration violations.
Sessions has threatened to withhold some federal grant funds from cities and counties that refuse to assist federal immigration agents.
Holder and other former Justice Department lawyers believe the bill is defendable, and if the Trump administration tries to compel California cities to act by withholding funds, it will find itself in court, De León said. Defenders of so-called sanctuary cities often rely on a 1996 Supreme Court ruling that cited the 10th Amendment and found the federal government can’t compel local governments to cooperate with enforcing federal laws.
“It is immoral, and quite frankly un-American, that America’s top law enforcement official would withhold dollars that our local police officers need — precious dollars we need desperately to counter terrorism, to deal with the issue of human trafficking as well as international drug cartels,” De León said.
On Tuesday, Sessions urged Brown not to sign the bill, calling it “unconscionable” and a threat to public safety. Brown responded to Sessions’ comment on CNN by calling the legislation well-balanced.
“It protects public safety, but it also protects hardworking people who contribute a lot to California,” Brown said. He has until Oct. 15 to sign the bill.
De León also shot back against Sessions’ statement that the federal money isn’t an “entitlement,” saying Californians pay more in federal taxes than they receive in federal funding.
“That’s not a gift or a grant from the Department of Justice to California. Those are our dollars; they belong to the people of California,” he said.
California, with alliance of states, pledges to keep pushing climate policies despite lack of federal progress

California and a growing alliance of states committed to fighting global warming said Wednesday that they’re slashing greenhouse gas emissions at the rate required by the Paris climate agreement.
However, the rest of the country would need to join their effort for the United States to actually hit the target of cutting emissions by at least 26% below 2005 levels by 2025.
President Trump has pledged to pull the country out of the Paris deal, but the states reiterated their pledge to keep pressing forward during a news conference in New York.
“We’re all in,” California Gov. Jerry Brown said. “Eventually, Washington will join with us. You can’t deny science forever.”
California’s climate goal is even more ambitious than the Paris target. A law signed by Brown last year requires the state to cut emissions to 40% below 1990 levels by 2030.
California became a founding member of the U.S. Climate Alliance, along with New York and Washington state, months ago.
“Either we end this problem, or this problem will end us,” said New York Gov. Andrew Cuomo.
On Wednesday, North Carolina became the 15th member of the U.S. Climate Alliance. Other members include Massachusetts, Oregon and Puerto Rico.
“Clean air and a healthy environment are vital for a strong economy and a healthier future,” North Carolina Gov. Roy Cooper, a newly elected Democrat, said in a statement.
Bay Area cities sue major oil companies over climate change

San Francisco and Oakland are suing to get five oil companies, including San Ramon-based Chevron, to pay for the cost of protecting the Bay Area from rising sea levels and other effects of global warming.
“These fossil fuel companies profited handsomely for decades while knowing they were putting the fate of our cities at risk,” San Francisco City Atty. Dennis Herrera said in a statement.
The lawsuits, which were filed Tuesday in state court in San Francisco and Alameda counties and announced Wednesday, don’t ask for a specific dollar amount. But the cities could try to put oil companies on the hook for billions.
Long-term improvements in San Francisco’s seawall are projected to cost $5 billion, according to one of the lawsuits.
“The law is clear that the defendants are responsible for the consequences of their reckless and disastrous actions,” Oakland City Atty. Barbara J. Parker said in a statement.
A spokesman for Chevron, Melissa Ritchie, said the lawsuits would not help address climate change.
“Reducing greenhouse gas emissions is a global issue that requires global engagement and action,” she said in a statement. “Should this litigation proceed, it will only serve special interests at the expense of broader policy, regulatory, and economic priorities.”
California sues to stop Trump’s border wall: ‘No one gets to ignore the laws. Not even the president’

California Attorney General Xavier Becerra announces lawsuit against Trump Administration.
California Atty. Gen. Xavier Becerra filed a lawsuit Wednesday alleging that President Trump’s proposal to expedite construction of a wall at the U.S.-Mexico border violates laws aimed at protecting the environment.
Becerra announced the legal challenge standing in front of the existing border fencing at Border Field State Park near San Diego, saying the federal government failed to comply with federal environmental laws and relied on federal statutes that don’t authorize border wall projects in San Diego and Imperial counties.
“No one gets to ignore the laws. Not even the president of the United States,” Becerra said. “The border between the U.S. and Mexico spans some 2,000 miles. The list of laws violated by the president’s administration in order to build his campaign wall is almost as long.”
He said the project involves the improper waiver of 37 federal statutes, many aimed at protecting the environment.
Filed in federal court in San Diego and including the California Coastal Commission as a plaintiff, the lawsuit states its purpose is “to protect the State of California’s residents, natural resources, economic interests, procedural rights, and sovereignty from violations of the United States Constitution” and federal law.

The lawsuit also alleges that federal officials have not shown any data suggesting new border barriers in the San Diego area will reduce illegal entry into the U.S., nor that there is a significant problem in that area.
It adds that the wall would have a chilling effect on tourism to the United States from Mexico.
In August, the U.S. Department of Homeland Security issued a notice that it was waiving federal and state laws on the environment to expedite the construction of prototypes of the wall along the San Diego border with Mexico.
The California lawsuit claims the federal government violated the U.S. Constitution’s separation-of-powers doctrine “by vesting in the Executive Branch the power to waive state and local laws.”
The lawsuit also says the Department of Homeland Security decided to build the walls without complying with the Clean Water Act, the National Environmental Policy Act and the Coastal Zone Management Act.
As a result, the lawsuit alleges, the federal government lacks proper environmental analysis of the impact of the 400-foot prototypes of the wall currently planned, as well as the 2,000-mile-long final wall.
A federal official declined comment.
“As a matter of policy, we do not comment on pending litigation,” said Tyler Q. Houlton, a spokesman for the Department of Homeland Security.
State Assemblywoman Lorena Gonzalez Fletcher (D-San Diego) stood with Becerra at the event, saying the wall is unnecessary and will put a barrier between relations involving the two countries.
“Maybe to people in Iowa, it sounds like a really good idea,” she said. “We don’t need more structure. We need a good relationship [with Mexico].”
Times staff writers McGreevy reported from Sacramento and Ulloa from San Diego.
California to sue Trump administration over plan for U.S.-Mexico border wall
California Atty. Gen. Xavier Becerra plans to announce a lawsuit Wednesday on behalf of the state that will challenge President Trump’s proposal to build a wall at the U.S.-Mexico border, a project Becerra has called “medieval.”
Becerra is scheduled to travel to Border Field State Park near San Diego to announce that a lawsuit is being filed in federal court over construction of border wall projects in San Diego and Imperial counties.
The lawsuit, which includes the California Coastal Commission as a plaintiff, states its purpose is “to protect the State of California’s residents, natural resources, economic interests, procedural rights, and sovereignty from violations of the United States Constitution” and federal law. It adds that the wall would have a chilling effect on tourism to the United States from Mexico.
The state’s lawsuit alleges that the Trump administration has failed to comply with federal and state environmental laws and relied on federal statutes that don’t authorize the proposed projects. The brief alleges the federal government violated the U.S. Constitution’s separation-of-powers doctrine “by vesting in the Executive Branch the power to waive state and local laws, including state criminal law.”.
The lawsuit also says the Department of Homeland Security decided to build the walls without complying with the Clean Water Act and the National Environmental Policy Act.
As a result, the lawsuit alleges, the federal government lacks proper environmental analysis of the impact of 400-foot prototypes of the wall currently planned, as well as the 2,000-mile-long final wall.
The Democratic attorney general has been critical of the wall for months, including in April during an appearance on ABC’s “This Week.”
“I’m still trying to figure out who believes that a medieval situation to fix our broken immigration system is what we need,” Becerra said.
He also accused Trump at the time of reneging on his promise to have Mexico pay for the wall.
“I think American taxpayers probably are very much aligned with Mexico. None of them, whether it’s Mexico or our taxpayers, wants to pay for a medieval wall,” he said.
This is the latest of more than two dozen lawsuits and legal briefs filed against the Trump administration by Becerra, who was appointed attorney general in January and is running for election to the post next year. He previously sued to challenge Trump’s plans to end a program that protects young immigrants from deportation, ban immigration from some countries and roll back environmental laws.
Last week, three advocacy groups sued the federal government to block construction of a border wall, alleging that the Trump administration overstepped its authority by waiving environmental reviews and other laws.
The action by the Sierra Club, Defenders of Wildlife and Animal Legal Defense Fund seeks to prevent construction of wall prototypes in San Diego. U.S. Customs and Border Protection officials said last month that prototypes for a border wall may be completed by the end of October.
Becerra’s lawsuit is the latest attempt by California Democrats to fight the wall proposal. A bill that would have banned state government contracts for any company that helps build the wall passed the state Senate, but stalled recently in an Assembly committee.
Sen. Ricardo Lara (D-Bell Gardens) authored the bill, testifying at a committee hearing that “the wall is another attempt to separate and divide us. It sends a message that we are better off in a homogenous society.”
Todd Bloomstine, a lobbyist representing the Southern California Contractors Assn., opposed the bill, asking the panel, “What next unpopular project would be [on the] blacklist?”
UPDATE
8:30 a.m. This article was updated to provide additional details of the lawsuit.
This article was originally published at 6 a.m.
Judge rules state used misleading language in summary of ballot measure to repeal California gas tax

A judge tentatively ruled Tuesday that the state-written title and summary of an initiative to repeal the recent gas-tax increases were misleading and should be rewritten by the state attorney general’s office.
The ruling by Sacramento Superior Court Judge Timothy M. Frawley, scheduled to be finalized at a court hearing on Friday, was welcomed by the initiative’s lead proponent, Assemblyman Travis Allen (R-Huntington Beach).
“This preliminary ruling is a major victory for Californians,” Allen, a candidate for governor, said in a statement. “This brings us one step closer to repealing Jerry Brown’s hugely unpopular gas tax. I look forward to the final ruling on Friday, and ensuring that the Repeal the Gas Tax Initiative receives the straightforward ballot title and summary that it deserves.”
Judge Frawley agreed with Allen’s legal claims that the title and summary drafted by Atty. Gen. Xavier Becerra’s office is “confusing, misleading, and likely to create prejudice against the proposed measure.”
The judge said the initiative would repeal taxes and fees approved by the Legislature this year, but the title and summary issued by the state makes it sound like it would eliminate transportation funding without using the words “taxes and “fees” in the title.
He ordered state officials to come to Friday’s hearing prepared to discuss alternate language for the ballot measure.
“To avoid misleading the voters and creating prejudice against the measure, the Attorney General must prepare a ‘true and impartial statement’ that reasonably informs voters of the character and real purpose of the proposed initiative in clear and understandable language,” the ruling says. “The existing circulating title and summary fails this test.”
If the judge finalizes the order after hearing arguments Friday, Allen can use the new title and summary to circulate a petition. Allen needs to collect 365,000 signatures from registered voters in 150 days to put the measure on the November 2018 ballot.
Gov. Jerry Brown: Trump’s rhetoric about North Korea adds to “non-rational bluster”

California Gov. Jerry Brown said President Trump’s name calling and threats at the United Nations can get in the way of diplomacy and statesmanship.
Earlier Tuesday, Trump called North Korean leader Kim Jong Un a “Rocket Man on a suicide mission” and said the United States may have no choice but to “totally destroy North Korea.”
“It just raises the temperature and the exchange of non-rational bluster back and forth,” Brown said in a interview with CNN’s Jake Tapper. “I don’t think that’s positive.”
Brown is in New York for some climate meetings related to the United Nations General Assembly.
Villaraigosa to address PAC that typically supports GOP candidates

Antonio Villaraigosa, one of the top Democrats running for governor, will address a group Wednesday that typically supports Republican candidates.
Tickets to see the gubernatorial candidate speak at a breakfast meeting hosted by the Fresno Chamber of Commerce’s Political Action Committee cost $40, money that supports the group’s mission of electing pro-business candidates.
“We need the right people making decisions for the community. The PAC endorses the most business-friendly candidate and raises money to get them elected. Donations to the PAC are used for candidate contributions, independent expenditures, or for the promotion of the endorsed candidates,” according to the group’s website.
The PAC has made $31,350 in political donations since 2006, according to the financial disclosure documents filed with the secretary of state’s office. Of that, all but $1,500 was donated to Republican candidates. Among the recipients were Chuck Poochigian, who received $1,000 in his unsuccessful run for attorney general in 2006 against now-Gov. Jerry Brown; then-Fresno Mayor Ashley Swearengin, who received $3,000 for her unsuccessful 2014 state controller bid, and state Sen. Andy Vidak, who received $6,100 over multiple election cycles.
Nathan Ahle, president and chief executive of the PAC, said that all of the major gubernatorial candidates will be invited to address the group.
Villaraigosa, the former mayor of Los Angeles, has spent a notable amount of time campaigning in the Central Valley, once a GOP stronghold that is now more politically mixed and a region where Democrats are not as rigidly liberal on economic and environmental issues as coastal and Bay Area voters. The economic recovery has also not taken hold as strongly in the Central Valley as it has in other parts of the state, an inequity frequently raised by Villaraigosa on the campaign trail.
“The mayor is taking his campaign for economic opportunity and economic equality to every corner of California,” campaign spokeperson Michelle Jenny said.
Updated at 7:45 p.m.: This post was updated with a response from the Villaraigosa campaign.
Yes, ‘dahlink’: Frederic Prinz von Anhalt, widower of Zsa Zsa Gabor, is running for California governor

Frederic Prinz von Anhalt, widower of the whimsical celebrity and actress Zsa Zsa Gabor, is back.
Von Anhalt has filed to run for governor of California — his second attempt after a short-lived campaign in 2010 — saying he’s fed up with seeing roads falling apart, people struggling to afford rent and an explosion of homelessness in the state.
“I’ve lived in this city for 36 years. I’ve never seen so many people eating out of a trash can in the Western world,” Von Anhalt said Tuesday. “We talk about Hollywood, and this being the entertainment center of the world. How is this possible?”
Von Anhalt, Garbor’s ninth and last husband, is running as an independent. He filed an official “Candidate Intention Statement” with the California Secretary of State’s office Monday, the first step in launching an official campaign.
The 74-year-old Bel-Air resident, a German immigrant, said he has enough money to help support his own campaign. He said he dropped out of the 2010 governor’s race only because his wife became seriously ill. She died in December.
“She was the one … who wanted me run,” Von Anhalt said.
Von Anhalt also flirted briefly with a run for Los Angeles mayor in 2013, a race eventually won by Eric Garcetti.
FOR THE RECORD
5:33 p.m.: An earlier of this post said Von Anhalt was age 71. He is 74.
Assemblyman urges other legislatures to join California in censuring President Trump

A California lawmaker who authored a resolution to support a censure of President Trump sent letters to 49 other state legislatures Tuesday to urge them to join the effort.
Assemblyman Tony Thurmond, a Richmond Democrat, sent the letters days after the Assembly became the first state legislative body to support a congressional censure of the president.
“California has spoken and we look to the rest of the nation to join us,” Thurmond said in a statement. “It’s important that all our states unite and show that the United States of America stands against hate.”
California’s attorney general asks Senate for more tools to fight online sex trafficking

California Atty. Gen. Xavier Becerra pleaded with a U.S. Senate committee on Tuesday to change a decades-old Internet freedom law in order to give states more power to go after online sex traffickers.
“We’re losing the fight against sex trafficking, which means we’re losing our children,” Becerra said.
Some in Silicon Valley have pushed back on the idea for years, saying that it would be a disaster for a free and open Internet to change the 1996 Communications Decency Act so websites can be held liable by states and victims if criminal material is posted on their sites.
The Stop Enabling Sex Traffickers Act would allow states and victims to sue websites that “knowingly” assist or benefit from sex trafficking. The federal government currently can pursue criminal charges against sites, but Becerra argued that the Department of Justice doesn’t have the resources to pursue every incident.
California’s U.S. senators have been walking a fine line with the California-centered tech industry over the issue, and neither is among the 28 co-sponsors of the bill. Spokespersons for Sens. Dianne Feinstein and Kamala Harris indicated the senators want more tweaks to the bill’s language, but haven’t said what changes they’d need in order to support the bill.
Harris’ lack of support was noted during Tuesday’s hearing, with several senators saying they were working with her to address her concerns. Harris championed changing the Communications Decency Act when she was California’s attorney general, and brought a suit against Backpage.com executives on charges of pimping, money laundering and conspiracy.
Becerra left Congress to replace Harris as attorney general and has continued the state’s suit against the classified advertising giant.
Late last month, a Sacramento Superior Court judge threw out the pimping charges, citing the exemption written into the Communications Decency Act.
“The Internet has become an easy way to make money in this criminal enterprise, and we need the tools to go after these folks,” Becerra said. “We’re fighting with two hands tied behind our back.”
After the hearing, he indicated that he understands his former congressional colleagues have had to balance Silicon Valley interests with the fight against sex traffickers, and said, “Everyone has got to get there in their own way.”
5:05 p.m.: This post was updated to clarify that Harris is working with the committee on a change to the bill’s language.
It was originally posted at 2:40 p.m.
Feinstein criticizes Trump for using U.N. speech ‘as a stage to threaten war’

Sen. Dianne Feinstein (D-Calif.) criticized President Trump for using his speech to the United Nations General Assembly on Tuesday “as a stage to threaten war.”
It’s the second time this week Feinstein has been harshly critical of Trump. On Monday, she said he needed to “grow up” and stop obsessing over former rival Hillary Clinton.
Feinstein got flak from some progressive Californians last month when she called for “patience” in dealing with the president, saying that Trump could be a good president if he learned and changed.
After cap-and-trade vote, Assemblyman Chad Mayes faces a second Republican challenger for reelection

Former Palm Springs Police Chief Gary Jeandron on Tuesday became the second Republican to announce plans to challenge Assemblyman Chad Mayes (R-Yucca Valley) in the 2018 election.
Jeandron, a La Quinta resident, said he was angered over Mayes’ vote as Assembly Republican leader to support an extension of the state’s controversial cap-and-trade program, which requires businesses to buy permits to release greenhouse gas emissions. Jeandron saw the action as continuing a “wrongful tax increase” and said he is signing a no-tax pledge.
“I just don’t believe [Mayes] has held Republican values,” Jeandron told The Times. “He has been blinded by ambition. He has been seduced by the governor.”
Mayes’ vote led to an outcry by Republican leaders, and he eventually succumbed to pressure to step down as leader of the Assembly Republicans.
Mayes defended his position, telling colleagues during the floor debate, “many of us believe that climate change is real and … we have to work to address it.”
Jeandron, who lost to Mayes in the 2014 election, joins San Jacinto City Councilman Andrew Kotyuk in planning to challenge Mayes for the 42nd Assembly District seat.
Republican John Cox tasted political defeat many times before launching his bid for California governor

Candidate for California governor John Cox is relatively new to the state’s politics, but Cox has run for office multiple times, and even tangled with Barack Obama on the debate stage when the pair ran in the 2004 Illinois U.S. Senate race.
Neither candidate was considered their party’s favorite. But things began looking up for Obama, of course, who won the Senate race and then the presidency. Cox dropped out before the GOP primary election. It was his third try for elected office in Illinois and his third defeat.
Now he’s back, this time in his new home of California, running for governor against a trio of Democratic heavyweights. Once again, Cox is a practical unknown. Once again, the Republican is in a left-leaning state reaching for a coveted political office. Once again, Cox’s campaign is being fed by cash from his own bank account.
After she was confronted by protesters, Pelosi says Democrats want a ‘clean’ Dream Act — with no border wall
House Minority Leader Nancy Pelosi on Monday said she understood the fear in young protesters who shouted her down at a San Francisco news conference, asking for a legal path to citizenship for themselves and their parents.
Speaking at Sacramento State hours after the disruption, Pelosi said she agreed with the protesters, pointing to the Dream Act as only the first step to broader immigration reform.
“We are all disrupters ourselves,” she said, standing next to fellow congressional Democrats. “So we recognize it and respect it in others.”
Both press events were scheduled by Pelosi to discuss a legislative fix to help thousands of young people affected by President Trump’s decision to rescind the Deferred Action for Childhood Arrivals program. The Obama-era policy provided temporary status for 800,000 people brought to the country illegally as children.
Pelosi and Senate Minority Leader Chuck Schumer of New York met with Trump last week after the termination of DACA was announced.
In Sacramento, Pelosi said they had come to an agreement to a “clean” Dream Act, which would provide a path to permanent status for citizens who work, study or serve in the military, without tougher border enforcement or increased deportations.
Meanwhile, Democrats are fighting with the president over the construction of a wall along the U.S-Mexico border. And House Speaker Paul Ryan of Wisconsin “has made it clear he wants some kind of border security,” Pelosi said.
“That is not under discussion,” she said. “We can discuss other issues, but we are not going to discuss how we protect the Dreamers.”
Feinstein, who called for patience with Trump, lashes out over his attacks on Clinton
Sen. Dianne Feinstein (D-Calif.) said it was “appalling and disgusting” to see President Trump retweet a video edited to look like he hit former rival Hillary Clinton in the head with a golf ball.
“He continues to obsessively lash out at her — at his rallies, with his words and now through social media — in a manner that is utterly unbecoming of the president of the United States,” Feinstein said in a statement Monday. “Every one of us should be offended by the vindictive and candidly dangerous messages the president sends that demean not only Secretary Clinton, but all women. Grow up and do your job.”
Clinton is out with a new book about the campaign, and Trump has repeatedly used Twitter to deride her as a sore loser. He retweeted the animated GIF Sunday which shows him hitting a golf ball that then knocks down Clinton.
Feinstein, who has yet to say whether she’ll run again in 2018, has walked a fine line with Trump in recent months. She’s criticized him at times, but drew ire from some progressive Californians last month when she called for “patience” in dealing with the president, saying that Trump could be a good president if he learned and changed.
Democrats want to replace DACA with the Dream Act, a bill this L.A. member of Congress has been pushing for 16 years

Sixteen years ago, Downey Rep. Lucille Roybal-Allard helped file legislation that would have allowed people brought to the country illegally as children to stay in the United States.
That bill became the Dream Act. Its failure to pass Congress led to the Deferred Action for Childhood Arrivals program, which President Trump this month decided to end as he urged Congress to find a replacement.
If Democrats have their way, DACA’s replacement will look a lot like what Roybal-Allard proposed in 2001. Democratic leaders emerged from a meeting with Trump last week saying Roybal-Allard’s bill, which includes a path to citizenship for some immigrants in the country illegally, must be part of Congress’ plan to protect DACA recipients.
Bigger tax breaks for homeowners and renters could be on California’s 2018 ballot

California homeowners and renters could receive more tax breaks under a proposed initiative for the November 2018 state ballot.
The measure would increase a state tax credit for homeowners and renters to $500 a year, which would continue to go up as housing costs rise. The Howard Jarvis Taxpayers Assn., the anti-tax group behind Proposition 13’s property tax restrictions, is sponsoring the initiative.
Currently, homeowners receive a $70 annual credit and renters $60. Neither figure has increased in more than 25 years, according to the association.
Jon Coupal, the association’s president, contrasted its approach to rising housing costs with the recent package of bills passed by the Legislature to spend more on low-income housing construction and ease local home building regulations.
“While the government seeks to address the housing crisis with more regulations, more government costs and more debt, we believe this is the most efficient way to provide immediate tax relief for every Californian who has to pay for a roof over their head,” he said.
Coupal said his organization plans to conduct polls to test the initiative’s viability before deciding if it will finance a signature-gathering campaign. The association also is considering an effort to repeal the gas tax hike that lawmakers approved in the spring.
The proposal is one of many housing-related measures that could appear on the November 2018 ballot. The California Assn. of Realtors is considering an effort to expand Proposition 13’s property tax breaks. And Gov. Jerry Brown is expected to place on the ballot a $4-billion bond to finance low-income housing construction and provide home loans for veterans after lawmakers approved it last week.
San Diego members of Congress team up for Tijuana sewage spill fix
California lawmakers are building a wall against President Trump’s policies
California state legislators ended their annual session the way they began it — building a wall to protect undocumented immigrants from President Trump.
Not an iron wall, as Trump promised to erect along the U.S.-Mexico border, but a legal barrier to prevent local police and sheriffs from teaming with the president’s agents to enforce federal immigration law.
The legislators did a lot of other things, too, before adjourning early Saturday until January.
They sent Gov. Jerry Brown bills to address California’s dearth of affordable housing, to borrow $4 billion for parks and waterworks, to spend $1.5 billion in greenhouse-gas pollution fees, to provide tuition-free community college for first-year students and to lift some secrecy from prescription drug pricing.
Earlier in the session, the heavily Democratic Legislature passed its boldest, most controversial bill of the year: A $5.2-billion annual increase in fuel taxes and vehicle fees to finance transportation infrastructure, especially to repair crumbling highways. Republicans will attempt to repeal the bill at the ballot box in 2018. Brown says that “borders on insanity.”
Trump is ‘riding a very dead horse’ on climate change, Gov. Brown says at New York conference

Gov. Jerry Brown on Monday touted steps California has taken toward a healthier climate, but warned that powerful forces he called “climate deniers” are resisting technologies and policies designed to improve conditions.
“I like all the optimism around here, but I don’t want to minimize the steep hill that we have to climb,” Brown said at the start of a gathering of international leaders called Climate Week NYC. “Decarbonizing the economy when the economy depends so totally on carbon is not child’s play. It’s quite daunting.”
Hosted by the Climate Group, an international nonprofit organization that works with business and government to promote clean technologies and policies, the event was scheduled to bring together high-profile governors, executives of Fortune 500 companies and leaders of multinational businesses for a week to share their strategies in tackling climate change.
The discussions come amid concerns about global warming and after Hurricanes Harvey and Irma caused devastation in Houston, Florida and across parts of the Caribbean. Some scientists believe that warmer ocean waters caused by climate change are creating stronger storms.
Nancy Pelosi shouted down at DACA news conference for working with Trump
More than four dozen immigration activists upset with Democrats for negotiating with President Trump shouted down House Minority Leader Nancy Pelosi at a San Francisco news conference Monday.
“We are not your bargaining chip,” the crowd chanted at one point, according to KCBS News political reporter Doug Sovern.
San Francisco Chronicle reporter Evan Sernoffsky said on Twitter that some in the group were yelling, “All of us or none of us.” Other reporters said the group chanted, “Shut down ICE.”
Pelosi held the news conference to advocate for speedy passage of a legislative fix to the legal status of hundreds of thousands of people brought to the country illegally as children.
Pelosi and Senate Minority Leader Charles E. Schumer of New York met with Trump last week after he announced an end to the Deferred Action for Childhood Arrivals program. The Obama-era program deferred deportation for some people brought to the country illegally as children.
Pelosi and Schumer said their discussion with the president included the possibility of adding more immigration enforcement — which some immigration advocates are against — to legislation to address DACA.
At the news conference, Pelosi first made remarks and introduced an immigrant in the country illegally, at which point the shouting began, according to a Pelosi aide. The group surrounded Pelosi, with some gesturing close to her face. She attempted to calm the crowd for about half an hour before leaving the news conference. The aide said the group was made up of local DACA beneficiaries.
“We need to have a conversation, but that was completely one-sided; they don’t want any answers,” Pelosi told reporters afterward, according to a transcript.
Pelosi said the activists should be focused on Republican members of Congress, not Democrats.
“I understand their frustration, I’m excited by it as a matter of fact, but the fact is they’re completely wrong. The Democrats are the ones who stopped their assault on ‘sanctuary cities,’ stopped the wall, the increased deportations in our last bill that was at the end of April, and we are determined to get Republicans votes to pass the clean Dream Act. Is it possible to pass a bill without some border security? Well we’ll have to see. We didn’t agree to anything in that regard, except to listen,” Pelosi said.
UPDATES
1:06 p.m. This post was updated with more details throughout and quotes from Pelosi.
This post was originally published at 12:12 p.m.
Doctor running against Rep. Ed Royce wins endorsement of group trying to elect scientists
Gov. Jerry Brown, at New York climate event, says Trump’s actions are ‘stupid’ and ‘dangerous’
Democrats’ hopes of flipping seats in California are soaring, but it won’t be as easy at it seems

Democrats know they have to win at least a few seats in California if they want to regain control of the House in 2018. But though the energy and hopes of many Democratic activists here are soaring, flipping Republican-held seats here could be harder than it appears.
There are a few bits of conventional wisdom that suggest Democrats have a long road ahead. For one, Republicans often turn out in greater numbers than their Democratic counterparts in midterm-election years.
And even though Hillary Clinton won seven of the Republican-held districts Democrats are now targeting, past election data show voters there still lean much more conservative than other parts of the state.
If past is prologue, says Rob Pyers, research director for the nonpartisan election guide California Target Book, Democrats will have a hard time picking up more than a couple of seats in California.
With most voters unlikely to tune in until at least next spring, there are many factors that could affect the political calculus, including whether the California Republican Party will be able to field a competitive candidate for governor, or whether ballot initiatives such as a potential repeal of the newest gas tax hike will propel GOP voters to the polls.
California will be the ‘keeper of the nation’s future’ in the era of Trump, state Democratic lawmakers promise

Within a day of President Trump’s election last November, California’s top Democratic lawmakers responded with a joint statement that contained an audacious promise. It was their state, not Washington, D.C., that would be the “keeper of the nation’s future.”
An artistic rendering of that vow, with looping calligraphy and a roaring grizzly, is now on display in the offices of Senate leader Kevin de León and Assembly Speaker Anthony Rendon. In the wake of Trump’s win, the words seemed to be a sort of foundational document — California’s declaration of resistance.
That pugilistic posture is often conveyed in shorthand: California versus Trump. But the ensuing legislative year, which ended Friday, revealed the messy reality of squaring up against the federal government.
“It’s been challenging,” De León (D-Los Angeles) said, bleary-eyed as he took a break during the final days of the session. “You have to debate, you have to negotiate, you have to make your case, and I think at the end of the day, we’ll still have the most far-reaching policy in the nation.”
California Politics Podcast: Lawmakers leave Sacramento after a busy year
From immigration issues to housing, some of the biggest debates of the Legislature’s nine-month session happened at the very end.
In governing, as in life, deadlines often make things happen.
On this week’s California Politics Podcast, we take an early look at some of the most important decisions lawmakers made in the final few days of the 2017 session in Sacramento. That includes a landmark decision to intervene in the issue of illegal immigration, and to pass a long discussed package of bills to begin addressing California’s housing crisis.
We also look at some of the broader political themes of the entire legislative year -- most notably, the effort by Democrats in the Legislature to provide a “resistance” to actions taken by President Trump.
I’m joined by Times staff writers Melanie Mason and Liam Dillon.
Gov. Jerry Brown signs bills that spend climate change cash, expand rules for marijuana shop owners

A detailed plan for spending more than $621 million collected through California’s climate change program was signed into law by Gov. Jerry Brown on Saturday, along with new rules on the sale of medical and recreational marijuana.
Brown signed seven bills, all related to the state budget, just hours after the Legislature sent them to his desk in its final day of the 2017 session.
The climate money, raised through California’s sale of greenhouse gas pollution credits, represents the bulk of a $1.5 billion spending agreement between the governor and Democratic legislative leaders earlier in the week.
Brown also signed a bill on Saturday to allow a single store to be used by both medical and recreational marijuana distributors. The stores would also be able to run a manufacturing operation at the same site, and businesses could group together multiple licenses for pot cultivation in one facility.
Passage of ‘sanctuary state’ bill draws rebukes from Trump administration officials, praise in California

California lawmakers on Saturday passed a “sanctuary state” bill to protect immigrants without legal residency in the U.S., part of a broader push by Democrats to counter expanded deportation orders under the Trump administration.
The landmark legislation by Sen. Kevin de León (D-Los Angeles) would limit state and local law enforcement communication with federal immigration authorities, and prevent officers from questioning and holding people on immigration violations. But the bill sent to Gov. Jerry Brown drastically scaled back the version first introduced, the result of tough negotiations between Brown and De León in the final weeks of the legislative session.
Its passage already is reverberating across the country. Trump administration officials have sounded off in opposition. And immigrant rights groups and some California law enforcement officials have come out in support of what they call a hard compromise.
Supporters unable to resurrect California clean-energy proposal on final day of legislative session

Despite a last-minute push from environmentalists and actors from “The Avengers,” legislation that eventually would require all of California’s electricity to come from clean sources failed to advance this year.
Facing opposition from unions and utilities, Assembly leadership refused to put the measure, SB 100, up for a vote on Friday, the final day of the legislative session.
“The decision to not move the bill this year is disappointing,” said Kathryn Phillips, director of the Sierra Club’s California chapter. “But we are committed to moving this policy next year. There’s no time to waste.”
The measure, written by Senate President Pro Tem Kevin de León (D-Los Angeles), was one of two major pieces of energy legislation to stall this year. The other, a proposal from Gov. Jerry Brown to integrate California’s electricity grid with other states in the region, also failed to generate the support necessary this week.
Closely watched California Internet privacy bill dies in final minutes of legislative session

California lawmakers on Saturday shelved a bill that would have required Internet service providers such as Verizon, Comcast and AT&T to get permission from customers before using, selling or allowing access to their browser history.
The legislation by Assemblyman Ed Chau (D-Monterey Park) would have enshrined in state law some federal Internet privacy regulations that were rolled back this year by President Trump and Congress. The regulations limited what broadband providers can do with their customers’ data.
The defeat capped a behind-the-scenes battle that pitted telecom companies against state Internet service providers (ISPs) and brought other bills to a halt in the state Senate as negotiations unfolded over legislation that would have had national significance.
Most of the “California Privacy Act” would have codified the repealed restrictions crafted by the Federal Communications Commission under the Obama administration.
But it also would have barred Internet service companies from refusing to provide service or limiting service if customers do not waive their privacy rights. And it would have prohibited them from offering customers discounts in exchange for waiving their privacy rights or charging customers a penalty for refusing to do so.
The bill had the support of former FCC Chairman Tom Wheeler and smaller California ISPs. Opponents — which included tech giants like Google — argued it was being rushed through the legislative process.
For ISPs that are already complying with the former federal regulations, the bill would haven’t made much of a difference operationally, said Ernesto Falcon, legislative counsel for the Electronic Frontier Foundation, a digital rights group based in San Francisco. But the influence of the legislation could have been sweeping.
“California is a critical state because you are covering a large part of the nation just because of its population,” he said. “It sets the stage for other states to follow suit.”
For now, efforts to implement the rules could move to the ballot box. A ballot initiative proposed this month would give California consumers the right to know what personal information businesses are collecting, what they do with it and to whom they are selling it.
It’s a wrap for the California Legislature for 2017. Here’s what lawmakers accomplished

California lawmakers wrapped up their work for the year early Saturday morning, with sweeping new legislation to address issues from illegal immigration to the state’s housing crunch — with hundreds of bills being debated and decided in the final 48 hours.
Leaders of the state Senate and Assembly praised the work of the Legislature in remarks after the final gavels fell in both houses.
”I think this has been an historic year for all of our accomplishments,” said Senate President Pro Tem Kevin de León (D-Los Angeles) just after 2 a.m. Saturday. “We put our values into action.”
This was the first year of the Legislature’s two-year session. Lawmakers now return to their home districts and aren’t scheduled to return to Sacramento until January.
Two of the year’s most talked-about efforts both happened in the closing 48 hours of the legislative session.
Lawmakers gave final approval to a bill curtailing communication between local law enforcement officers and federal immigrations officials, often dubbed the “sanctuary state” measure, SB 54. And they approved a package of bills aimed at addressing California’s growing affordable housing crisis, including funds generated by a new real estate transaction fee and a $4-billion bond that voters must approve next year.
The year also saw the Legislature approve a number of other notable new laws:
- A sweeping law signed by Gov. Jerry Brown in July that extends the state’s landmark cap-and-trade climate change program until 2030.
- A $52-billion transportation plan agreed to in April, funded by a new annual vehicle fee and an increase in the state’s fuel taxes.
- A $183.2-billion state budget that boosts both several government programs and adds money to the state’s cash reserves.
Several closely watched proposals passed in the Legislature’s final hours of work are now headed to Brown’s desk, though it’s unclear whether he will sign them into law.
They include a number of efforts to push back against the policies of President Trump’s administration — from guidelines on campus sexual assault enshrined in federal law by former President Obama to bills designed to allow California to step in and embrace environmental and land-use policies that Democrats fear could be discarded by Republicans in Washington.
“We’re wrapping up what may be the most progressive legislative session in memory,” Assembly Speaker Anthony Rendon (D-Paramount) said in his closing floor remarks early Saturday morning.
Lawmakers ultimately rejected a number of other closely watched proposals, from a hotly debated effort to push back school start times for high schoolers to new rules regarding the release of police body camera video to the public.
The final day of the legislative calendar for 2017 crept beyond the traditional midnight deadline and included a small bit of controversy in the Senate. There, Republicans claimed that Democrats had failed to follow the proper procedure to continue beyond midnight — a charge that stalled the proceedings for more than half an hour. Democrats later said the rules allowed debate on the final bills to continue.
Brown now has until Oct. 15 to sign or veto bills sent to his desk. While he rarely endorses bills during their debate in the Legislature, the governor has historically signed most of the bills sent to him by lawmakers.
Parks and water improvements likely to be on California’s 2018 ballot

Californians likely will see a $4-billion bond to fund improvements to parks and water infrastructure on the 2018 statewide ballot.
State lawmakers passed the bond early Saturday morning, and Gov. Jerry Brown has pledged to sign it.
“This is the single-largest investment in the history of the United States to park-starved communities,” said Sen. President Pro Tem Kevin de León (D-Los Angeles), the author of the measure, SB 5.
Anti-Trump environmental protection proposal fails to advance in California Legislature

A proposal to help California guard against rollbacks of federal regulations stalled early Saturday morning at the end of the state’s legislative session.
SB 49 would have enshrined large swaths of federal environmental protection regulations and other rules into state law. The goal was to prevent changes made by the Trump administration from affecting California.
“It’s trying to freeze time,” said Sen. Henry Stern (D-Los Angeles), an author of the legislation.
Assemblyman Ian Calderon (D-Whittier), who helped push the legislation in the Assembly, said it struggled to get the necessary votes among members concerned about giving regulators outsized power. He said lawmakers could continue working on the issue next year.
“It’s not dead,” he said. “It’s just paused.”
Two related measures, Senate bills 50 and 51, were approved by lawmakers and sent to Gov. Jerry Brown. One would try to prevent the federal government from selling federal land without first offering it to the state, and the other would direct California officials to preserve climate change data at risk of being deleted by the federal government.
Legislature declares California will be a ‘sanctuary state’

California lawmakers on Saturday passed a Senate bill that would turn the state into a sanctuary for immigrants without legal residency in the country, part of a broader push by Democrats to counter expanded deportation orders under the Trump administration.
After passionate debate on both House chamber floors, staunch opposition from Republican sheriffs and threats from Trump administration officials against so-called sanctuary cities, SB 54 by Sen. Kevin de León (D-Los Angeles) was approved with a final 27-11 vote. But the bill sent to Gov. Jerry Brown was drastically scaled back from the version first introduced, changes that were negotiated between Brown and De León in the final weeks of the legislative session.
On the Senate floor minutes before 2 a.m. Saturday, De León said the changes did not erode the mission of the bill, which was to protect hardworking families, and reflected a compromise between law enforcement officials and advocates.
“This is a measure that reflects the values of who we are as a great state,” he said.
SB 54 would limit state and local law enforcement agencies from communication with federal immigration authorities, and prevent all state and local police forces from questioning and holding people on immigration violations.
But amendments added this week would permit officers to continue sharing information and transferring people for immigration authorities if they have convictions for one or more of roughly 800 crimes.
In their respective chambers Friday, at least 20 members of the Assembly and six members of the Senate took the floor for debate on the bill.
Opponents pointed to the concerns from sheriff’s organizations, saying it tied officers’ hands, allowing serial thieves, chronic drug abusers and gang members to slip through the cracks. Supporters countered that the Trump administration was trying to paint all immigrants illegally in the country as criminals.
They pointed to provisions in the bill that would make hospitals, schools and courthouses safe zones for immigrants from federal immigration authorities at a time of fear for some communities. Some children without legal status were not going to school, they said, while police statistics showed a drop in reports of sexual assault and domestic violence as immigrant victims refused to come forward.
California taxpayers will provide $270 million if L.A.’s 2028 Olympics goes over budget under bill passed by Legislature

California legislators pledged up to $270 million in state tax dollars on Saturday to cover costs should Los Angeles’ 2028 Olympic bid go over budget.
The 2028 Summer Games are expected to have a $5.3-billion price tag, and organizers think corporate sponsorships, ticket sales and other revenue sources could cover expenses. Los Angeles was awarded the 2028 Games this week, and city officials have asked the state for financial assistance.
Gov. Jerry Brown has not specifically weighed in on the measure, AB 132, but has promised broad support for the Olympics. He also signed a measure last year that would have provided a similar financial guarantee when Los Angeles was bidding on the 2024 Games.
Bill benefiting Facebook’s new headquarters, Hollywood development heads to governor’s desk
California’s 2020 presidential primary should be in early March, lawmakers decide

California lawmakers gave final approval on Saturday to moving the state’s primary elections to early March beginning in 2020, a renewed effort at relevance in the quadrennial presidential sweepstakes.
SB 568 would shift all primary elections — including those for statewide, legislative and congressional offices — to the first Tuesday in March, as long as it comes after the first Monday.
“Moving California’s presidential primary to March from June means candidates in both parties can’t treat immigration, climate change, criminal justice reform and investing in jobs and innovation like afterthoughts, as they did too often in 2016,” state Sen. Ricardo Lara (D-Bell Gardens), the bill’s author, said in a written statement.
California has tried to move its presidential primary in prior years as a way to entice Democratic and Republican candidates to come to the state and campaign. But in almost every election cycle, other states moved their primary or caucus even earlier, thus leaving California as a political also-ran.
Whether Gov. Jerry Brown will sign the bill into law is unclear. In 2011, he agreed to a plan by lawmakers to permanently hold all primary elections in June. This bill would undo that, prompted by Democrats who lamented the state again missing real presidential relevance in 2016. Hillary Clinton clinched the Democratic nomination just before California voters went to the polls.
Republican opponents said the early primary would, in turn, force candidates to file their candidacy papers for state offices as early as the December before the election year. They argued that would dissuade some newcomers from challenging incumbents who already might have amassed a large campaign war chest.
“Some of you may love that, but I don’t think it’s right for the voters,” said Assemblyman Matt Harper (R-Huntington Beach).
Brown has until Oct. 15 to act on the bill, along with dozens of others sent to him before the Legislature was to adjourn for the year early on Saturday morning.
As legislative session drags on past deadline, Capitol denizens have some fun with Hamilton tweets
As debate in the California Legislature dragged on past midnight, and with it, debate on whether lawmakers could even technically still debate past midnight, some Capitol insiders had some fun with lyrics from the musical “Hamilton.”
Continuing a phenomenon that appeared to have started the night before, Capitol reporters, lobbyists and general policy wonks used lyrics from America’s hottest democracy musical to comment on and poke fun at the legislative sausage-making.
It all started Thursday, when CalMatters reporter Laurel Rosenhall seemed to take the first shot.
And she wasn’t going to throw it away.
Rosenhall promised there’d be more Friday. And there was.
Gov. Brown supports bill sent to him that would end lifetime listing of many sex offenders on public registry

After an emotional debate, state lawmakers on Saturday gave final legislative approval to a controversial bill that would end the lifetime listing of many convicted sex offenders on a public registry in California.
The bill, which was shelved then revived, was sent to the governor on the last day of the legislative session with Assemblywoman Lorena Gonzalez Fletcher (D-San Diego) calling it one of the most difficult votes she has cast.
“It’s not an easy thing to do, but sometimes we have to make hard votes,” Gonzalez Fletcher told her colleagues, adding that being a mom made it difficult to change a system aimed at tracking rapists and child molesters.
The measure by Sen. Scott Wiener (D-San Francisco) would allow, starting in 2021, for the names of those who committed lower-level, nonviolent sex crimes or who are judged to be low risks to re-offend to be removed from the registry after 10 or 20 years, depending on the crime. The offender must petition the local district attorney for a review.
Wiener called his bill “a long overdue reform of California’s broken sex offender registry.”
Gov. Jerry Brown is expected to sign the bill.
“SB 384 proposes thoughtful and balanced reforms that allow prosecutors and law enforcement to focus their resources on tracking sex offenders who pose a real risk to public safety, rather than burying officers in paperwork that has little public benefit,” said Ali Bay, a spokeswoman for the governor.
Los Angeles County Dist. Atty. Jackie Lacey sought the change because the current registry has grown to a difficult-to-manage 105,000 people, which reduces its value to law enforcement trying to solve sex crimes by checking those on the list.
Because the registry is public, it also punishes people who have not committed new crimes for decades, including some who engaged in consensual sex, bill supporters argued.
“The only other states that still use this Draconian, outdated, ineffective law are Alabama, South Carolina and Florida,” Assemblyman Evan Low (D-Campbell) said during the floor debate.
The Assembly vote Friday was 42-22, with most Republicans, including Melissa Melendez of Lake Elsinore, voting against the bill.
Melendez objected to some of the crimes that would put offenders on a second tier, eligible for removal from the list after 20 years, which include rape by deception and lewd and lascivious behavior with a child under 14.
“We put so many children at risk if we do this,” Melendez told her colleagues.
The proposal also went to the Senate after midnight on Saturday for approval of amendments. It took a circuitous route to the governor’s desk. After a legislative analysis estimated it would cost $75 million over six years to revamp the database, an Assembly panel shelved a previous version of the bill for the year.
Wiener revived the proposal by taking a bill that would have studied allowing bars to stay open later, gutting that language and inserting the provision on the sex offender registry.
It’s now Saturday, and California’s Legislature is still going
With several big-ticket items pending, the final day of the Legislature has now stretched into day two.
The legislative session was scheduled to end at the end of the day on Friday, but there’s still more work left.
So lawmakers are voting to keep debating past midnight.
California lawmakers approve last of bills to enhance protections for young people arrested and doing time
As work drags into the night at California’s Capitol, a lawmaker’s favorite bill can be held ‘hostage’
Dads, get ready to change a lot more diapers
After ending his holdout on housing vote, an Assembly Democrat gets one of his bills to move

High drama flowed through the Assembly floor Thursday night when key affordable housing legislation stood two votes short before passing.
After Assembly Speaker Anthony Rendon (D-Paramount) left the roll call vote open for an hour, two of the hold-outs — Democratic Assemblymen Marc Levine of San Rafael and Adrin Nazarian of North Hollywood — returned to the floor and voted yes. Their support secured passage of Senate Bill 2, legislation that could raise $250 million annually for low-income development and one of the highest-profile measures of the year.
The next day, a Senate fiscal committee shook loose an unrelated energy bill authored by Nazarian, even though the measure had been held weeks ago — an extremely rare occurrence on the Legislature’s final day of the year.
So did Nazarian secure a promise on his bill in exchange for his vote?
No, Nazarian said.
“This is a pressure-cooker time right now,” Nazarian said in an interview with The Times on Friday afternoon. “This is what happens.”
Nazarian said he had some concerns about the housing bill, which would charge a $75 fee on most real estate transactions, and was tired of adding more fees onto taxpayers.
But he was also frustrated at the Senate for holding his bill and was striking back.
“I had decided that I would, from time to time, abstain on several bills at a time indiscriminately just so there would be a certain level of discomfort — or at least a message to the leadership that we can’t be arbitrary,” he said.
Nazarian said he had expressed his concerns earlier in the week to Rendon and did so again while the two jockeyed over SB 2 on Thursday, a session fueled by coffee and beer.
For his part, Rendon also denied there had been any promises given to Levine and Nazarian for voting yes on the housing bill, simply saying the pair had been convinced.
“There were no side deals in this at all,” Rendon said after Thursday’s vote. “This was about the housing crisis that Californians have experienced for over a generation.”
Nazarian agreed, telling The Times that SB 2 was the best part of a package of housing legislation passed by lawmakers in the waning hours before they adjourn for the year at the end of Friday.
And while Nazarian’s energy bill had advanced out of a Senate committee, it was still not a sure thing to pass. As of 8:30 p.m. Friday, his measure had yet to receive a vote on the Senate floor.
California Assembly votes to support censure of Trump over comments on Charlottesville violence

The California Assembly on Friday night voted to support a congressional censure of President Trump for his response to violence that broke out in Charlottesville, Va., during a protest over a Confederate statue.
The Assembly passed a resolution 41 to 5 to denounce comments by the president that seemed to equate white supremacists and neo-Nazis with the protesters demonstrating against them.
Trump said “many sides” were to blame for violence at an Aug. 12 rally where a man plowed his car into a group of counter-protesters, killing one of them.
Trump later denounced the Ku Klux Klan and neo-Nazis, but repeated that “both sides” were to blame.
“This isn’t about what you think about President Trump,” said Assemblyman Tony Thurmond (D-Richmond), who authored the resolution. “This is about his statements, his inability to condemn hate, and his failure to act.”
U.S. House Minority Leader Nancy Pelosi, a San Francisco Democrat, introduced a resolution for a congressional censure shortly after Trump’s comments. A congressional censure does not remove a president from office, and they are rare.
Assemblyman Matthew Harper (R-Huntington Beach) was the lone Republican to speak out against the resolution to support the censure. He said it wasn’t necessary for Assembly members to spend time reiterating that they don’t like Trump.
“Let’s utilize our time on issues that are germane to the state of California,” Harper said during the debate.
Assemblywoman Shirley Weber (D-San Diego) said the conversation was necessary because racial hatred in the country persists.
“This is California,” she said, “and we refuse to let this come in and infect our state.”
Gov. Brown: Housing legislation will help Californians buy homes and afford rent
California taxi cabs will face fewer regulations under bill headed to the governor

Taxi cab drivers will need fewer permits to operate in California under a bill headed to Gov. Jerry Brown.
The measure, Assembly Bill 1069, allows taxi drivers to reduce the number of permits they’ll need to work to a maximum of two per county — one where they live and one where they predominantly work. The bill’s author, Assemblyman Evan Low (D-Campbell), has argued the legislation will help drivers save tens of thousands in fees annually and allow them to better compete with Uber and Lyft.
Last year, Brown vetoed legislation from Low that would have moved taxi cab regulation to the state, instead of the local governments that handle it now. AB 1069 still allows cities and counties to regulate the industry.
California lawmaker on a bill that finances home loans for veterans: ‘For me it was really honoring my father’
For me it was really honoring my father, who was a veteran. For our family of 12, we lost our home in a fire. He got a loan to help. I think there’s a lot of us that have had personal experiences with homelessness. This is why we had to [do this].
— Sen. Jim Beall (D-San Jose), on SB 3, his bond measure that would finance low-income housing developments and veterans’ home loans
Billions in new funding for low-income housing passes the California Legislature

State legislators gave final approval to a package of major legislation aimed at addressing the state’s housing affordability problems.
On Friday afternoon the state Senate passed Senate Bills 2, 3 and 35 — legislation Gov. Jerry Brown has said he will sign.
SB 2, a $75 fee on mortgage refinances and other real estate transactions except for home and commercial property sales, is expected to raise $250 million a year to help finance low-income developments.
SB 3 will put a $4-billion bond on the November 2018 ballot, with $3 billion to subsidize the construction of low-income housing and the remaining $1 billion for home loans for veterans.
SB 35 will ease local regulations for home building in an effort to spur construction, adding to overall supply.
The Assembly passed all three bills Thursday night after a tense vote on SB 2, which needed a two-thirds supermajority to pass. In the Senate on Friday, all 27 Democrats voted yes on SB 2, providing the exact amount of votes needed.
Republicans opposed to the measure argued that the state should not be spending more to subsidize housing.
“I think it’s still an ill-founded concept that government provides all the answers and is the best arbiter of providing low-income housing,” said Sen. Jim Nielsen (R-Gerber).
‘Sanctuary state’ legislation clears the California Assembly after emotional debate
Follow our team on a big day (and every day)
California will spend big on clean vehicles under plan approved by lawmakers

State lawmakers on Friday approved a $1.5-billion plan for spending cap-and-trade revenue, with most of the money going toward financial incentives to get dirty cars, trucks, buses and other vehicles off the road.
The plan, which was included in Assembly Bills 109 and 134, was negotiated by Gov. Jerry Brown and legislative leaders. Lawmakers extended the cap-and-trade program, which requires companies to buy permits to emit greenhouse gases, earlier this year.
The centerpiece of the plan is $895 million for clean vehicles, which will be divided among programs aimed at electric cars, school buses, farm equipment and other priorities.
Lawmakers hope the money will help make a dent in California’s emissions from transportation, which the state has struggled to reduce.
The legislation also included some union-friendly provisions. The cap-and-trade money could not be used to replace port vehicles with automated equipment. In addition, state regulators could eventually be asked to evaluate whether an automaker treats its workers in a “fair and responsible” manner before its vehicles are eligible for rebates.
Fierce debate in the Assembly on bill to create ‘sanctuary state’ immigration rules
Later school start times for California students laid to rest for the year

A bill that would require California middle and high schools to begin their day no earlier than 8:30 a.m. is being shelved for the year, its author said Friday, a day after it fell well short of the votes needed for passage.
The legislation was introduced by Sen. Anthony Portantino (D-La Cañada-Flintridge), who said he will revisit the issue in January.
Portantino said he is “disappointed in the opposition that promoted non-science and unsubstantiated arguments against SB 328, forcing us to move this fight for our children’s health to January. I’m committed to this issue and I will continue to work to see it become law.”
Supporters had cited research from sources including the Journal of Clinical Sleep Medicine showing that later starting times for schools reduce the negative impacts of sleep deprivation. Adolescents’ brains are “hard-wired” to not sleep before 11 p.m., the supporters said.
“School districts around the country that have moved teenage school start times later have seen measurable, positive results for student achievement and student public health,” Portantino said after introducing SB 328.
The measure received 26 of the 41 votes it needed for passage in the Assembly late Thursday, with opponents saying the state should not impose a blanket restriction on local school districts better positioned to determine the best hours based on their individual circumstances.
Republican Assemblyman Matthew Harper, who served on the school board in his hometown of Huntington Beach, said during the floor debate that some coastal schools have to accommodate surfing teams, while Central Valley schools might have to schedule around agricultural needs.
“Each individual school board should make that determination incorporating the local needs of their local communities,” Harper said. “This one-size-fits-all approach really is kind of ridiculous.”
California lawmakers sign off on new disclosure of campaign donors in ballot measure advertisements
New rules to more clearly reveal big donors to California ballot measure campaigns would be required under legislation sent Friday to Gov. Jerry Brown.
The proposal, Assembly Bill 249, was hailed by supporters as a sweeping effort to combat the growing reliance on campaign committees with innocuous sounding names -- the only information often available to voters in campaign advertising.
“The status quo allows donors to hide behind layers of misleading committee names,” said the bill’s author, Assemblyman Kevin Mullin (D-South San Francisco), during floor debate on Friday.
Similar proposals stalled in recent legislative sessions. This year’s version, if it becomes law, would likely make most of its impact on ballot measure campaigns by requiring advertisements to detail the three largest contributors.
Republican lawmakers said the bill’s definition of a donor would create too little disclosure when it comes to the money collected by public employee unions.
“While the intentions of this bill are good, it creates a massive loophole and therefore an unfair playing field,” said Assemblyman Matt Harper (R-Huntington Beach).
Whether Brown will sign the bill remains unclear. Last week, the state’s campaign watchdog agency raised concerns about whether the law will be too difficult to effectively enforce.
Gov. Jerry Brown heads to New York and Connecticut for climate change events next week

Gov. Jerry Brown is hitting the road next week to talk about climate change on the East Coast, his office announced Friday.
He’s scheduled to speak at multiple events in New York on Monday, including one at the United Nations.
On Tuesday he heads to Yale University for a panel conversation moderated by former Secretary of State John F. Kerry, then he returns to New York on Wednesday for an event with former New York City Mayor Michael Bloomberg.
Brown will participate in more events on Thursday and Friday, including a news conference with the premiers of Quebec and Ontario, Canadian provinces that have partnered with California’s cap-and-trade program, which requires businesses to purchase permits to pollute.
The governor has been ramping up his travels this year. He was in China this summer, and he recently returned from Russia and Alaska. Later this year he’s attending a United Nations conference on climate change in Germany.
Bill that would help reduce California’s backlog of untested rape kits heads to governor’s desk

A bill that would tackle the backlog of untested sexual assault evidence kits in the state is on its way to Gov. Jerry Brown.
AB 41, written by Assemblyman David Chiu (D-San Francisco), would help determine how many untested kits there are in the state.
The bill passed the Assembly on a vote of 79 to 0 on Thursday.
“Survivors of sexual assault deserve to know what happened to the sexual assault evidence kits they submitted,” Chiu said in a statement. “To get at the heart of the backlog problem we need to know how many kits are collected each year, and if they’re not analyzed, we need to know why.”
The bill would require law enforcement to report annual data on sexual assault kit collection and testing to the state Department of Justice.
Under the legislation, local agencies will have access to a database to log rape kits and provide updates for them.
More comprehensive data could help law enforcement make improvements and decide whether more resources are needed to test the kits.
Chiu’s bill comes in response to a national conversation about mismanaged rape kit evidence, which can be used to investigate and prosecute sexual assault crimes.
Major housing bills advance in Assembly

California lawmakers advanced key housing legislation late Thursday, clearing the most substantial hurdle for a package of bills aimed at addressing the state’s housing affordability crisis.
Legislators in the Assembly passed SB 2, a $75 fee on mortgage refinances and other real estate transactions except for home and commercial property sales. The measure is expected to raise $250 million a year to help finance new and rehabilitated developments for low-income residents — a key step, lawmakers said, in beginning to get housing costs under control.
“We are living during the worst housing crisis our state has ever experienced,” said Assemblyman David Chiu (D-San Francisco).
The bill required two-thirds support from Assembly members, a threshold that the bill’s author, Sen. Toni Atkins (D-San Diego), and legislative leaders had been struggling to meet.
California’s first dog Colusa Brown gets political during late-night Assembly vote
Democratic lawmakers still wrangling votes for key California housing legislation hours from deadline
‘Avengers’ actors dial the Capitol to support California clean-energy proposal
Some of the Avengers are assembling to push for clean-energy legislation in California.
Mark Ruffalo, a.k.a. the Hulk, Chris Evans, a.k.a. Captain America, and Don Cheadle, a.k.a. War Machine, have been tweeting and calling lawmakers’ offices to rally support for Senate Bill 100.
The legislation, which appears unlikely to advance before the session ends Friday evening, would phase out fossil fuels for generating electricity by 2045.
Sarah Shanley Hope, executive director for the Solutions Project, a nonprofit that funds grass-roots organizations in California and around the country, said the actors took a break from filming the next “Avengers” movie in Atlanta to gather around a phone and dial up Assembly offices.
“They were calling the public numbers just like anyone else,” said Shanley Hope, who helped arrange the calls.
The message to lawmakers? “You can be the real superheroes this week.”
Chris Hemsworth, a.k.a. Thor, wasn’t on the phone calls. But he posted his support for the legislation on Twitter.
California lawmakers pass resolution to oppose anti-Semitism, other forms of discrimination

California lawmakers passed a resolution Thursday to take a stand against anti-Semitism and other types of discrimination.
“History is going to judge us,” said Sen. Joel Anderson (R-Alpine), who supported the resolution. “Let’s not be on the wrong side.”
The resolution came in response to a rise in anti-Semitic incidents across the country, lawmakers said. Verbal discrimination, cemetery desecrations and targeted assaults are among the actions it opposes.
Resolutions that touch on current events with national interest are generally less common in the California Legislature.
Several senators who supported the resolution shared their experiences with anti-Semitism.
Sen. Jeff Stone (R-Temecula) said his great-grandmother escaped Poland during World War II while the rest of her family died in the Auschwitz concentration camp.
Sen. Hannah-Beth Jackson (D-Santa Barbara), who is Jewish, recalled being called discriminatory names as a child.
It has been frustrating to see anti-Semitism persist, she said.
“There was a period of time I thought we were bridging that gap in our country,” Jackson said on the Senate floor.
Bill to keep Obama-era rules aimed at cracking down on campus sexual assault clears Legislature

A week after U.S. Education Secretary Betsy DeVos announced a review of Obama-era guidelines on campus sexual assault, the California Legislature voted to enshrine the former president’s rules into state law.
A measure by state Sen. Hannah-Beth Jackson (D-Santa Barbara) is off to Gov. Jerry Brown’s desk after being approved by the state Senate on Thursday. The bill, SB 169, would codify in state law existing Title IX regulations, which require schools to treat students equally, regardless of sex.
The federal law is best known for mandating that boys and girls get equal opportunities to participate in sports, but it has also guided schools on how to clamp down on sexual assault and harassment.
In 2011, the Obama administration established guidelines meant to spur more aggressive action against campus rape and harassment. DeVos has argued that policy does not properly protect the rights of the accused.
Although DeVos announced a formal review last week, she had signaled early in her tenure that she was planning to revisit the Obama-era policy. Jackson introduced her bill in January.
Jackson said last week the secretary’s decision “puts women and girls at grave risk.”
“Contrary to Secretary DeVos’ claims, the Obama administration guidelines created, for the first time, a fair, equitable and clear process for students and schools to effectively respond to rape and sexual assault while protecting both the accused as well as the victim,” she said in a statement. “In California, we will continue to fight to ensure that women and girls can be safe in their educational pursuits.”
Male, female or nonbinary? California clears way for driver’s licenses to have gender-neutral option

A measure allowing Californians to select a third, nonbinary gender option on their driver’s licenses and birth certificates is headed to Gov. Jerry Brown.
The bill, Senate Bill 179 by Sen. Toni Atkins (D-San Diego), cleared the state Senate on Thursday without debate. Atkins and other backers of the measure have characterized it as an expansion of rights for transgender, intersex and other people who do not identify as male or female.
“Many of us have an ID that matches our gender presentation, and so showing it is hassle-free,” Atkins said in a statement. “But for Californians who have an ID that does not match their gender presentation, showing it at airports, in shops or to law enforcement can be extremely stressful and lead to harassment or a delay in completing a transaction. It doesn’t need to be this way.”
California lawmakers approve new rules for rolling out 5G cellular systems, but local governments remain opposed

Lawmakers gave final approval Thursday to new rules for how “small cell” high-speed cellular equipment will be installed in communities across California, even as local government officials warned the move will strip them of making choices tailored to their communities.
The state Senate vote on SB 649 marked the end of a tumultuous few months of lobbying by the telecommunications industry and city and county officials, with relative little common ground found even as the bill was amended a half-dozen times.
If signed into law by Gov. Jerry Brown, the bill would downsize the role played by city and county officials in setting limits on where the equipment for new 5G cellular service would be placed. Local governments would have less power to block the installation of the devices, which supporters claim would help ensure more communities are connected faster. They also argued that SB 649 would provide a boost to the state’s economy.
“This is a bill that will create lots of jobs,” said state Sen. Ben Hueso (D-San Diego), the proposal’s author. “It will increase connectivity in our state.”
But local government officials insisted throughout the legislative process that people should have input on where new, potentially unsightly equipment would be placed in their communities. During final debate in the state Senate, lawmakers asked a series of questions about where the line would be drawn between local decision-making and a new statewide policy.
In reversal, state Senate approves ballot measure that would expand the L.A. County Board of Supervisors

After falling short of votes earlier in the week, a bill that would expand the Los Angeles County Board of Supervisors won the two-thirds majority vote needed for passage in the state Senate on Thursday. The proposal, which would increase the board’s members from five to seven, would be put on the June 2018 ballot for voter approval should it pass the Assembly.
Acknowledging the measure faces a tough sell, Sen. Tony Mendoza (D-Artesia) said he will take it up in that chamber in January so he has time to muster the needed votes.
“Today was a huge step in the right direction for the people of L.A. County and all Californians,” Mendoza said. “The LA. County Board of Supervisors has remained the same since 1850, when the population was just 3,000. It is time we give L.A. County’s 10 million residents a fair and representational government.”
Mendoza won sufficient votes after he said he will drop a controversial proposal to make the county administrative officer an elected position.
Los Angeles County’s delegation in the Senate split over the proposal, but four Republicans and two Democrats from other parts of the state changed their position and voted to support the measure, giving it the bare 27-vote margin it needed to pass.
With the county Board of Supervisors opposed, Democratic senators from Los Angeles County who voted against the measure included Ricardo Lara, Henry Stern and Holly Mitchell.
Mitchell said it would not be proper to allow all of the counties in California to determine how Los Angeles is governed.
“The people of Los Angeles County, while we appreciate your concern, have voted three times against a proposal just like this one,” Mitchell said during the floor debate. “If you are concerned about the people of Los Angeles County, allow the people of Los Angeles County to determine their own future and fate.”
Mendoza said his proposal is different from the failed county initiatives because his includes strict cost-containment measures. He criticized county board members who are opposing his bill.
“They are not looking at the greater good. They are looking at self-preservation,” Mendoza said.
Sen. Jeff Stone (R-Temecula) is a former Riverside County supervisor who agreed with the concern that each Los Angeles board member is representing too many people at more than 1 million.
“People deserve to be able to have an elected official they can depend on,” Stone said.
However, Sen. John Moorlach (R-Costa Mesa), a former Orange County supervisor, said it is awkward having the state tell Los Angeles County how to govern.
“I see this as antagonistic,” he said, offering that a better solution might be to divide Los Angeles County into two or three counties.
Proposal would close Aliso Canyon — but not for a decade

The troubled Aliso Canyon natural gas storage facility would be closed down in a decade under new legislation, but that’s not fast enough for some activists.
The facility sprung a leak in October 2015, releasing more than 100,000 tons of methane into the air and forcing thousands of people to evacuate their nearby homes. It was later reopened, but recent problems required Southern California Gas Co. to shut down a third of the storage wells.
The proposal to require Aliso Canyon to shut down no later than 2028 was inserted into budget legislation, Assembly Bill 127, in the final days of the legislative session. It echoes a timeline laid out by the California Energy Commission, part of Gov. Jerry Brown’s administration, in July.
Activists criticized the possibility of waiting a decade before Aliso Canyon would be closed.
“It’s unacceptable for this facility to remain open and we are pleading that Gov. Brown place our health over SoCalGas’ profits and shut down this dangerous facility now,” said a statement from Matt Pakucko, president of Save Porter Ranch, a community near Aliso Canyon.
Efforts to keep the facility closed, most notably a proposal from Sen. Henry Stern (D-Los Angeles) to require an investigation to determine the original cause of the 2015 leak, failed to advance this year.
Stern said 10 years is too long to allow Aliso Canyon to keep operating before shutting down the facility.
“I think it’s feasible to do it now,” he said, noting that Southern California made it through a scorching hot summer without needing natural gas stored there to avoid blackouts.
Another piece of legislation, Senate Bill 112, is identical to AB 127 but doesn’t include the Aliso Canyon provision. It remains to be seen which one will advance before lawmakers adjourn for the year on Friday evening.
“We’re going to continue to call on the Brown administration to close down Aliso Canyon,” said Adam Scow, California director for Food and Water Watch.
Pot edibles that look like gummy bears should be illegal to sell in California, lawmakers say

California companies would be prohibited from selling marijuana edibles made in the shape of a person, animal, insect or fruit under a measure given final legislative approval Thursday and sent to the governor for consideration.
“We are trying to protect children,” said Assemblyman Rudy Salas (D-Bakersfield), who authored AB 350.
Lawmakers said marijuana edibles have been made in the past to look like gummy bears or miniature pineapples. In April, some middle school students in San Diego got sick after a classmate sold them marijuana-laced gummy bears.
The state plans to begin issuing licenses for the sale of recreational marijuana to people 21 and older in January, so lawmakers have introduced several bills aimed at preventing pot from being marketed to minors.
Citing conspiracy theory, Rep. Dana Rohrabacher blames Democrats for Charlottesville violence: ‘It was a setup’

Rep. Dana Rohrabacher says Democrats, not white supremacists, are to blame for the deadly violence in Charlottesville, Va., last month.
“It’s all baloney,” Rohrabacher told the San Francisco Chronicle in an article about his 2018 reelection chances.
Rohrabacher, a Republican from Costa Mesa, told the Chronicle he believes a supporter of former presidential candidates Hillary Clinton and Bernie Sanders prompted the violence by arranging for Civil War reenactors to protect a Robert E. Lee statue at the center of the dispute between white supremacist protesters and counter-protesters.
“It was a setup for these dumb Civil War reenactors,” Rohrabacher said. “It was left-wingers who were manipulating them in order to have this confrontation” and to “put our president on the spot.”
The conspiracy theory that a Democrat organized the white supremacist rally that led to the death of one person was stoked by right-wing provocateur Alex Jones of InfoWars and has been debunked by nonpartisan fact-checking site Politifact.
Rohrabacher is among the Republicans in a battleground district in 2018. Andrew Godinich, a spokesman for the Democratic Congressional Campaign Committee, criticized Rohrabacher’s comment.
“These views are repugnant. They are un-American. It is 2017, not 1861 – and any member of Congress that hesitates to condemn white supremacists has no business serving in the House of Representatives,” he said in a statement.
Assemblyman Chris Holden refuses to advance clean energy legislation despite push from environmentalists

Environmentalists are stepping up the pressure on Assemblyman Chris Holden (D-Pasadena), urging him to advance Senate Bill 100 on clean energy.
The legislation, which would put the state on a path to phasing out fossil fuels for generating electricity by 2045, has been held in Holden’s committee.
Senate leader Kevin de León (D-Los Angeles), who authored the legislation, said he still wants to see the measure passed before lawmakers adjourn for the year on Friday evening.
But Holden has indicated that he’s not going to budge. In a new statement on Thursday, Holden said he supports the goal of the legislation, but said some issues still need to be worked out.
“Unfortunately, it is too late in the legislative process to work on any amendments to address concerns of the opposition,” he said, citing a new constitutional amendment that requires all legislation to be publicly available for three days before a vote. “Therefore we look forward to resolving those issues and moving this important legislation forward next year.”
Group aims to repeal California gas tax hike on November 2018 ballot

A group of California Republicans on Thursday filed papers to launch an initiative drive aimed at repealing a gas tax and vehicle fee increases and require future tax hikes be approved by voters.
The tax and fee increases signed by Gov. Jerry Brown will raise $5.2 billion annually for road and bridge repairs and expanded mass transit. The hikes — raising the gas tax from 18 cents to 30 cents per gallon — start Nov. 1.
Brown blasted the initiative proposal.
“I can’t believe the proponents of this ballot measure really want Californians to keep driving on lousy roads and dangerous bridges,” the governor said in a statement. “Taking billions of dollars a year from road maintenance and repair borders on insanity.”
Reform California, headed by former San Diego City Councilman Carl DeMaio, filed papers with the state attorney general’s office Thursday to start the process to collect 587,407 signatures to qualify the measure for the November 2018 ballot.
“Sacramento politicians really crossed the line with these massive car and gas tax hikes and we intend to give taxpayers the chance to reverse that decision with this initiative,” DeMaio said in a statement.
The initiative paperwork was filed by an attorney for the California Republican Party, which is expected to play a big role in the effort.
Delegates to the party must vote on a position, but state party chairman Jim Brulte said, “The California Republican Party historically supports the right of voters to vote on taxes. This gas tax is one that will punish suburban and rural Californians as well as many people who live in cities.”
The initiative was opposed by state Sen. Jim Beall (D-San Jose), who carried the gas tax bill.
“The Legislature and governor took action to solve a $130-billion-plus backlog in deferred road maintenance that threatens California’s economy,” Beall said. “Delaying that action will cause the backlog to grow and put our roads at risk of being ruined beyond repair, costing taxpayers more to replace and rebuild the existing system.”
Lucy Dunn, president and CEO of the Orange County Business Council, warned that the initiative could “have the effect of halting billions of dollars worth of local road repair and improvement projects mid-stream. It will kick people off the job site and completely leave road construction in disarray.”
This is the second initiative proposed to repeal the gas tax. Assemblyman Travis Allen, a Republican candidate for governor, filed paperwork to get a ballot measure going, but that’s tied up in a court dispute.
DeMaio’s group was buoyed by its success this year in collecting more than 100,000 signatures in an effort to force a recall election of state Sen. Josh Newman (D-Fullerton) for his vote in favor of the gas tax. That matter has not yet been resolved.
UPDATE
3:40 p.m. This article was updated to include comments from Brulte, Beall and Dunn.
This article was originally published at 2:31 p.m.
Rep. Dana Rohrabacher still waiting to tell Trump what he learned at his meeting with WikiLeaks founder Julian Assange

Rep. Dana Rohrabacher said Thursday he hasn’t yet arranged a meeting with President Trump to discuss what he learned from WikiLeaks founder Julian Assange about the theft of Democratic emails during the 2016 election.
“The meeting has not been put on the calendar yet, but I have spoken to senior people at the White House about arranging a meeting,” Rohrabacher, a Costa Mesa Republican, said between House votes Thursday. “I have to believe it will happen, yes. It’s an important issue.”
In August, Rohrabacher traveled to London to meet with Assange, who remains in asylum in the Ecuadorian embassy there. He said they discussed a potential presidential pardon in exchange for information on the theft of emails from the Democratic National Committee, which were published by WikiLeaks before the 2016 presidential election. Rohrabacher said in a statement that Assange “emphatically stated that the Russians were not involved.”
Multiple U.S. intelligence agencies have agreed Russia was involved in the theft of Democratic Party emails and tried to influence the 2016 election to benefit Trump. Members of Congress and the Justice Department are investigating Russia’s meddling in the election, and Senate investigators are reportedly considering talking with Rohrabacher about the meeting with Assange.
Democrats are hoping to oust Rohrabacher in 2018.
California lawmakers back bill to protect workers’ reproductive health choices over opposition from religious groups

Employees would not risk losing their jobs for reproductive health choices, including having an abortion, in-vitro fertilization or a child out of wedlock, under a bill that passed the Legislature on Thursday.
The measure, by Assemblywoman Lorena Gonzalez Fletcher (D-San Diego), takes aim at employer codes of conduct, particularly at religious institutions, that could cost workers their jobs for making such health decisions.
“This is not a partisan bill,” Gonzalez Fletcher said on the Assembly floor. “It’s an issue of basic health, privacy and worker rights.”
The measure prompted a thorny debate on how to balance worker privacy with freedom for religious institutions to ensure their workers align with their values.
The California Catholic Conference, in a letter to lawmakers, said the bill marked “an unmistakable effort to target religious organization employers in this state.”
“The adoption of standards of conduct that are often shaped by the employer’s 1st Amendment rights of religious freedom and association, and that protect the employer’s ability to infuse those policies with the tenets of its particular faith, has always been permitted and respected,” the letter said.
That doggie in the window would have to be a rescue dog under a new bill passed by the Legislature
L.A. Congressman Jimmy Gomez endorses one of the three Democrats looking to unseat Darrell Issa
California could soon bar the expansion of immigrant detention centers

California lawmakers have approved legislation introduced by Democrats to counter the potential expansion of immigrant detention facilities under the Trump administration.
The bill by Sen. Ricardo Lara (D-Bell Gardens) would prohibit any city, county or law enforcement agency from entering into a contract with the federal government or a private company to detain immigrants — unless it already has done so by January 2018. It also would bar cities and counties that contract with private companies from expanding their facilities or number of beds.
The state Senate on Wednesday passed SB 29 with a 27-13 vote. It is now headed to the governor’s desk for final approval.
Lara introduced the bill as part of a legislative package to protect immigrants from President Trump’s call for expanded deportations. It dovetails with another measure — folded into the state budget in June — that would require the California Department of Justice to perform annual audits of detention centers.
The budget measure also temporarily prohibits cities and counties from adding beds to public jails and facilities that detain immigrants.
But a broader statewide push has been building in recent years to overhaul locally run detention centers and ensure that they provide people with proper access to food, medical care and lawyers.
Efforts followed a report from the Department of Homeland Security’s inspector general, which found that hundreds of immigrant detainees housed in Orange County’s largest detention facility were served spoiled food, given mold-covered shower facilities and offered phones that didn’t work.
California has three cities that contract with U.S. Immigration and Customs Enforcement and private companies to hold immigrants: Adelanto Detention Facility in Adelanto, which has 2,000 beds; Mesa Verde Detention Facility in McFarland, with 400 beds; and the Imperial Regional Detention Center in Holtville, with 704 beds.
Column: What does it mean for San Francisco liberals that Pelosi and Trump are working together?
What happens when the congressional representative of this uber-liberal enclave — who also happens to be leader of House Democrats — starts dancing with the devil?
Nancy Pelosi, along with her Senate counterpart, Charles E. Schumer of New York, convinced President Trump to override his advisors and ignore congressional Republicans by agreeing to a three-month extension of the nation’s debt limit, emergency aid for Hurricane Harvey victims and other federal spending.
The next day, at Pelosi’s behest, the president tweeted reassurance to “Dreamers” — immigrants brought to America illegally as children — that they needn’t worry about deportation during the six months Congress works to resolve their ambiguous state.
And Wednesday night, “Nancy and Chuck,” as the president chummily called the pair, joined the president for dinner at the White House, where Democrats said they reached agreement with Trump to permanently protect the Dreamers as part of a larger border security package.
Trump failed to win a measly 10% of the vote here in November but, even so, many said they were just fine with Pelosi’s new BFF.
Expanded work-site protections against ICE raids could be coming to California under bill sent to Gov. Brown

After negotiations to help quell opposition from dozens of business associations and agricultural groups, the state Assembly sent a bill to Gov. Jerry Brown on Wednesday that would expand workplace protections for employees without legal residency in the U.S.
The bill by Assemblyman David Chiu (D-San Francisco) would prohibit employers from allowing federal immigration agents on private business property without a judicial warrant. It also would require business owners to give their employees public notice — within 72 hours — of federal immigration inspections of employee records.
Businesses that fail to provide notice to employees face penalties of $2,000 to $5,000 for a first violation and $5,000 to $10,000 for each subsequent violation, unless some exceptions apply.
New amendments scaled back some of the requirements on employers. Under the bill’s provisions, employers would have more flexibility to notify employees about reviews. And they would no longer have to report to the state labor commissioner any self-audits of employee records or any work-site raids or audits by U.S. Immigration and Customs Enforcement.
Some opponents remain, including California Citrus Mutual, the California Cotton Ginners and Growers Assn. and and the Society for Human Resource Management. The California Chamber of Commerce, the California Farm Bureau Federation and the Western Growers Assn. were among those removing their opposition to the proposal.
Chiu has said he filed the bill in response to President Trump’s attack on immigrant communities, a message that has reverberated across California, a state with its own troubled past with work-site raids. In the 1980s, the federal government launched aggressive immigration raids in Mexican and Central American neighborhoods in Los Angeles.
“In an environment of division and fear, California must continue to defend its workers, to guard its values and to ensure that its laws protect all of our residents,” Chiu said.
New parents at California’s small businesses would get 12 weeks of leave under bill headed to Gov. Jerry Brown

Employees at many small businesses across California could not be denied up to 12 weeks away from work to care for a new child under legislation sent Wednesday to Gov. Jerry Brown.
The bill, which applies to workers with at least a year of continuous employment at a company of 20 to 49 employees, cleared its final hurdle in the state Senate. Employees would no longer be in danger of being fired when leaving to care for a newborn, similar to existing protections for workers at larger companies.
“For our lowest-income workers, this is a situation where they cannot afford to take that time working for smaller employers,” said state Sen. Hannah-Beth Jackson (D-Santa Barbara), the bill’s author.
Brown vetoed a similar measure last year, suggesting that any new parental leave law should allow for mediation before lawsuits filed by employees. As a result, the new bill requires a two-year pilot mediation program to be created by the state Department of Fair Employment and Housing.
Jackson said 40% of workers at small businesses in California are currently at risk of losing their job when they want to take time off to care for a new child. Opponents said the smallest of businesses can’t bear the costs of losing workers.
The bill was a top priority of the Legislative Women’s Caucus this year, with supporters saying it could provide help to 2.7 million workers whose employers aren’t covered by current law.
L.A. County crime-inspired measure would ban openly carrying rifles in unincorporated areas of California

Californians would be prohibited from openly carrying long guns in public, unincorporated areas of the state under a bill approved Wednesday by the Legislature and sent to the governor for consideration.
The measure, opposed by the National Rifle Assn., was requested by the Los Angeles County Sheriff’s Department to plug a loophole in state law that bans openly carrying handguns in areas outside cities.
“Shotguns and rifles should not be carried on our residential streets by untrained and unidentified members of the public,” said Sen. Anthony Portantino (D- La Cañada-Flintridge). “This can cause confusion and endanger public safety for citizens and law enforcement as well.”
In some cases, long guns have been brandished by people at political rallies.
The measure, which includes unloaded long guns, was introduced by Assemblyman Mike Gipson (D-Carson) with support from gun-control groups including the California chapters of the Brady Campaign, which wrote to lawmakers saying it is a natural follow-up after the state previously banned exposed handguns in incorporated or unincorporated areas in California and exposed long guns in cities.
The group cited high crime levels in areas of Los Angeles County involving long guns, including assault rifles. Each county’s Board of Supervisors would designate which unincorporated areas would be subject to the ban.
The NRA argued that the measure was proposed as a result of “irrational gun phobia” and said it violates constitutional rights.
“It is obvious that AB 7 is not about reducing California’s firearm crime rate, but is simply another attempt to further strip the law-abiding citizens of the Golden State of their Constitutional right to self-defense,” the group said in a statement.
Republican lawmakers, including Assemblyman Devon Mathis of Visalia, also opposed the bill. Mathis said it can affect hunters in the state’s rural and unincorporated areas.
He said the bill was introduced based on “the idea that carrying a shotgun is going to scare people. People just need to get over it and grow up.”
A bill that would set new rules for online dating contracts in California heads to Gov. Jerry Brown’s desk

Legislators on Wednesday gave final approval to a bill that would recognize online dating services under the state’s Dating Service Contract Act.
The bill, proposed by Assemblyman Kevin Mullin (D-South San Francisco), would set new specific contract requirements for Internet dating services.
The bill’s new requirements include allowing online-dating customers to cancel contracts by email and have access to electronic copies of contracts.
It passed in the Assembly 68-1 on Wednesday and now goes to Gov. Jerry Brown for his signature. It previously passed the Senate by a 35-0 vote.
California Assembly approves resolution denouncing Trump’s decision on DACA

After some intense exchanges on the house floor, the California Assembly on Wednesday passed a resolution that condemned President Trump for his decision to rescind protections for people who were brought into the country illegally as children.
House Resolution 66, coauthored by 57 members in the chamber, urges the president to stand with recipients of the Deferred Action for Childhood Arrivals, or DACA, program, and calls on Congress to find a “bipartisan and more effective” version of the initiative.
It was approved 57 to 1.
On the Assembly floor, lawmakers pointed to research that showed one-fourth of people with DACA status in the U.S. reside in California — about 222,000 people who they said have contributed to tech, agriculture, business and the arts. Supporters shared personal stories about relatives who came into the country illegally.
Assemblywoman Blanca Rubio (D-Baldwin Park), who was brought to the country illegally when she was 6, said she was proud to serve as a legislator and contribute to the state’s economy.
When you talk about DACA recipients, “it is not just some kid. It is somebody like me.”
The only dissenting member was Assemblyman Matthew Harper (R-Huntington Beach), who argued DACA was the result of abusive federal overreach by President Obama.
The Obama administration policy that created the program was, he said, “a cruel trick that we live with the consequences of today.”
Assemblyman Devon Mathis (R-Visalia), the only other member to speak against, didn’t vote. But he ignited passionate rebuttal from members when he said they needed to stop filing “dumb—” resolutions, politicizing “every damn thing.”
“Our president didn’t say he wanted to get rid of DACA,” Mathis said. “He didn’t say he wanted to round up all the ‘Dreamers.’”
One of those rebuttals came from Assemblyman Miguel Santiago (D-Los Angeles), who said this era would go down as one of the darkest periods in the country’s history.
Trump doesn’t support DACA students or Dreamers, he said.
“You can’t rewrite history in five minutes on the Assembly floor,” he said. “You can’t turn around and say that he supports people who look like me because he clearly hasn’t.”
First year of California community colleges could be free under bill headed to Gov. Jerry Brown’s desk
Hoping to entice more students into California’s community college system, lawmakers on Wednesday passed a bill to make students’ first year free.
The Assembly gave final approval to a measure by Assemblyman Miguel Santiago (D-Los Angeles) that waives fees for first-time full-time students.
“We know that if a student goes full time, a student’s success rate is much higher than if they go part time,” Santiago said on the Assembly floor.
Arguing that a free first year of community college would help serve as a bridge for high school students who wouldn’t otherwise continue school, Santiago described his bill, AB 19, as a “huge step to make a college-going community and culture in California.”
Legislators introduced a slew of measures to tackle the cost of college. The most sweeping measures, such as an Assembly Democrat’s plan to make attending state universities “debt-free,” fizzled.
AB 19 still faces a significant hurdle from Brown. His finance department opposes the measure, expressing concern that the aid would be available to all students regardless of need, instead of targeting financially strapped Californians.
Bill to shed more light on prescription drug prices heads to Gov. Jerry Brown’s desk

Powered by increasing scrutiny of costly prescription drugs, a measure that would require sweeping new disclosure on how medicines are priced cleared its final legislative hurdle Wednesday.
The state Senate approved the bill with no debate, belying the fierce behind-the-scenes jockeying that pit pharmaceutical companies against health insurers, labor unions and liberal activists.
The measure, SB 17 by state Sen. Ed Hernandez (D-Azusa), would require health plans to report to the state the 25 drugs that are most frequently prescribed, those that are most costly and those that have had the highest year-to-year increase in spending. It also would require drug makers to provide advance notice of planned price increases if the hikes exceed certain thresholds.
Proponents touted the measure’s disclosure requirements, which they called the most comprehensive in the country, shedding light on how drug costs contribute to overall healthcare spending.
“California will soon be able to bring some much needed information regarding drug pricing by pharmaceutical companies,” Hernandez said in a statement. “Although this state legislation was passed in California, it’s a monumental achievement for the entire nation. If signed into law, SB 17 will set national health care policy, having impact for consumers and providers in other states.”
But the bill was strenuously opposed by drug manufacturers, who argued that by focusing the disclosure on list prices — the sticker price that is often sharply discounted for insurance companies and consumers — the information would paint an inaccurate picture.
Two other transparency measures, including a nearly identical bill by Hernandez, had failed in the past. And the bill’s success was far from guaranteed when it hit the Assembly floor earlier in the week. The measure initially fell 10 votes short, setting off a dogged arm-twisting effort by Hernandez and other bill supporters.
Ultimately, the “yes” votes came in a rush, giving the bill an ample margin of passage.
State Senate committee approves budget proposal to assist DACA recipients in California
A state Senate budget and fiscal committee on Wednesday approved an additional $30 million in funding for legal services and financial aid to help DACA recipients and young immigrants without legal residency known as “Dreamers.” The budget proposal was struck Tuesday by legislative leaders and must be approved by the time the Legislature adjourns for the year Friday.
California stands with the millions of immigrants who make this state a vibrant and prosperous place. We are suing the Trump administration for canceling the Deferred Action for Childhood Arrivals program, and we are investing millions of dollars in new legal aid to help law-abiding people stay with their families in the U.S.
— Gov. Jerry Brown
Smoking pot or tobacco at California beaches could soon be illegal under bills headed to Gov. Brown

California parks and beaches would be off-limits to those smoking tobacco or marijuana, or using electronic cigarettes, under legislation sent to Gov. Jerry Brown by state lawmakers Wednesday.
The Legislature approved similar bills by Assemblyman Marc Levine (D-San Rafael) and Sen. Steve Glazer (D-Orinda) that would apply the ban to 300 miles of state beaches and areas of 280 state parks that have not been designated by park officials for smoking.
“Californians and the millions of tourists that travel here should be able to visit parks and beaches without stepping around cigarette butts or inhaling secondhand smoke,” Levine said.
Secondhand smoke is a health risk, and discarded cigarette butts contain chemicals that can harm animals that eat them, the lawmakers said. Some health groups support the measures, although the American Cancer Society dropped its support over an amendment.
“This bill would reduce the serious health hazards posed by smoking — to people and wildlife — in our state parks and beaches,” Glazer said. “It would reduce fire hazards and litter and the costs for those now borne by the public.”
A similar bill was vetoed last year by Brown, who said a complete prohibition was too broad.
“A more measured — and less punitive — approach might be warranted,” Brown wrote.
In response, Glazer reduced the fine proposed for violating the ban from $250 to $100, while Levine’s bill would put the penalty at $50.
The ban would not be enforced at parks where signs notifying the public aren’t posted, and parks officials would have power to designate some areas of parks for smoking.
Current law already prohibits smoking within 25 feet of a playground, as well as in public buildings.
The bills exempt use of cigarettes or smoking devices as props in film or television production, and use of tobacco for ceremonial purposes by a federally recognized Native American tribe.
The bills would cost up to $1.1 million for signage, state officials estimate.
------------
UPDATES:
4:37 p.m.: This article was updated to reflect passage of Glazer’s bill.
This article was originally published at 4:25 p.m.
11:45 am on 9/15: This article was updated to reflect that the American Cancer Society dropped support for the bill after it was amended.
------------
Debate about ending daylight saving time in California to continue in 2018

The debate about whether to nix daylight saving time in California will continue in 2018.
Assemblyman Kansen Chu (D-San Jose) plans to have lawmakers take up his bill in January when the Legislature reconvenes.
If approved by the Senate with a two-thirds vote, the proposal to repeal the Daylight Saving Time Act — which was approved by voters in a 1949 ballot measure — will be placed on the 2018 statewide ballot.
Legislators can decide later whether to have the state stay on standard time or adopt daylight saving time year round. Year-round daylight saving time would require federal approval.
This is Chu’s second attempt to end daylight saving time in the state. His previous bill died in the Legislature in 2016.
California bill aiming to block megaprojects from sidestepping key environmental law passes Legislature
California lawmakers vote to give judges discretion over longer sentences in gun crimes

State lawmakers on Wednesday approved a bill that would allow judges to decide against imposing prison-sentence enhancements of 10 or more years in cases where firearms are used to commit a felony.
The Senate sent the bill to Gov. Jerry Brown for consideration after its author, Sen. Steven Bradford (D-Gardena), said crime is not reduced by the current mandate requiring judges to add sentence enhancements if a gun is used.
“I hope this [bill] will lead to more fair and equitable sentencing in cases involving guns where no one is hurt and a shot was not fired,” Bradford said.
The senator said longer sentences do not deter crime, but instead “disproportionately increase racial disparities in prison populations and they greatly increase the population of incarcerated persons.”
The measure passed the Senate on a 21-13 vote with Republicans in opposition, as they were earlier in the week in the Assembly.
Assemblywoman Melissa Melendez (R-Lake Elsinore) noted she recently attended the funeral of a sheriff’s deputy shot to death by a criminal.
“You want to get rid of an enhancement for someone who kills cops?” she asked her colleagues.
Bradford said there still will be cases that will see sentence enhancements.
“This bill does not prohibit firearms sentencing enhancement,” Bradford told his colleagues Wednesday, saying it allows judges to “exercise justice as they see fit,” and “make sure the punishment fits the nature and severity of the crime.”
Kamala Harris on Medicare for all: ‘This should not be thought of as a partisan issue, it’s not even a bipartisan issue’
This should not be thought of as a partisan issue; it’s not even a bipartisan issue. This is a nonpartisan issue. Cancer, diabetes, high blood pressure affect folks around our country regardless of whether they are in a red state or a blue state, regardless of their income, regardless of their status, and we should not differentiate in the way that we do public health policy.
— Sen. Kamala Harris (D-Calif.) on Medicare for all
Central Valley Republicans join Democrats to sponsor Dream Act
Central Valley Reps. Jeff Denham and David Valadao have signed on as co-sponsors of legislation to grant legal status to hundreds of thousands of people brought to the country illegally as children.
Democrats are pushing for a quick vote on the bill, known as the Dream Act, after President Trump announced earlier this month he will end the Obama administration’s Deferred Act for Childhood Arrivals program within six months.
Denham of Turlock and Valadao of Hanford joined two other Republicans who are co-sponsoring the bill, along with nearly 200 Democrats.
“Congress can provide a legislative solution so these individuals may continue to live in America — the only home they know,” Valadao said in a statement.
Denham and Valadao represent districts with large Latino populations and are among the Republicans that Democrats want to oust from office in 2018 as they attempt to win back control of the House. The Democratic Congressional Campaign Committee issued a statement Wednesday morning criticizing the Republicans for not yet co-sponsoring the bill. After the news broke that they would, DCCC spokesman Andrew Godinich said they still need to convince fellow Republicans to support it.
Denham and Valadao urged Trump not to end the program, and House Speaker Paul Ryan (R-Wis.) to allow a vote on legal status for the so-called Dreamers.
Denham posted a public service announcement on his website this week urging Dreamers concerned about being deported to contact his Modesto office. His staff said they are working to get Central Valley radio stations to run it.
Key lawmaker says California energy legislation will hold until next year

Ambitious legislation on clean energy and regional electricity cooperation won’t advance until next year, said Assemblyman Chris Holden, a key committee chairman.
“Every piece of legislation needs work,” he said in an interview on Wednesday.
Holden (D-Pasadena) is directly involved in two controversial energy measures. He authored legislation, Assembly Bill 762, that contains a proposal from Gov. Jerry Brown to lay the groundwork for a regional electricity grid. A separate proposal, Senate Bill 100 from Senate leader Kevin de León, for phasing out fossil fuels for electricity is currently pending in the utilities and energy committee that Holden chairs.
He said both measures should be considered as part of a “comprehensive conversation” next year.
The legislative session ends Friday, and the deadline for amending the measures was Tuesday night. Changes that might be needed to assuage various concerns from utilities, unions and lawmakers were not made.
“There’s not a lot of time for the engagement we need to make it work,” Holden said. He also said there wasn’t enough support in the Assembly to pass the energy legislation.
De León (D-Los Angeles) said during a brief interview in the Capitol that nothing was final.
“It’s too early to tell,” he said when asked if the legislation stood a chance during the last few days.
Assembly Speaker Anthony Rendon (D-Paramount) said it was up to Holden whether the measures advance.
Proposal to expand the L.A. County Board of Supervisors falls short in Senate vote

A proposal to expand the Los Angeles County Board of Supervisors has failed to muster the required two-thirds vote to pass the Legislature, but its author was granted a chance to seek another vote later this week.
Sen. Tony Mendoza (D-Artesia) proposed expanding the board from five to seven members and creating a new, elected chief executive officer to allow for more diverse representation.
He introduced Senate Constitutional Amendment 12, which would have put the expansion on the statewide ballot next year.
The measure was opposed by Los Angeles County officials who said voters in other parts of the state should not decide how the county is governed.
The bill divided L.A. County’s delegation in the Senate. Mendoza offered to remove the elected chief executive provision from the bill to win votes, but that change was opposed by others in the delegation.
The Senate vote was 21-7, with Democrats Hannah-Beth Jackson of Santa Barbara, Holly Mitchell of Los Angeles and Henry Stern of Woodland Hills opposing.
Five other Democrats did not cast votes. The bill would need six more votes in the Senate to pass.
“I believe the decision whether to expand the size of the L.A. County Board of Supervisors belongs with the voters of L.A. County, not voters who live in Humboldt, San Diego or any other county,” Jackson said. “Local governance decisions should remain within the purview of local communities affected by those decisions.”
Key California housing legislation still lacks votes

With less than three days left before state lawmakers adjourn for the year, supporters of legislation to address California’s housing affordability crisis still lack the votes to pass a key bill.
Senate Bill 2 from Sen. Toni Atkins (D-San Diego) would charge a $75 fee on mortgage refinances and other real estate transactions aside from home and commercial property sales. The bill would raise an estimated $250 million a year to help finance low-income housing developments. It requires a two-thirds supermajority vote in both houses of the Legislature to pass.
Assuming no Republicans back the measure, every Democrat has to vote yes. And multiple Democrats in the Assembly who could potentially face tough reelection battles next year remain wary.
The lack of action on SB 2 has held up potentially a dozen or more other housing bills, including Senate Bill 3, a $4-billion bond to fund housing developments on the 2018 statewide ballot, and Senate Bill 35, which would ease some local regulations on home building.
Housing advocates would like to see SB 2 put to a vote even if its passage isn’t guaranteed, if only to see which legislators are opposed.
“It’s tough and we understand why Sen. Atkins wants to fight for the last vote,” said Michael Lane, policy director for the Non-Profit Housing Assn. of Northern California.
If SB 2 doesn’t pass, Lane said he’s hoping its failure won’t torpedo the remainder of the housing bills. Last year, major housing legislation crumbled after Gov. Jerry Brown and lawmakers couldn’t agree on a package to spend more money on low-income housing subsidies while also relaxing local housing regulations.
“There’s no way they can back out of this and have another faceplant,” Lane said.
Which California member of Congress has the toughest fight ahead? We rank them
If Democrats want to reclaim power in the House, they must forge a path through California. Taking multiple factors into account, The Times’ California politics editors have ranked the state’s hottest races by the intensity of the fight ahead for the congressmen (and one congresswoman). We’ll be updating our rankings, and subscribers to the Essential Politics newsletter will be the first to learn what’s changed.
Hearing on cap-and-trade spending deal gets testy

Gov. Jerry Brown and legislative leaders may have reached a deal on spending $1.5 billion in cap-and-trade revenue, but some Democrats still have concerns.
Sen. Hannah-Beth Jackson (D-Santa Barbara) wondered during a budget hearing on Wednesday how much of the appropriations “were designed to meet certain expectations” of different interest groups and lawmakers who supported extending the cap-and-trade program earlier this year. The program requires companies to buy permits to release greenhouse gas emissions, and the revenue is supposed to be spent on initiatives that further reduce emissions.
“There are a lot of Christmas trees out there,” Jackson said. “Everybody wants to pluck a bit of the ornaments, but my concern overall is the whole accountability issue. As you identify these projects, are there certain expectations that you think that they are going to accomplish, because I haven’t seen them.”
Sen. John Moorlach (R-Costa Mesa) questioned a last-minute provision in the spending legislation that could give unions more leverage in negotiations with automakers.
“Who is running this state?” he said.
The provision would ask state regulators to create a process for determining if automakers are “fair and responsible” in their treatment of workers. If they fall short of that standard, their vehicles could become ineligible for electric car rebates in the future.
Moorlach asked what “fair and responsible” meant. Amy Costa, chief deputy director at Brown’s Department of Finance, said it would be up to state officials to develop the guidelines.
Merriam-Webster dictionary is using Rep. Barbara Lee’s words to explain what ‘woke’ means
The brand new Merriam-Webster dictionary definition of “woke” includes a a quote from Rep. Barbara Lee as the example of how to use the word in a sentence.
The online dictionary defined woke on Monday as “aware of and actively attentive to important facts and issues (especially issues of racial and social justice).”
The entry, which she proudly shared on her Twitter account, cites a passage from a June Essence article by Lee (D-Oakland).
“But we will only succeed if we reject the growing pressure to retreat into cynicism and hopelessness. ... We have a moral obligation to ‘stay woke,’ take a stand and be active; challenging injustices and racism in our communities and fighting hatred and discrimination wherever it rises.”
Lee’s career has long been focused on social and racial justice issues. She was mentored by Rep. Shirley Chisholm, the first black woman to run for president, and has worked on education, healthcare, affordable housing and other social issues during her 11 terms representing Oakland.
Her words have often been influential in her liberal East Bay district and among the party’s progressive base.
The slogan “Barbara Lee speaks for me” became a rallying cry among antiwar activists after her lone House vote against the Authorization for Use of Military Force in the days after Sept. 11, 2001, terrorist attacks. The authorization is still used to justify American military actions around the world, and she’s been pushing for a new authorization for 16 years.
Orange County businessman is the latest Democrat to challenge Rep. Mimi Walters
Greg Ramsay, a former healthcare administrator turned ice cream shop owner, will join the already crowded roster of Democrats hoping to unseat Republican Rep. Mimi Walters of Irvine.
Ramsay, 59, said in an interview that while the district’s field is already full of “qualified Democrats,” he believes his military experience and business background will set him apart.
“Democrats on their own don’t have the registration to win this district,” said Ramsay. “I think I have a great chance of attracting that crossover vote [of Republicans and nonpartisans].”
Republicans in Walters’ 45th Congressional District hold a 9 percentage point voter registration advantage, and she has enjoyed large margins of victory in previous elections.
Ramsay, who served in the Navy and worked for years as a contract negotiator for healthcare companies, opened Andrew’s Ice Cream and Desserts in the city of Orange a few years ago.
In a statement announcing his run, Ramsay said he opposes “tax breaks for the rich,” the Trump administration’s decision to end deportation protection for some people under the Deferred Action for Childhood Arrivals program, and President Trump’s decision to ban transgender military service. He said he supports the idea of a single-payer healthcare system.
Six other Democrats have said they’re running for the seat, which is among several the party has in its sights for 2018. They include former Obama administration advisor Brian Forde, UC Irvine law professors Dave Min and Katie Porter, businessman Ron Varasteh, former congressional staffer Kia Hamadanchy and actor Eric Rywalski.
Bill to create ‘safe injection sites’ for drug users fails in California Senate
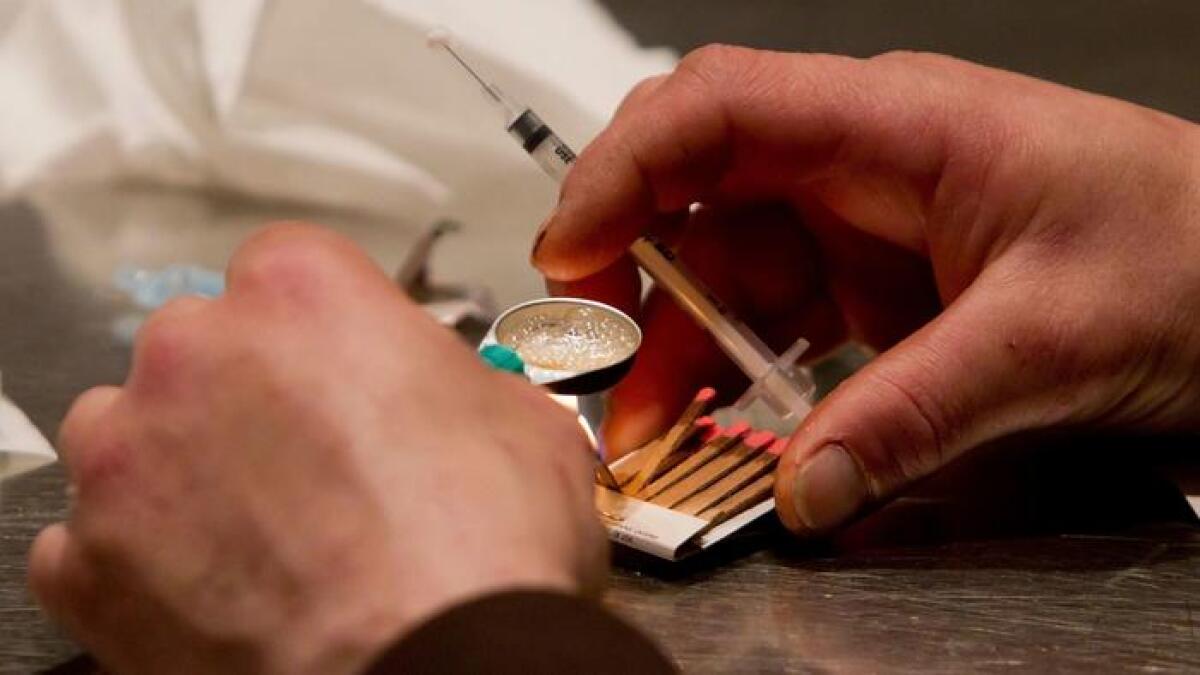
A controversial proposal to allow certain California counties and cities to establish sites where people could inject drugs without legal consequences stumbled in the state Senate on Tuesday night.
The measure, by Assemblywoman Susan Talamantes Eggman (D-Stockton), would establish a first-in-the-nation program in which users of heroin and other intravenous drugs could inject in settings with clean needles and under the supervision of trained staff. The goal: to stave off overdoses in an era in which heroin use is on the rise.
San Francisco is already in discussions to develop an injection center, which is modeled after a site in Vancouver, Canada. State Sen. Scott Wiener, a Democrat who represents San Francisco, said the proposal “gets to the core of who we are as a society in terms of how we respond to that public health crisis.”
“One thing that unites us on both sides of the aisle is we all want people to get off drugs and lead healthy, successful lives,” Wiener said on the Senate floor. “To my colleagues I would ask: How are we doing? How the heck are we doing? I think pretty darn poorly.”
Though supporters saw the potential sites — which the bill would allow in eight counties including Los Angeles and San Joaquin — as a preventive measure against drug deaths, opponents warned such venues would enable illegal activity.
Sen. Ted Gaines (R-El Dorado Hills) said safe injection sites would “create sanctioned shooting galleries for street heroin.”
Republicans were unanimous in their opposition, but ultimately the bill was felled by several Democrats who abstained or voted no. The measure came up two votes short, but it still could come up for a second try before the Legislature adjourns at the end of this week.
California Senate bill headed to Gov. Brown would limit sentence enhancements for some drug charges

A state Senate bill headed to Gov. Jerry Brown would reduce sentence enhancements for some low-level, nonviolent drug offenses, part of a push by Democratic legislators to help young people facing charges or doing time in California.
Under current state law, a person convicted for sale or possession for sale of a small amount of drugs can face a sentence of three to five years behind bars, plus an additional three years in jail for each prior conviction for similar drug offenses.
The legislation, by Sens. Holly Mitchell (D-Los Angeles) and Ricardo Lara (D-Bell Gardens), would repeal the three-year sentence terms for each prior conviction. It moved out of the state Assembly on Tuesday with a 41-25 vote.
Another bill by Mitchell and Lara was sent to Brown last week and would limit the collection of costly court and administrative detention fees against their families. Three more proposals in the legislative package remain pending.
Juvenile justice bills have been at the center of several advocacy and outreach efforts organized this year by actor, activist and musician Common and a coalition of criminal justice organizations, as lawmakers weigh a number of legislative proposals meant to advance the state’s shift away from tough-on-crime policies.
On the Senate floor, Mitchell has called the sentence-enhancement bill a modest reversal of harmful policy under the so-called war on drugs, which disproportionately targeted minorities and has not stopped the flow of narcotics. Supporters urged approval of the bill to counter the direction on drug crimes taken by U.S. Atty. Gen. Jeff Sessions, who directed federal prosecutors to pursue “the most serious, readily provable offense” in drug cases.
Lawmakers block effort to allow 17-year-olds to vote in California elections
California lawmakers blocked an effort to allow 17-year-olds to vote in local and state elections.
Assembly Constitutional Amendment 10, proposed by Assemblyman Evan Low (D-Campbell), failed to gather a required two-thirds vote in the Assembly.
The proposal aimed to promote early civic engagement. It would have made California the first state to allow 17-year-olds to vote in elections.
“This is a bold idea. But bold ideas are required to make significant change,” Low said on the Assembly floor before the vote.
Several legislators raised concerns about whether 17-year-olds have the necessary judgment needed to vote.
“There’s been no reason why 17 is a magic number,” said Assemblyman Matthew Harper (R-Huntington Beach) about lowering the voting age.
Low’s office plans to take the measure up for reconsideration before the Legislature convenes Friday.
Vice President Mike Pence’s fundraising trip to California rescheduled for October

Vice President Mike Pence’s fundraising trip to California, intended to bolster the state’s vulnerable GOP members of Congress, has been rescheduled to October because of ongoing hurricane recovery efforts, according to a person familiar with the planning.
Pence had been scheduled to headline four high-dollar fundraisers in the state on Thursday and Friday alongside House Majority Leader Kevin McCarthy. The largest, a reception and dinner at the Beverly Hilton Hotel in Beverly Hills on Thursday, costs up to $100,000 to attend and was expected to draw a notable crowd of the state’s most influential GOP donors — as well as a vocal group of liberal protesters.
The events are now scheduled to place Oct. 8-10.
The fundraisers are for California Victory 2018, a joint committee that benefits political action committees for Pence and McCarthy, the National Republican Congressional Committee and the congressional campaign accounts of McCarthy and Reps. Darrell Issa of Vista, Dana Rohrabacher of Huntington Beach, Mimi Walters of Irvine, Ed Royce of Fullerton, Steve Knight of Lancaster, David Valadao of Hanford and Jeff Denham of Turlock.
Aside from McCarthy, the other seven members of Congress are being targeted in the midterm elections by Democrats because they represent districts won by Hillary Clinton in the 2016 presidential election. Flipping those seats is key to the Democrats’ effort to retake control of the House in 2018.
California governor, legislative leaders allocate $30 million for ‘Dreamers’ in wake of DACA decision

Gov. Jerry Brown and California legislative leaders have agreed to earmark $30 million for financial aid and legal services to help young people brought into the country illegally as children, a response to President Trump’s recent decision to cancel the Deferred Action for Childhood Arrivals program.
The funding proposal, expected to be taken up Tuesday in a Senate budget and fiscal committee, comes a day after state Atty. Gen. Xavier Becerra filed a lawsuit challenging Trump’s decision to rescind DACA, which grants temporary deportation protection and work permits for about 800,000 people across the country.
The funding includes an additional $10 million for young immigrants without legal residency, known as “Dreamers.” Most of that money will go to state community college students, while $3 million has been allocated for loan programs at California State University and the University of California.
The other $20 million was added Sunday to a pending budget bill. That money that would go to nonprofits that contract with the state to help people apply for or renew their DACA status.
The efforts are part of a larger push by California state leaders working to counter the Trump administration’s call for expanded immigration enforcement and deportation orders.
Gavin Newsom hires veteran Democratic strategist as campaign manager in governor’s race
Unions could get a boost from California’s cap-and-trade spending proposal

Cap-and-trade funding for electric car rebates in California could come with new strings attached, part of a last-minute proposal intended to help unions.
If passed by lawmakers, the legislation would require state regulators to develop a process for determining whether automakers are “fair and responsible in the treatment of their workers” before vehicles can be eligible for the rebates. The change could take effect next summer.
The proposal, part of AB 134 and SB 119, could give unions additional leverage because rebates are an important part of the sales pitch for electric cars, shaving thousands of dollars off the sticker price.
It was inserted into a $1.5-billion plan for spending revenue from the cap-and-trade program, which requires companies to buy permits to release greenhouse gas emissions. The plan includes $140 million for rebates.
Steve Smith, a spokesman for the California Labor Federation, said the proposal should be passed so “when public funds are given to private companies, we know those companies are acting responsibly with respect to their workers.”
Two automakers in particular, Tesla and Nissan, have been embroiled in labor disputes.
The United Auto Workers has been trying to organize employees at Tesla’s factory in Fremont, Calif., where the company is building its new, more-affordable Model 3. Workers filed complaints saying the company was trying to hinder unionization, a charge that Tesla has denied.
Tesla and the United Auto Workers did not immediately respond to requests for comment.
Nissan, which builds the Leaf, faced accusations of unfair labor practices before a union vote in August, when employees rejected an effort by the United Auto Workers to organize a Mississippi factory. The company has denied the accusations.
Global Automakers, which represents Nissan and other companies, sent a letter to lawmakers calling the labor amendment “counterproductive to building a sustainable market for zero emission vehicles.”
“This provision creates an unpredictable standard that would be impossible to adhere to while creating uncertainty in an already challenging market,” wrote Damon Shelby Porter, director of state government affairs for Global Automakers.
Another labor-friendly provision could govern how $140 million is spent on new vehicles at ports. If passed by lawmakers, none of the money could be used for “fully automated cargo handling equipment.”
This post has been updated with more details on the legislation and a comment from the California Labor Federation.
California Assembly bill requiring law enforcement agencies to preserve untested rape kits heads to governor
‘Revenge porn’ victims will be able to maintain privacy in court under new law signed by Gov. Brown

Gov. Jerry Brown on Monday signed a state Senate bill that will allow victims who have intimate images shared without their consent to file a civil lawsuit under a pseudonym to maintain their privacy.
The legislation by Sen. Bob Wieckowski (D-Fremont) was introduced to protect the confidentiality of anyone who brings a civil action against “revenge porn.” Under the new law, when a victim’s pseudonym is used in court, it will also have to be used in all pleadings, documents, proceedings and other case records.
Personal information, such as telephone numbers, email addresses and usernames, and any images of the plaintiff must be redacted or not included in the court file.
Through the law, Wieckowski said he sought to increase the protections put in place by a prior law he authored in 2014. That measure allows victims of revenge porn to seek damages in civil court, and to be able to seek a restraining order to get the offending photos taken down from the Internet.
The bill coasted through the Legislature with bipartisan support.
Court orders Rep. Darrell Issa to pay opponent Doug Applegate $45,000 after failed defamation lawsuit

A judge has ordered Rep. Darrell Issa to pay his opponent from last year’s election more than $45,000 in legal expenses incurred during a defamation lawsuit.
In November, Issa, a Vista Republican, sued Democrat Doug Applegate over attack ads the congressman said hurt his reputation. In March, a judge said Issa didn’t prove his case and sided with Applegate, who argued that he was exercising his free speech rights with the television commercials, and that Issa’s lawsuit was an attempt to silence criticism.
Now the judge has ordered Issa to reimburse Applegate, his campaign, and campaign manager Robert Dempsey for the legal costs of defending themselves against the suit.
Issa’s office referred questions to his attorney, who did not respond to a request for comment. Applegate is running against Issa again in 2018. His campaign manager also did not respond to requests for comment.
Villaraigosa craves return to spotlight in run for governor, but concedes ‘maybe my time is over’

A few dozen migrants from Mexico looked up from the Salinas Valley field where they were picking strawberries and watched Antonio Villaraigosa’s convoy rumble toward them in a cloud of dust.
Moments later, the former Los Angeles mayor, wearing shiny black dress shoes, stepped out of a sedan.
“Hola, señora — Antonio Villaraigosa,” he told Estela Almanza, a fruit sorter.
He inspected a handful of ripe berries for news cameras and greeted Almanza’s coworkers, most of them covered in hats, scarves and hoodies. “Buenas tardes. Hola.”
The harvest was the highlight of a Monterey Bay campaign swing for Villaraigosa, a Democrat running for governor. It came almost 50 years after he broke into politics as an East L.A. teenager, urging Safeway shoppers to join a grape boycott for farmworker rights. He went on to serve as state Assembly speaker and win two terms as mayor.
But now, four years after his mayoralty came to an end, Villaraigosa, 64, is no longer the scrappy upstart whose rise to power symbolized Latinos’ growing clout in California.
Instead, he stands out as the oldest of the top contenders for governor in the June 2018 primary. He is painfully aware that Californians might deny him what he craves: one more act in public life.
“Maybe it passed me up,” he conceded to guests at a July reception in Stockton. “Maybe I’m yesterday’s news. Maybe I’m just a guy who was starting out 20-some-odd years ago, broke glass ceilings — but maybe my time is over.”
The burst of candor was not a sign that he lacks hope; he doesn’t. But it did reflect his recognition that the odds, once again, are stacked against him.
Debate over early California primary is deja vu. And if it passes, it probably won’t change a thing
Big money for clean vehicles in California cap-and-trade spending deal

California will use cap-and-trade revenue for a massive investment in clean trucks, buses, cars and other vehicles, according to details of an agreement obtained by The Times on Monday evening.
The $1.5-billion spending plan comes less than two months after lawmakers extended the state’s cap-and-trade program, which requires companies to buy permits to emit greenhouse gases, until 2030.
The spending negotiations included more money than usual because some was left over from the previous fiscal year, held in reserve by Gov. Jerry Brown until cap and trade’s future was secure.
Here are some highlights on how the $1.5 billion would be spent if it passes the Legislature before it adjourns for the year at the end of the week.
— The biggest-ticket item is $895 million for new vehicles, a priority repeatedly highlighted by Senate Democrats. The money would flow through a variety of programs, including $140 million to the state’s ports, $85 million for farm vehicles and $140 million for electric car rebates.
— Brown originally wanted $300 million to help local regulators improve air quality in polluted neighborhoods, a goal that was packaged with the cap-and-trade extension passed by the Legislature in July. That part of the plan was reworked so the money flows through a clean vehicle program, an investment that supporters hope will yield quicker dividends for the same communities.
— Forest management, fire prevention and emergency response would receive $225 million. This was one of the issues pushed by the Assembly Republicans who voted to help Democrats extend the cap-and-trade program.
— A variety of other programs would see more money under the deal, including $18 million for weatherizing low-income homes, $46 million for urban forestry and greening and $15 million for restoring wetlands.
It’s important to remember that the $1.5 billion doesn’t include all of the cap-and-trade program’s revenue.
An additional $900 million wasn’t up for debate because it’s being automatically distributed according to an annual formula.
That includes $375 million for building the bullet train from Los Angeles to San Francisco.
Smoking pot while driving or riding in a car in California will soon be punishable with a fine
With state-licensed marijuana sales months away, Gov. Jerry Brown on Monday signed a bill that prohibits smoking or consuming cannabis while driving or riding in a vehicle in California.
The measure was written by Sen. Jerry Hill (D-San Mateo) in anticipation of the state’s Jan. 1 start of marijuana sales for recreational use. The new law makes a violation punishable with a $70 fine.
It is already illegal to drive while intoxicated with marijuana and to have an open bag of cannabis in a motor vehicle. The new law bans actually smoking marijuana or consuming cannabis edibles while driving or riding in a vehicle. It is similar to open container laws that prohibit drinking while driving.
In proposing the law, Hill cited a 2012 study by the California Office of Traffic Safety that found more weekend nighttime drivers in California tested positive for marijuana than alcohol.
The governor vetoed another marijuana bill that would have barred marijuana packaging that could appeal to children, such as wrappers that make edibles look like candy. Brown said his administration is already drafting rules to keep children away from marijuana.
California lawmakers vote to reduce penalty for knowingly exposing sexual partners to HIV

State lawmakers on Monday gave final legislative approval to a bill that would reduce from a felony to a misdemeanor the crime of knowingly exposing a sexual partner to HIV without disclosing the infection.
SB 239, which now goes to the governor, was introduced by Sen. Scott Wiener (D-San Francisco), who said the current law discriminated against those who have human immunodeficiency virus, or HIV, the precursor to AIDS, because exposure to other communicable diseases is a misdemeanor.
The same reduction in crime level would apply to people who donate blood or semen without disclosing that they have tested positive for HIV or AIDS.
“Right now HIV is singled out for uniquely harsh treatment as a felony,” Wiener told his colleagues during the floor debate.
Republicans, including Sen. Joel Anderson of San Diego, voted against the bill, saying it puts the public at risk.
“I’m of the mind that if you purposefully inflict another with a disease that alters their lifestyle the rest of their life, puts them on a regiment of medications to maintain any kind of normalcy, it should be a felony,” Anderson said. “It’s absolutely crazy to me that we should go light on this.”
He said tougher penalties should be extended to those who expose others to other infectious diseases.
Sen. Jeff Stone, a Republican pharmacist from Murrieta, also said it should remain a felony if someone exposes a partner to HIV, which he said would “condemn one to probably $1 million in drug therapy for the rest of their lives.”
Wiener noted that modern drug treatment can make someone with HIV noninfectous to others, but he said the law had not kept up with science.
He said some people may choose not to be tested if it makes them liable for a felony should they expose someone they have sex with to HIV.
“These laws do not prevent HIV infections,” Wiener said during the debate. “All they do is stigmatize people living with HIV and reduce access to testing and care.”
The bill is supported by groups including the American Civil Liberties Union of California, the Black Aids Institute and Equality California, which advocates for the LGBTQ community.
Iraqi and Afghan refugees could soon pay resident student tuition at California community colleges

Iraqi and Afghan refugees who worked with the U.S. Armed Forces, whether as interpreters, translators or advisors, could soon be exempted from paying nonresident student fees at community colleges in California.
State legislation filed by Assembly members Kevin McCarty (D-Sacramento), Lorena Gonzalez Fletcher (D-San Diego) and Adrin Nazarian (D-Sherman Oaks) would extend in-state tuition and eligibility for state-administered financial aid programs to refugees with special immigrant visas.
It moved out of the state Assembly Monday with a 51-1 vote and no debate. It now heads to Gov. Jerry Brown for final approval.
California received more than 725,000 refugees between 1975 and 2015. Nearly 8,000 arrived in 2016. The bill was part of legislation that sought to better integrate refugee families amid what lawmakers called religious- and racially charged rhetoric at the federal level spurring fear and confusion in their districts’ refugee and immigrant communities.
Another bill that would have helped refugees with special immigrant visas to apply relevant work experience obtained overseas toward a professional license was held in a Senate Judiciary Committee. But McCarty, Gonzalez Fletcher and Nazarian were able to secure a $10-million allocation in this year’s budget deal for school districts with high student refugee populations.
The funding will allow schools to hire translators and counselors for refugee students.
Lawmakers said legislation passed Monday would provide access to education for many displaced families. Tuition and fees vary across California. At state community colleges, resident students pay $46 per college credit. Nonresident fees vary by the district, but the statewide average is $234 per credit.
California may slow revolving door of legislators becoming lobbyists

A measure aimed at slowing the revolving door of California legislators becoming lobbyists was given final approval by lawmakers Monday and sent to Gov. Jerry Brown for consideration.
The measure, Assembly Bill 1620 by Assemblyman Matt Dababneh (D-Woodland Hills), would change the current rule that prohibits legislators from lobbying state agencies for one year after resigning from office. Depending on when they step down, they could be banned for as long as three years under the new rule — with no lobbying allowed during the two-year session after they were elected, and one year after that session.
Some legislators have resigned mid-term to go to work for interest groups lobbying the state government, and are only subject to a one-year waiting period.
“This has eroded and undermined confidence in our institution,” Dababneh said.
Lawmakers sign off on bill to give California teachers paid pregnancy leave

A bill that would provide paid pregnancy leave for teachers and school employees passed the California Assembly on Monday, and will go to Gov. Jerry Brown’s desk.
The bill, written by Assemblywoman Lorena Gonzalez Fletcher (D-San Diego), would require public and charter schools to give teachers and staff paid time off for pregnancy, childbirth, miscarriages or other reproductive health issues. It passed the Assembly, 52 to 11. It previously passed the Senate by a 31-8 vote.
Teachers currently have to use vacation or sick days, or forfeit pay, in order to take time off during a pregnancy.
“Female teachers shouldn’t face extra employment burdens simply because they’re pregnant,” Gonzalez Fletcher said in a statement. “It’s unfair. It’s discriminatory. And it will drive more and more women away from the profession at a time when we can least afford to do so.”
About 73% of California’s teachers are women, according to data analyzed by the state Department of Education.
From the Trust Act to the ‘sanctuary state’ bill: A bitter fight over which immigrants California should protect

Negotiations are coming down to the wire on Senate leader Kevin de León’s so-called sanctuary state legislation, which would limit state and local law enforcement agencies from enforcing federal immigration laws.
Gov. Jerry Brown has said the goal of Senate Bill 54 should be to curb federal power, but that some immigrants in the U.S. illegally who have committed crimes “have no business being in the country.”
For those who remember the passage of the bill’s predecessor, the California Trust Act, the debate is familiar.
Like De León’s legislation, the Trust Act was introduced by Democrats to blunt the impact of federal policy on immigrant communities. And it also ignited a bitter fight over who the state should protect when the federal government casts a wide deportation net that can entangle hardworking families and criminals alike.
Vice President Pence cancels California fundraising trip because of hurricanes

Vice President Mike Pence’s California fundraising trip scheduled for later this week has been canceled because of hurricane recovery efforts, according to the Beverly Hills Police Department.
Pence had been scheduled to headline four high-dollar fundraisers in the state on Thursday and Friday to bolster California’s vulnerable GOP members of Congress, according to invitations obtained by The Times.
The largest – a reception and dinner at the Beverly Hilton on Thursday – cost up to $100,000 to attend.
Lt. Michael Hill of the Beverly Hills Police Department said the agency had been informed by the U.S. Secret Service that Pence would no longer be attending. He said it was unclear if the remainder of the fundraiser, which features House Majority Leader Kevin McCarthy, would go on as scheduled or if it would be postponed altogether.
Protesters had been planning to greet Pence, with more than 300 people saying on social media they planned to attend a demonstration outside the hotel organized by liberal groups opposed to President Trump’s agenda. Another 2,000-plus people indicated they were interested in the protest.
The American Civil Liberties Union had also gotten involved, sending a letter to police and city officials questioning the police department’s interaction with protest organizers and the permitting procedures.
Hill said he was aware of the letter but that the department had not yet responded to it.
The fundraisers were supposed to benefit California Victory 2018, a joint fundraising committee that benefits Pence’s and McCarthy’s political action committees, the National Republican Congressional Committee and the congressional campaign accounts of McCarthy, Darrel Issa of Vista, Dana Rohrabacher of Costa Mesa, Mimi Walters of Irvine, Ed Royce of Fullerton, Steve Knight of Palmdale, David Valadao of Hanford and Jeff Denham of Turlock.
Law that would expand firearms ban on California campuses goes to Gov. Jerry Brown’s desk

A measure that would expand a firearms ban on school campuses in California won final legislative approval Monday and was sent to Gov. Jerry Brown, a rifle owner who has been skeptical about some gun control measures.
The measure approved by the state Assembly on Monday eliminates the power of school district administrators to give people with concealed weapon permits permission to have firearms on K-12 campuses.
Assemblyman Kevin McCarty (D-Sacramento) said the state’s gun-free-zone law was amended two years ago to allow superintendents to authorize guns to be carried on campuses in rare situations, including when someone is the victim of domestic violence.
“The risk of having something bad happen with that firearm is greater than the reward,” McCarty said.
The bill is opposed by gun rights groups, including the National Rifle Assn., as well as most Republican lawmakers.
“You are not keeping people safe by doing this,” said Assemblyman James Gallagher (R-Yuba City). “You are taking away people’s rights and you are taking away people’s ability to defend themselves.”
A separate gun control bill that is also on its way to the governor’s desk won a unanimous vote in the Assembly. The measure by Assemblyman Reggie Jones-Sawyer (D-Los Angeles) added two hate crimes involving use of force to intimidate people based on race, sex or sexual orientation to the list of misdemeanors that result in a ban on the right to have a firearm for 10 years.
California Assembly bill to protect tenants from deportation heads to Gov. Jerry Brown

The California Assembly sent a bill to Gov. Jerry Brown on Monday that would prohibit landlords from threatening their tenants with deportation and establish protections for immigrants in eviction cases.
The legislation by Assemblyman David Chiu (D-San Francisco) would bar landlords from disclosing information about immigration status in order to intimidate, harass or evict tenants without following proper procedures. It also would allow immigrant tenants to file civil claims against their landlords if they do.
In such eviction cases, attorneys would be prohibited from threatening to report the immigration status of tenants under the legislation’s provisions.
The bill moved out of the Assembly with a 49-18 vote without debate.
The legislation comes as immigrant rights groups in Los Angeles, the Bay Area and other areas across the state have received reports of landlords threatening to report tenants to immigration authorities unless they move out. Often, advocates say, the threats are in response to tenants reporting issues such as exposed electrical wiring or vermin.
Another state Assembly bill pending approval in the Senate would ensure that no state office or entity in California could compel a landlord to obtain and disclose information on a tenant’s immigration status.
“Trump’s escalating war on immigrants is ripping apart families and mass deportations could be our new reality,” Chiu said in a statement. “This bill will deter the small minority of landlords who unscrupulously take advantage of the real or perceived immigration status of their tenants to engage in abusive acts. I appreciate the support of the Senate.”
Times reporter Melanie Mason contributed to this story.
California lawmakers ease permitting rules for Uber and Lyft drivers

Drivers for Uber and Lyft will only need one business license to work statewide under legislation headed to Gov. Jerry Brown’s desk.
Senate Bill 182, which passed the state Senate Monday, would require a single license to drive passengers anywhere in the state, which drivers can obtain in the city where they live. Local governments don’t typically enforce rules that require ride-hailing drivers to have business licenses, but in theory every city a driver passes through could charge a fee.
Uber and Lyft supported the measure, saying they wanted to prevent their drivers from having to comply with a patchwork of rules across the state. The bill’s author, Sen. Steven Bradford (D-Gardena), has said the state needs to help facilitate new ride-hailing technology.
Cities, especially San Francisco, were opposed to the bill, arguing it would hurt their ability to raise revenues and regulate the industry.
California lawmakers take action to help ‘independent’ voters when it comes to voting in presidential primaries
Rep. Keith Ellison to headline Orange County Democratic fundraiser

Democratic National Committee Vice Chair Keith Ellison is headlining the Orange County Democratic Party’s biggest fundraiser of the year later this month.
Ellison, a Minnesota congressman, will speak at the Harry S. Truman Awards Dinner on Sept. 23 at the Hilton Hotel in Costa Mesa. Individual tickets cost $190, while the top-tier ticket costs $1,000 and includes entry to a VIP reception and premium seating during the dinner.
The theme for the event is “Orange is the New Blue,” a reference to the changing politics in the one-time conservative bastion that was the home of the late President Nixon and the foundation of the late President Reagan’s political career.
In 2016, Orange County’s voters supported Hillary Clinton in the presidential campaign, the first time they supported a Democrat for the White House since the Great Depression. And Orange County is home to four congressional districts that Democrats are targeting in their effort to retake the House in 2018.
Bill to provide free tampons in schools with low-income students heads to governor’s desk

A bill to provide free menstrual products in public schools with low-income students is heading to the governor’s desk.
AB 10 by Assemblywoman Cristina Garcia (D-Bell Gardens) would require Title I-funded schools with students in grades six through 12 to stock restrooms with feminine hygiene products. It passed the Assembly 63-0 on Monday, and now goes to Gov. Jerry Brown for his signature.
“We hear stories about young girls who miss school on a daily basis or extend the use of their menstrual products and get infected,” Garcia said on the Assembly floor before the vote.
Gov. Jerry Brown and Senate leader Kevin De León strike deal on changes to ‘sanctuary state’ legislation

Gov. Jerry Brown and state Senate leader Kevin de León agreed Monday to amend a “sanctuary state” bill that would limit the role of state or local law enforcement agencies in holding and questioning immigrants in the country illegally.
Senate Bill 54, which De León introduced earlier this year, would prohibit police and sheriffs from asking about a person’s immigration’s status, detaining people for U.S. Immigration and Customs Enforcement “hold” requests and participating in any program that deputizes police as immigration agents.
Brown had made it clear he wanted changes to the original language of SB 54, and those negotiations have been underway at the state Capitol for several weeks.
Under amendments endorsed by Brown on Monday, the bill would allow law enforcement officers to transfer and share information about inmates convicted of roughly 800 crimes not specified in the bill’s earlier iterations.
That list of offenses, which include many types of felonies but also crimes that could be charged as misdemeanors, was originally crafted as part of the Trust Act, which Brown signed in October 2013, and prohibited law enforcement agencies from holding people for ICE longer than 48 hours for most minor crimes.
Other major amendments include:
- Immigration authorities would be able to interview people in jails, but will not be given permanent office space in jails.
- Officials from the California Department of Corrections and Rehabilitation would be exempt from the bill, but required to provide increased protections for immigrant inmates and required to offer them the same chance as other prisoners at earning time credits toward their sentences.
- Federal immigration agents would have access to law enforcement databases. But the state attorney general’s office would develop recommendations that would largely limit the agents’ access to information.
- A series of technical changes to the bill’s language to ensure officers can participate in joint task forces.
“This bill protects public safety and people who come to California to work hard and make this state a better place,” Brown said in a statement.
SB 54 has attracted national attention and is the centerpiece in Democrats’ legislative agenda to protect immigrants without legal residency after President Trump’s call for expanded deportations.
To address concerns from Republican lawmakers and sheriffs, De León amended the bill earlier this year to allow officers to continue working on federal task forces not focused on immigration enforcement, and to permit greater communication between ICE and law enforcement regarding felons with violent or serious convictions.
But the California Sheriffs Assn. still opposed the bill, while immigrant rights groups urged Brown not to cave in to those demands at a time of fear for immigrant communities.
The Sherrifs Assn. did not immediately respond to requests for comment. The California Police Chiefs Assn., which opposed the bill, said it has switched its position to neutral.
“The compromise reached on Senate Bill 54 does two things: It addresses the significant public safety concerns we raised during this debate, and it reaffirms what we have held since the beginning, which is that California law enforcement should not be used to assist in mass deportations,” said Gardena Police Chief Ed Medrano, president of the police chiefs group.
Joseph Tomás McKellar, co-director of the immigrant rights group PICO California, said in a statement Monday that the bill isn’t perfect but would “ensure California leads the country towards keeping thousands of families united while rebuking the demonization and scapegoating of immigrants and other racially and economically excluded groups.”
The bill must still be approved by the state Assembly, where its fate has remained uncertain. Final action must come before lawmakers adjourn for the year Friday.
A spokesman for Assembly Speaker Anthony Rendon said he “supports SB 54 and the compromise reached by Gov. Brown and Sen. De León.”
UPDATE
5:21 p.m.: This article was updated with additional details about the amendments, and with reaction from law enforcement associations and Assembly Speaker Anthony Rendon.
This article was originally posted at 2 p.m.
California sues Trump administration over plan to end DACA

California on Monday sued the Trump administration, challenging as unconstitutional the president’s plan to rescind a program to protect young immigrants brought to the country illegally from deportation.
The lawsuit comes a week after 15 other states, led by New York and Washington, filed a similar legal challenge.
California Atty. Gen. Xavier Becerra said Monday he decided to file a separate suit because the state and its economy will be especially harmed by the president’s action because it is home to a quarter of the 800,000 people in the Deferred Action for Childhood Arrivals, or DACA, program.
“I think everyone recognizes the scope and breadth of the Trump decision to terminate DACA hits hardest here,” Becerra said after the other states sued.
Becerra’s lawsuit says the DACA program approved by former President Obama is legal and that its repeal violates due process rights and will hurt the state’s economy.
“It’s fully lawful, it’s totally American in its values and it’s an unmitigated success for California’s economy and the country’s economy,” Becerra said in a recent interview.
The lawsuit is joined by Maine, Minnesota and Maryland and argues in part that the repeal “may lead to the untenable outcome that the [Trump] Administration will renege on the promise it made to Dreamers and their employers that information they gave to the government for their participation in the program will not be used to deport them or prosecute their employers.”
The lawsuit was criticized Monday by Robin Hvidston, who heads a California group seeking tougher enforcement of immigration laws.
“It’s misguided and premature and a misuse of tax dollars,” said Hvidston, executive director of the Claremont-based group We the People Rising.
She noted that President Trump delayed repeal of the program for six months to give Congress a chance to address the issue, and that several Republican-led states have sued to end the DACA program.
Political party insiders would love to scrap California’s top-two primary system

Political parties and open primaries are the electoral equivalent of oil and water. They may coexist, but they don’t mix.
So it’s hardly surprising that neither California’s dominant Democrats nor its fading Republicans have ever really embraced Proposition 14, the sweeping ballot measure that abolished partisan primaries six years ago.
Some, in fact, say they’ve seen enough. It’s time to scrap it.
Ahead of final week, California lawmakers change bills to garner support for housing package

A package of bills to address California’s housing affordability crisis inched forward late last week ahead of a do-or-die week in the Legislature.
Lawmakers introduced or changed two bills aimed at attracting support for key parts of the housing package from wary colleagues and Gov. Jerry Brown.
SB 2 from Sen. Toni Atkins (D-San Diego) would charge a $75 fee on mortgage refinances and other real estate transactions other than home sales and use the estimated $250 million raised a year to help finance low-income housing construction. But Atkins has struggled to secure the two-thirds supermajority vote of the Assembly needed. No Democrats in the Assembly can vote against the measure for it to pass.
Late Friday, Assemblyman Rudy Salas (D-Bakersfield) authored a new bill, AB 166, that would allow low-income residents to bypass the $75 fee. Salas, who was the only Democrat in the Assembly to vote no on a gas-tax increase earlier this year, was also considered a potential holdout on SB 2. It was unclear if the introduction of AB 166 is enough to secure SB 2’s passage.
Also late Friday, Assemblyman Richard Bloom (D-Santa Monica) changed his legislation, AB 1505, which would allow cities to force developers to set aside a certain number of homes in their projects for low-income residents.
Brown has long opposed the policy, vetoing a similar bill in 2013 and saying the policy generally makes it harder to attract development to low- and middle-income communities.
The changes to the bill would allow the state Department of Housing and Community Development to review proposed local ordinances to ensure that the cities don’t use these rules to block all development.
On Twitter, Bloom characterized the amendments as minor:
Other major housing legislation lawmakers are considering include a $4-billion bond for the 2018 ballot to finance low-income development and provide home loans for veterans, and new rules aimed at easing local development regulations. The deadline for all bills to pass both houses of the Legislature is Friday.
Retirement watch: Who in California’s congressional delegation is most likely to leave Washington?
No one in the country’s largest state delegation to Congress has announced plans to retire by 2018. Yet.
Still, members who are thinking about it are considering things like health issues, federal investigations and even the chance of the House switching chambers in 2018.
They have until March to decide, but we’re keeping a particularly close eye on a handful.
California Atty. Gen. Xavier Becerra to announce a lawsuit challenging Trump’s DACA decision

California on Monday will wade into the legal battle over President Trump’s decision to scrap the nation’s 5-year-old program protecting young immigrants without legal residency.
Atty. Gen. Xavier Becerra plans to announce a lawsuit against the Trump administration over last week’s rescinding of the Deferred Action for Childhood Arrivals program, known as DACA. The action is scheduled to be announced at a late morning event in Sacramento, and a news release from the attorney general’s office said he will appear at the event with several DACA recipients from California.
The decision comes five days after a coalition of 15 states announced joint legal action against the president’s decision to cancel the program next March. Becerra made it clear a week ago that he intended to challenge the action in court, a decision supported by Gov. Jerry Brown’s administration. He was one of 20 state attorneys general who wrote to Trump in July urging the program be kept in place.
The lawsuit will be the second filed by California officials. Last week, the University of California took legal action against the DACA decision on grounds that it would violate the due process rights of thousands of immigrant students on “nothing more than an unreasoned executive whim.”
California is estimated to be home to more than one in every four DACA program recipients. On Sunday, protesters denounced Trump’s decision during an event at MacArthur Park in Los Angeles.
FOR THE RECORD
8:51 a.m.: An earlier version of this article stated that Atty. Gen. Xavier Becerra planned to announce the lawsuit on Tuesday. It is to be announced on Monday.
California Politics Podcast: The state’s lawmakers lash out at Trump’s decision on young immigrants
Few states have a larger stake than California in the fate of the young immigrants enrolled in a controversial federal program that President Trump moved to cancel last week.
And lawmakers from both major parties are calling for a solution that would allow those young men and women to stay in the country.
This week’s California Politics Podcast takes a closer look at the reaction in political circles to Trump’s decision to abandon the Deferred Action for Childhood Arrivals program, or DACA.
We also preview the biggest topics still on the to-do list of the Legislature as it wraps up its work for the week.
I’m joined by Times staff writer Melanie Mason and Marisa Lagos of KQED News. You can subscribe to the weekly podcast on iTunes, Soundcloud and Stitcher.
What’s in Gov. Jerry Brown’s regional electric grid proposal? Here are the details

After years of stop-and-go, behind-the-scenes negotiations, Gov. Jerry Brown’s proposal to integrate California’s electricity grid with neighboring states will finally be unveiled.
The proposal, which was obtained by The Times on Friday, has not yet received a public hearing, and is only being introduced with a week left in the legislative session.
The effort involves a sweeping transformation at the California Independent System Operator, which runs most of the state’s electricity grid. Right now the organization, known as Cal-ISO, is run by a board chosen by the governor and confirmed by state senators.
Under the new proposal, Cal-ISO would launch a discussion with regulators and utilities in the region to create a new governance structure where oversight is shared among multiple states. The process would be completed by Oct. 31, 2018.
At that point, the plan would be reviewed by a commission of eight California officials, including four state lawmakers, three state regulators and the governor. A final determination would be due by Dec. 31, 2018.
Brown’s office has managed to reach a consensus with trade unions that have previously resisted a regional plan over concerns that jobs would leave California.
But pushing the proposal through the Legislature is no sure thing. Senate President Pro Tem Kevin de León (D-Los Angeles) is skeptical of any plan that would reduce the state’s authority over its electricity grid.
In addition, there are concerns among some advocates that changing how the grid is managed could invite interference from federal regulators appointed by President Trump, who has been hostile to the kind of environmental initiatives valued by California.
Sen. Kamala Harris heads to a key presidential battleground state to fundraise for a fellow senator

Sen. Kamala Harris headed to Ohio on Friday for a two-day fundraising swing.
The fundraisers are not for her — they’ll benefit her Senate colleague Sherrod Brown, who is up for reelection next year. But Harris’ appearance in the presidential battleground state is sure to draw attention given the speculation swirling around her political future.
Harris is the special guest at five fundraisers for Brown in Cincinnati, Columbus and Shaker Heights.
A prodigious fundraiser, she has already been active raising money for 2018 candidates through her email lists and political action committee. But the trip to Ohio is the first time she has ventured to another state to headline a fundraiser.
Harris’ advisors have avoided sending her to states or events that would overtly signal presidential ambitions, such as Los Angeles Mayor Eric Garcetti’s recent trip to campaign for a Manchester, N.H., mayoral candidate.
But her travel schedule is expected to increase in coming months, as she campaigns and raises money for 2018 House and Senate candidates. In each of these visits, Harris will forge relationships with key Democratic elected officials, party leaders and donors — all building blocks she will need if she seeks the party’s presidential nomination in 2020.
Harris’ name is a constant on speculative lists about Democrats contemplating a White House bid, a reflection of how much her political profile has skyrocketed this year, fueled by a headline-making speech at the Women’s March on Washington in January, pointed questioning of President Trump’s appointees during Senate confirmation hearings and viral video of GOP male colleagues interrupting her.
The senator and her team have taken pains to tamp down presidential speculation, given that Harris was sworn in just eight months ago. Most recently, MSNBC host Lawrence O’Donnell broached Harris about her 2020 intentions.
“Lawrence, I don’t even know what I’m having for dinner,” Harris responded, and then burst into laughter.
Santa Clara Valley beer magnates host political fundraiser for Gavin Newsom

Santa Clara Valley beer distribution magnates and philanthropists Michael Fox Sr. and his wife, Mary Ellen Fox, are hosting a fundraiser for Democratic Lt. Gov. Gavin Newsom’s campaign for governor at their home in Saratoga in late September.
The “suggested” price to be a “chair” of the cocktail reception fundraiser and get two tickets is writing a check for or raising $29,200. Other suggested donation levels are $5,000 or $15,000.
Prominent San Francisco attorney Jeremiah F. Hallisey, a former University of California regent and Democratic National Committee member, is helping organize the Newsom fundraiser.
Initiative to give younger homeowners property tax breaks will cost local and state governments billions of dollars

A proposed 2018 statewide initiative to extend Proposition 13’s property tax breaks from older to younger homeowners ultimately will cost local governments and the state billions of dollars a year, according to a financial analysis of the measure released Friday.
The measure, proposed by the California Assn. of Realtors, would allow any California homeowner to sell a house and apply a portion of its existing property tax rate — which is capped under Proposition 13 — to a new home. Similar benefits are already available in some cases to homeowners older than 55.
The fiscal analysis from the nonpartisan Legislative Analyst’s Office found that cities and counties would receive less money because the measure would reduce the increase in property taxes that often accompanies the purchase of a new home. Similarly, state costs would grow because of constitutional requirements to replace any lost property tax dollars that would otherwise have helped fund K-12 schools.
The analysis also found that home sales could increase by tens of thousands a year, but that the ultimate effect on home prices was unclear.
The California Assn. of Realtors also has proposed two ballot measures that are less expansive, one that would extend the rules for older homeowners to apply property tax breaks to new homes and the other to all homeowners moving within specified counties. Financial analyses for those measures found local and state government costs would be lower, but would still require more state tax revenue to fund schools.
Alex Creel, senior vice president and chief lobbyist for the California Assn. of Realtors, said his organization planned to review the financial analyses, the forthcoming title and summary of the ballot initiatives written by the attorney general’s office and potentially conduct polling before deciding whether to mount a campaign for the November 2018 ballot.
“Without the full picture, at this point it’s too early to say exactly what path we’ll take,” Creel said in a statement.
Conservative blogger files complaint about Republican Travis Allen’s spending in campaign for California governor

California’s campaign watchdog agency has launched an investigation into a complaint filed against Republican Assemblyman Travis Allen of Huntington Beach that alleges he misspent funds in his campaign for governor.
The complaint to the Fair Political Practices Commission was filed by conservative blogger Aaron Park, who lives east of Sacramento. It is common practice for the agency to launch an investigation whenever it receives a complaint.
In the complaint, Park alleges Allen used donations from an Assembly campaign account to pay for Facebook ads to support his run for governor. Park argued that would be a violation of the state’s Political Reform Act.
Park supports Allen’s Republican rival in the governor’s race, Rancho Santa Fe businessman John Cox. He believes Allen should drop out, arguing that the assemblyman doesn’t have enough political support or fundraising capability to win.
“I’m a supporter of John Cox and have been very early on,” Park said. “And I don’t know why Travis is running for governor. I really don’t. It just seems really bizarre to me.”
Maryann Marino, spokeswoman for Allen’s gubernatorial campaign, said all of Allen’s spending and expenditures were proper and reported on campaign finance reports filed with the California Secretary of State’s office. Marino said “the FPPC inquiry will not come up with anything.”
FPPC spokesman Jay Wierenga acknowledged that the agency received the complaint, but did not address the substance of allegations since the matter is under investigation.
Allen, 43, was first elected to the state Assembly in 2012 and announced his bid for governor in June. He worked as a certified financial planner before he ran for the California Legislature.
Park, in his complaint, also questioned whether a Facebook page that Allen created to support his Assembly campaigns, which he said were promoted in social media ads, could be converted for use by Allen’s gubernatorial campaign.
Additionally, the website run by a committee Allen formed to support his statewide ballot initiative to repeal the recently approved gas tax also appeared to solicit donations for his campaign for governor.
The initiative’s website, which was paid for by the “Join Travis Allen to Repeal the Gas Tax Ballot Measure Committee,” asked supporters to make their donation checks payable to “Travis Allen for Governor 2018.” State regulations may bar this since the two are separate and distinct campaigns.
After Marino was contacted by The Times, the initiative website was changed. It now says donation checks should be made payable to “Join Travis Allen to Repeal the Gas Tax Ballot Measure Committee.”
Marino said that was due to a technical error and added that very few donations are made by check.
‘We are here, see us’: California Congress members greet ‘Dreamers’ fasting on Capitol lawn
About a dozen Democrats, mostly Californians, left the Capitol on Thursday to check on the two dozen people fasting on the lawn over President Trump’s decision to end the Deferred Action for Childhood Arrivals program.
Rep. Lucille Roybal-Allard of Downey said the members wanted to let the people who were fasting know they are not alone and “there are people in Congress, in positions of power fighting for them every single day.”
Organized by Center for Community Change and United We Dream, the fasting DACA recipients wanted to be a visual reminder after Trump decided this week to end the program that gives legal status to about 800,000 people brought to the country illegally as children.
“We are here, see us, hear us,” said Center for Community Change spokeswoman Jasmine Nazarett. “The fasters are giving up everything, they are giving up food for four days to call attention, as an appeal to the moral core of the country, of the president, of the Congress.”
Nazarett said the fast began Tuesday morning just before Atty. Gen. Jeff Sessions made the announcement about the program’s phaseout and will end Friday evening with broth and Jell-O.
The fasting DACA recipients, also known as “Dreamers,” traveled from places like Arkansas, Colorado, New York, Arizona and California. Throughout the week, they went into the House and Senate office buildings to try to meet with members of Congress.
Rep. Karen Bass of Los Angeles said she felt an emotional connection to a group of young people willing to travel across the country and put themselves at risk.
“They put themselves physically at risk — the fast — and they put themselves at risk because who’s to say ICE won’t come right there and scoop them up right now,” Bass said. “So, the least we could do is to show them solidarity by coming out and letting them know we support them.”
Effort to crack down on dialysis clinics stalls in California Legislature
A measure to impose stricter regulations on for-profit dialysis clinics that treat patients with chronic kidney disease was tabled for the year on Friday by the bill’s author, Sen. Ricardo Lara (D-Bell Gardens).
The proposal, backed by Service Employees International Union-United Healthcare Workers, would have mandated the number of employees administering treatment at clinics, increased inspections and required a 45-minute transition time between patients.
Lara said in a statement that he introduced the measure “in response to the shocking stories I heard from patients and workers about lack of protections and oversight in this rapidly expanding industry.
“Dialysis in California is a billion-dollar industry yet we treat it like a Wild West with bare minimum standards,” he said.
The bill was fiercely opposed by clinic operators, as well as some physician and patient groups.
Lara said he would convene talks with the governor’s office, the industry, labor and patient groups to advance the bill next year.
SEIU-UHW has filed two ballot measures for 2018 as a backup plan should their legislation fail.
“This legislation has successfully raised awareness of the disturbing patient care problems in dialysis clinics that the industry claimed were not happening, and we are eager to have productive discussions to find solutions that improve patient care for the 66,000 Californians who need dialysis to survive,” said Dave Regan, president of SEIU-UHW, in a statement.
“If the discussions are not productive, we will ask California voters to stand up for dialysis patients through a statewide ballot initiative planned for the November 2018 election.”
Union negotiations pave way for Gov. Jerry Brown to advance ambitious plan for regional electricity grid

Gov. Jerry Brown is clearing a major obstacle in his push for closer energy cooperation between California and its neighbors, but the outcome remains far from certain in the final week before lawmakers adjourn for the year.
The governor wants California’s electricity grid to be integrated with those of other states, making it easier and more cost effective to share renewable energy around the region. The concept could eventually reshape the energy landscape in the West by providing a wider market for solar, wind and hydroelectric power.
Brown’s efforts have previously stalled in the face of opposition from construction unions that fear new power plants would be built outside California, costing them jobs.
But behind-the-scenes negotiations between the governor’s office and labor leaders have created a framework to advance the regional proposal, according to sources with knowledge of the conversations who declined to be identified while details are still being discussed.
The proposal would lay the groundwork for transforming California’s electricity grid operator into an independent board that could serve the broader region, a process requiring lengthy negotiations among multiple states. Sacramento would no longer have sole oversight over the grid, which is currently managed by a board appointed by the governor and confirmed by state senators.

Union concerns about jobs could be assuaged through a proposal that’s currently part of Assembly Bill 813. The bill would expedite utilities’ plans to purchase renewable energy, taking advantage of federal tax credits that are scheduled to start expiring next year.
The acceleration could help ensure more renewable projects are built and operated in California.
More challenges remain if Brown wants to push through legislation this year. The legislative session ends in a week, and lawmakers are already confronting sharp divisions on other energy issues.
Front and center is the increasingly bitter battle over a proposal to phase out fossil fuels for generating electricity by 2045. The legislation by Senate President Pro Tem Kevin de León (D-Los Angeles) is facing opposition from unions representing electrical and utility workers.
Ramping up renewable energy to the level sought by De León requires more regional cooperation, some environmental advocates insist. However, the Senate leader has been skeptical because state officials would have to sacrifice some of their influence over the grid if it’s integrated with other states’ operations.
All of these issues remain in flux with little time left to finalize the details.
“Lots of things are being done on the backs of envelopes right now,” said Tom Dalzell, business manager for the International Brotherhood of Electrical Workers Local 1245.
Former Rep. Loretta Sanchez to executive produce political drama for NBC

Ten-term former Rep. Loretta Sanchez is coming to Hollywood — only this time, instead of asking for money, it looks as if she’s aiming to make some.
Sanchez, a Democrat from Santa Ana who served 20 years in the House and ran for Senate in 2016, is named as an executive producer on a political drama that just got a script commitment from NBC, the Los Angeles Times has confirmed.
Lawmaker revives bill that would scale back sex offender registry in California

A proposal to end the lifetime listing of many convicted sex offenders on a public registry in California was revived Friday when its author put the language in a separate bill, bypassing a committee that shelved the measure last week.
Sen. Scott Wiener (D-San Francisco) took a bill he authored that would extend the hours of bars in the state, gutted it of its old language and added the proposal to change the sex offender registry program.
The new bill, SB 384, would require that the names of those who committed lower-level, nonviolent sex crimes or who are judged to be low risks to reoffend be removed from the registry after 10 or 20 years.
The measure is supported by Los Angeles County Dist. Atty. Jackie Lacey because of concern that the registry has become too large, with 105,000 names, and is requiring criminal justice workers to spend a lot of time on paperwork for people who are unlikely to commit new offenses.
“Our current sex offender registration system is broken — it burdens our law enforcement with unnecessary work tracking and monitoring low-level offenders with little to no risk of repeat offense when these officers should be out monitoring high-risk offenders,” Wiener said.
The Assembly Appropriations Committee shelved a previous version of the bill because it would involve “significant ongoing cost in the tens of millions of dollars” for technology costs, according to an analysis by legislative staff.
The new bill will not have to go through the Appropriations Committee. Wiener said it will get a vote of the full Assembly next week.
NRA files another lawsuit challenging California’s assault rifle restrictions
The National Rifle Assn. has filed a second lawsuit challenging California’s assault weapons restrictions, this time alleging that regulations developed by the state Department of Justice are too burdensome and go beyond the agency’s powers.
The NRA had previously filed a lawsuit against a ban on the sale of rifles with bullet buttons that allow detachment of an ammunition magazine, which was approved by the Legislature.
The measure required people who owned guns with bullet buttons before the ban to register them with the state.
The new lawsuit, filed Thursday in Fresno Superior Court, seeks to block the new regulations, arguing that new rules requiring registration of existing assault weapons “go far beyond” the allowed registration process, and “unlawfully expand the scope” of the state’s registration requirement.
The lawsuit says the regulations require excessive personal information as a condition of registration, including where and how the firearm was acquired, and a requirement to provide the state DOJ with photographs of the firearm.
“Individual owners of firearms deemed ‘assault weapons’ under the new law, including plaintiffs, and members and supporters of plaintiff [the California Rifle and Pistol Assn.] are irreparably harmed as a direct result of defendants’ adoption of these illegal regulations,” the lawsuit says.
Proposal for 100% clean energy faces new political challenges as it nears the finish line

With the clock ticking until the end of the legislative session, there’s new and potentially damaging opposition to a high-profile clean energy proposal.
The legislation, SB 100, would phase out fossil fuels for generating electricity by 2045, strengthening California’s already formidable reputation as a leader in the fight against climate change.
Although it received strong support from powerful trade unions when it was announced earlier this year, now electrical workers and utility employees are opposed. Their unions, representing roughly 120,000 workers, issued an alert Thursday asking lawmakers to reject the legislation, authored by Senate President Pro Tem Kevin de León (D-Los Angeles).
Scott Wetch, a lobbyist for the unions, said the legislation is “just not ready for prime time” and should be placed on hold.
The controversy involves broader questions about the future of California’s electricity grid. The Public Utilities Commission has launched a pilot program that could lead to increased reliance on technologies such as energy storage and rooftop solar.
The unions fear those initiatives will result in fewer jobs for their members, as well as a less-reliable, less-regulated electricity grid. They want a provision in SB 100 that would require lawmakers to review the results of the pilot program before it can be expanded by regulators.

Tom Dalzell, business manager for the International Brotherhood of Electrical Workers Local 1245, said de León promised to address the issue in April, before the legislation was officially announced.
“He understood our concerns and said he would protect the distribution system,” Dalzell said.
No such promise was made, said Jonathan Underland, a spokesman for de León. Underland said “a single lobbyist,” meaning Wetch, “is pushing amendments completely unrelated to SB 100 and impugning the pro tem’s integrity to justify his means.”
“He’s entitled to critique a state agency, but he shouldn’t hijack SB 100 to wage that battle,” Underland added.
Environmentalists criticized the unions for launching their opposition near the end of the session, after the measure has cleared nearly every hurdle except for a final vote on the Assembly floor.
Kathryn Phillips of the Sierra Club said attempts to stop the legislation were “irrational” because clean energy initiatives will create new jobs. A coalition of environmental groups said the unions’ proposed amendments would hamper efforts to reduce greenhouse gas emissions.
“These investments in clean resources are critical to California’s carbon-free electricity future,” they wrote in their message to lawmakers.
Bill that would expand the evidence prosecutors can use against sex traffickers in court goes to Gov. Brown

The state Senate on Thursday sent Gov. Jerry Brown a bill that would expand the evidence that prosecutors can bring forth at trial against defendants charged with selling victims for sex.
The legislation, filed by Sen. Toni Atkins (D-San Diego), would allow prosecutors to call on witnesses or provide records that speak to a criminal suspect’s character, in attempts to show to the jury a pattern of abuse toward the victim. Such evidence is prohibited at trial, except in cases involving sexual assault domestic violence, or abuse of a child or an elder.
In a statement, Atkins said the change in the court rule would lead to more convictions of sex predators.
Sex traffickers can be difficult to prosecute, social workers and prosecutors say, as victims are often young and tied to their abusers through complicated psychological and emotional bonds. Often, they refuse to testify out of fear or because they are coerced.
Atkins is among the lawmakers pushing the issue at the Capitol, where legislation has focused on targeting traffickers, protecting victims and addressing what advocates say is a law enforcement culture in which child survivors sometimes are treated like criminals.
Another of her proposals would have required hotels and motels to train their employees to spot signs of human trafficking. But it was shelved in a fiscal committee.
Rep. Duncan Hunter’s chief of staff steps down amid investigation into congressman’s campaign funds
Rep. Duncan Hunter’s chief of staff, Joe Kasper, is leaving the embattled congressman’s office after 15 years on Capitol Hill.
Kasper has been the Alpine Republican’s voice throughout much of the congressional ethics and FBI investigations into whether Hunter misused thousands of dollars in campaign funds for personal expenses.
His name has been officially tied to the investigations just once, in an FBI warrant to search Hunter’s campaign treasurer’s office. The warrant said agents were looking for communication with Kasper, Hunter, Hunter’s wife and others.
Kasper worked for Hunter’s father, former Rep. Duncan Hunter, before joining his son’s office. He started out as communications director and worked his way to chief of staff.
As chief of staff, Kasper spoke to the media on his boss’ behalf and had a hand in legislative issues.
“Few members allow for the responsibility and autonomy that I had — and I’ll be forever grateful to hold Rep. Hunter’s confidence, respect and friendship. I also have to thank Rep. Hunter’s father, who hired me as young upstart on Capitol Hill and gave me all the life-lessons and guidance I needed to set my pace over more than a decade,” he said in a statement announcing his departure.
Kasper said he is headed to a job at the Pentagon, but did not say what role he would have there.
“It was a very difficult decision given my close relationship with Rep. Duncan Hunter and knowing what we’ve accomplished over the years,” he said in the note.
Assembly advances resolution denouncing proposed transgender military service ban
California state senators ask Trump and Congress to remove Confederate names and statues
California congresswoman returns to D.C. with pop of pink hair
It’s just a flash of fuchsia, but it’s not the hair color you expect to see on a member of House leadership. House Democratic Caucus Vice Chairwoman Linda Sanchez returned to Washington after the August recess with a bit of flair back there.
“I’m all about being your authentic self, and as I told the staff who might have had some concerns, it’s business in the front. It’s professional, it’s not mohawked or shaved. It’s pink,” she told The Times. “I think it’s pretty subtle.”
Sanchez (D-Whittier) said she’s wanted to dye her locks pink for a long time. In a way, it’s a rebellion against the drab, staid colors people who work on Capitol Hill often are expected to wear.
“We deal with so much seriousness that every now and again you want to mix it up and do something a little out of the routine,” she said. “I just have never been a pearls and navy-blue suit kind of gal. My style is a little bit influenced by California and definitely Latino love of color.”
DNC chairman blasts Fresno GOP for fundraising with former Sheriff Joe Arpaio

The head of the Democratic National Committee on Thursday blasted Fresno Republicans for inviting controversial former Maricopa County Sheriff Joe Arpaio of Arizona to headline a party fundraiser.
“It is shameful that the Fresno County Republican Party is fundraising off one of the nation’s most notorious agents of racism and bigotry,” said DNC chairman Tom Perez, who oversaw federal prosecution of Arpaio when he led the U.S. Department of Justice’s civil rights division.
Arpaio was convicted in July of criminal contempt for violating a federal court order to stop racially profiling Latinos and had been scheduled to be sentenced on Oct. 5. But in late August, President Trump pardoned Arpaio, who was an early supporter of the candidate during the 2016 presidential campaign.
“President Trump and the Republican Party may not believe justice is blind, but the American people still do and they want to see Arpaio held accountable, not pardoned for his prejudice and paraded around at a fundraiser,” Perez said.
Arpaio is scheduled to be the guest speaker at a “2nd Amendment Barbecue” at a Fresno restaurant on Sept. 29. Tickets cost $70 to $1,500.
“Sheriff Joe is a no-nonsense law and order leader, a veteran and a patriotic American. Although he has been maligned by the left, he still stands strong, and FCRP is excited to welcome him to this event,” reads an invitation for the event.
The controversy over the event is prompting police to prepare for protesters and causing some elected Republicans to stay away, the Fresno Bee reported on Wednesday.
Los Angeles man who was detained by ICE after dropping his daughter off at school is welcomed in the state Senate
Tom Steyer drops by a Riverside union rally, just like three of the top Democrats running for governor

Billionaire environmentalist Tom Steyer ventured to the Inland Empire on Thursday to show his support for a powerful public employee union’s three-day strike against Riverside County — just like three of the top Democratic candidates for governor have done this week.
But Steyer said not to read anything into it.
Speculation abounds about whether the former hedge fund manager from San Francisco, who has spent tens of millions of dollars funding Democratic candidates and liberal causes across the country, may run for governor or perhaps U.S. Senate.
Steyer continues to be coy about any future political plans, saying that he is still considering his options.
Steyer, interviewed by telephone Thursday afternoon, said he joined the rally held by the Service Employees International Union Local 721 in Riverside to show his solidarity for the union’s complaints about hazardous working conditions and in support of the union’s contract negotiations.
He said he made plans to go before he heard that three gubernatorial candidates — Lt. Gov. Gavin Newsom, former Los Angeles Mayor Antonio Villaraigosa and state Treasurer John Chiang — were going to show up.
“I’ve been going to those rallies for years. I didn’t even know they were going to be there,” Steyer said.
Steyer has had strong political ties with the SEIU, a politically powerful public employees union with more than 700,000 members in California. Steyer’s organization, NextGen, joined with SEIU to rally support for the recently passed cap-and-trade bill, as well as efforts in 2016 to help Democratic candidates.
Steyer said the rights of American workers are “under attack” by the Trump administration, as are the rights of immigrants and voting rights for African Americans.
“I went through the Trump budget,” Steyer said. “They are cutting every form of investment in the American people.”
Steyer also offered an opinion about recent criticism of Sen. Dianne Feinstein, who came under attack by some California liberals last week after she called for “patience” when dealing with President Trump. Steyer said his fellow Democrat, California’s senior senator, has a more optimistic view of the potential for bipartisan cooperation than he does.
“I feel as if this is an administration that is trampling on the rights of Americans,” Steyer said. “These are people who are doing things that are absolutely wrong. And there’s no compromise with wrong.”
Steyer described Feinstein as a “great public servant” but sidestepped a question about whether she should run for reelection in 2018.
Rep. Barbara Lee proposes legislation to remove Confederate statues from the U.S. Capitol

On the heels of a clash between white supremacists and counter-protesters in Virginia last month, Rep. Barbara Lee wants statues of Confederate heroes removed from the U.S. Capitol.
The Oakland Democrat filed legislation Thursday that would require that all statues of people who voluntarily served the Confederate States of America be removed from the Capitol’s Statuary Hall. Sen. Cory Booker (D-N.J.) filed similar legislation in the Senate, which is co-sponsored by California’s Democratic Sen. Kamala Harris.
Furor over the removal of Confederate statues from public spaces grew after a protest about a statue of Confederate Gen. Robert E. Lee in Charlottesville, Va., became violent.
Each state is allowed to place two statues of state figures in the United States’ National Statuary Hall Collection, and about 10 statues from Southern states depict men who were Confederate soldiers or generals.
Under Lee and Booker’s legislation, states could reclaim the statues if they pay the shipping costs and are welcome to send a replacement.
“Having these monuments in Statuary Hall really doesn’t tell the story of my ancestors, of men who wanted to keep my ancestors in chains. The story needs to be told,” she said.
Lee said she hopes the statues would be placed in museums, where they can be contextualized.
“They don’t belong in public spaces where we honor and celebrate men who wanted to keep slavery in existence,” she said.
Shortly after the Charlottesville melee in which a woman was killed, Minority Leader Nancy Pelosi (D-San Francisco) urged House Speaker Paul D. Ryan to remove the statues.
A spokesman for Ryan told Politico last month that GOP leadership thinks the states should make the decision to remove a statue, an indication that the legislation faces an uphill battle in Congress.
Starting in 2000, some states, including California, have chosen to remove their statues, frequently in order to replace them with more contemporary or well-known figures.
California’s current statues are of President Ronald Reagan and Franciscan missionary Junípero Serra.
California lawmakers propose allowing marijuana growers and sellers to work alongside each other
With the first marijuana licenses due to be issued in January, California lawmakers proposed Thursday that growers and sellers be able to group multiple permitted operations together.
The change would allow a store that is licensed to sell marijuana for medical use to also sell pot for recreational use if it is licensed to do so. In addition, a marijuana store would be able to run a manufacturing operation at the same site, and businesses could group together multiple cultivation licenses in one facility, which would allow medical pot to be grown next to adult-use cannabis, said Hezekiah Allen, head of the California Growers Assn.
The measure also would repeal a rule that licensed medical-cannabis manufacturers can provide products only to medical pot retailers.
Lawmakers said the changes, which are contained in a bill by the Assembly Budget Committee that addresses inconsistencies and confusion created by past cannabis measures, will provide flexibility for license holders and convenience for customers.
While Allen supports allowing medical and recreational marijuana sales at the same location, he said his group is “concerned about the potential for ‘licensing clustering’ to be a way around limits on cultivation licensing.”
The measure also would repeal a rule that all customers at a recreational-cannabis retailer be 21 or older, allowing 18-year-olds at stores that provide medical marijuana.
California Senate leader Kevin de León proudly displays his ‘legislative unicorn’

Senate President Pro Tem Kevin de León (D-Los Angeles) called state officials’ major deal to extend California’s cap-and-trade program to fight climate change a “legislative unicorn” because diverse interests supported it. On Thursday, he brought a gift he received afterward to the Senate chambers, and explained why.

Senate President Pro Tem Kevin de León (D-Los Angeles) describes why he has a ”legislative unicorn”
Bill to shed more light on prescription drug go-betweens is shelved for the year
An effort to shed more light on a little-scrutinized part of the prescription drug supply chain — pharmacy benefit managers — sputtered on Thursday after facing concerns from the Brown administration.
Pharmacy benefit managers, or PBMs, such as Express Scripts or CVS Caremark, act as go-betweens connecting drug makers and purchasers, such as health plans and consumers. By negotiating in bulk with manufacturers, PBMs claim they can secure steep discounts, which can be passed on to purchasers.
But drug makers and consumers alike have said there is little assurance that such savings actually reach consumers. As concerns continue to mount about high prescription prices, PBMs have increasingly been scrutinized.
Assemblyman Jim Wood (D-Healdsburg) proposed a measure that would have required pharmacy benefit managers to register with the state and disclose upon the purchaser’s request information about their dealings with manufacturers, such as drug acquisition costs and the amount they’ve received in rebates and administrative fees.
PBMs were opposed to the measure, calling it a costly mandate.
Gov. Jerry Brown’s administration had a different concern. According to Wood, Brown’s office wanted the disclosures mandated by the bill to be made to the state, not the purchasers.
“We have agreed to continue discussions in the next few months to reach final agreement on how best to achieve the transparency we believe is so important to purchasers so they can have a complete picture of what contributes to escalating pharmaceutical drug costs,” Wood said in a statement. “Once this is resolved, we will move the bill next year.”
Bill blocking public release of police body camera footage depicting rape victims passes Legislature

A bill that would block the public release of police body camera footage or other videos that depict victims of rape, incest, sexual assault, domestic violence or child abuse is headed to Gov. Jerry Brown’s desk.
The measure, AB 459 from Assemblyman Ed Chau (D-Arcadia), overwhelmingly passed the Assembly on Thursday with no debate.
Generally, police departments across California don’t release body camera footage outside of a courtroom. State lawmakers have struggled to pass broader legislation governing transparency of the footage. A bill that would have dramatically expanded public access to the videos was shelved earlier this week.
California lawmakers vote to slim down bulky statewide ballot guides

California lawmakers voted Thursday to allow elections officials to print only summaries of ballot measures in statewide voter guides, concluding that the bulky paper documents could easily be replaced with more information posted online.
“The book is so burdensome,” said state Sen. Bob Hertzberg (D-Van Nuys) during debate on the floor of the Senate.
Assembly Bill 606, which now awaits the signature of Gov. Jerry Brown, requires the secretary of state to make clear in future voter guides the Internet address where voters can find the full text of ballot measures. Voters would also be given the option of calling a toll-free number to request a full guide of the legal language.
The bill comes on the heels of the state’s largest-ever voter information guide in 2016, a 224-page document that included details on candidates for office and the 17 propositions on the Nov. 8 ballot.
Critics during Thursday’s floor debate voiced concerns about the accuracy of the new summaries, or the fact that many voters wait until the last minute to review ballot propositions and therefore wouldn’t receive one in the mail before election day.
“For some it works, for many others, it would not,” said state Sen. Steve Glazer (D-Orinda).
Lineup at California GOP convention takes a hard right with Tom Cotton, Grover Norquist, Judge Jeanine Pirro

Arkansas Sen. Tom Cotton, an up-and-comer in the GOP and — at 40 — the youngest member of the Senate, will highlight the conservative lineup of speakers at the California Republican Party’s convention in Anaheim in October.
Cotton, who served as an Army officer in Iraq and Afghanistan, was a harsh critic of President Obama and is considered a hawk on national defense. During a hearing in June, Cotton openly mocked the idea that the Trump administration may have colluded with Russia to influence the 2016 election.
“As we gather to focus on electing Republicans in a blue state, these speakers will remind us that Republican values are California values — entrepreneurship, belief in a better future for our state and our country, and freedom,” California Republican Party Chairman Jim Brulte said in a statement Thursday.
The other speakers scheduled to appear include: House Majority Leader Kevin McCarthy (R-Bakersfield); anti-tax crusader Grover Norquist; Fox News star Judge Jeanine Pirro and conservative economist Stephen Moore of the Heritage Foundation.
By tapping the conservative crew of speakers, the California GOP will try to energize the Republican faithful as the party tries to claw its way back to political relevance in left-leaning California.
Near the top of the state party’s agenda is dismantling the Democratic supermajorities in the Assembly and state Senate.
But the GOP has a lot of work to do. Democrats hold nearly a 19-percentage-point advantage in voter registration in California and, thus far, no big-name Republicans have entered the 2018 races for governor or U.S. Senate.
The chief of staff who has served Nancy Pelosi for a decade plans to leave this month
Longtime staffer Nadeam Elshami will step down as House Minority Leader Nancy Pelosi’s chief of staff later this month, raising fresh questions about how long Pelosi intends to remain in office.
San Francisco’s Pelosi has said that she planned to retire if Hillary Clinton had won the presidency last November, but she has appeared reinvigorated by her role as foil to President Trump.
While the departure of an influential aide always raises eyebrows about a politician’s future, it doesn’t necessarily mean Pelosi has made new plans about her retirement.
No reason was given for Elshami’s departure, and his own plans aren’t clear. He’s been Pelosi’s shadow for a third of her three-decade tenure on Capitol Hill.
“Nadeam’s deep insight and effectiveness has been a vital part of our Caucus’ unity throughout his time as Chief of Staff, especially during critical battles to protect the Affordable Care Act, Wall Street Reform and other landmark progress for working families,” the Democrat said in a statement.
Elshami joined Pelosi’s office in 2007 and became her chief of staff four years ago after leading her press team. He previously worked for Assistant Senate Democratic Leader Richard Durbin (D-Ill.), Sen. Barbara Boxer (D-Calif.) and Rep. Jan Schakowsky (D-Ill.), having risen through the ranks on Capitol Hill since starting in a Senate newsroom 25 years ago.
His replacement will be Daniel Weiss, who served 21 years as chief of staff for former California Rep. George Miller (D-Martinez).
Weiss is vice president for federal policy and director of the Washington, D.C., office for Common Sense Media. He worked in various positions from 1988 to 2015 while Miller was a member of the House Democratic leadership and a Pelosi confidant.
FOR THE RECORD
11:04 a.m.: A previous headline incorrectly indicated Elshami worked for Pelosi for multiple decades. He has worked for her for a decade.
Facebook, real estate developer want California lawmakers’ help for their big projects
Major developers are asking the Legislature for last-minute help in getting their projects built.
Facebook and a New York-based developer, Millennium Partners, are supporting new legislation that would give a boost to their proposed large, mixed-use projects in the Bay Area and Los Angeles, respectively.
They want relief under the California Environmental Quality Act, or CEQA, the state’s primary environmental law governing development. Under the new measure, Senate Bill 699, any CEQA lawsuit against their projects would face a nine-month deadline to be completed — potentially sparing the developers years of litigation.
Facebook wants to expand its Menlo Park headquarters to include housing, grocery and retail development. Millennium Partners has been planning to build two skyscrapers in Hollywood.
A separate last-minute bill, SB 789, would provide major relief under CEQA to benefit the 2028 Olympic Games in Los Angeles and a new arena for the Los Angeles Clippers in Inglewood.
Immigrant-rights advocates rally outside the governor’s mansion as push for ‘sanctuary state’ bill continues
Former congressman Mike Honda will work to unseat Republican incumbents in California

Former congressman Mike Honda, who lost a bitter election last year to a fellow Democrat, will helm a political group looking to win more Democratic seats in California.
Red to Blue California, a political action committee formed in March, announced Thursday that Honda will serve as its chairman, taking on an unpaid advisory role in its effort to unseat Republican incumbents in 2018.
“In all my years of public service, I cannot think of a more critical time for us to stand up and fight for the values of equality, tolerance and justice that we hold dear. Taking back Congress starts right here in California,” Honda said in a statement.
The group was formed by Michael Eggman, who lost to Rep. Jeff Denham (R-Turlock) by three percentage points last year. With the addition of Honda, Eggman will become president of the group, which aims to raise $7 million to spend in seven California GOP districts next year.
As of June 30, Red to Blue California had reported raising about $37,000 with major contributions from Palo Alto philanthropist Eva Grove and Stanford professor Martin Hellman. Spokesman Andrew Feldman said the group collected “six figures” in July and August, much of it from small donors.
Honda was defeated in 2016 by repeat challenger Ro Khanna, who capitalized on Honda’s ongoing ethics investigation and argued that voters in the Silicon Valley district needed a change in leadership.
Khanna was the first member of Congress to join a group that has promised to challenge fellow incumbent Democrats, saying competitive primaries would “strengthen the Democratic Party.”
Rumored future candidate and California investor Joe Sanberg unveils digital ad touting work fighting poverty
Joe Sanberg, a wealthy Westwood investor who pushed the state to create income tax credits for the working poor, will launch a statewide digital ad buy on Thursday about the program and plans to form a federal political action committee to support candidates who support his goals.
In the ad, Sanberg describes the workers who benefit from the state’s recently expanded earned income tax credit over images of a janitor, a dishwasher, a home healthcare aide and a gardener.
“They say not all heroes wear capes. In California, they wear hairnets, uniforms and gloves,” Sanberg says. “Now, thanks to our governor and Legislature, over a million California heroes are eligible for the earned income tax credit, including for the first time the self-employed. In our nonprofit, we’ve committed to helping them get tax credits they’ve earned. Join our fight for financial security. Capes optional.”
Sanberg, 38, is an Orange County native who is rumored to be considering a run for elected office. His profile has risen in the state Democratic Party for his work to fight poverty.
In addition to championing efforts to create and expand the state earned income tax credit, he founded a nonprofit that provides guidance to families who qualify for the credit.
The 30-second digital ad, which may eventually run on television, is reminiscent of an introductory message designed to introduce a potential candidate to Californians who are unfamiliar with his or her work.
Republicans trounce Democrats in California’s annual legislative softball game
Republicans and Democrats took a break from end-of-session negotiations on Wednesday night for California’s annual legislative softball game.
After losing two years in a row, Republicans won 14 to 6. The game raised $71,500 for the Children’s Receiving Home of Sacramento, a local nonprofit.
One notable Republican wasn’t on the field — state Sen. Anthony Cannella of Ceres, the only member of his party to vote for a gas tax increase this year.
It was the second legislative sports event of the year. Democrats and Republicans played soccer last month, with the Democrats coming out on top.
California will file separate lawsuit over end of DACA program, attorney general says

California plans its own lawsuit against the federal government because it is disproportionately harmed by President Trump’s plan to end the Deferred Action for Childhood Arrivals program, Atty. Gen. Xavier Becerra said Wednesday.
Becerra outlined his plans after 15 other states, including New York and Washington, filed their own lawsuit Wednesday challenging the end of the DACA program, which protects children who were brought into the country illegally from deportation.
With a quarter of the 800,000 DACA participants coming from California, the state and its economy will be hurt more than other states, Becerra said,
“I think everyone recognizes the scope and breadth of the Trump decision to terminate DACA hits hardest here,” Becerra said in an interview.
The federal lawsuit will be filed in California, he said.
“California will sue the Trump Administration over its termination of the DACA program for one simple reason,” Becerra said. “Our state has become the world’s sixth-largest economy due in part to the success of over 200,000 Dreamers whose livelihoods have been put at risk by President Trump’s wrong-headed decision on DACA.”
Updated 5:35 pm to include state in which lawsuit would be filed and additional comment.
State Senate bill to ease fees on families with children inside the juvenile justice system heads to Gov. Brown
California would cover over-budget costs for 2028 Olympics bid under new bill

State lawmakers will provide up to $270 million in guarantees under legislation unveiled last week should Los Angeles’ 2028 Olympic bid go over budget.
The measure, AB 132, aims to fulfill a promise from Assembly Speaker Anthony Rendon (D-Paramount) and Senate President Pro Tem Kevin de León (D-Los Angeles) to give state support for the Olympic bid.
Cost concerns were the major worry when the Los Angeles City Council approved the 2028 bid last month. The 2028 Summer Games are expected to have a $5.3-billion price tag, and organizers believe corporate sponsorships, ticket sales and other revenue sources could cover expenses.
But city officials and bid organizers had asked the state to step in if the Games have a budget shortfall. Last year, state lawmakers overwhelmingly approved a similar measure, but it covered only a potential 2024 Olympic bid, so new legislation was needed. Los Angeles agreed to host the 2028 Games as part of a deal that awarded the 2024 Games to Paris.
Under AB 132, the state’s financial guarantee is $20 million more than promised in last year’s legislation, an increase that accounts for inflation, said Jeff Millman, a spokesman for the bid committee, LA 28.
“This is an LA 28 priority, and we welcome the Legislature’s consideration during this session,” Millman said.
Lawmakers will have to work quickly to pass the measure this year. The deadline for bills to pass both houses of the Legislature is Sept. 15.
Schwarzenegger joins McCain, Kasich in calling for Supreme Court to end gerrymandering

Former California Gov. Arnold Schwarzenegger is among about three dozen prominent Republicans who filed friend-of-the-court briefs in a closely watched gerrymandering lawsuit that is scheduled to be heard before the U.S. Supreme Court next month.
Breaking ranks with GOP leadership, Schwarzenegger joined with Ohio Gov. John Kasich, Arizona Sen. John McCain, former Kansas Sen. Bob Dole and other present and former elected officials on Tuesday to argue that redistricting — the drawing of legislative and congressional district lines — in a way that favors any political party is unconstitutional.
Schwarzenegger attributes gridlock in the nation’s capital to redistricting that results in many politicians being drawn into “safe” districts, which he argues discourages collaboration and encourages extreme partisanship.
“No matter what happens, we don’t solve the problem. But at the same time, 98% of the congressional guys are getting reelected. It just shows you how fixed the system is,” he told reporters during a conference call on Wednesday.
Schwarzenegger said both parties are guilty of trying to redraw district lines in ways that help their chances, but that such efforts create a lack of competitiveness. He drew an analogy with his days as a bodybuilder.
“It was very clear I didn’t lift as much, and I didn’t do as well as when there was competition and fear. And the more competition there was, the more I lifted, the more I performed,” he said. “This is just the same thing, but in politics.”
Redrawing of legislative and congressional lines occurs at least once a decade to accommodate changes in population. States are responsible for redrawing the lines, and the political party in power is often seen as heavily influencing the outcome. In a handful of states, including California, the lines are redrawn by independent bodies.
The case the Republican politicians are weighing in on involves the 2011 redrawing of state Assembly district lines in Wisconsin. A group of Democratic voters argued that the new districts were drawn so unfairly that they violated their constitutional rights. A federal judicial panel agreed in November, leading the state to appeal and the upcoming Supreme Court hearing.
Schwarzenegger first became interested in gerrymandering when he was governor. In 2008, he championed a successful ballot measure that created an independent commission to draw legislative district boundaries. Voters approved another ballot measure two years later that expanded the commission’s purview to include congressional districts.
Addressing gerrymandering has been one of Schwarzenegger’s priorities since he left Sacramento, in addition to fighting climate change, restarting his movie career and occasionally trolling President Trump.
Schwarzenegger has used his celebrity to garner attention for what is a relatively obscure subject, including creating biting videos that have gone viral. He is also crowd-sourcing money to help pay the legal bills for the plaintiffs in the Wisconsin case and has pledged to match every dollar raised — so far more than $100,000.
Lobbying for California bill to crack down on prescription drug prices intensifies
Backers of a measure to require pharmaceutical companies to disclose more information on the list prices of their drugs are stepping up their lobbying efforts in the closing days of the California legislative session.
Labor unions, consumer groups, health plans and other high-profile advocacy organizations such as the AARP and NextGen, which is bankrolled by billionaire activist Tom Steyer, made the rounds at the state Capitol on Wednesday to urge Assembly members to back the bill, SB 17, by state Sen. Ed Hernandez (D-West Covina).
Similar measures have faltered in the past, but Hernandez said this year, business-friendly Democrats and some Republicans have signaled an interest in supporting the bill.
“The dynamics and the politics of this have changed dramatically,” he said at a news conference Wednesday.
Drug manufacturers have mounted vigorous opposition to the measure, arguing it focuses on drugs’ sticker prices, which rarely reflect what consumers pay for medication.
“It may be inconvenient for SB 17 supporters to admit, but this bill focuses on a false marker for prescription drug costs by only collecting information on the list price, and not actual spending after all negotiations, discounts and rebates,” said Priscilla VanderVeer, spokeswoman for the Pharmaceutical Research and Manufacturers of America.
Hernandez, meanwhile, is capitalizing on the prescription drug debate as he mounts a 2018 bid for lieutenant governor. His campaign released a digital ad touting the senator as a foe to “big pharma.”
After ‘a dark day,’ immigrant rights advocates rally in Sacramento to fight for workplace protections from ICE raids

Immigrant rights advocates shared stories Wednesday of workers left in the lurch after President Trump’s decision to rescind a program that offered temporary immigration relief for thousands of people brought into the country illegally as children.
But members of the Service Employees International Union and allied employers vowed to continue their fight to protect immigrant workers without legal residency.
Dozens gathered in Sacramento in support of a state bill that would prohibit employers from allowing federal immigration officials to enter non-public areas of a work site without a warrant. The bill also would require employers to notify their workers when officials intend to review employee eligibility forms or other records.
Assemblyman David Chiu (D-San Francisco), who introduced the legislation, said it had gained new urgency after “a dark day” in which U.S. Atty. Gen. Jeff Sessions announced the cancellation of the Deferred Action for Childhood Arrivals program, or DACA.
Chiu said about 97% of DACA recipients are students or workers, statistics reflected in a recent survey by the Center for American Progress. One in 10 California workers who pick crops, prepare meals or care for children and elders do not have legal immigration status, according to SEIU.
AB 450 has gained the support of more than 20 labor groups and employer associations. But it is facing heavy opposition from more than 50 business associations and agriculture groups across California that argue it requires employers to fully understand federal law, and puts employers in a bind.
“We wouldn’t be here talking about this bill, AB 450, if Donald Trump had not declared war on workers, if he had not declared on immigrants,” Chiu said, adding that the president “has threatened to hire 10,000 new ICE agents to fan across America, into California, into workplaces to deport our family members and critical workers to our economy.”
Fresno Rep. Jim Costa to miss votes because of knee replacement
Gov. Jerry Brown urges cooperation on trade and climate at Russian conference
California’s congressional delegation backs aid for Hurricane Harvey victims

Nearly all 53 of California’s U.S. House representatives voted Wednesday to provide $7.85 billion in assistance to the victims of Hurricane Harvey.
The vote was the first step in securing the expected aid needed for those affected by the hurricane. Recovery efforts could cost more than $120 billion, and Texas Gov. Greg Abbott has said President Trump told him the funds are just a down payment.
Three Republicans — Justin Amash of Michigan, Andy Biggs of Arizona and Thomas Massie of Kentucky — voted no on the aid package.
California Republican Rep. Darrell Issa of Vista and Democratic Rep. Jim Costa of Fresno did not vote. Costa’s staff said he will miss votes this week while he recovers from a knee replacement. A representative for Issa was not immediately available for comment.
Many Republicans, including eight in the California delegation, voted against a $50.5-billion relief package in 2013 following Hurricane Sandy, which devastated the Northeast, and demanded offsetting budget savings to provide aid to the area represented largely by Democrats. Several of those who voted no said the bill included too much spending unrelated to the storm.
Democrats were closely watching how Republicans would vote for Harvey aid. Several of the Republicans who voted against Sandy assistance are in tough reelection fights in 2018.
Why a trio of Democratic candidates for governor are dropping by a public union strike in Riverside
A powerful public employee union’s three-day strike against Riverside County to protest working conditions will draw three of California’s top Democratic candidates for governor on Wednesday.
Lt. Gov. Gavin Newsom, former Los Angeles Mayor Antonio Villaraigosa and state Treasurer John Chiang all plan to drop by to offer their support for Service Employees International Union Local 721, a clear nod to just how much political muscle public employee unions have in California.
The SEIU represents more than 700,000 government workers and its state council alone spent more than $14 million during the 2016 election, and that doesn’t include separate political spending by local chapters. (The SEIU Local 721’s political committees, for example, dished out more than $1.5 million in 2016.)
The union is in the midst of contract negotiations with Riverside County, and called for the strike in response to “bad faith” bargaining by the county, including over health and safety provisions, according to the union website.
A Riverside County spokesman disputed the union’s assertion, saying the county has negotiated in good faith.
“It is common for labor groups to criticize public agencies in order to apply pressure during negotiations,” said spokesman Ray Smith. “In Riverside County, labor groups know they can portray the status of negotiations however they choose, because the county respects the privacy of the process and will not comment about it.”
Newsom, Villaraigosa and Chiang are stopping by the protest at different times. They rally is being held outside the Riverside University Hospital in Moreno Valley.
Essie Justice Group targets the heavy and invisible burden that California’s bail system places on women
As a public defender in New York City, Gina Clayton realized the U.S. bail system was putting a heavy and invisible burden on women. Now, she is the founder of the Essie Justice Group, a support network for women with incarcerated loved ones that this year has been one of the main drivers behind legislation to overhaul the way offenders receive bail in California.
The group, with cohorts in Los Angeles and the Bay Area, offers spaces for women to share experiences they often don’t talk about at home. In healing and building bonds, Clayton says, their mission is to launch female leaders who can lobby their district representatives, organize their own events and speak at public forums against a punitive criminal justice system that disproportionately affects black and Latino communities.
L.A. Olympics organizers to state senator: Please take us out of your bill

The organizing committee for Los Angeles’ bid to host the 2028 Olympic Games wants the summertime sports event removed from last-minute state legislation that would ease its ability to build transit projects.
On Friday, state Sen. Steven Bradford (D-Gardena) unveiled a bill that would exempt any bus, rail or other transit project related to Los Angeles’ 2028 event from the California Environmental Quality Act, or CEQA, the state’s primary law governing development. The law requires developers to disclose and reduce a project’s environmental impact — a process that often is costly, time-consuming and fraught with litigation.
But in a letter sent to Bradford on Friday, LA 2028 CEO Gene Sykes said the measure wasn’t needed.
“While we appreciate any efforts to support the Games, as the LA 2028 plan does not require building any new transit infrastructure, a CEQA exemption is unnecessary and we request that references to the Olympics be removed from the legislation as amended,” Sykes wrote.
It’s unclear what coordination Bradford’s office had with Olympic organizers prior to introducing the bill. Both a spokesman for Los Angeles Mayor Eric Garcetti and an executive with the Metropolitan Transit Authority have told the Los Angeles Times that they didn’t request the legislation.
The bill also includes major relief under CEQA for a proposed NBA arena for the Los Angeles Clippers in Inglewood.
Bradford’s office didn’t immediately respond to a request for comment on the LA 2028 letter.
California lawmakers move to preserve climate change data

The California Assembly advanced legislation Tuesday that seeks to protect climate science and scientists from President Trump’s administration.
The measure, Senate Bill 51, was approved 51 to 12. It must return to the state Senate for another vote before heading to Gov. Jerry Brown’s desk.
Authored by state Sen. Hannah-Beth Jackson (D-Santa Barbara), the bill would ask the California Environmental Protection Agency to preserve any scientific information “at risk of censorship or destruction by the federal government.”
The legislation would also prevent state regulators from suspending professional licenses for federal employees who might face disciplinary action for publicly disclosing scientific or environmental information.
Senate Bill 51 is one piece of a package of measures intended to strengthen California’s environmental protections despite rollbacks in national regulations under Trump.
California lawmakers act to name stretch of 134 Freeway in honor of former President Obama
State lawmakers Tuesday gave final approval to designating a section of the 134 Freeway as the President Barack H. Obama Highway in honor of the 44th president of the United States.
Supporters of the measure will now raise the private funds needed to place signs with Obama’s name along the section of the 134 between the 210 Freeway and the 2 Freeway, which includes parts of Glendale, Pasadena and Eagle Rock.
Obama, who left office in January, attended Occidental College in Eagle Rock in 1979 before transferring to Columbia University in 1981.
State Sen. Anthony Portantino (D-La Cañada Flintridge) said he decided to seek renaming the stretch of the Ventura Freeway after learning Obama lived in Pasadena as a student and used the freeway to commute to class at Occidental.
Portantino made a veiled reference in his comments on the floor to President Trump’s decision that day to end a program that protects young immigrants from deportation.
“It is particularly proud to stand today to recognize [Obama’s] compassion and heart and dignity on a day when we sorely need compassion, heart and dignity expressed,” Portantino told his colleagues.
In an interview, the senator said the renaming makes sense because “President Obama has a strong and productive connection to Southern California, and particularly to this stretch of freeway.”
The Senate vote was 38 to 0 with most Republicans in support (two did not vote). In the Assembly, Republicans either voted against granting the honor or withheld their vote.
Assemblyman Matthew Harper (R-Huntington Beach) voted against the measure, saying the naming is premature and will confuse motorists given that Los Angeles is renaming a stretch of Rodeo Road in southwest L.A. as Obama Boulevard.
He noted that a section of the 90 Freeway was named after President Nixon until he ended up resigning after the Watergate scandal.
“With Obama being so young, it’s kind of undetermined what his overall legacy will be and how history will judge him,” Harper said. He called Obama’s link to Los Angeles County tangential, adding, “He didn’t even graduate from a California university.”
Caltrans will now do a cost estimate for the signage. The cost of signs for naming other stretches of freeways in honor of public figures has ranged from $3,000 to $7,000.
The late President Reagan was honored with his name on signs on a freeway east of Simi Valley.
6:55 p.m.: This article was updated with the final Senate vote tally.
4:40 p.m. This article was updated to include the possible cost of the action.
This article was originally published at 4:24 p.m.
Sen. Dianne Feinstein says she agrees DACA is ‘on shaky legal ground’ as she calls on Congress to act
Sen. Dianne Feinstein (D-Calif.) signaled Tuesday that she believes former President Obama’s executive order to protect young immigrants who were brought into the U.S. as minors was on shaky legal ground, and said that is why Congress must act to save it.
Feinstein’s remarks are likely to fuel criticism among the most liberal members of her party, some of whom have said that she has grown out of touch with her constituents as she ponders whether to seek a sixth term next year.
Joe Arpaio to headline Fresno Republican Party fundraiser

Joe Arpaio is coming to Fresno.
The recently pardoned former Maricopa County sheriff is scheduled to be the guest speaker at the Fresno County Republican Party’s late September fundraiser.
Billed as an annual “2nd Amendment Barbecue,” the Sept. 29 event has a wide range of ticket prices. A single seat costs $70, and $1,500 gets you a table of 10, “VIP Gold” status and a photo with the former sheriff at a more exclusive reception.
The Fresno Bee reported Arpaio was invited before President Trump issued the pardon. Several people have written letters to the editor to protest the event.
Arpaio was convicted in July of criminal contempt for violating a federal court order to stop racially profiling Latinos in Arizona. He was scheduled to be sentenced on Oct. 5 and faced a maximum of six months in jail. Trump pardoned him in August.
Previous Fresno GOP barbecues have honored military and law enforcement officials in the news. Last year’s theme was “Blue Lives Matter.”
“Sheriff Joe is a no-nonsense law and order leader, a veteran and a patriotic American. Although he has been maligned by the left, he still stands strong, and FCRP is excited to welcome him to this event,” reads an invitation for the event.
L.A.’s 2028 Olympic bid could get a big boost under new California legislation

Los Angeles’ 2028 Olympic bid could get a huge boost under new state legislation unveiled Friday.
Under the bill, any bus, train or other mass transit project connected to the Olympic bid wouldn’t have to follow the state’s primary law governing development, saving lots of time, money and eliminating some litigation risk.
The legislation, Senate Bill 789, also would provide major relief under the California Environmental Quality Act to a proposed NBA arena for the Los Angeles Clippers in Inglewood.
But the bill would cut through longstanding regulations that environmentalists and community activists in California have held as sacrosanct to preserving the state’s natural beauty and involving residents in the development process. And Mayor Eric Garcetti has said the city didn’t ask for the legislation and doesn’t need it for the Olympic bid to be successful.
California police body camera transparency bill is shelved for the year

A bill that would have opened public access to police body camera videos across California has been shelved.
The measure, Assembly Bill 748, would have made public footage from police shootings and other cases considered to be in the public interest, including video of police uses of force or violent political protests.
The bill, authored by Assemblyman Phil Ting (D-San Francisco), squeaked through the Senate Public Safety Committee in July, but no further hearings were held.
The measure’s demise is another example of state lawmakers’ inability to agree on how accessible to the public police body camera footage should be despite a dramatic increase in the use of the equipment among California police departments.
“The patchwork releases of body camera footage only sow further public distrust with law enforcement and the communities they serve,” Ting said in a statement. “California needs a statewide standard for the disclosure of footage. In order to let the footage speak for itself, we need more time to find the breakthrough in this bill and I will continue to engage with stakeholders to find a transparent and equitable solution.”
Sept. 5, 1:52 p.m., This post was updated with a statement from Assemblyman Phil Ting (D-San Francisco).
California lawmakers are vowing to step in and help ‘Dreamers’ after Trump moves to cancel DACA

President Trump’s decision to abandon existing protections for young men and women in the United States without legal status will likely draw a sharp rebuke from Gov. Jerry Brown and an assortment of California elected officials, all of whom have vowed to take extraordinary measures to keep those immigrants from being deported.
DACA decision could be a key issue in districts represented by vulnerable California Republicans

Now that President Trump is putting what should happen to the “Dreamers” on Congress’ agenda, vulnerable Republicans will be squarely at the center of the debate.
The Trump administration’s announcement Tuesday about the Deferred Action for Childhood Arrivals program could have a broad effect on Democratic efforts to retake control of the House in 2018, and nowhere more so than in California, where more than a fourth of the estimated 800,000 recipients, often called Dreamers, are thought to live.
To secure the 24 seats they need, Democrats are specifically targeting nine of the Golden State’s 14 Republican members of Congress, several of whom represent districts with large minority populations. Stories of the 200,000 or so Californians affected by this decision likely will be a recurring theme of campaigns for the next year.
Nearly all of the targeted Republicans have opposed DACA, which delayed deportation for hundreds of thousands of Californians in the country illegally. Just two of the GOP lawmakers with districts that could flip in the midterms have publicly tried to persuade the president to leave DACA in place.
Follow our live coverage of the DACA decision and reaction

The Times has live updates about the Trump administration’s decision to seek a congressional fix to the Deferred Action for Childhood Arrivals program.
An unusual (prehistoric) lobbying campaign
California Politics Podcast: A week of suspense over the fate of bills and the 2018 Senate race
The long Labor Day holiday arrives with significant buzz about how the week ended in Sacramento and what might happen on the campaign trail in 2018.
This week’s California Politics Podcast takes a look at some of the most notable pieces of legislation quietly killed on Friday by lawmakers. We also check in on the closely watched proposals aimed at easing the state’s housing crisis, where supporters are still scrambling to line up votes in the Legislature.
And we discuss the widespread attention Sen. Dianne Feinstein received this week about President Trump — a moderated tone that drew a rebuke from a prominent Democrat and ignited debate about the 2018 race for the U.S. Senate.
I’m joined by Times staff writer Liam Dillon and Marisa Lagos of KQED News.
Gov. Jerry Brown signs bill to extend protections for immigrant witnesses in California
Proposed California ballot initiative would give consumers more control over their personal information online

A ballot initiative proposed Friday would allow California consumers to know what personal information businesses are collecting from them, what they do with it — and to who they are selling it.
Backers of the initiative, dubbed the California Consumer Privacy Act of 2018, are aiming for a spot on the November 2018 statewide ballot. The measure would establish a consumer’s right to request that a business disclose what categories of personal data it gathers, and to say no to the sale of any of that information without fear of losing services or facing discrimination.
It would require businesses to make those disclosures free of charge within 30 days.
Robin Swanson, a general consultant for the measure, says it would “give Californians more control over what personal information is shared.”
The proposed ballot initiative, led by Mary Ross, president of Californians for Consumer Privacy, comes several months after President Trump signed into law a repeal of privacy regulations limiting what broadband providers can do with customer data.
Assemblyman Ed Chau (D-Monterey Park) has been attempting to revive those rules for Californians through pending legislation. His bill would require Internet service providers, such as Verizon, Comcast and AT&T, to get permission from customers before using, selling or permitting access to data about their browsing history.
But the ballot initiative goes further, and would apply to all businesses that collect and deal data for commercial purposes.
Former U.S. Atty. Gen. Eric Holder files brief on behalf of California Senate in Chicago’s ‘sanctuary city’ lawsuit
The California Senate is throwing its support behind Chicago in a lawsuit against the Justice Department over its plan to withhold federal money from “sanctuary cities,” which limit collaboration between state and local authorities with federal immigration agents.
Former U.S. Atty. Gen. Eric H. Holder Jr. and his firm, Covington & Burling, on Thursday filed a friend-of the-court brief on behalf of the state Senate in the federal case, saying sanctuary jurisdictions have policies consistent with federal law.
U.S. Atty. Gen. Jeff Sessions, Holder says, does not have the constitutional authority to mandate that cities, counties or states participate in federal immigration efforts as a condition to receive their federal public safety awards.
The lawsuit, filed last month by Chicago Mayor Rahm Emanuel and city officials, asks a judge to block the Trump administration from enforcing three new conditions it included in petitions for Edward Byrne Memorial Justice Assistance Grant money. The city uses the grant to buy police cars and other equipment, and to fund an anti-violence program.
Holder, who was said to have filed the brief pro-bono, was temporarily hired by the Senate and Assembly to serve as outside counsel to offer advice on the state’s legal strategy against the incoming administration. On Friday, a Covington & Burling spokeswoman said the firm remains “engaged with the California Senate on an ongoing basis.”
In the brief, Holder said the California Legislature has a particular interest in the Chicago case as it weighs Senate Bill 54, which seeks to limit state and local law enforcement agencies from using resources to question, detain and provide information on immigrants illegally in the country.
Covington & Burling analyzed the legislation this year and concluded that “states have the power over the health and safety of their residents and allocation of state resources.”
California Republicans ask House Speaker to consider bill to help ‘Dreamers’ as nation awaits Trump DACA decision

Central Valley Reps. David Valadao of Hanford and Jeff Denham of Turlock are asking House Speaker Paul Ryan to allow the House to consider legislation to protect from deportation the hundreds of thousands of people brought to the country illegally as children.
Many of these so-called Dreamers came forward and underwent background checks, handed over personal data and even their fingerprints after President Obama created the Deferred Action for Childhood Arrivals program in 2012. In exchange they got assurances they wouldn’t be deported for two years if they follow the law and are working, enrolled in school or serving in the military.
More than a quarter of the estimated 800,000 recipients are thought to live in California. Valadao and Denham were among 10 House Republicans who signed a letter to Ryan, stressing that Congress must find a solution.
“We did not support the way that President Obama established this program and usurped Congressional law making authority. However, these individuals have come forward and provided the federal government with their personal information and biometrics. It would be wrong to go back on our word and subject these individuals to deportation,” the Republicans’ letter states. “These individuals’ status in the United States should not be left to the political winds of different administrations that come to power.”
Denham and Valadao represent districts with large Latino populations and are among Democrats’ targets in 2018. They joined a handful of Republicans in a recent letter urging President Trump not to end the program, and are co-sponsors of legislation aimed at finding a fix.
Ryan told radio station WCLO in Janesville, Wis., Friday that he didn’t think Trump should end the program and that a legislative solution is needed.
“[T]here are people who are in limbo,” Ryan said. “These are kids who know no other country, who were brought here by their parents and don’t know another home.”
House Minority Leader Nancy Pelosi of San Francisco sent her own letter to Ryan on Friday, calling his remarks “heartening” and asking him to meet with House Democrats and the Congressional Hispanic Caucus about possible legislation when Congress returns next week from the August recess.
NRA marks win as lawmakers gut measure that would have limited rifle purchases in California

The National Rifle Assn. won a rare victory in the California Legislature on Friday when a committee gutted key portions of a bill that would have prohibited buying more than one rifle in any 30-day period.
Instead of limiting the number of guns, the bill was amended by the Assembly Appropriations Committee, without explanation, to leave in only a requirement that law enforcement officials securely store firearms in vehicles when no trunk is available.
State law already bans buying more than one handgun a month, but Sen. Anthony Portantino (D-La Cañada Flintridge) introduced the measure to also include long guns in that limit.
The limit was opposed by groups including the NRA and the Firearms Policy Coalition.
“This is an important win for current and future gun owners,” said Craig DeLuz, spokesman for the Firearms Policy Coalition. “The rationing of civil rights should never be tolerated.”
Portantino said it appeared the governor and others had concerns about the bill. He noted that Gov. Jerry Brown has been cautious about regulating long guns, which are often used by hunters.
“We’ll take the half a loaf we got and continue to work on the issue,” he said after the vote.
Ten bills regulating pot in California are sidelined for the year as state bureau works to finalize its own rules

Ten bills aimed at regulating marijuana were shelved Friday by state lawmakers, giving California’s new Bureau of Cannabis Control time to finish its own rules before lawmakers pile on with additional restrictions.
The bills held by the Senate Appropriations Committee without comment would have further regulated where pot can be used, how marijuana is marketed, the trademarking of products and would have required the state to produce a consumer guide.
The actions come as the state Bureau of Cannabis Control is preparing to begin issuing licenses and regulations for the growth, transport and sale of marijuana for medical and recreational use starting Jan. 2.
Many of the bills sidelined Friday duplicate or provide additional detail for tasks already undertaken by the bureau.
The consumer guide, which would have told Californians where they can buy marijuana and what the rules are for using it, includes information the bureau has already begun posting on its website.
One of the bills shelved, AB 1090, would have prohibited the possession, smoking or ingesting of cannabis on the grounds of a school, day care center or youth center at any time.
Analysts for the committee noted in a report that it is already illegal to possess or use cannabis in such places when children are present.
“Current law generally prohibits smoking on school grounds and at day care centers, at all times,” the analysis said. “Because current law prohibits smoking cannabis in any public place and where smoking tobacco is prohibited, this would include schools and youth centers.”
Another bill shelved, AB 76, would have prohibited the operator of a website from marketing marijuana products to people younger than 21. State law already bars the marketing of marijuana to minors, without specifying the venue.
The state has already allocated money to create a California Cannabis Research Program to look at issues including the impact of marijuana on motor skills. The committee balked Friday at expanding the studies to look at synthetic compounds, and to allow the state to grow and study its own marijuana after state finance officials said the changes would cost California $3 million.
“Legislative leaders are working with the administration on a budget trailer bill to resolve cannabis-related issues. It makes sense to take a comprehensive approach,” said Sen. Ricardo Lara (D-Bell Gardens), chairman of the committee.
Leonardo DiCaprio boosts California energy bill
Actor and environmentalist Leonardo DiCaprio voiced his support for Senate Bill 100, which would phase out fossil fuels for generating electricity in California.
Senate President Pro Tem Kevin de Leόn, the measure’s author, responded with a clip from “Titanic.”
Bill to study police shootings in California shelved by state Senate committee

A measure that would that would have funded a study of police shootings across California by state Atty. Gen. Xavier Becerra failed in a Senate committee Friday.
The bill, Assembly Bill 284 from Assemblyman Kevin McCarty (D-Sacramento), would have authorized Becerra to examine the circumstances, policies, training and oversight involved in police shootings that resulted in death or serious injuries between 2015 and 2016 for a report issued by July 2019.
Becerra testified on behalf of the measure during a Senate committee hearing in July, saying it would help the state develop policies that would reduce police shootings in the future. According to Becerra, California had 230 police shootings that resulted in death or serious injury in 2016.
A Senate Committee on Appropriations analysis of the bill said the study would have cost $3.5 million in the first year and $1.9 million in the second year.
State senators block additional environmental review for Mojave Desert groundwater project
Lawmakers halted a proposal Friday that would increase environmental scrutiny of a groundwater pumping project in the Mojave Desert.
The episode is another chapter in a long-running controversy over whether Cadiz Inc., a company based in Los Angeles, will be allowed to take water from under the desert floor and sell it to Southern California cities.
The legislation, AB 1000 from Assemblywoman Laura Friedman (D-Glendale), would give the State Lands Commission and the Department of Water Resources the authority to block the project if it would have a negative environmental impact, as some have warned.
The proposal was introduced after the Trump administration reversed the Obama administration’s opposition to the project earlier this year.
U.S. Sen. Dianne Feinstein (D-San Francisco) and Gov. Jerry Brown have expressed concern about Cadiz’s plans.
Brown took the rare step of weighing in on pending legislation, writing in a letter that the proposal was “basic common sense” necessary to protect desert landscapes that “may be the most fragile ecosystems of all.”
However, the Senate Appropriations Committee shelved the legislation.
Sen. Ricardo Lara (D-Bell Gardens), the committee’s chair, said there already was an adequate review process in place for the project.
“Making an exception for one particular case will create precedent for the Legislature to block other controversial projects,” he said in a statement.
Senate President Pro Tem Kevin de León (D-Los Angeles) supported halting the legislation, but Feinstein blasted the decision.
“Blocking Cadiz is one concrete way to stop the Trump administration from hurting California,” she said in a statement. “I hope our state leaders reconsider this bill and move it forward.”
Sen. Dianne Feinstein’s political advisor defends against criticism over her call for ‘patience’ with Trump

Sen. Dianne Feinstein’s top political advisor pushed back Friday at criticism from liberal activists and some fellow elected Democrats who took issue with the senator’s call for “patience” in dealing with President Trump. Feinstein made the remarks Tuesday at San Francisco’s Commonwealth Club, adding that Trump could be a good president if he learned and changed.
Bill Carrick, Feinstein’s longtime strategist, argued that California’s senior senator has been a vocal and persistent critic of Trump and his policies.
“The reality is she has opposed and confronted the Trump administration on many, many issues, starting with the Supreme Court nomination of Judge [Neil] Gorsuch,” Carrick said, adding that Feinstein is currently pressing the president not to end the Deferred Action for Childhood Arrivals policy, or DACA, an Obama-era program that protects young immigrants from deportation and provides work permits for employment. “So her opposition has been consistent and aggressive against Trump when she thinks he’s wrong, which is very often.”
Feinstein has not yet announced whether she will seek a sixth term next year.
Media literacy bill fails in California Legislature

Media literacy classes will not be coming to California schools.
Lawmakers killed legislation Friday to teach students how to evaluate the accuracy, credibility and comprehensiveness of online news.
The bill, SB 135, by Sen. Bill Dodd (D-Napa), called for curriculum to promote communication, digital citizenship and responsible technology use.
Teachers could choose whether to use the developed curriculum in the classroom.
Lawmakers have taken no action on a similar bill introduced by former Assemblyman Jimmy Gomez, now serving in Congress.
2:45 p.m.: This post was updated to reflect the current status of the similar legislation.
Effort to limit pot advertising on clothing in California falls short
The pot industry scored a victory in the state Legislature on Friday as lawmakers killed a proposal to ban marijuana advertisements on clothes for young people.
Sen. Ben Allen (D-Santa Monica) had proposed the legislation with the intent to make marijuana less attractive to young people by prohibiting sellers and manufacturers from using merchandise such as clothes and hats to promote their products.
California voters approved a ballot measure in November legalizing recreational marijuana starting in January.
Opponents of Allen’s bill, including the California Cannabis Manufacturers Assn., said such a law would be a financial burden, depriving them of legitimate profits.
The groups argued that the advertisement of medicinal marijuana should not be restricted in the same way as adult-use marijuana. The group wrote that the bill “undercuts a legitimate revenue center for cannabis licensees,” and that it impinges on free speech.
Supporters of the bill, including the state chapter of the American Academy of Pediatrics and the California Police Chiefs Assn., believed the measure would decrease marketing to youth.
The Assembly Appropriations Committee, which evaluates bills that will cost a lot of money, put the measure on hold without explanation.
“The Legislature in the past has wisely prohibited advertising with branded merchandise by tobacco companies, expressly because items like hats and t-shirts are known to entice kids to smoke,” Allen said. “This was a commonsense measure to apply similar restrictions that would help prevent marijuana use by teens.”
1:25 p.m.: This card was updated with a comment from Allen.
State bill requiring California police to disclose surveillance equipment stalls in fiscal committee
A bill that would have required law enforcement agencies in California to disclose all of their surveillance equipment to the public stalled on Friday in the state Assembly Appropriations Committee amid its high costs.
Under the legislation by state Sen. Jerry Hill (D-San Mateo), police and sheriff’s departments would have had to submit a plan to local officials — and present it at an open hearing — on what surveillance technology they employ and how, including facial recognition software, drones and social media monitors.
If a law enforcement agency had not adopted a policy by a July 2018 deadline, it would have had to stop its use of the technology within 30 days.
The bill required law enforcement agencies to generate public reports on the use of their gear every two years. The state Department of Justice and state Highway Patrol also would have had to comply with similar guidelines.
The fiscal committee found the state Justice Department would have faced significant costs to hire more people and would see an increase in workload to assist with online investigations, data collection and reporting surveillance use policies throughout the state.
Law enforcement agencies would also feel the burden. The Los Angeles County Sheriff’s office alone calculated the need for 10 positions and $600,000 to comply with the bill’s provisions, the committee found.
The bill was predicated on two laws that went into effect last year. One of those requires agencies to draft and publicly post privacy and usage policies for devices often called “Stingrays” or “Dirtboxes,” which simulate cellphone towers and cast a broad dragnet over communications.
Bill to reduce names on California’s sex offender registry shelved

A bill that would have ended lifetime listing of many convicted sex offenders on a public registry was shelved Friday after officials said it could cost tens of millions of dollars to make the change.
State Sen. Scott Wiener (D-San Francisco) and Los Angeles County Dist. Atty. Jackie Lacey had proposed that the names of those who committed lower-level, nonviolent sex crimes or who are judged to be low risks to reoffend be removed from the registry after 10 or 20 years.
State finance officials said in a report the bill would involve “significant ongoing cost in the tens of millions of dollars” for technology costs.
Millions of dollars would also be required to process more than 40,000 requests of individuals eligible to petition for termination, the report said.
Wiener had sought the change as a way to make the system more efficient for law enforcement.
“Our sex offender registry is broken and useless to law enforcement, with many nonviolent and low-level offenders who committed their offenses decades ago,” Wiener said. “If we’re serious about monitoring high-risk sex offenders — as we should be — we must reform this registry.”
He said it takes hours for law enforcement to do paperwork on each person on the registry each year, and the volume (105,000 people on the registry) makes it harder for police investigating new crimes to find potential offenders.
Corrections officials hear suggestions, complaints about revamping California’s parole system
About 100 people gathered in Sacramento on Friday to offer ideas and concerns about new regulations that have overhauled California’s parole system, an effort that will allow thousands more inmates to be considered for early release.
The group gathered outside a meeting where corrections officials were to hear public feedback, the first such meeting since state regulators gave the guidelines initial approval in April. The event drew criminal justice reform advocates, crime victim and public safety officials from across the state.
The regulations are being used to implement Proposition 57, last fall’s sweeping effort to provide new ways for inmates to earn time credits toward their sentences for good behavior and for enrolling in certain career, rehabilitation and education programs.
The ballot measure also allows the State Board of Parole Hearings to grant early release to a new population of inmates: those whose primary sentences are for crimes not designated as “violent” under California law and have served the full term of their sentences.
More than 50 reform advocates — including former inmates and crime victims — said at a small rally before the meeting that state prisoners should be allowed to receive credits retroactively, for rehabilitation and work-study programs they completed before Proposition 57 went into effect.
They also called on corrections officials to extend the new law’s benefits to those sentenced for a third offense under the state’s three-strikes law and to prisoners serving sentences for crimes they committed as youths.
“Speak with fire, speak with passion, because [inmates] can’t speak for themselves,” said Jay Jordan with Californians for Safety and Justice, who said coalition members had sent 10,000 letters in support of such changes.
Amika Sergejev with the Young Women’s Freedom Network in San Francisco said the regulations will block any benefit to some offenders who weren’t supposed to be excluded under Proposition 57.
Sergejev, who said she served seven years for manslaughter after killing a 65-year-old man in a car crash, grew personally from completing programs while incarcerated.
“I am here really representing the sisters that I left behind,” she said.
But crime victims also gave a glimpse into the tough balance that corrections officials have had to strike with the new regulations.
Linda Wilson, who said she escaped an abusive partner, shed tears at the meeting while relating that her abuser continued to torment and threaten her from prison. She said some mentally ill and abusive offenders cannot be reformed and should not be allowed to manipulate the system.
“A second striker who does the same crime against the same person shows a pattern,” she said.
Last call stays the same, as lawmakers turn off the taps on keeping California bars open until 4 a.m.

Lawmakers rejected a proposal on Friday to allow many California bars to extend hours of operation until 4 a.m., a bill that would have marked the first expansion of the hours of sale for alcohol since 1935.
Instead, the bill was revised to create a task force for studying the issue of keeping bars open beyond 2 a.m., with a report due back to the Legislature by the end of 2019.
Senate Bill 384 had garnered widespread attention, with supporters saying it would have simply given local communities the option to extend operating hours. Backers also cited that bars and restaurants outside of California are allowed to sell beer, wine and hard liquor after 2 a.m., putting some cities at an economic disadvantage.
The bill’s author, state Sen. Scott Wiener (D-San Francisco), told The Times earlier this year that young adults often end up moving to unsafe and illicit parties after the bars close, and that the bill simply dealt with “the reality of life.”
SB 384 had a long list of opponents, who argued that the extended serving hours would only push the problems with alcohol consumption further into the predawn hours.
A legislative committee analysis found nine states plus the District of Columbia allow alcohol sales after 2 a.m.
In a written statement on Friday, Weiner criticized the action to turn the issue into fodder for further study.
“There’s nothing radical about letting local communities decide for themselves whether to let their bars and nightclubs go later,” he said. “It’s embarrassing that California shuts down its nightlife so early. We’re not going to give up.”
12:49 p.m. This story was updated with comment from Wiener. The story was originally published at 11:59 a.m.
Proposal for 100% clean energy marches forward in Sacramento

California lawmakers advanced legislation on Friday to phase out fossil fuels for generating electricity.
The measure, SB 100 from Senate President Pro Tem Kevin de León (D-Los Angeles), was approved by the Assembly Appropriations Committee. If passed by the full Assembly in the coming weeks, it can be sent to Gov. Jerry Brown’s desk.
The legislation would accelerate the state’s adoption of renewable energy, requiring utilities and other electricity providers to obtain 60% of their power from sources like the sun and the wind by 2030. Then it would task regulators with ensuring the final 40% doesn’t come from fossil fuels by 2045.
Offshore drilling crackdown stalls in California Legislature
Legislation that would clamp down on offshore drilling along California’s coast stalled on Friday.
The measure, SB 188, had been introduced by Sen. Hannah-Beth Jackson (D-Santa Barbara) after President Trump announced in April that his administration would consider allowing more drilling.
“I’m really disappointed,” Jackson said. “I’m not going to give up,” adding that she may bring back her proposal next year.
Trump’s executive order sparked outrage in California, where no new leases have been issued for state waters since 1969 and none for federal waters since 1984.
Jackson’s proposal would have prevented new oil infrastructure, such as pipelines or piers, on state land along the coast. Existing leases would not be renewed if it meant an increase in oil production.
“This is important to protect our beautiful coast and fight back against President Trump,” said Assemblyman Al Muratsuchi (D-Torrance), who carried the legislation in the Assembly.
It faced a range of opposition before stalling in the Assembly Appropriations Committee on Friday.
The oil industry said lawmakers shouldn’t restrict decision-making by the State Lands Commission, which has already pledged to block new drilling infrastructure. Labor groups expressed concern it would affect jobs for their members.
Gov. Jerry Brown’s Department of Finance also opposed the legislation, saying it could reduce state revenue and lead to more oil being transported by barges instead of pipelines.
This post has been updated with a new comment from the measure’s author and details on the State Lands Commission opposition to drilling.
Sen. Dianne Feinstein faces liberal backlash as she decides whether to seek reelection

At a time when the Democratic base is more restive than it has been in decades, Sen. Dianne Feinstein ignited a firestorm earlier this week when she refused to back an impeachment push and instead called for “patience” with President Trump.
The statements — provocative in Democratic circles, near-heretical in her hometown of San Francisco, where she made them — reflected a moderation and pragmatism that have hallmarks of Feinstein’s career.
But because of the state’s shifting demographics and political leanings, these qualities, after proving politically advantageous for decades, could become an albatross as the 84-year-old decides whether to seek a sixth term.
Potential rivals are already circling.
Hundreds of bills face Sacramento’s ‘suspense file’ deadline

On Friday, lawmakers make final decisions about which of the year’s most costly bills will get a full vote in both houses, with clearing of the “suspense file” in appropriations committees of both houses — lists that include 472 pieces of legislation.
The bills were all placed in what amounts to legislative limbo because they would spend $150,000 or more of taxpayer funds in the coming fiscal year. But the holding pattern for the bills is also a reflection of the desire for political horse-trading in the final weeks of the 2017 legislative session, as majority Democrats weigh which proposals are most important and which ones can wait.
The clearing of the “suspense file” in the state Senate and Assembly appropriations committees is also one of the more opaque parts of the legislative process. Unlike traditional committee hearings in which members cast a public vote, the Senate and Assembly bills dealt with on Friday will be moved or killed on broad party-line actions. The chairperson in each committee will not announce individual votes, allowing lawmakers to avoid scrutiny for either approving or killing the bills in question.
By far the largest number of bills — 334 — await action in the Senate Appropriations Committee, which on Friday is considering bills written by members of the Assembly. There are 138 bills written by senators on the “suspense file” in the Assembly Appropriations Committee. More than 800 bills had to be acted on during the first round of the process in late May.
Lawmakers have until Sept. 15 to act on the bills that remain active after Friday’s fiscal committee vetting process.
